Anterior uveitis constitutes up to 75% of all cases of uveitis and human leucocyte antigen (HLA)-B27–associated uveitis is the most commonly diagnosed cause of acute anterior uveitis. This haplotype is frequently associated with systemic diseases such as ankylosing spondylitis, inflammatory bowel disease, reactive arthritis, psoriatic arthritis, and undifferentiated spondyloarthropathies. This group of diseases is also referred to as seronegative spondyloarthropathies (“seronegative” meaning negative rheumatoid factor, and “spondylo” meaning spine).
Etiology and Epidemiology
 Genetic, geographic, and environmental factors are involved.
Genetic, geographic, and environmental factors are involved.
 The prevalence of HLA-B27 is 5% to 8% in Western populations. HLA-B27 is less frequent in nonwhite populations.
The prevalence of HLA-B27 is 5% to 8% in Western populations. HLA-B27 is less frequent in nonwhite populations.
 The lifetime cumulative incidence of acute anterior uveitis is 0.2% in the general population, but increases to 1% in the HLA-B27–positive population.
The lifetime cumulative incidence of acute anterior uveitis is 0.2% in the general population, but increases to 1% in the HLA-B27–positive population.
 Depending upon the population studied, the HLA-B27 haplotype accounts for 40% to 70% of cases of acute anterior uveitis.
Depending upon the population studied, the HLA-B27 haplotype accounts for 40% to 70% of cases of acute anterior uveitis.
 More than half of the patients with an HLA-B27–associated acute anterior uveitis present with an associated systemic disease.
More than half of the patients with an HLA-B27–associated acute anterior uveitis present with an associated systemic disease.
 HLA-B27–associated uveitis has been thought to be more common in males than in females, but recent work has called this into question.
HLA-B27–associated uveitis has been thought to be more common in males than in females, but recent work has called this into question.
 It more commonly occurs in younger people.
It more commonly occurs in younger people.
 The risk of developing spondyloarthritis or uveitis in a B27-positive patient is 25%.
The risk of developing spondyloarthritis or uveitis in a B27-positive patient is 25%.
 In patients with spondyloarthropathy, the prevalence of uveitis is as high as 32.7%.
In patients with spondyloarthropathy, the prevalence of uveitis is as high as 32.7%.
Symptoms
 Sudden onset of redness, pain, photophobia, and blurred vision.
Sudden onset of redness, pain, photophobia, and blurred vision.
 Associated systemic complaints may include low back pain, arthritis, psoriasis, oral ulcers, chronic diarrhea, and urethritis.
Associated systemic complaints may include low back pain, arthritis, psoriasis, oral ulcers, chronic diarrhea, and urethritis.
Signs
 Most commonly, patients have acute and/or recurrent episodes of uveitis, usually lasting several days to weeks. However, it may be chronic in 25% of cases.
Most commonly, patients have acute and/or recurrent episodes of uveitis, usually lasting several days to weeks. However, it may be chronic in 25% of cases.
 Rarely are both eyes simultaneously inflamed.
Rarely are both eyes simultaneously inflamed.
 Fine keratic precipitates (KPs) and endothelial dusting occur, but the uveitis is always nongranulomatous.
Fine keratic precipitates (KPs) and endothelial dusting occur, but the uveitis is always nongranulomatous.
 Severe anterior chamber reaction with fibrin can occur, and a hypopyon is common and is associated with disease severity (Figs. 4-1 and 4-2).
Severe anterior chamber reaction with fibrin can occur, and a hypopyon is common and is associated with disease severity (Figs. 4-1 and 4-2).
 A fibrin net may form across the pupillary margin.
A fibrin net may form across the pupillary margin.
 Posterior synechiae are frequently present.
Posterior synechiae are frequently present.
 Posterior segment involvement is underrecognized, even though vitritis, vasculitis, papillitis, and macular edema may occur, especially in chronic, undertreated cases.
Posterior segment involvement is underrecognized, even though vitritis, vasculitis, papillitis, and macular edema may occur, especially in chronic, undertreated cases.
SERONEGATIVE SPONDYLOARTHROPATHIES (Figs. 4-3 to 4-7)
 Ankylosing spondylitis is a chronic arthritis that mainly affects the spine and sacroiliac joints.
