Trigeminal Nerve
Eric E. Kraus
Craig H. Smith
ANATOMY
GASSERIAN GANGLION AND BRAINSTEM NUCLEI
The trigeminal nerve contains both a sensory and a motor root. The cell bodies of the sensory portion lie in the gasserian (or semilunar) ganglion, with the exception of those for muscle spindle information, which lie in the mesencephalic nucleus in the midbrain. The gasserian ganglion is located in Meckel’s cave near the petrous tip of the temporal bone just behind the internal carotid and the posterior portion of the cavernous sinus. Proximally, the sensory root extends to the pons, where the fibers enter the main sensory nucleus, the nucleus of the spinal tract, and the mesencephalic nucleus (Figs. 1 and 2). The classic teaching that the nucleus of the spinal tract mediates pain and temperature sensation while the main sensory nucleus mediates fine touch is probably an oversimplification; still, the functional organization of the nuclei is not well understood.1
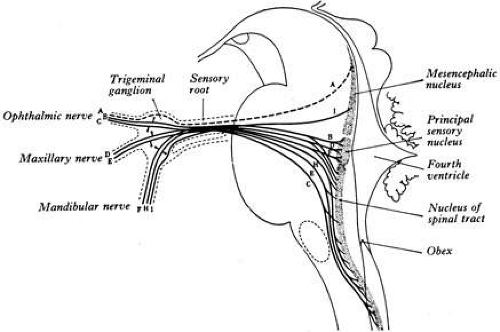 FIG. 1. Trigeminal nuclei and ganglion. (From Warwick R, Williams PL: Gray’s Anatomy, 35th ed. Edinburgh: Churchill Livingstone, 1973:1001.) |
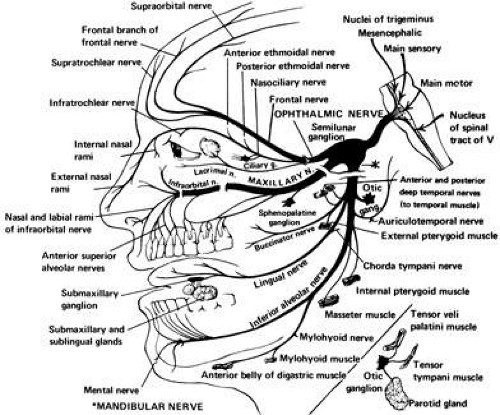 FIG. 2. Branches of the trigeminal nerve. (From Chusid JG: Correlative Neuroanatomy and Functional Neurology. Los Altos, CA: Lange Medical Publishers, 1976:92.) |
The mesencephalic nucleus has special distinction because it is the only example in which sensory cell bodies lie within the central nervous system, rather than outside in a sensory ganglion. A collateral branch synapses directly on the motor nucleus of the trigeminal nerve, mediating a monosynaptic reflex for the jaw jerk.
Most of the fibers from the main sensory and spinal tract nuclei cross to the contralateral side and, in a situation analogous to the sensory fibers coming from the spinal cord, travel in the medial lemniscus and trigeminothalamic tract to the ventral posterior nucleus of the thalamus. From there, information is projected to the postcentral gyrus of the parietal lobe. Muscle spindle information from the mesencephalic nucleus projects to the cerebellum.
The motor nucleus of the trigeminal nerve is located in the midpons, and its fibers pass beneath the gasserian ganglion to join the mandibular branch of the fifth nerve to supply the muscles of mastication.
The three sensory divisions of the trigeminal nerve are the ophthalmic (V1), maxillary (V2), and mandibular (V3) (see Fig. 2; Fig. 3). Although autonomic fibers do not originate from the trigeminal nerve, parasympathetic fibers from cranial nerves three (oculomotor), seven (facial), and nine (glossopharyngeal), and sympathetic fibers from cervical ganglia, travel with the widely distributed trigeminal nerve to reach their destination.
Ophthalmic Division
The ophthalmic branch occupies the lateral wall of the cavernous sinus and divides into the lacrimal, nasociliary, and frontal nerves (see Fig. 2; Fig. 4). These branches pass through the superior orbital fissure to enter the orbit.
