Fig. 1.1
(a) Severe lacerations due to blunt facial trauma associated with facial fractures. (b) A linear cut wound of the cheek caused by assault with a sharp object
Avulsions
Owing to the abundant blood supply to the facial region, even the narrow-based avulsion flaps can survive if carefully re-approximated. Small insignificant avulsion flaps can be removed, but larger ones should be preserved with limited excision of the thinned out leading part. Compression dressing can help in decreasing the resulting edema.
Special Types of Injury
Human and animal bites: Copious irrigation should be done together with sharp debridement of infected and devitalized tissues. Prophylactic systemic antibiotics should be administered, and the wound should be planned for delayed reconstruction. It should be noted that human bites are more liable to become infected as they carry greater contamination than animal bites.
Facial burns: The modern principle of early excision and grafting of burns has a very limited application in the face; only circumscribed contact full-thickness burns benefit from this approach.
Soft tissue loss: The defect is covered by a full-thickness graft (Wolf graft), local flaps (rarely used especially in the young because of the scar they leave), or distant flaps from the forehead or neck, if the defect is too large for local repair.
1.2.3.2 According to the Location of Injury
Lip Injuries
If these lacerations are planned to be repaired under local anesthesia, alignment should be done before injection of the local anesthetic solution through marking, tattooing, or suturing. Orbicularis oris muscle injury should be carefully assessed and repaired. Alignment of the vermillion border is necessary for good cosmetic results to preserve what is known as “Cupid’s bow” [7] (Fig. 1.2).
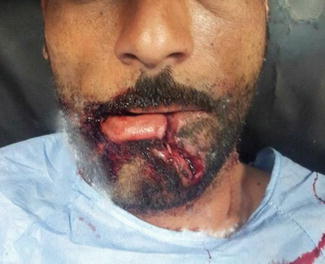

Fig. 1.2
A full-thickness lower lip laceration extending to the chin
Nasal Injuries
Proper alignment is necessary for sound esthetic reconstruction especially around the nasal rims. Speculum examination of the nasal septum should be performed to detect septal hematomas that—if left untreated—can end up in erosion and loss of septal cartilage. Such hematomas can be evacuated through small incisions. Repair of full-thickness nasal lacerations should proceed from deep to superficial layers starting from the nasal mucosa, cartilage, and finally the skin. Various algorithms have been described for reconstruction of nasal defects [8–10]. In “avulsion injuries,” the missed segment is cleansed and re-sutured as a composite graft, but if lost, a “composite graft” from the auricle may be used.
Eyebrow Injuries
No shaving of the eyebrow should be attempted. Tissues of questionable vitality should also be preserved. Proper anatomical alignment is required to achieve the best cosmetic results. In case of tissue loss in the eyebrow region, primary repair with interval hair graft harvested from the posterior scalp region should be sought.
Eyelid Injuries (Fig. 1.3)
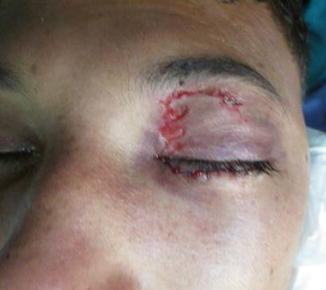
Fig. 1.3
Left eyelid laceration
The lower eyelid is usually more involved than the upper. Exclusion of any associated lacrimal or globe injury is mandatory at the time of wound assessment. Debridement should be minimal, and careful layer by layer repair should be done. Knots should be directed away from the eye globe. If the eyelid margin is involved by the injury, proper alignment of the cilia is required for optimum repair. An eyelid tissue defect may require lateral canthoplasty to allow for medial mobilization of the whole lid to close the defect [11].
1.2.4 Postoperative Care
Postoperative management of traumatic facial lacerations is rarely discussed in the literature. Many conflicting data regarding the optimum type of dressing, the use of topical antimicrobials, and the need for systemic antimicrobials in certain types of wounds exist. At other instances, the data are not strong enough to provide enough evidence.
In 2010, Nicholas Medel et al. [12] reviewed the literature for postoperative management options for facial lacerations. The authors came up with certain recommendations for the postoperative period, stating however that not all of them are based on randomized trials. These recommendations included applying Steri-Strips plus Mastisol until suture removal or preferably for few weeks to decrease the tension. They also recommended the use of topical antimicrobials for the first 2 days and encouraged showering after the first night. Sutures should be removed after 4–5 days of suturing.