Ankylosing spondylitis is a chronic arthritis that mainly affects the spine and sacroiliac joints.
 The major symptoms are lower back pain and stiffness.
The major symptoms are lower back pain and stiffness.
 90% of patients are HLA-B27–positive.
90% of patients are HLA-B27–positive.
 Uveitis may be the first manifestation of the disease and may occur prior to onset of joint pain.
Uveitis may be the first manifestation of the disease and may occur prior to onset of joint pain.
 Nonsteroidal anti-inflammatory medications and physical therapy are the mainstays of treatment. Methotrexate and anti-TNF agents have also been successfully used.
Nonsteroidal anti-inflammatory medications and physical therapy are the mainstays of treatment. Methotrexate and anti-TNF agents have also been successfully used.
 Reactive arthritis syndrome (Reiter’s syndrome)
Reactive arthritis syndrome (Reiter’s syndrome)
 The classic triad is papillary conjunctivitis, urethritis, and polyarthritis (“can’t see, can’t pee, can’t climb a tree”). However, these symptoms may be mild or absent.
The classic triad is papillary conjunctivitis, urethritis, and polyarthritis (“can’t see, can’t pee, can’t climb a tree”). However, these symptoms may be mild or absent.
 Anterior uveitis is usually less common (10% of cases).
Anterior uveitis is usually less common (10% of cases).
 Most of the patients are young male adults.
Most of the patients are young male adults.
 The HLA-B27 positivity rate is 60%.
The HLA-B27 positivity rate is 60%.
 Bacteria such as Chlamydia, Salmonella, Yersinia, and Shigella have been associated with the disease, and may trigger the disease in a susceptible patient, however their role remains controversial.
Bacteria such as Chlamydia, Salmonella, Yersinia, and Shigella have been associated with the disease, and may trigger the disease in a susceptible patient, however their role remains controversial.
 Keratoderma blennorrhagicum (scaling skin), circinate balanitis (rash around the penis), aphthous stomatitis, plantar fasciitis, and uncommonly iritis are additional diagnostic criteria.
Keratoderma blennorrhagicum (scaling skin), circinate balanitis (rash around the penis), aphthous stomatitis, plantar fasciitis, and uncommonly iritis are additional diagnostic criteria.
 Inflammatory bowel disease (IBD)
Inflammatory bowel disease (IBD)
 Ulcerative colitis and Crohn’s disease are the main diagnostic entities.
Ulcerative colitis and Crohn’s disease are the main diagnostic entities.
 The risk of developing uveitis is up to five times higher in patients with ulcerative colitis than those with Crohn’s disease.
The risk of developing uveitis is up to five times higher in patients with ulcerative colitis than those with Crohn’s disease.
 Patients with IBD who develop uveitis may develop sacroiliitis and are HLA-B27 positive in 60% of cases.
Patients with IBD who develop uveitis may develop sacroiliitis and are HLA-B27 positive in 60% of cases.
 Patients may also have erythema nodosum and pyoderma gangrenosum.
Patients may also have erythema nodosum and pyoderma gangrenosum.
 Behçet’s disease and Whipple’s disease are the main differential diagnoses to consider.
Behçet’s disease and Whipple’s disease are the main differential diagnoses to consider.
 Psoriatic arthritis
Psoriatic arthritis
 One-fifth of patients with psoriatic arthritis may develop sacroiliitis.
One-fifth of patients with psoriatic arthritis may develop sacroiliitis.
 Patients present with cutaneous, joint, and ungual involvement.
Patients present with cutaneous, joint, and ungual involvement.
 The typical skin lesions are elevated, well-circumscribed plaques.
The typical skin lesions are elevated, well-circumscribed plaques.
 Patients may have central arthritis affecting the spine, or distal arthritis affecting the fingers. In advanced cases, patients may have “sausage digit deformity.”
Patients may have central arthritis affecting the spine, or distal arthritis affecting the fingers. In advanced cases, patients may have “sausage digit deformity.”
 Nail changes include nail pitting, ridging, and discoloration can occur.
Nail changes include nail pitting, ridging, and discoloration can occur.
 The rate of uveitis in patients with psoriatic arthritis is 25%.