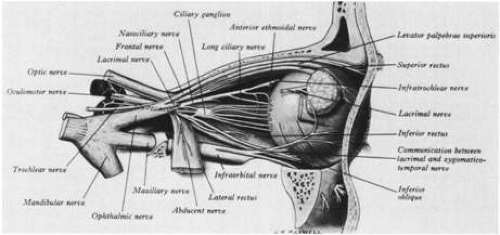 FIG. 4. Nerve supply to the right globe. (From Warwick R, Williams PL: Gray’s Anatomy, 35th ed. Edinburgh: Churchill Livingstone, 1973:1003.) |
The lacrimal nerve supplies the conjunctiva and the skin of the lateral portion of the upper lid. It also receives postganglionic, parasympathetic facial nerve fibers from the sphenopalatine ganglion, which it transmits to the lacrimal gland.
The long ciliary nerves and the sensory root of the ciliary ganglion are the sole sensory supply to the eye and are branches of the nasociliary nerve. The sensory root traverses (but does not synapse) the ganglion and leaves as short ciliary nerves. Both long and short ciliary nerves transmit somatic sensory information from the iris, cornea, and ciliary muscle. Postganglionic sympathetic fibers from the superior sympathetic ganglion in the neck travel the internal carotid plexus to reach the iris dilators and ciliary muscle by way of the long and short ciliary nerves. Preganglionic parasympathetic fibers from the Edinger-Westphal nucleus travel with the oculomotor nerve to the ciliary ganglion where they synapse. Postganglionic parasympathetic fibers reach the iris constrictors and ciliary muscle by way of short ciliary nerves.
The cornea is supplied by 60 to 80 nerves that course radially from the limbus and branch into over 1,000 small axons that terminate as free nerve endings in the stroma and epithelium.
The nasociliary nerve also forms the anterior and posterior ethmoidal nerves and the infratrochlear nerve, which innervate the sphenoid and posterior ethmoid sinuses, the upper eyelid, the caruncle, the canaliculi and lacrimal sac, the mucosa of the nasal septum and inferior and middle turbinates, and the tip and side of the nose. Sympathetic fibers to Müller’s muscle of the upper lid also travel this route.
The frontal nerve divides into the supraorbital and supratrochlear nerves, which innervate the medial portion of the upper eyelid, forehead, scalp, frontal sinus, and bridge of the nose.
Maxillary Division
The maxillary division runs inferiorly in the cavernous sinus, passes through the foramen rotundum to the pterygopalatine (sphenopalatine) fossa, and becomes the infraorbital nerve as it enters the orbit through the infraorbital fissure. Branches of the maxillary nerve include the sphenopalatine, posterosuperior alveolar, and zygomatic nerves. The infraorbital nerve continues along the orbital floor in the infraorbital canal to the infraorbital foramen, where it divides into inferior palpebral, lateral nasal, and superior labial nerves.
The maxillary division supplies sensation to the nasopharynx, maxillary sinus, roof of the mouth, soft palate, upper teeth, and an area of the face that extends from the upper lip to the side of the nose, then to the lower eyelid, and then to the zygoma. In addition, the maxillary division receives lacrimal postganglionic parasympathetic fibers from the sphenopalatine ganglion, which it delivers to the lacrimal nerve of the ophthalmic division.
Mandibular Division
The mandibular nerve does not reach the cavernous sinus like the other two divisions; rather, it passes out of Meckel’s cave through the foramen ovale. The auriculotemporal, buccinator, lingual, and inferior alveolar nerves provide sensation to the lateral scalp, posterior cheek and temporal areas, temporomandibular joint, anterior pinna, upper and outer walls of the external auditory canal, anterior half of the tympanum, lower lip and gums, chin, anterior two-thirds of the tongue, floor of the mouth, lower teeth, and lower half of the buccal surface.
Motor fibers innervate eight muscles: tensor tympani, tensor palati, lateral pterygoid, medial pterygoid, temporalis, masseter, mylohyoid, and anterior belly of the digastric.
Postganglionic parasympathetic glossopharyngeal nerve fibers from the otic ganglion travel with the auriculotemporal nerve to the parotid gland. The chorda tympani of the facial nerve attaches to the lingual nerve and transmits preganglionic parasympathetic fibers to the submandibular ganglion and taste sensation from the anterior two-thirds of the tongue.
Intracranial Innervation
All three divisions of the trigeminal nerve have intracranial branches that supply most of the pain sensitive structures above the tentorium cerebelli. Of the three, the ophthalmic division supplies the greatest area. These structures include the basal dura mater, the dural venous sinuses, and the cerebral blood vessels at the base of the brain.2,3,4 Pain can be referred to the eye or face from any of these structures.
