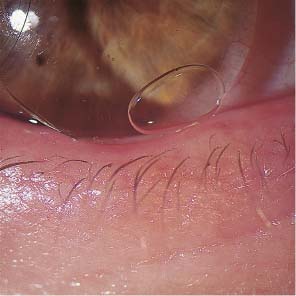
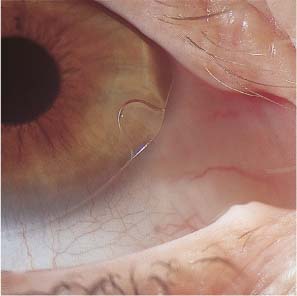
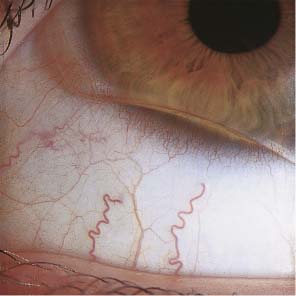
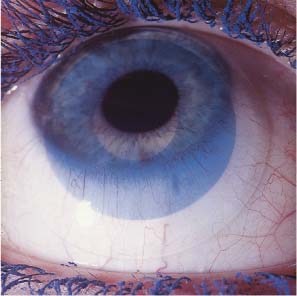
4 Visual Impairment Intermittent Visual Impairment Diagnostic Evaluation of Visual Impairment and Glare Some 45% of contact lens wearers complain on follow-up visits that their vision is poorer than when their lenses were first fitted; this percentage is considerably larger than with spectacle wearers. Worsened vision in contact lens wearers is usually due to faulty lens care and handling, but it may also be unrelated to the contact lenses. Contact lens wearers develop eye diseases that impair vision, such as progressive myopia, glaucoma, cataracts, and retinal detachments, just as frequently as wearers of spectacles. As outlined in Table 22, visual impairment in contact lens wearers can be divided into two categories. In the first category, the problem arises only when contact lenses are worn and disappears immediately when spectacles are worn instead. In the second, the problem persists when spectacles are worn. Findings Cause 1. Contact lens on eye No improvement with phoropter lenses Deposits Material defect, tear deficiency, wetting problem, primary ocular disease 2. Contact lens on eye Improvement with phoropter lenses Faulty insertion Slipped or lost lens, inverted lens, lens on wrong eye, both lenses on one eye 3. Contact lens removed No improvement with phoropter lenses Clouding of refractive media Corneal erosion, infection, CDS, primary ocular disease 4. Contact lens removed Improvement with phoropter lenses Orthokeratologic effect Change in refractive error not related to the contact lens Faulty contact lens handling and insertion can lead to visual impairment by disturbing the function of the optical system comprising the lens and the surrounding tear film. The patient may be shocked by sudden binocular visual deterioration one morning only to discover, on ophthalmological examination, that the right lens was switched with the left, or that both lenses were inserted in the same eye. Such problems are readily diagnosed with refractive testing and slit-lamp examination. Vision is immediately normalized with additional lenses in the phoropter. If refractive testing reveals an error of 20 D or more with a rigid lens, then the lens was presumably forcibly inverted at some point during cleaning and disinfection, and thereby optically neutralized. The diagnosis can be confirmed under the slit lamp with an inverting prism or by measurement of the lens parameters. In contact lens wearers, as in wearers of spectacles, visual impairment that is correctable with additional lenses often develops when myopia increases or decreases or when the refractive error fluctuates for other reasons. These changes are often gradual and may not be noticed by the patient until they are detected in an ophthalmological follow-up examination. Sudden loss of a contact lens causes a marked, acute loss of visual acuity, which may be a dangerous event if, for example, the lens wearer is driving a vehicle at the time. Lens loss often occurs with vigorous movement or a blow to the head, or during water sports, where only a few splashes may suffice to wash the lens out of the eye. When the patient complains of lens loss, the examiner should verify that the lens is truly no longer in the eye, as the supposedly lost lens—or fragments thereof—is sometimes found in the conjunctival sac, occasionally weeks after the event. It may also become embedded in the conjunctival tissue and manifest itself months later as an encapsulated, chronic inflammatory process. Visual impairment caused by a primary ocular disease (e.g., clouding of the refractive media) presents in the same way in contact lens wearers as in persons who do not wear contact lenses. Determination of the cause requires testing of subjective visual acuity with and without contact lenses (or with and without spectacles, in patients who wear them). The ocular diseases that most often impair vision in contact lens wearers are the common ophthalmological disorders: glaucoma, cataract, macular degeneration, and others. Retinal detachment occurs with equal frequency in contact lens wearers and spectacle wearers. The frequency is related to the degree of myopia, not to the wearing of contact lenses. Hyperopic eyes are prone to glaucoma. Patients with hypertension, diabetes mellitus, or other metabolic disturbances may develop chronic changes in the fundus that impair vision, whether or not contact lenses are worn. Moreover, the contact lens wearer complaining of impaired vision should always be examined for uveitis, retinal detachment, and optic neuritis—all of which have no relation to the wearing of contact lenses, even if the patient attributes the problem to the lenses, or to the specialist who fitted them. Thus, the treating ophthalmologist must continually bear in mind that the normal aging process, and all other disorders that can befall the eye, occur with equal frequency in contact lens wearers as in other patients. The follow-up of contact lens wearers cannot be limited to a check of the contact lens system but must also be directed toward the detection and, if possible, treatment or prevention of all such processes. Fig. 291 “Lost” hard lens displaced into the nasal canthus; fluorescein staining. Fig. 292 Soft keratoconus lens, flatly fitted. Air bubble beneath raised edge of lens. Fig. 293 Soft lens on toric cornea, flatly fitted; wrong lens type. Fig. 294 Truncated soft toric lens, flatly fitted, superiorly displaced. Fig. 295 Soft, tinted lens, flatly fitted, inferiorly displaced. Visual impairment when contact lenses are worn that cannot be improved with additional lenses at the phoropter is most likely due to defective contact lenses. Possible defects include scratches, craters, fractures, deposits, and deformations (see p. 147). For example, a tear in the center of the lens causes a visual impairment that cannot be corrected with over-refraction. The same is true of deposits, one of the commonest causes of visual problems among contact lens wearers. Lipids and proteins from the tear fluid are continually deposited on the lens surface as long as it is in the eye and will accumulate over time if the daily cleaning routine is inadequate or too infrequently performed. Jelly-bump deposits frequently form on lenses of high water content. These are stubborn calcium-protein deposits (see p. 151) that are difficult to remove and markedly impair visual acuity and wearing comfort. In most cases, the deposits cannot be removed completely and new lenses are required. Note: Lenses with insoluble deposits or other defects should not be reworn under any circumstances, even for brief periods, because of the danger of corneal and conjunctival injury.
Visual Impairment
Causes of Visual Impairment
Changes in Refraction
Faulty Lens Handling and Insertion, Lens Loss
Permanent Visual Impairment
Primary Ocular Diseases Masked by Contact Lenses
Material Defects and Defective Lenses
![]()
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


Ento Key
Fastest Otolaryngology & Ophthalmology Insight Engine