The rate of uveitis in patients with psoriatic arthritis is 25%.
 Uveitis in this subgroup of patients has some specific characteristics such as bilaterality, chronicity, and severity.
Uveitis in this subgroup of patients has some specific characteristics such as bilaterality, chronicity, and severity.
 Posterior segment involvement (CME, retinal vasculitis, and papillitis) is not uncommon.
Posterior segment involvement (CME, retinal vasculitis, and papillitis) is not uncommon.
 Undifferentiated spondyloarthropathies
Undifferentiated spondyloarthropathies
 There is an HLA-B27 positivity rate of 25%, and uveitis occurs somewhat less frequently in this group.
There is an HLA-B27 positivity rate of 25%, and uveitis occurs somewhat less frequently in this group.
Differential Diagnosis
 Idiopathic anterior uveitis
Idiopathic anterior uveitis
 Sarcoidosis
Sarcoidosis
 Other nongranulomatous uveitis
Other nongranulomatous uveitis
 Behçet’s disease–associated uveitis
Behçet’s disease–associated uveitis
 Infectious uveitis (herpetic uveitis, syphilis, Lyme disease, Whipple’s disease, or infectious endophthalmitis)
Infectious uveitis (herpetic uveitis, syphilis, Lyme disease, Whipple’s disease, or infectious endophthalmitis)
 Drug-induced uveitis: rifabutin, biphosphonates, prostaglandin analogues, and cidofovir
Drug-induced uveitis: rifabutin, biphosphonates, prostaglandin analogues, and cidofovir
 Tubulointerstitial nephritis and uveitis (TINU)
Tubulointerstitial nephritis and uveitis (TINU)
 Lens-induced uveitis
Lens-induced uveitis
 Masquerade syndromes (retinoblastoma and metastatic tumors)
Masquerade syndromes (retinoblastoma and metastatic tumors)
Diagnostic Evaluation
 HLA-B27 typing
HLA-B27 typing
 ESR, C-reactive protein
ESR, C-reactive protein
 Work-up to rule out items on the differential diagnosis, including serum angiotensin-converting enzyme (ACE), chest radiograph, Lyme titer, VDRL/RPR/FTA-Abs, tuberculin skin test
Work-up to rule out items on the differential diagnosis, including serum angiotensin-converting enzyme (ACE), chest radiograph, Lyme titer, VDRL/RPR/FTA-Abs, tuberculin skin test
 If indicated:
If indicated:
 MRI of the sacroiliac joint and lumbar spine
MRI of the sacroiliac joint and lumbar spine
 Swab for chlamydia, Shigella, Yersinia, and other gram-negative bacteria.
Swab for chlamydia, Shigella, Yersinia, and other gram-negative bacteria.
 Specialized consultations: rheumatology, gastrointestinal, dermatology, and infectious disease
Specialized consultations: rheumatology, gastrointestinal, dermatology, and infectious disease
Treatment
 Cycloplegic and mydriatic drops will relieve pain and break posterior synechiae.
Cycloplegic and mydriatic drops will relieve pain and break posterior synechiae.
 Topical corticosteroids are the mainstay of treatment for ocular disease and usually need to be administered every hour for the first 48 hours, then slowly tapered.
Topical corticosteroids are the mainstay of treatment for ocular disease and usually need to be administered every hour for the first 48 hours, then slowly tapered.
 If the uveitis is severe, subconjunctival injections of dexamethasone can be considered daily for 3 consecutive days. Sub-Tenon’s triamcinolone injection can also be used.
If the uveitis is severe, subconjunctival injections of dexamethasone can be considered daily for 3 consecutive days. Sub-Tenon’s triamcinolone injection can also be used.
 If there is no improvement on topical/periocular steroids, systemic corticosteroids and/or systemic immunosuppressive agents may be proposed.
If there is no improvement on topical/periocular steroids, systemic corticosteroids and/or systemic immunosuppressive agents may be proposed.
 Systemic NSAIDs may decrease the recurrence rate as well as exposure to corticosteroids.
Systemic NSAIDs may decrease the recurrence rate as well as exposure to corticosteroids.
 Anti-TNF-α treatment may be useful in treatment-resistant and/or sight-threatening cases.
Anti-TNF-α treatment may be useful in treatment-resistant and/or sight-threatening cases.
