Chapter 55 Endoscopic Endonasal Approaches to the Skull Base and Paranasal Sinuses
 Videos corresponding to this chapter are available online at www.expertconsult.com.
Videos corresponding to this chapter are available online at www.expertconsult.com.
INTRODUCTION/BACKGROUND
Approaches to the skull base via the paranasal sinuses were introduced in the late 19th and early 20th century. Tumors of the sellar region were first approached through various incisions in the forehead to gain access to the sphenoid sinus via the ethmoid sinuses. Cushing introduced what became the standard for transsphenoidal surgery in 1910 when he first used a sublabial incision to gain access to the sinuses.1 coincidentally, on the exact same day, June 4, Oscar Hirsch used an endonasal approach to gain access to the sphenoid sinus. This would eventually replace the sublabial approach, but Cushing’s influence delayed this for decades.
This transsphenoidal approach to the sella turcica was conceptually unchanged for approximately 70 years. However, the operation and its outcomes were changed greatly during this period by advances in technology which provided improved visualization, intraoperative image-guidance and instrumentation. Dott, Guiot and Hardy added pneumoencephalocisternography, radiofluoroscopic guidance, and the operative microscope. All of this revolutionized the approach and improved outcomes. A similar change in technology began in the 1980s with the development of early intraoperative CT and MR image-guidance systems and the introduction of the endoscope by Carrau.2,3 At the same time, otolaryngologists were developing and refining functional endoscopic sinus surgery (FESS).4–9 It was the collaboration between otolaryngologists and neurosurgeons that led to the expansion of the standard transsphenoidal approach to include the rest of the anterior skull base and beyond.
EXPANDED ENDONASAL APPROACHES: ANATOMIC MODULES
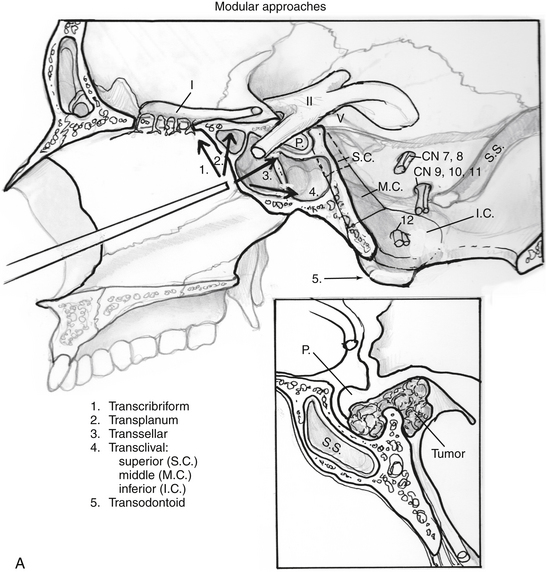
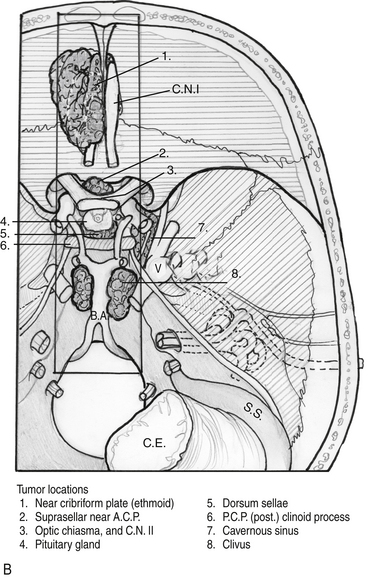
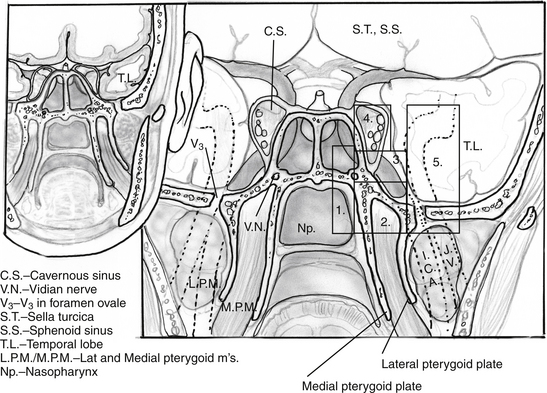
Endoscopic endonasal approaches (EEAs) can be divided into the sagittal or rostral-caudal plane (between the carotids) and coronal or paramedian plane (lateral to the carotid). The sagittal plane can be divided from rostral to caudal, anterior to posterior into the transfrontal, transcribriform, transplanum/transtuberculum, transsellar, transclival and transodontoid approaches (Fig. 55-1). The coronal plane is somewhat more complex in that the lateral expanded approaches vary based upon which fossa is involved (Fig. 55-2). The anterior fossa, lateral approaches consist of the supra- and transorbital approaches. The middle fossa is the most complex and is broken into five “transpterygoid” anatomic zones of approach: medial pterygoid (petrous apex), petroclival junction, quadrangular space or Meckel’s cave, superior cavernous sinus, and the infratemporal fossa (Fig. 55-3). These are all critically dependent upon their relationship with the internal carotid artery (ICA). Finally, the posterior fossa or inferior expanded approaches consist of the transcondylar and parapharyngeal space approaches.