PHYSIOLOGY
OCULAR SENSATION
Because of its high concentration of free nerve endings, the cornea is one of the most sensitive pain structures in the body. Sensitivity to pain is greatest in the center of the cornea and decreases toward the limbus. Pain receptors are also found in the extraocular muscles, conjunctiva, uvea, sclera, and optic nerve sheaths. The retina, optic nerve, and lens, however, are devoid of pain sensitivity.1
TRIGEMINAL REFLEXES
Several trigeminal reflexes are of clinical importance. It has been known for many years that pressure, or manipulation of, the ocular structures will cause bradycardia. This is usually called the oculocardiac reflex and is responsible for the bradycardia and other arrhythmias seen in ocular surgery, in particular, strabismus surgery.5 The oculocardiac reflex, however, is only a portion of the broader trigeminocardiac reflex in which the afferent limb of the reflex is by way of a branch of the trigeminal nerve, and the efferent limb is by way of the vagus nerve.6,7 Vagal stimulation on the heart causes slowing and, rarely, asystole.
Other reflexes involving the trigeminal nerve include the jaw jerk, snout reflex, and sneeze reflex. Corneal stimulation can produce the corneolacrimal (reflex tearing), corneomandibular, and corneooculogyric reflexes.8 Nausea and vomiting may occur during an acute attack of glaucoma or certain intraorbital inflammatory processes.
CLINICAL ASSESSMENT
SENSORY FUNCTIONS
Corneal sensitivity is tested by the light touch of a cotton-tipped applicator drawn to a fine point. If local cornea disease is present, each quadrant should be assessed separately, because it may be only a portion of the cornea that is denervated; otherwise, it is sufficient to test just the inferior cornea. The response to corneal stimulation is assessed both subjectively through the patient’s report and objectively by observation of the corneal reflex.
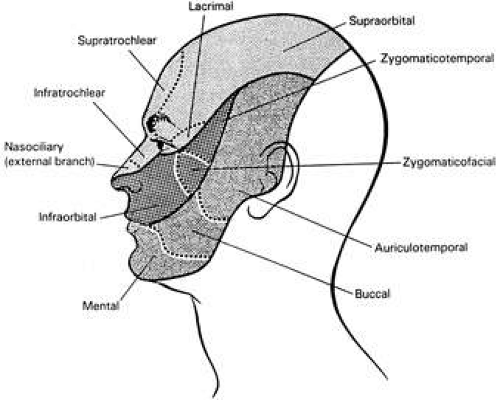
Cutaneous sensation is assessed as it is elsewhere in the body by testing light touch with cotton and pain with pin prick. The dermatomes of each of the three divisions of the trigeminal nerve should be tested separately (see Fig. 3). Temperature, vibration, stereognosis, and two-point discrimination can also be demonstrated, but this is usually an unnecessary procedure.
MOTOR FUNCTIONS
The motor root of the trigeminal nerve is assessed by palpating the temporal and masseter muscles as the patient clenches his or her jaw, and noting pterygoid strength during jaw opening and lateral movement against resistance. Weakness of the pterygoids will produce a deviation of the jaw to the ipsilateral side when the patient opens their mouth. Observation may reveal a more prominent zygomatic arch on the symptomatic side due to muscle wasting. Although more difficult to see, flattening or depression of one side of the palate and deviation of the uvula to the other side at rest may indicate tensor veli palatini dysfunction. Elevation of the palate voluntarily or to gag, however, is mostly a tenth cranial nerve function.
A unilateral supranuclear lesion rarely causes any weakness of the muscles of mastication because cortical innervation of the trigeminal motor nuclei is bilateral. An increased jaw jerk, evaluated by tapping over a finger placed on the middle of the chin with a reflex hammer while the patient relaxes his or her jaw, can be seen in supranuclear lesions. Normally, the jaw jerk is mild or absent in the nondisease state.
Observation for involuntary movements of the jaw is important. Rhythmic jaw tremor can be seen in both essential tremor and Parkinson’s disease. Mouth retraction and jaw opening or closing may be seen in Meige’s syndrome (see elsewhere in these volumes). Fatigable weakness of the jaw, or a history that the patient has to use his or her hand to close the jaw, is a feature of myasthenia gravis. A history of clonic jaw activity or chewing movements may indicate seizure activity. Jaw claudication is a frequent complaint in temporal arteritis. Spasms of the muscles of mastication are called trismus and can be seen in hemimasticatory spasm, tetanus, encephalitis, strychnine poisoning, and hysteria.