 Prophylactic treatment using sulfasalazine remains controversial.
Prophylactic treatment using sulfasalazine remains controversial.
Prognosis
 Generally favorable with aggressive therapy
Generally favorable with aggressive therapy
 Uveitis often recurs and may become chronic. Presence of chronic inflammation is the main prognostic factor.
Uveitis often recurs and may become chronic. Presence of chronic inflammation is the main prognostic factor.
 Posterior iris synechiae, band keratopathy, posterior subcapsular cataract, ocular hypertension, hypotony, cystoid macular edema, and epiretinal membrane formation are the major complications.
Posterior iris synechiae, band keratopathy, posterior subcapsular cataract, ocular hypertension, hypotony, cystoid macular edema, and epiretinal membrane formation are the major complications.
REFERENCES
Braun J, Baraliakos X, Listing J, et al. Decreased incidence of anterior uveitis in patients with ankylosing spondylitis treated with the anti-tumor necrosis factor agents infliximab and etanercept. Arthritis Rheum. 2005;52(8):2447–2451.
Chang JH, McCluskey PJ, Wakefield D. Acute anterior uveitis and HLA-B27. Surv Ophthalmol. 2005;50:364–388.
Durrani K, Foster CS. Psoriatic uveitis: a distinct clinical entity? Am J Ophthalmol. 2005;139:106–111.
Loh AR, Acharya NR. Incidence rates and risk factors for ocular complications and vision loss in HLA-B27-associated uveitis. Am J Ophthalmol. 2010;150: 534–542.
Zamecki KJ, Jabs DA. HLA typing in uveitis: use and misuse. Am J Ophthalmol. 2010;149(2):189–193.
Zeboulon N, Dougados M, Gossec L. Prevalence and characteristics of uveitis in the spondyloarthropathies: a systematic literature review. Ann Rheum Dis. 2008;67:955–959.
Figure 4-1. A. Slit-lamp photograph shows severe acute anterior uveitis with fibrin in the anterior chamber and 360 degrees of posterior synechiae in a patient with reactive arthritis. B. Remission occurred with maximal topical corticosteroids, cycloplegic and subconjunctival injection of dexamethasone each day for 3 days.
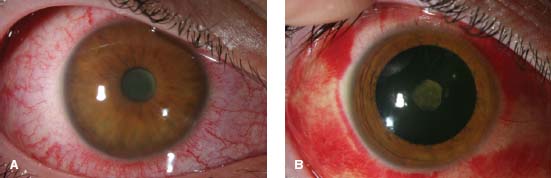
Figure 4-2. Slit-lamp photograph showing acute anterior uveitis with fibrin in the anterior chamber and a hypopyon in a patient who is HLA-B27 positive with ankylosing spondylitis.
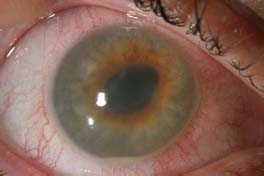
Figure 4-3. Right ankle arthritis in a patient with ankylosing spondylitis.
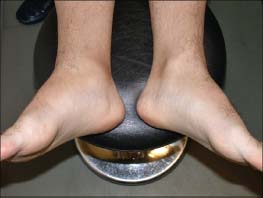
Figure 4-4. Sausage toes of the right foot in a case of seronegative spondyloarthritis. (Courtesy of P. Quartier.)
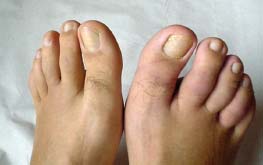
Figure 4-5. Pelvis radiograph shows irregular margins and sclerosis of the sacroiliac joints. (Courtesy of P. Quartier.)
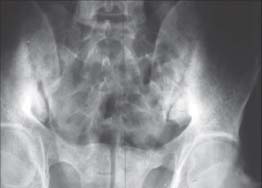
Figure 4-6. A. Lateral lumbar spine radiograph demonstrating a syndesmophyte. (Courtesy of P. Quartier.) B. This person has vertical syndesmophytes on multiple vertebrae causing a “bamboo spine.” (Courtesy of V. Vuillemin.)