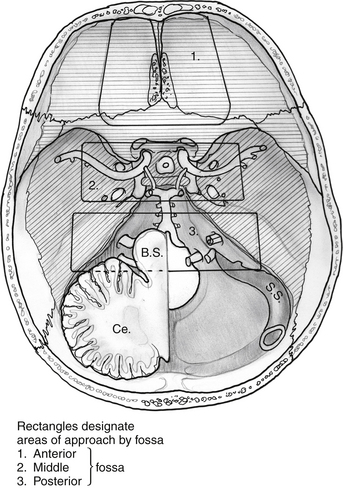
Figure 55-2 Superior view of skull base with general regions of approach by fossa. 1) anterior, 2) middle, 3) posterior.
Sagittal Plane
Transcribriform Approach
A complete sphenoethmoidectomy is performed on each side and the nasofrontal recesses are visualized. If needed, exophytic tumor within the nasal cavity can be debulked. The superior nasal septum is transected from the crista galli to the sphenoid rostrum as needed. As mentioned above, a transfrontal approach can be performed to establish an anterior margin. The transcribriform approach provides direct access to the vascular supply of tumors such as olfactory groove meningiomas, allowing early devascularization. The anterior and posterior ethmoidal arteries should be identified early and cauterized or clip ligated. The lateral bony margins are drilled to form “gutters” or osteotomies for the length of the tumor or planned resection as needed. If necessary, the lamina papyracea can be removed as well to allow retraction on the periorbita, thereby displacing the orbital contents for even more lateral access. In fact, the lateral access can extend all the way to the midorbital line at the level of the superior rectus muscle. After the lateral margins are drilled, the planum or tuberculum can be drilled as needed for a posterior margin. Even if necessary for tumor resection, it may be safest to leave the bone of the optic canals intact as long as possible. Finally, the dura is dissected from the crista galli to allow its removal. The remaining bone of the cribriform plate can now be dissected free (Fig. 55-4). If necessary for purely extradural lesions, the dura should be left intact. This may not be possible over the olfactory filaments, which can be cauterized to minimize CSF leakage, but should nonetheless undergo formal repair (see below). Obviously, olfaction (when present) is sacrificed if a bilateral approach is undertaken.
Intradural tumor resection must be performed with caution, especially when approaching the interhemispheric fissure, as there are frequently anterior cerebral artery branches or even the anterior communicating artery on the surface of the tumor (Fig. 55-5). An endonasal ultrasonic aspirator or two suctions can be used depending upon tumor consistency and proximity of involved structures. Microsurgical concepts of preserving arachnoid planes when possible and sharp dissection of critical structures is maintained throughout. All of this may require the use of angled scopes (45° or 70°).
Transplanum/Transtuberculum Approach
Also described as an “extended” approach, the transplanum approach was the first expansion of a traditional transsphenoidal approach.10–13 This approach provides a natural corridor for many suprasellar tumors such as craniopharyngiomas, tuberculum meningiomas and large pituitary adenomas. It may also be used for biopsy or resection of infundibular lesions such as metastases or hypophysitis. This approach is often an integral addition to transsellar and transcribriform approaches.
A transsphenoidal exposure (see transsellar approach below) is augmented by a posterior ethmoidectomy. The posterior ethmoidal arteries are a good landmark for anterior extent to preserve olfaction while providing adequate access. The optic canals are obviously critical to identify in order to avoid damage to the nerves. Whenever drilling over or near the optic canals, it is important to constantly irrigate to avoid heat transmission from the drill to the nerves. After the sella is exposed, the planum can be drilled and thinned. This can require an angled endoscope for adequate visualization depending upon the slope of the anterior skull base. Though somewhat counterintuitive, the planum is most easily removed in an anterior to posterior direction after the bone has been adequately thinned, exposing dura at the anterior extent and laterally. The lateral margins are actually the optic nerves which form the sides of a trapezoid which include the anterior planum and tuberculum sellae. Often there is no need to expose the optic nerves. However, in many tuberculum meningiomas, there is extension of disease into the medial optic canals (Fig. 55-6). This disease is not easily accessed via a craniotomy and requires release and retraction of an often already compromised optic nerve. In these cases, the bone overlying the tumor in the optic canal should be thinned (“blue-lined”) with a drill and carefully removed with a dissector.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree