I. Congenital
1. Inclusion (sequestration) dermoid cyst
2. Meningocele/encephalocele
3. Cirsoid aneurysm
II. Acquired
A. Traumatic
1. Caput succedaneum
2. Hematoma (subcutaneous, subgaleal[subaponeurotic], subperiosteal)
B. Inflammatory
1. Infected granuloma
2. Osteomyelitis
3. Cock’s peculiar tumor
4. Suppuration (abscess)
5. Cellulitis and erysipelas
C. Sebaceous Cyst
Single – multiple – Cock’s peculiar tumor
D. Neoplastic
Benign tumors
Malignant tumors
1. Papilloma
2. Hemangioma
3. Lymphangioma
4. Cirsoid aneurysm
5. Plexiform neurofibroma
6. Lipoma
7. Osteoma
8. Chondroma
Primary tumors
1. Squamous cell carcinoma
2. Basal cell carcinoma
3. Malignant melanoma
4. Multiple myeloma
5. Fibrosarcoma
Secondary tumors from:
1. Thyroid
2. Breast
3. Bronchogenic carcinoma
4. Kidneys
5. Suprarenal glands
6. Prostate
E. Pott’s puffy tumor
2.2 Congenital Swellings
2.2.1 Inclusion (Sequestration) Dermoid Cyst
These cysts are due to inclusion of some of the surface epithelial cells (ectoderm) into the subcutaneous (SC) tissue at the lines of embryonal fusion of skin dermatomes. Although it presents later in life (childhood and adolescence), still it is considered “congenital” because it results from a congenital defect that develops between 3 to 5 weeks of intrauterine life [1–3]. The secretions of the skin (sweat and sebaceous) accumulate inside these cysts, and by time they grow slowly, forming a small cyst. In the scalp, very rarely, it may have an intracranial extension through a defect in the underlying bone, forming a dumbbell-shaped swelling, often called “hourglass dermoid.”
Pathologically, dermoid cysts have been c1assified in three groups: (1) congenital (teratorna type), (2) congenital inclusion cysts (due to desquamation, proliferation, and edema of dermoid cells), and (3) acquired (by implantation) [2, 4]. Microscopically, dermoid cysts are different from epidermoid cysts as they contain all the skin appendages, such as hair follicles, sebaceous glands, and sweat glands [5].
Clinically, an inclusion dermoid cyst may be seen at birth but usually a few years later when it begins to fill up. There is a preponderance for females in the anterior fontanel dermoid cysts [1, 5]. The main concerns are paternal distress at the cosmetic disfigurement and definite diagnosis. Dermoid cysts rarely become big enough to cause disability and rarely become infected [1, 5–7].
The anterior fontanel is the most common site [1, 6], but other midline or paramedian locations have also been reported [1, 8]. Different sites in the body including the head, neck, and trunk are summarized in Table 2.2. Congenital dermoid cysts are usually single, small in size (1–2 cm), and ovoid or spherical in shape, with a smooth surface and well-defined borders. Consistency is cystic or soft. The cyst may fluctuate but will not transilluminate (opaque). It is not pulsatile, compressible, or reducible and is non-tender. The skin overlying is normal unless it is inflamed [1, 4, 7, 8]. Dermoid cysts lie deep to the skin, in the SC tissue. Unlike sebaceous cysts, they are not attached to the overlying skin (you can pinch the skin over it), but like sebaceous cysts, they are not attached to deep structures.
Table 2.2
Different sites of inclusion dermoid cysts in the body
1. Head |
Midline of the scalp (most common site) |
Postauricular region |
Preauricular (temporal) region |
Inner and outer canthus |
At the fusion of the mandibular and maxillary processes |
Midline of the chin |
2. Neck, (midline, anteriorly, and posteriorly): |
Upper part (sublingual) |
Lower part (suprasternal) |
3. Trunk: |
Midline anteriorly (presternal dermoid) |
Midline posteriorly (pilonidal sinus) |
Plain X-ray (PXR) of the skull may show a soft tissue mass and flattering, indentation, or pitting of the outer table of the skull. Sometimes bone defects extending up to the inner table are noted [1, 5, 7, 9]. Computed tomography (CT) scan is valuable in showing extracranial localization of the cyst and excluding the intracranial extension [9] (Fig. 2.1). Diagnostic aspiration of the cyst is never recommended because it increases the risk of contamination and secondary infection [1].