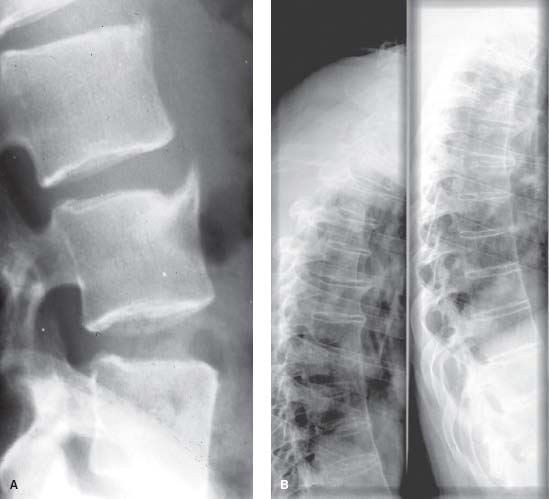
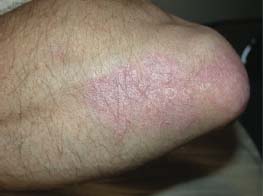
Figure 4-7. Plaque psoriasis on the elbow of a patient with HLA-B27–associated uveitis and psoriatic arthritis.
POSNER-SCHLOSSMAN SYNDROME
Bahram Bodaghi
The Posner-Schlossman syndrome (PSS), also known as recurrent glaucomatocyclitic crisis syndrome, is an unusual clinical entity that occurs in young to middle-aged adults. Initially considered an immune-mediated condition, it may be due to a viral infection.
Epidemiology
 It predominantly occurs in young to middle-aged patients but it may also be diagnosed in the elderly.
It predominantly occurs in young to middle-aged patients but it may also be diagnosed in the elderly.
 There seems to be a clear male preponderance.
There seems to be a clear male preponderance.
 The disease remains rare but must be considered in all cases of unilateral uveitis associated with high intraocular pressure (IOP).
The disease remains rare but must be considered in all cases of unilateral uveitis associated with high intraocular pressure (IOP).
Etiology
 Since its initial description in 1948, there has been much speculation regarding its pathogenesis. Despite lack of evidence, developmental abnormalities of the angle, allergic factors, primary vascular abnormalities, sympathetic nervous system defects, and inflammatory mechanisms have all been proposed as possible mechanisms for this disorder.
Since its initial description in 1948, there has been much speculation regarding its pathogenesis. Despite lack of evidence, developmental abnormalities of the angle, allergic factors, primary vascular abnormalities, sympathetic nervous system defects, and inflammatory mechanisms have all been proposed as possible mechanisms for this disorder.
 Recent data based on specific intraocular antibody production and molecular biology suggest cytomegalovirus infection as the inciting agent in PSS.
Recent data based on specific intraocular antibody production and molecular biology suggest cytomegalovirus infection as the inciting agent in PSS.
Symptoms
 Patients present with moderate blurred vision, often due to mild corneal edema secondary to an acute rise in IOP.
Patients present with moderate blurred vision, often due to mild corneal edema secondary to an acute rise in IOP.
 It is almost always unilateral with recurrent attacks in the same eye.
It is almost always unilateral with recurrent attacks in the same eye.
 Patients may experience very mild pain or discomfort.
Patients may experience very mild pain or discomfort.
Signs
 Mild decrease in vision
Mild decrease in vision
 Dilated conjunctival vessels
Dilated conjunctival vessels
 White keratic precipitates of different sizes predominantly located at the central cornea (Fig. 4-8)
White keratic precipitates of different sizes predominantly located at the central cornea (Fig. 4-8)
 Minimal aqueous flare without cells
Minimal aqueous flare without cells
 Posterior synechiae are not present.
Posterior synechiae are not present.
 The IOP is markedly elevated, ranging from 40 to 60 mm Hg.
The IOP is markedly elevated, ranging from 40 to 60 mm Hg.
 The angle is open, although anterior synechiae may be present.
The angle is open, although anterior synechiae may be present.
 There is usually no iris heterochromia.
There is usually no iris heterochromia.
 Vitritis is absent and there is no posterior segment involvement.
Vitritis is absent and there is no posterior segment involvement.
 Between the attacks, the examination is unremarkable (with the exception of glaucomatous optic atrophy).