1.2.5 Complications
Scars
An unsightly scar results from hypertrophic scarring, poor wound characteristics, or poor surgical technique. The patient should be consulted regarding the possibility of developing scars, in spite of meticulous surgical technique, before the repair process is pursued. Patients with tendencies to develop keloid have higher probability of such complications. Some topical agents can be used after removal of sutures to promote proper healing and achieve better cosmetic results with variable success rates. Scar revision can be done after complete healing of the wounds (6–12 months) via different surgical modalities.
Infection
Abundant blood supply to the face region decreases the incidence of infection. Therefore, routine use of topical or systemic antibiotics in facial wounds is not advised. In certain scenarios, including human and animal bites, severely contaminated wounds, and retained FBs, use of prophylactic antibiotics seems reasonable. Most of facial wound infections are, however, superficial and respond well to antibiotic therapy. Studies show that wound infection occurs maximally in the first 48 h after repair, though these results are not specific to facial lacerations.
1.3 Injury of Specialized Structures
1.3.1 Parotid Gland and Duct Injury
Although traumatic salivary gland injury is rare, the parotid gland and duct location makes it more prone to traumatic injury compared to other salivary glands. It occurs in around 0.21 % of trauma cases, being far more commonly associated with penetrating modes of trauma [13, 14]. Unfortunately, half of these injuries pass unnoticed during the initial evaluation and management, which results in the development of sialoceles and salivary fistulas [15].
1.3.1.1 Evaluation
The key to proper management of parotid gland and duct injuries is early recognition at the time of primary assessment. Detailed history of the mechanism and timing of injury is required. Whenever an injury to the parotid gland or duct is suspected, the patient should be asked about the timing of the last meal since a recent meal will result in increased salivation with pouring of saliva into the wound [16]. On examination, an injury to the parotid gland or duct should be suspected whenever the wound affects the region extending from the tragus of the ear to the upper lip (imaginary line). When suspicious, massaging of the gland region can express saliva from the injured region. In many cases, cannulation of the parotid duct orifice with injection of saline and/or methylene blue (MB) is required to confirm or exclude parotid duct injury. Care should be taken not to stain the surrounding tissue when using MB, making detection of facial nerve injury and its repair troublesome.
Penetrating injuries to the parotid gland and duct region are usually associated with injuries to surrounding structures including:
Facial nerve: Injury of the facial nerve is associated with 20 % of gland injuries and more than half of parotid duct injuries. Facial nerve assessment should therefore be done as part of the initial evaluation. The buccal branch is the most commonly affected one due to its intimate relation to the parotid duct [17].
External auditory canal (EAC): Otorrhagia should raise suspicion of EAC injury.
Temporomandibular joint (TMJ): Occlusion and jaw opening should be evaluated.
Vascular injury: Injury to the intraglandular vasculature can be troublesome. In such conditions, only proper compression should be applied until appropriate intraoperative evaluation and management is pursued. No blind attempts to control bleeding should be done for fear of facial nerve injury [18].
1.3.1.2 Treatment
Isolated Gland Injury
The wound should be properly cleansed. The gland capsule is simply sutured using absorbable sutures. Pressure dressing is used for 2 days to prevent development of sialoceles. Cannulation of the duct for 2 weeks maybe required to prevent obstruction of the salivary outflow due to associated edema. Close follow-up is required to recognize any complications as early as possible [19, 20].
Parotid Duct Injury
According to Van Sieckel’s classification [21], parotid duct injury of the intraglandular portion (site A) requires no repair; repairing the parotid duct capsule is sufficient in this location. Injury of the part overlying the masseter muscle (site B) is the most commonly affected portion and should be treated by direct anastomosis whenever possible. Injury to the portion distal to masseter muscle (site C) is optimally treated by direct anastomosis, but this is usually difficult, so oral reimplantation can be done in this situation.
Anastomosis is better done over a catheter introduced through the duct orifice. Injection of saline or MB facilitates recognition of the distal stump. The proximal stump is found through fine exploration of the wound. Massaging of the gland may aid the identification of the proximal stump through expression of saliva. At least 3 stitches with fine nylon sutures (9-0 or 10-0) are used to repair the duct. Alternatively, 7-0 or 8-0 silk sutures can be used. If a segment is lost, an autologous venous graft can be used for the repair [22]. Pressure dressing is required for 2 days, and the intraductal catheter should be left in place for 2 weeks postoperatively. Antisialogogues and antibiotics should be prescribed. Observation of the postoperative course is mandatory [18, 21].