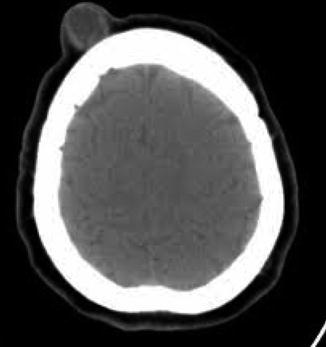

Fig. 2.1
CT scan of the skull showing no intracranial extension of the dermoid cyst in the scalp
The differential diagnosis of inclusion dermoid cysts of the scalp inc1udes encephalocele, sebaceous cyst, lymphangioma, hemangioma, melanoma, cephalhematoma, and lipoma [1, 8, 9].
Complications include infection (abscess formation) and depression of the underlying bone resulting in increased intracranial tension. It may have an intracranial extension causing cerebral compression, intracranial infection, or recurrence (after partial excision).
Treatment of congenital inclusion dermoid cysts is complete excision with careful dissection from the underlying bone and periosteum. This provides definitive diagnosis, prevents infection, and serves cosmetic reasons [2, 5]. If there is an intracranial connection, it is advisable to leave it until adulthood as the bones will fuse (close) and obliterate the stalk. The subcutaneous part can then be excised completely. If infected, forming an abscess, incision and drainage should be performed. This is followed later on by excision of the wall of the cyst, to avoid recurrence.
2.2.2 Meningocele/Encephalocele
Encephalocele is sometimes known by its Latin name “cranium bifidum.” It is a neural tube defect (NTD) that results in a saclike protrusion of the brain and the membranes that cover it through openings in the skull, most commonly in the occipital region. If the bulging portion contains only cerebrospinal fluid (CSF) and the overlaying membrane, it may be called a meningocele. If it also contains brain tissue, it may be referred to as a meningoencephalocele [10]. There are various types depending on location, which also has an impact on severity of the condition: occipital, frontoethmoidal, nasofrontal, and naso-orbital.
Although the exact cause is still unknown, there are several factors that have been reported to influence the risk of development of encephaloceles These include low levels of folic acid, vitamin C, and riboflavin during the first trimester of pregnancy; exposure to teratogens, trypan blue, or arsenic during early pregnancy; family history of NTDs; viral infections such as rubella or cytomegalovirus (CMV); diabetes mellitus; and maternal obesity and smoking [11, 12].
Encephaloceles are often associated with other craniofacial abnormalities or cerebral malformations [13]. The child may present with neurological deficits, hydrocephalus, spastic quadriplegia, microcephaly, ataxia, visual problems, seizures, as well as mental and growth retardation.
Usually encephaloceles are noticeable deformities and are diagnosed immediately after birth. The swelling itself is fixed to the skull and not adherent to the skin. It is tense, rounded, fluctuant, and translucent and yields an impulse on straining (crying). It may be small (Fig. 2.2) or huge in size. Prenatally these defects can be diagnosed by following tests: serum alpha-fetoprotein (AFP) levels, quadruple/triple screen, US, and amniocentesis [14, 15].
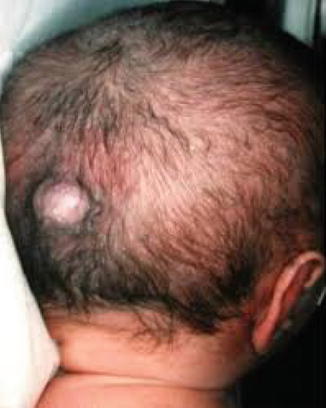

Fig. 2.2
A small encephalocele in the occipital region of the skull
Currently, the only effective treatment of encephalocele is reparative surgery that can be carried out pre- or postnatally. Prenatal surgery has a better outcome than that of postnatal. Prenatal fetal surgeries may include open fetal surgery and minimal invasive fetal surgery [16].
Postnatal surgery is usually performed during infancy. The extent of surgical correction depends on the location and size of the protrusion. The goals of surgical treatment include (1) closure of open skin defects to prevent infection and desiccation of brain tissue, (2) removal of nonfunctional extracranial cerebral tissue, (3) total craniofacial reconstruction, and (4) relief of intracranial pressure that may delay normal brain development. Occasionally, shunts are placed to drain excess CSF from the brain [12].
Prognosis is difficult to predict preoperatively and depends on the type of brain tissue involved and location of the encephalocele. In general, when the bulging material consists of primarily CSF, a complete recovery can occur. When a large amount of brain tissue is present in the encephalocele, there is a higher chance of perioperative complications. If surgery is successful and developmental delays have not occurred, a child can develop normally.
2.2.3 Cirsoid Aneurysm
Cirsoid aneurysms are rare arteriovenous fistulas of the scalp that are usually congenital though traumatic fistulas have also been reported [17]. In approximately 90 % of the patients, the superficial temporal artery (STA) is the main supply to the fistula, and in the remaining cases, there is usually involvement of both the STA and the occipital artery [17, 18]. It presents as an elongated, pulsating, tender mass, not attached to the skin or the skull (Fig. 2.3).