ELECTROPHYSIOLOGIC TESTING
Electrophysiologic testing of the trigeminal nerve can be accomplished in several ways. The blink reflex is the work horse when evaluating the sensory system, and both the masseter reflex and direct electromyography (EMG) are used when evaluating the motor system.
The afferent component of the blink reflex is mediated through the trigeminal nerve, and the efferent component is mediated through the facial nerve. The stimulation site is over the supraorbital nerve, and the recording site is over the orbicularis oculi muscle. Connections are made between the trigeminal and facial nuclei in the brainstem at pontine and medullary levels. Identification of an abnormality in the reflex is based on the specific pattern of direct facial nerve stimulation and the early monosynaptic R1 and late oligosynaptic R2 latencies.9 The main application is in cases of facial pain in which clinical evaluation alone does not satisfactorily document trigeminal dysfunction. Unfortunately, demonstration of a lesion with this method may not be very high. The reported sensitivity of the blink reflex is 50% to 85% for tumor, infection, trauma, some polyneuropathies, multiple sclerosis (MS), and stroke, and it is usually normal in trigeminal neuralgia.9
Other tests of sensory function are the corneal reflex, in which direct stimulation of the cornea elicits bilateral R2 responses, but not R1 responses,10 and somatosensory evoked potentials,11 which are less useful.
The masseter or jaw reflex is a monosynaptic reflex involving proprioceptive fibers that travel by way of the mandibular division of the trigeminal nerve to the brainstem. Before reaching the mesencephalic nucleus, which lies in the midbrain, a branch synapses on the motor nucleus of the trigeminal nerve in the pons. Impulses are sent back to the masseter muscle by way of the motor nerve, causing the jaw to close.12 Use of both the blink and masseter reflexes may increase the yield of demonstrating a trigeminal nerve lesion.13 EMG of the masseter muscle may document denervation.
TRIGEMINAL NERVE DYSFUNCTION
Trigeminal nerve disorders may present with loss of function (e.g., anesthesia and paresis of mastication) or abnormal sensation (e.g., pain and paresthesias). Most pathologic processes involving the nerve can produce both. In general, peripheral nerve lesions produce anesthesia on the face and inside the mouth, whereas, central lesions only involve the face. Lesions peripheral to the gasserian ganglion usually involve only one or two trigeminal divisions, whereas proximal lesions tend to affect the whole half of the face.14 Lesions of the ganglion itself may follow either pattern. Combined involvement of cranial nerves three, four, and six or a Horner’s syndrome may localize the lesion to the cavernous sinus.
Clues to a brainstem lesion should be sought when one is faced with trigeminal nerve dysfunction. As there is some dissociation of light touch with the main sensory nucleus, and pain and thermal sensation with the nucleus of the spinal tract of the trigeminal nerve, so too might this dissociation be appreciated clinically. Also, the compact nature of the pons and medulla make it likely that other cranial nerves, as well as the ascending and descending tracts connecting the spinal cord with the cerebrum, will be affected.8
Supranuclear lesions most often have a wider distribution of dysfunction than just the face (e.g., ear, neck). Sensory loss can be seen in thalamic, internal capsule, and cortical disease. Clinical weakness usually requires bilateral disease such as would be seen with bilateral strokes or amyotrophic lateral sclerosis.
The following sections describe in more detail the diseases that can affect the trigeminal nerve. An anatomic division has been made starting at the cornea and moving through the peripheral branches, cavernous sinus, gasserian ganglion, middle cranial fossa, trigeminal root, brainstem and thalamus, basal ganglia, and sensory cortex. Finally, the authorsbriefly discuss a few systemic diseases that may affect the trigeminal nerve. The diseases that present almost entirely with facial pain will be discussed separately (see Facial Pain section). However, it should be remembered that there is often a great deal of overlap between the conditions that present with anesthesia and pain. Figure 5 portrays three diseases on a continuum. The left-hand side of the figure is trigeminal neuralgia; the quintessential disease presenting with second long shocks and no sensory loss. On the right hand side are diseases with constant symptoms represented by atypical (chronic) facial pain with pain only, and trigeminal sensory neuropathy with anesthesia only. Unfortunately, many people present with a mixture of several features and it can be difficult to know how to proceed with work-up and provide treatment.