In case of badly lacerated parotid duct, ligation of the proximal stump can be done aiming at atrophy of the parotid gland. This can be aided by the use of anticholinergic drugs. Alternatively, oral reimplantation of the proximal stump into the oral mucosa can be done [18].
1.3.1.3 Complications
Sialoceles
These result due to unrecognized injury to the parotid gland or duct or improperly treated injuries. They present as soft cystic swellings. Aspiration will confirm the diagnosis (amylase content can be done when doubtful and is diagnostic if >100,000 IU/L) [20]. If they develop few days following surgery, the wound should be re-explored and the underlying injury should be properly managed. On the other hand, if they develop as a delayed complication, repeated aspiration and pressure dressings are usually effective [14]. This can be aided by the use of anticholinergics to decrease salivary secretion. Some authors advocate nasogastric feeding to limit the stimuli for salivary secretion [16]. Intraglandular low-dose botulinum toxin injection can block the parasympathetic impulses and result in decreasing the salivary secretion [23, 24]. In resistant cases, parotidectomy can be performed [20]. Radiotherapy is now abandoned for fear of risk of malignancy.
Salivary Fistulas
They present as a communication with the skin surface pouring salivary secretions. They may follow spontaneous rupture of sialoceles. Again, if they are detected early postoperatively, the wound should be re-explored and properly managed. If delayed, compression dressing and anticholinergics are used [20]. Tympanic neurectomy aiming at destruction of tympanic nerve carrying parasympathetic supply to the gland is better not done due to its limited short-term success (probably due to reinnervation). Parotidectomy remains the last resort for resistant cases [25, 26].
1.3.2 Facial Nerve Injury
Facial nerve injuries can result from either blunt or penetrating trauma. An injury can occur at any part along the course of the nerve; thus, it can be classified according to the site of injury into five different types as follows [27]:
Type | Description |
|---|---|
I | Involves the portion inside the facial canal in the internal auditory canal (IAC) |
II | Involves the horizontal course of the facial nerve through the middle ear |
III | Involves the vertical course of the facial nerve through the mastoid |
IV | Involves the facial nerve through its course in the parotid tissue |
V | A combination of the above types of injuries |
1.3.2.1 Evaluation and Treatment
Facial nerve integrity should be evaluated in any patient presenting with craniofacial injury through exclusion of motor facial deficits. If facial nerve affection is present, grading of the injury is essential as it can help in estimating the magnitude of the injury and the probable recovery potential. The “House-Brackmann” grading system is the most commonly used for this purpose [28]. A computed tomography can help in delineating the site of injury in cases of temporal bone fractures. Electroneurography aids in the identification of the degree of injury and in follow-up. Deteriorating results warrant nerve exploration [29].
For intratemporal injuries, a simple mastoidectomy is done for approaching the injured site. Only decompression is required if the nerve is not severed. If the nerve is severed, mobilization may be required to attain tension-free repair.
Injuries distal to the stylomastoid foramen should be suspected in any deeply seated wound along the course of the nerve as in case of deep cheek lacerations. A motor deficit should promote meticulous nerve exploration with the target being primary repair. The utilization of nerve monitor and surgical microscope is greatly helpful in this situation. It is well established that injuries distal to a line connecting the lateral canthus and gonial notch of the mandible do not require repair due to the distal branching of the facial nerve [18]. Otherwise, more proximal injuries require primary repair. Identification of the cut ends is the first concern, sometimes requiring a classic superficial parotidectomy to identify and trace the branches.
Crushed ends should be carefully trimmed and approximated without tension. Two or three nonabsorbable 8-0–10-0 monofilament sutures are placed through the epineurium with the help of surgical microscope (although several debates exist regarding the time and technique of repair). Mobilization may be required to attain such tension-free repair. If such approximation is not feasible, cable nerve grafting is done using either the great auricular nerve or sural nerve. Inferior to direct anastomosis and nerve grafting are the nerve substitution techniques involving either a hypoglossal-facial or a cross-facial anastomosis [30].
Recovery of motor functions usually requires at least 6 months following the injury. However, extent of recovery and the duration required vary widely according to the extent of nerve affection, site of trauma, and the methodology of the repair process. A certain degree of synkinesis almost always results.
In case of failure of primary treatment, a variety of secondary facial reanimation techniques exist with variable success rates. These techniques include the nerve substitution techniques, dynamic muscle slings, or static procedures [29].
1.3.3 Ear Injuries
The cartilage should have the primary priority. Any exposed cartilage should be covered by skin to avoid secondary infection that may result in a painful chondritis, which is very difficult to treat. After debridement and suturing, if cartilage is still exposed, local postauricular or mastoid skin flaps can be used for cover. If the ear is totally avulsed, microsurgical reimplantation can be considered.
