Fig. 9.1
Triangles of the neck: anterior triangle (submental, digastric, carotid, and muscular triangles) and posterior triangle (occipital and subclavian triangles)
9.1.1.2 Posterior Triangle
9.2 Introduction
Neck swellings represent a very important entity in the surgical practice. Sticking to the definition, a neck swelling should include any mass that presents in the neck whatever its origin is. However, for the sake of classification, neck swellings described in this chapter will not include masses arising from the thyroid gland, parathyroid glands, salivary glands, pharynx, larynx, or lymph nodes, as these entities are detailed in separate chapters. Accordingly, diseases of such organs will be mentioned in this chapter only by name, so that differential diagnosis is complete.
Swellings of the neck are generally categorized into two groups: midline and lateral neck swellings. Midline neck swellings include those few swellings which clinically present in the neck midline from the submental triangle just below the chin above to the suprasternal notch below. Swellings which do not respect this anatomical imaginary midline are termed lateral neck swellings, whether presenting in the anterior or posterior triangles.
Midline and lateral neck swellings may be further classified in different ways. They may be classified as solid versus cystic, congenital versus acquired, or according to the anatomic subregion of presentation. It should be noted that half of all neck masses seen in a general hospital are of thyroid origin [2].
9.2.1 Diagnosis of a Neck Mass
A complete history with full head and neck examination, including flexible laryngoscopy, is crucial to reach a proper diagnosis. This is also dependent on the location of the mass and the patient’s age. In children, most neck masses are inflammatory or congenital. However, in the adult population, a neck mass >2 cm in diameter has a >80 % probability of being malignant.
Fine-needle aspiration, preferably with the assistance of ultrasound (US) or CT guidance, can provide a valuable tool for early treatment planning that provides less oncologic disruption to a tissue mass than an open biopsy. The use of CT scanning and/or MRI imaging is dictated by the patient’s presentation.
If no definite diagnosis can be concluded after this workup, an open biopsy may be the last resort for reaching a proper diagnosis and plot a therapeutic plan. Special caution should be taken while handling the biopsied material to avoid tissue destruction and the need for rebiopsy. Putting the skin incision for such a biopsy should take into consideration the possibility of performing a future neck dissection, composite resection, and/or a major reconstruction [3].
9.3 Midline Neck Swellings
Midline neck swellings are summarized, according to their anatomical site, in Table 9.1.
Table 9.1
Classification of midline neck swellings
Anatomical region | Causes |
|---|---|
A. Submental region | 1. Submental lymph nodes (LNs) 2. Sublingual dermoid cyst 3. Hourglass ranula 4. Abscess related to the mandible (central incisors) |
B. Hyoid bone region | 1. Thyroglossal cyst 2. Median ectopic thyroid tissue 3. Subhyoid bursitis 4. Tumor of the hyoid bone |
C. Laryngeal region | 1. Prelaryngeal (Delphian) LNs 2. Laryngeal tumors 3. Bursa in front of Adam’s apple 4. Chondritis of thyroid cartilage |
D. Tracheal region | 1. Pretracheal LNs 2. Nodule in the isthmus of the thyroid gland |
E. Suprasternal space (space of Burn) | 1. Enlarged LNs 2. Lipoma 3. Teratoma 4. Thymoma 5. Aneurysm of the aorta or innominate artery 6. High aortic arch |
9.3.1 Neck Dermoid Cysts
Neck dermoid cyst may present anywhere along the midline. It may present as a sublingual mass above or below the mylohyoid muscle and may bulge into the submental triangle. It is either epidermoid, true dermoid, or teratoid, which is the rarest variety. It usually presents between 10 and 25 years of age, affecting both sexes equally. The patient complains of a swelling, which becomes painful and tender if infected. On examination, the swelling is smooth, spherical, opaque, fluctuant, and clearly defined.
It is treated by surgical excision. If it is sublingual in position, the mucous membrane appears normal and the cyst can be felt bidigitally. Surgical excision is preferable through the oral route because of the hidden scar (Fig. 9.2) [2, 4].