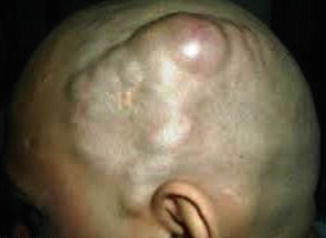

Fig. 2.3
Cirsoid aneurysm in the scalp with marked tortuous dilated vessels in a 23-year-old gentleman
The swelling empties easily on pressure and refills very rapidly on releasing the pressure. A thrill may be felt and a loud continuous bruit may be heard. There may be throbbing headache and hemorrhage. Untreated patients can develop progressive cosmetic deformity from the markedly tortuous subcutaneous vessels and, in severe cases, scalp necrosis [18].
The skull may show a bone defect, and angiography is the investigation of choice as it can show the feeding artery. Aneurysm of the STA and metastatic deposits from follicular carcinoma of the thyroid should be ruled out prior to the diagnosis of cirsoid aneurysm. Clinical examination with imaging confirms the diagnosis.
Simple elective ligation and complete excision of the cirsoid aneurysm are curative [19], without significant blood loss or scalp necrosis [20]. Alternative techniques for nonsurgical closure include intra-arterial embolization, transcatheter coagulation, injection of sclerosing solutions, and irradiation; however, results have been variable [21].
2.3 Acquired Swellings
2.3.1 Traumatic
2.3.1.1 Caput Succedaneum
Caput succedaneum is an edema of the scalp at the neonate’s presenting part of the head. It often appears over the vertex of the newborn’s head (Fig. 2.4) due to pressure against the mother’s cervix during labor. Edema in caput succedaneum crosses the suture lines and may involve wide areas of the head or it may just be a size of a large egg.
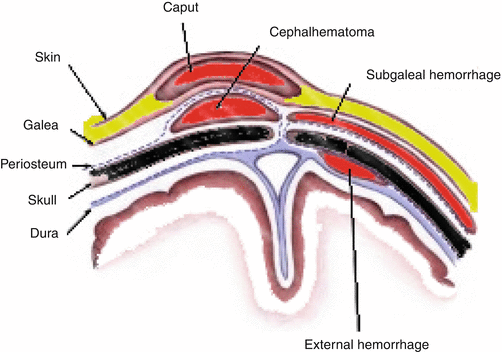

Fig. 2.4
Diagram showing the anatomical sites of caput succedaneum and cephalhematoma
Causes of caput succedaneum include mechanical trauma of the initial portion of scalp pushing through a narrowed cervix, prolonged or difficult delivery, and vacuum extraction. It is more common after rupture of the membranes or in presence of too little amniotic fluid such that there is no longer a “cushion” for the baby’s head. Vacuum extraction done during a difficult birth can also increase the chances of a caput succedaneum. The caput corresponds to the area where the extractor is used to hasten the second stage of labor [21].
A caput succedaneum may be detected by prenatal ultrasound (US) before labor begins. It has been reported as early as 31 weeks of pregnancy. The newborn presents with a soft and puffy scalp swelling that extends across the midline and over suture lines. It may or may not have some degree of discoloration or bruising. Jaundice may result as the bruise breaks down into bilirubin. Caput succedaneum needs no treatment as the edema is gradually absorbed and disappears on the third day of life [22].
2.3.1.2 Cephalhematoma
A cephalhematoma is a collection of blood between the skull and the periosteum of a newborn baby secondary to rupture of blood vessels crossing the periosteum. Because the swelling is subperiosteal, its boundaries are limited by the individual bones, in contrast to a caput succedaneum.
Cephalhematoma occurs in approximately 0.2–2.5 % of live births, usually due to prolonged second stage of labor or instrumental delivery, particularly ventouse. Vitamin C deficiency has been reported to possibly be associated with development of cephalhematomas [23].
The baby presents with a well-demarcated, fluctuant swelling that most commonly occurs over the parietal bone and occasionally over the occipital bone. It does not cross suture lines and there is no overlying skin discoloration. A cephalhematoma is not present at birth but appears by day 2–3 of life. It may worsen over the first few days and may take a few months to resolve as the blood clot is slowly absorbed from the periphery toward the center. In time the swelling hardens (calcification), leaving a relatively softer center that may be mistaken for a “depressed fracture,” but the lip is above the level of the rest of the skull.
< div class='tao-gold-member'>
Only gold members can continue reading. Log In or Register to continue
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