1.4 Fractures of Facial Bones
1.4.1 Surgical Anatomy
Anatomically, the MF region is divided into three zones as demonstrated in Fig. 1.4:
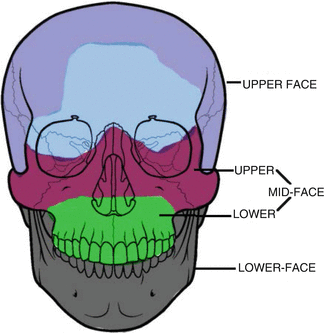

Fig. 1.4
The three anatomical zones of the maxillofacial (MF) region
1.
The upper face: Fractures involve the frontal bone and the frontal sinus.
2.
The middle face: This is again divided into upper and lower zones. The upper midface consists of the zygoma, nasal bones, ethmoid bone, and non-tooth-bearing segment of the maxilla. This is where maxillary Le Fort II and Le Fort III fractures occur. Also, it is where nasal bones, naso-ethmoidal complex (NEC), or zygomaticomaxillary complex (ZMC) and the orbital floor fractures occur. The lower midface includes the maxillary alveolus, teeth, and palate and is the site of Le Fort I fractures.
3.
The lower face: This is the site where mandibular fractures occur.
1.4.2 Nasal Fractures
Nasal fractures represent the most common type of facial fractures due to the prominence of the nose placing it at a higher risk of attaining trauma together with the relatively lower force required to cause such injury [31]. The nose shape and contour represent some of the main aesthetic aspects of the face. Also, nasal trauma can affect one of its functions related to air humidification, smell sensation, and respiration. Therefore, nasal fractures should be dealt with great care to restore both of its aesthetic and functional properties.
Nasal fractures can result from a variable cascade of injuries; sport injuries are of the most recognized causes especially in the adolescent population. Males attain nasal fractures twice as females as reported by several reports [32–34].
1.4.2.1 Assessment of Nasal Fractures
Detailed history regarding the mechanism of trauma should be taken to assess the possible extent of injury. Any accompanying manifestations including loss of consciousness, dizziness, or headache should be noted and dealt with carefully as they may reflect concussions with associated intracranial injuries. It should be noted that almost half of the assault injuries to the MF region are associated with high alcohol levels, which can lead to a variable degree of confusion. This, however, should not be assumed as the causative factor until both intracranial injury and hypoxia are excluded [5].
Inspection of the nasal region can reveal variable degrees of external deformity, the detection of which can be facilitated by examination through the different views (frontal, worm’s eye, bird’s eye views) (Fig. 1.5). However, such deformity can be obscured by the resulting edema. Palpation may reveal nasal or septal deviations; a step deformity or crepitus can also be felt. Good lighting and proper nasal speculum are required to detect the integrity of septal cartilage and bone together with the development of septal hematoma. If the physician is familiar with fiberoptic naso-endoscopy, it will be a valuable tool to assess the nasopharyngeal cavity and the posterior nasal complex. Epistaxis and cerebrospinal fluid (CSF) rhinorrhea can be present; the latter should raise suspicion of an associated skull base injury. Thorough examination of the whole facial region is required to rule out associated MF injuries with special focus on the naso-orbital-ethmoid varieties [35].
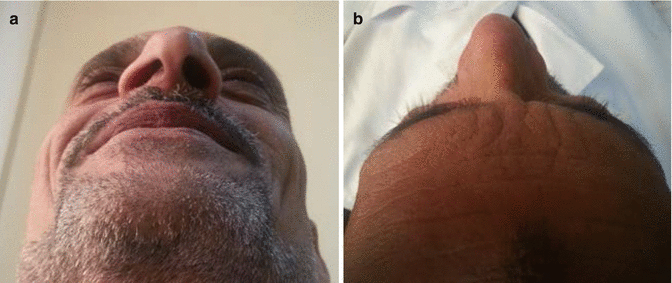

Fig. 1.5
(a) Worm’s eye view, (b) bird’s eye view for nasal deformity evaluation
Imaging
Although imaging is not required in all cases of nasal trauma and plain X-rays can be sufficient in isolated nasal injuries, CT scan represents a very informative tool in case of nasal fractures especially in the setting of suspected associated MF or intracranial injuries.
< div class='tao-gold-member'>
Only gold members can continue reading. Log In or Register to continue
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