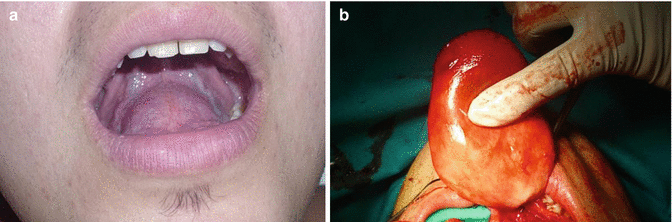

Fig. 9.2
(a) Sublingual dermoid cyst presenting as an intraoral swelling. (b) The cyst being excised through an intraoral route
9.3.2 Abscess in Relation to the Mandible
Infection may occur in relation to carious central incisors leading to a “subperiosteal abscess.” A sinus may be present. Plain X-ray appearance is diagnostic.
9.3.3 Subhyoid Bursitis
This rare condition usually affects old patients. It forms a translucent sausage-shaped swelling parallel to the lower border of the hyoid bone. The swelling is mobile with protrusion of the tongue.
9.3.4 Median Ectopic Thyroid Tissue
9.3.5 Tuberculous Thyroid Chondritis
The thyroid cartilage is thickened and tender and a rectangular abscess may complicate the condition. Tuberculous laryngitis and open pulmonary tuberculosis (TB) may coexist.
9.3.6 Cyst/Nodule of the Thyroid Gland Isthmus
This lesion is mobile with deglutition. Other parts of the thyroid gland may be affected as well. Absence of a track between it and the hyoid bone as well as being not mobile with tongue protrusion differentiates it from thyroglossal tract cyst.
9.3.7 Thyroglossal Cyst
9.3.7.1 Embryology and Pathogenesis
The thyroid gland buds off the foregut diverticulum at the base of the tongue in the region of the future foramen cecum at 3 weeks of embryonic life. As the fetal neck develops, the thyroid tissue becomes more anterior and caudal until it rests in its normal position. The “descent” of the thyroid is intimately connected with the development of the hyoid bone.
9.3.7.2 Sites
A thyroglossal cyst may present in the substance of the tongue (lingual thyroglossal cyst), in the suprahyoid region (as a mass in the floor of the mouth or submental triangle), or in the infrahyoid region, which is the commonest site, as the duct obliterates from above downward. This latter type might present in front of the thyroid cartilage, cricoid cartilage, or even at the suprasternal notch. Occasionally it presents as an intrathyroidal mass. The commonest site of all is the peri-hyoid bone cyst [1, 4, 8].
9.3.7.3 Incidence
Remnants of thyroglossal duct are estimated to persist in 7 % of the population. Cystic remnants are the commonest congenital anomaly of the neck. The lesion is most commonly appreciated in the 2- to 4-year-old child when the baby fat disappears. Some authors state that the incidence is higher in females and some deny any sex predilection [1, 2]. Ninety percent of the cases occur in the midline and 10 % are lateral, of which 95 % are left and 5 % are right. It is three times more common than the branchial cysts [2, 8].
9.3.7.4 Pathology
The cyst lined by cubical or stratified squamous epithelium. It contains mucoid fluid or cheesy yellowish material rich in cholesterol. Sometimes, the wall may contain “ectopic thyroid tissue” [4].
9.3.7.5 Clinical Picture
The cyst is painless and presents for a long time. Pain, tenderness, and an increase in size occur only if the cyst becomes infected, usually after upper respiratory tract infection. On examination, the cyst is 0.5–5 cm large, well defined, rounded, and with a smooth surface. It moves vertically up with protrusion of the tongue (characteristic sign) or swallowing. The lower jaw is held still with the mouth opened. The clinician holds the cyst between the finger and thumb and feels it tugged upward when the tongue protrudes. It is a difficult sign to elicit so one should not expect much movement. This sign is due to the cyst being abnormally attached to the hyoid bone by a fibrous tissue remnant and the hyoid bone being normally attached to the tongue through the hyoglossus muscle (Figs. 9.3 and 9.4). Although diagnostic, its absence does not exclude the diagnosis. This sign is absent from most of the cysts which are below the thyroid cartilage (which are indeed rare). Such a fibrous tissue track allows the cyst to be moved sideways but not up and down. Some cysts may form on both sides of the hyoid bone, i.e., dumbbell-shaped lesion. It fluctuates easily; however, few are not, being so tense. Many are opaque due to desquamated epithelial cells or debris of previous infection, few are illuminant, and many are too small to illuminate [1, 3, 8–10].