Between the attacks, the examination is unremarkable (with the exception of glaucomatous optic atrophy).
Differential Diagnosis
 CMV-induced anterior uveitis
CMV-induced anterior uveitis
 Herpetic anterior uveitis
Herpetic anterior uveitis
 Atypical cases of Fuchs’ iridocyclitis
Atypical cases of Fuchs’ iridocyclitis
 Nonspecific hypertensive iridocyclitis
Nonspecific hypertensive iridocyclitis
 Sarcoidosis
Sarcoidosis
 Tuberculosis
Tuberculosis
 Multiple sclerosis
Multiple sclerosis
Diagnostic Evaluation
 An anterior chamber tap may be performed for viral PCR and analysis of specific antibody production, confirming the presence of CMV.
An anterior chamber tap may be performed for viral PCR and analysis of specific antibody production, confirming the presence of CMV.
 Visual field testing and/or retinal nerve fiber layer analysis can be used to identify glaucomatous visual field abnormalities that may occur in severe or recurrent forms of the disease.
Visual field testing and/or retinal nerve fiber layer analysis can be used to identify glaucomatous visual field abnormalities that may occur in severe or recurrent forms of the disease.
 Ancillary tests to exclude other causes of unilateral uveitis and secondary glaucoma should be performed as clinically indicated.
Ancillary tests to exclude other causes of unilateral uveitis and secondary glaucoma should be performed as clinically indicated.
Treatment
 Treatment to lower the IOP is usually required during attacks in order to protect the optic disc.
Treatment to lower the IOP is usually required during attacks in order to protect the optic disc.
 Before the identification of PSS as a viral disorder, many authors found the use of short-term topical corticosteroids useful.
Before the identification of PSS as a viral disorder, many authors found the use of short-term topical corticosteroids useful.
 In CMV-associated PSS, specific antiviral therapy with topical or systemic drugs may be initiated.
In CMV-associated PSS, specific antiviral therapy with topical or systemic drugs may be initiated.
 The duration of antiviral therapy depends on the clinical presentation and the severity of visual field alteration. In severe cases with high clinical suspicion, a 2- to 3-month regimen may be considered.
The duration of antiviral therapy depends on the clinical presentation and the severity of visual field alteration. In severe cases with high clinical suspicion, a 2- to 3-month regimen may be considered.
 Cycloplegic agents are not required.
Cycloplegic agents are not required.
 Filtering surgery is usually not recommended but may be successfully used to treat glaucoma that progresses despite maximum medical therapy.
Filtering surgery is usually not recommended but may be successfully used to treat glaucoma that progresses despite maximum medical therapy.
Prognosis
 Generally speaking, recurrences decrease with increasing age, so the visual prognosis is usually good.
Generally speaking, recurrences decrease with increasing age, so the visual prognosis is usually good.
 However, in the absence of specific ocular antihypertensive medications or surgery, permanent visual loss may occur in approximately 25% of cases due to chronic ocular hypertension.
However, in the absence of specific ocular antihypertensive medications or surgery, permanent visual loss may occur in approximately 25% of cases due to chronic ocular hypertension.
REFERENCES
Bloch-Michel E, Dussaix E, Cerqueti P, et al. Possible role of cytomegalovirus in the etiology of Posner-Schlossman syndrome. Int Ophthalmol. 1987;11:95–96.
Chee SP, Bacsal K, Jap A, et al. Clinical features of cytomegalovirus anterior uveitis in immunocompetent patients. Am J Ophthalmol. 2008;145(5):834–840.
Posner A, Schlossman A. Treatment of glaucoma associated with iridocyclitis. JAMA. 1949; 139:82–86.
Teoh SB, Thean L, Koay E. Cytomegalovirus in aetiology of Posner-Schlossman syndrome: evidence from quantitative polymerase chain reaction. Eye (Lond). 2005;19(12):1338–1340.
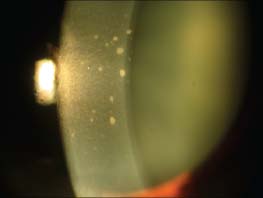
Figure 4-8. Typical white keratic precipitates that are most concentrated in the central cornea in a case of CMV-induced Posner-Schlossman syndrome.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


