Phacoantigenic/phacoanaphylactic uveitis is the result of an immunologic response from disruption of the lens capsule with subsequent release of lens proteins. The clinical diagnosis of phacoanaphylaxis, particularly in an eye with an intraocular lens implant, can be difficult, and on routine examination the condition may be indistinguishable from infectious endophthalmitis. Phacoantigenic uveitis is usually unilateral. The inflammation is predominantly anterior, with zonal granulomatous inflammation centered around the lens material. Traditionally, phacolytic uveitis refers to nongranulomatous inflammation resulting from lens proteins leaking through an intact lens capsule in an eye with a hypermature cataract. All of these entities may represent varying manifestations of a similar disease process and can all be considered lens-induced uveitis.
Etiology and Epidemiology
 It can occur after cataract surgery or trauma, and occasionally occurs spontaneously if there is a hypermature cataract with a leaking capsule.
It can occur after cataract surgery or trauma, and occasionally occurs spontaneously if there is a hypermature cataract with a leaking capsule.
 The immune system creates inflammation against previously sequestered lens proteins.
The immune system creates inflammation against previously sequestered lens proteins.
Symptoms
 Pain, redness, photophobia, and decreased vision
Pain, redness, photophobia, and decreased vision
Signs (Figs. 5-1 to 5-5)
 Circumciliary injection (ciliary flush)
Circumciliary injection (ciliary flush)
 Corneal edema
Corneal edema
 “Mutton fat” keratic precipitates
“Mutton fat” keratic precipitates
 Marked flare, abundant cells, lens matter in anterior chamber and/or a hypopyon
Marked flare, abundant cells, lens matter in anterior chamber and/or a hypopyon
 Posterior or peripheral anterior synechiae
Posterior or peripheral anterior synechiae
 A pupillary membrane
A pupillary membrane
 Irregular lens capsule, opaque lens, intense vitritis
Irregular lens capsule, opaque lens, intense vitritis
 Glaucoma due to trabeculitis, lens debris in angles or synechiae
Glaucoma due to trabeculitis, lens debris in angles or synechiae
 Hypotony due to cyclitic membranes, ciliary shutdown, or choroidal effusion
Hypotony due to cyclitic membranes, ciliary shutdown, or choroidal effusion
 Phthisis bulbi
Phthisis bulbi
Differential Diagnosis
 Phacolytic glaucoma
Phacolytic glaucoma
 Sympathetic ophthalmia (a bilateral disease)
Sympathetic ophthalmia (a bilateral disease)
 Low-grade endophthalmitis (e.g., Propionibacterium acnes)
Low-grade endophthalmitis (e.g., Propionibacterium acnes)
 Bacterial/fungal endophthalmitis
Bacterial/fungal endophthalmitis
Diagnostic Evaluation
 A high degree of clinical suspicion is important.
A high degree of clinical suspicion is important.
 An anterior chamber tap with histopathology may help differentiate lens-induced inflammation from infectious endophthalmitis.
An anterior chamber tap with histopathology may help differentiate lens-induced inflammation from infectious endophthalmitis.
 Histopathology may reveal zonal granulomatous inflammation.
Histopathology may reveal zonal granulomatous inflammation.
Treatment
 Definitive treatment involves removal of the inciting agent (i.e., the lens or residual lens matter).
Definitive treatment involves removal of the inciting agent (i.e., the lens or residual lens matter).
 Control of inflammation and glaucoma with corticosteroids and ocular antihypertensive medications is important in order to prevent long-term morbidity.
Control of inflammation and glaucoma with corticosteroids and ocular antihypertensive medications is important in order to prevent long-term morbidity.
Prognosis
 There is often a good outcome with prompt and aggressive management.
There is often a good outcome with prompt and aggressive management.
 If the lens is not promptly removed, complications such as glaucoma, hypotony, macular edema, or macular scarring can lead to visually significant morbidity.
If the lens is not promptly removed, complications such as glaucoma, hypotony, macular edema, or macular scarring can lead to visually significant morbidity.
REFERENCES
Kalogeropoulos CD, Malamou-Mitsi VD, Asproudis I, et al. The contribution of aqueous humor cytology in the differential diagnosis of anterior uvea inflammations. Ocul Immunol Inflamm. 2004;12(3):215–225.
Thach AB, Marak GE Jr, McLean IW, et al. Phacoanaphylactic endophthalmitis: a clinicopathologic review. Int Ophthalmol. 1991;15(4):271–279.
Figure 5-1. Slit-lamp photograph of a case of trauma-related phacoantigenic uveitis. Note the granulomatous keratic precipitates and ruptured anterior lens capsule with cortical material in the anterior chamber.
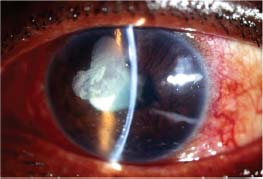
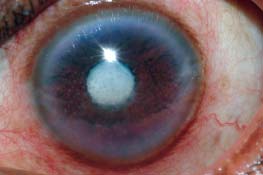
Figure 5-2. A 45-year-old woman presented with a 1-month history of pain, redness, and vision loss. She developed these symptoms shortly after blunt trauma to the eye. The fellow eye was normal. Slit-lamp photograph shows moderate anterior chamber inflammation, an intumescent cataract, and posterior synechia. (Courtesy of S. R. Rathinam, MD.)
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