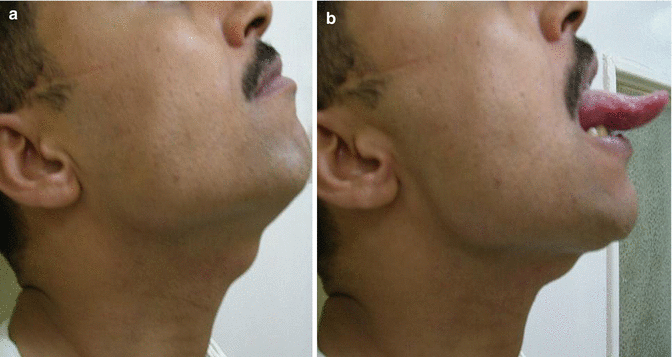
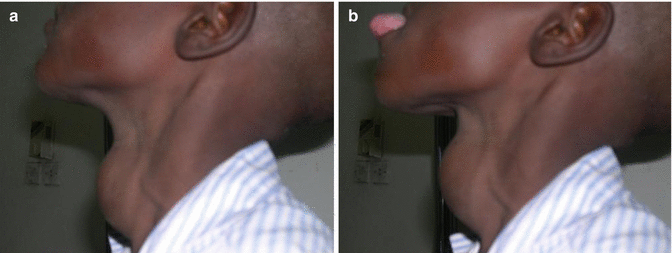

Fig. 9.3
(a) Thyroglossal cyst with the tongue in place. (b) With the tongue protruded. Note the upward movement of the cyst

Fig. 9.4
(a) Thyroglossal cyst with the tongue in place. (b) With the tongue protruded. Note the upward movement of the cyst. The cyst is large enough to mimic a goiter
9.3.7.6 Complications
Complications include infection, which is inevitable, as the lymphatic tissues in its wall communicate with the neck LNs. Ectopic thyroid tissue present in the cyst might lead to goiter manifestations. However, the most serious complication is the development of carcinoma. Thyroglossal carcinoma has no sex predominance, with a peak incidence in the fourth decade in females and in the sixth decade in males. Such tumors are very rare and are most commonly papillary thyroid carcinoma (PTC), followed (equally) by mixed papillary-follicular and squamous cell carcinoma. Adenocarcinoma was reported. Pure follicular and anaplastic carcinomas are extremely rare. Medullary cancer has never been reported. Their pathogenesis is debatable, and some presume they are metastasis from occult PTC; however, most authors suggest they are de novo neoplasms. Thyroglossal cyst carcinoma should be suspected whenever the cyst grows rapidly, when the US demonstrates a complex anechoic pattern or in the presence of calcifications. Still, they are treated by Sistrunk operation with low recurrence rates. This may be followed by thyroxin suppression therapy and regular measurements of thyroglobulin, which becomes undetectable if successful removal of the carcinoma was achieved, as long as TSH is adequately suppressed by thyroxin [2, 8].
9.3.7.7 Differential Diagnosis
A thyroglossal cyst should be differentiated from swellings in the midline of the neck, namely, dermoid cyst, sebaceous cyst, lipoma, enlarged LN, hypertrophied thyroid pyramidal lobe, and choristoma.
9.3.7.8 Treatment (Sistrunk Operation, 1928)
Prior to excision, an imaging study is performed to identify functioning thyroid gland in the lower neck. This ensures that the cyst does not contain the only functioning thyroid tissue in the patient, if any. A transverse incision is made over the cyst. Removal of the cyst, tract, central portion of the hyoid bone, as well as a core of tissues up to the foramen cecum is done. Incomplete excision leads to recurrence, and a recurrent lesion is more liable to recur again. Factors predictive of recurrence included more than two infections prior to surgery, age below 2 years, and inadequate initial operation. Failure to remove the central part of the hyoid bone results in recurrence in three out of four patients [4, 7, 9, 10, 11].
9.3.7.9 Thyroglossal Fistula
This is an acquired fistula related to the thyroglossal duct. It represents about 15 % of the cases. It is never congenital. The opening is small, midline, and with a crescentic skinfold above it. It moves up with swallowing and with protrusion of the tongue (Fig. 9.5).
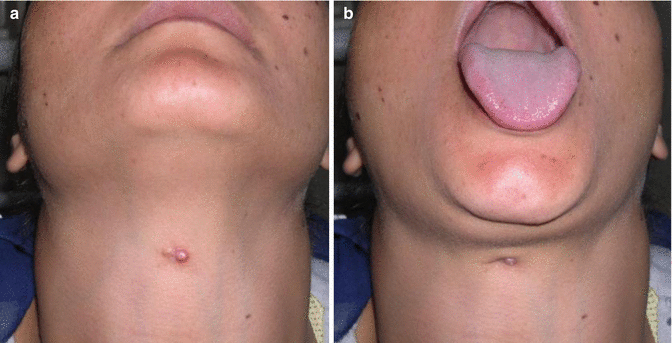

Fig. 9.5
(a) Thyroglossal fistula with the tongue in place, (b) Upward movement of the fistulous opening with protrusion of the tongue
There is intermittent discharge from the fistula which is often a seat of recurrent attacks of inflammation. The track may be felt as a thick fibrous cord extending up to the hyoid bone. It is surgically treated by excision through Sistrunk operation, but the incision is elliptical around the sinus, instead of being transverse [1, 7].
9.4 Lateral Neck Swellings
Lateral neck swellings are summarized, according to their consistency and anatomical location, in Table 9.2.
Table 9.2
Classification of lateral neck swellings
Anterior triangle | Posterior triangle |
|---|---|
Solid swellings | Solid swellings |
1. Lymph node enlargement 2. Thyroid gland nodule 3. Submandibular gland swellings 4. Parotid swellings (lower pole of the gland) 5. Swellings of the angle of the jaw 6. Paragangliomas (glomus tumors) 7. Schwannoma 8. Ganglioneuroma 9. Sternocleidomastoid (SCM) tumor 10. Lipoma | 1. Lymph node enlargement 2. Lipoma 3. Cervical rib |
Cystic swellings | Cystic swellings |
1. Pyogenic abscess 2. Cold abscess 3. Thyroid cyst 4. Branchial cyst 5. Plunging ranula 6. Laryngocele 7. Carotid artery aneurysm 8. Arteriovenous fistula | 1. Pyogenic abscess 2. Cold abscess 3. Retropharyngeal abscess 4. Cystic hygroma 5. Pharyngeal pouch 6. Subclavian aneurysm 7. Pneumatocele |
9.4.1 Solid Swellings of the Anterior Triangle
9.4.1.1 Lymphadenopathy
Enlargement of cervical LNs is the most common cervical swelling, whether presenting in a single fashion or a multiple fashion. Cervical LNs are enlarged in children mainly due to inflammatory causes and in adults mainly due to neoplastic causes. In adults, LNs tend to be more firm and less tender than those usually found in the neck of children due to recurrent upper respiratory tract infections. Cervical LN enlargement may represent a local disease in the neck (Fig. 9.6), be a part of generalized disease as lymphoma, or reflect a metastatic disease from below the clavicles as in the case of Virchow’s LNs.
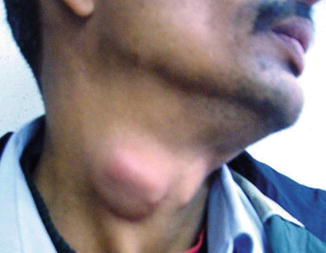

Fig. 9.6
A 35-year-old gentleman with enlarged and matted cervical LNs
Sonographic features of LNs help much in the diagnosis of their nature. Being rounded, of irregular contour, lost echogenic hilum, lost central and scattered peripheral vascularity, and internal necrosis are all in favor of malignancy. Elastography index and type of calcification if any are other parameters that might be included in the sonography report. The advantages of computed tomography in the imaging cervical LNs are the detection of extracapsular invasion as well as accurate assessment of their relation to carotid sheath vessels. Level VII LNs are definitely assessed by CT much more accurately than by US. Fine-needle aspiration cytology (FNAC) is a very important tool in completing the assessment of the patients presenting with cervical LNs [12].
9.4.1.2 Thyroid Swelling
A thyroid swelling is characteristically mobile with deglutition, and lies in the lower part of the front of the neck, deep to the SCM and strap muscles.
9.4.1.3 Swelling of the Lower Pole of Parotid Gland
Swellings arising from the lower pole of the parotid gland may be present in the lateral side of the neck, below the angle of the mandible (Fig. 9.7). This situation may give rise to diagnostic difficulty and should be included in differential diagnosis of a mass in the lateral side of the neck. A CT scan of the neck is helpful in identification of the parotid origin of the swelling.
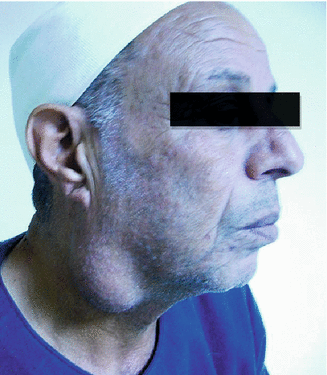

Fig. 9.7
Right parotid swelling (adenolymphoma) in a 64-year-old gentleman
9.4.1.4 Paragangliomas (Glomus Tumors: Chemodectomas)
Paragangliomas are tumors that are derived from neuroendocrine tissues in the paraganglia of nerves and are known to occur in the cervical, thoracic, and abdominal paravertebral spaces. They may also occur in the adrenal medulla where they are known as pheochromocytomas. Tumors that are thought to be derived from parasympathetic system are nonsecretor and nonfunctional tumors, whereas those which are thought to be derived from the sympathetic system are generally secretor and functional ones [13].
At imaging, four sites of origin may be distinguished and include carotid body tumor, glomus vagale, glomus jugulare, and their fourth partner, glomus tympanicum. Glomus vagale and glomus jugulare tend to displace the internal carotid artery (ICA) anteriorly. Glomus vagale tumors have smaller intracranial extensions and better developed capsules than glomus jugulare tumors.
Carotid body tumors show a greater tendency to splay the internal and external carotid arteries. What is the carotid body? It is a nest of chemoreceptor cells of neuroectodermal origin (3–6 mm) located on the posteromedial side of the carotid bifurcation (the carotid bulb). It responds to increased CO2, decreased O2, and acidity, i.e., hypoxia, resulting into increased blood pressure, heart rate, and depth and rate of respiration. It is usually benign but can become quite large and locally malignant, with regional metastases occurring in 20 % of cases and distant metastases rarely. All the three are tumors of the post-styloid parapharyngeal space [2, 3]. According to Shamblin’s classification, carotid body tumors are classified into three types depending on the degree of difficulty of resection. Type I describes tumors that are localized and easily resected, type II describes those which are adherent to or partially surrounding vessels, and type III describes those which intimately surround or encase the vessels and nerves [13].
Carotid Body Tumor
Carotid body tumors have a high incidence at high altitudes, such as in Peru, Colorado, and Mexico City. Chronic hypoxia leads to carotid body hyperplasia. Average presentation is in the fifth decade. No sex predominance is reported. Ten percent of the patients have a positive family history, where the disease is inherited as an autosomal dominant (AD) disease. The tumor presents on both sides in 30 % of the cases and has an association with adrenal pheochromocytoma. It usually runs a long history because it is a slowly growing tumor [2, 14].
Pathology
The carotid body tumor has a much more prominent surface vasculature than the glomus vagale and can be deeply embedded in the vessel wall, making resection extremely painstaking. Cells are histologically similar to normal carotid body. Cells are large, uniform epithelioid cells surrounded by a vascular stroma. It is hormonally inactive with rare proven metastases.
Symptoms
The tumor presents as a painless slowly growing lump over 5–7 years. Rarely, this is associated with attacks of transient cerebral ischemia manifested by giddiness, fainting, or transient paralysis or paresis, due to compression of the carotid artery by the tumor.
Clinical Examination
On examination the tumor is found in the upper part of the anterior triangle of the neck, in level with the hyoid bone, deep to the cervical fascia, and beneath the anterior edge of the sternomastoid muscle. Its size is variable from 2 to 10 cm. As it becomes larger, it extends upward. The overlying skin is normal. Hutchinson termed it the “potato tumor,” oval and hard. It has a smooth surface but sometimes is bosselated, with an indistinct edge. It is not tender and exhibits a normal temperature. It has a firm and rubbery consistency, is dull to percussion, and does not fluctuate. It is fixed to the carotid vessels, where it shows transmitted pulsations. It might sometimes show expansile pulsations from a soft very vascular tumor, and such tumors are also compressible and hence refill in steps synchronous with carotid pulse. However, sometimes it is not pulsating at all. A bruit may be present and the mass may decrease in size with carotid compression. The common carotid artery (CCA) can be felt below it, and the external carotid artery (ECA) may pass over its superficial surface (palpable pulsations). About 30 % of the cases present with a pharyngeal mass pushing the tonsil medially and anteriorly. Thus, biopsy of a pharyngeal swelling must never be taken from within the mouth. It can be moved horizontally with ease but has very little vertical mobility. Local LNs are not enlarged. Nerve involvement is rare [1–3, 13].
Investigations
Whenever a carotid body tumor is suspected, biopsy is contraindicated, but careful FNAC with a very narrow-gauge needle has been described. Carotid angiography will demonstrate a tumor circulation, cross-circulation if present, and determine tumor extent. Magnetic resonance imaging (MRI) is also useful to determine tumor extent. Some paragangliomas are demonstrated by metaiodobenzylguanidine (125I-MIBG) scintigraphy [15, 16].
Treatment
Metastases are exceptionally rare and the disease is rarely fatal. Thus, the mere presence of a carotid body tumor does not justify an attempt at removal. Provided that the patient has good general health, the indications for removal of a carotid body tumor are age <50 years; small- or medium-sized tumors; those extending into the palate or pharynx interfering with swallowing, speaking, or breathing; and tumors with an aggressive growth pattern. Although these tumors were originally thought to be radioresistant, cures have recently been reported. Radiotherapy using 131I-MIBG can be of value in patients who refuse surgery, in high-risk cases, or in metastatic disease [2, 7, 14–16].
Excision of a Carotid Body Tumor
An incision is made from the mastoid process to the clavicle down the anterior border of the SCM muscle. Dissection is adopted to expose the carotid sheath where the common carotid artery, internal jugular vein, and vagus nerve are identified. The common carotid artery is freed on all sides, preserving the vagus nerve carefully. A tape is placed loosely around the common carotid artery to allow easy and rapid occlusion of the carotid artery if the internal carotid artery is damaged later in the operation. Dissection proceeds from below upward along the adventitia, mobilizing the vagus nerve. On approaching the tumor, one will encounter large numbers of thin-walled veins, more brown than red in color. These veins bleed very easily and are a source of difficulty in this procedure. This difficulty can be overcome by dissection with two non-toothed dissecting forceps with fine points. The tissue is grasped close to the adventitia of the artery with these forceps and pulled apart. Surprisingly, this produces much less bleeding than attempts at sharp dissection, which are slow, tedious, and attended by steady bleeding. However, sometimes traditional ligation of such vessels freeing the tumor in a piecemeal fashion is sometimes necessary. The use of vascular clips may be time preserving. It should always be possible to preserve the vagus nerve but the hypoglossal nerve is often stretched and may need to be divided [2, 13, 14].
Glomus Vagale
Vagal paragangliomas arise from nests of paraganglionic tissue within the perineurium of the vagus nerve at its ganglion nodosum, i.e., just below the skull base. In large tumors there may be a small intracranial extension through the foramen jugulare. Intravagal tumors, however, are not restricted to this site and may be found at various sites along the nerve and down to the level of the carotid artery bifurcation.
In 50 % of the patients, there is more than 3-year history. It most commonly presents as a slowly growing and painless mass. It is associated with pulsating tinnitus, deafness, syncope, and/or vertigo. Pharyngeal pain is a late sign indicating irritation of the pharyngeal plexus, often preceding the onset of cranial nerve palsies. The mass is high in the anterolateral aspect of the neck, often noted near the origin of the SCM muscle with medial displacement of peritonsillar structures.
The diagnosis is confirmed by arteriography which tends to overestimate size owing to a surrounding pharyngeal plexus of veins. Surgery is indicated for vagal paragangliomas because of their tendency to spread into the cranial cavity. The approach used is that described for parapharyngeal tumors (trans-oral with mandibulotomy with transcervical approach or trans-parotid with transcervical one). The numerous thin-walled veins should be dealt with in the same way as for carotid body tumors. The most dangerous part of the dissection is superiorly where the internal carotid artery loops over the tumor and then immediately enters the skull. Injury is frequent at this site and therefore the help of a vascular surgeon is advisable [2, 4, 13, 14].
< div class='tao-gold-member'>
Only gold members can continue reading. Log In or Register to continue
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