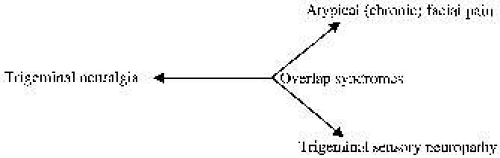 FIG. 5. Several diseases fall on a continuum between three features: timing (shock-like to constant), anesthesia, and pain. |
LOSS OF CORNEAL SENSATION
Corneal sensation is almost always decreased when a lesion of the trigeminal nerve impairs cutaneous sensation in the ophthalmic division. Direct ocular impairment from surgery, medications, corneal dystrophy, and infection can result in isolated loss of corneal sensation.15
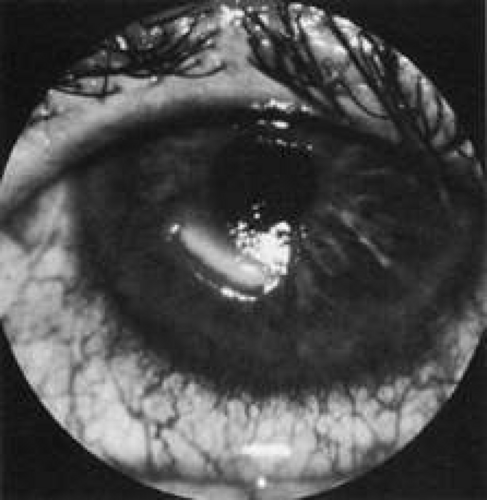
Neuroparalytic keratitis or widespread loss of corneal epithelium may occur in an eye that becomes denervated (Fig. 6). The etiology of the keratopathy is unknown, but it is presumed that loss of sensory innervation impairs corneal nutrition, surface maintenance, and repair.16,17 The keratopathy may respond poorly to artificial tear preparation and bandage soft contact lenses, but often the epithelial defect will heal after a tarsorrhaphy, which better protects the corneal epithethelium.18
PERIPHERAL BRANCHES
Peripheral branches of the trigeminal nerve can be affected by numerous disease processes. Facial trauma may impair branches of any of the three divisions, but most often the infraorbital, supratrochlear, and supraorbital nerves are damaged (see Fig. 3).19 Dental procedures are an important cause of trigeminal neuropathy, because the dental nerves course in the maxilla and mandible at the same depth as the roots of the teeth.20,21 Removal of the lower third molar deserves particular note.
Trigeminal pain and numbness are rarely the first sign of tumors of the nasopharynx, paranasal sinuses, oral cavity, and orbit. One retrospective review of 103 cases of orbital disease from all causes found sensory loss in only 3% of the patients.22
The usual presentation of trigeminal neuropathy is either anesthesia or paresthesias, but after partial regeneration of the nerve, pain may also occur.23 Even after the inciting cause is removed, return of function is not guaranteed. With trauma, as few as 50% will recover by 12 weeks, with a minority of the rest recovering by 2 years.21
In approximately 10% of cases, facial numbness occurs as a self-limited entity of unknown etiology.24,25,26,27 The term trigeminal sensory neuropathy is used by some authors to indicate this disease, whereas others mean something more broad by trigeminal sensory neuropathy, including conditions that are painful. The second and third trigeminal divisions are affected most often, and a sensory deficit can usually be detected in the involved dermatome. This condition is only rarely bilateral. Trigeminal motor function is typically normal. Involvement of the peripheral trigeminal branches is most likely the cause,25 and many authors have made an analogy with Bell’s palsy. Most patients recover sensory function over a period of a few weeks to months, but it may be recurrent. A diagnosis of idiopathic facial numbness should not be made until a thorough investigation is undertaken.26,27,28 The main differential is tumor, and there may be transient abnormalities of the trigeminal nerve on magnetic resonance imaging (MRI), furthering the confusion.29 The etiology usually remains in question until the patient shows improvement. If no improvement occurs, frequent clinical evaluations are recommended to detect a pathologic process early.
Hemimasticatory spasm is a condition of unilateral involuntary jaw closure that is often associated with facial hemiatrophy, but not always.30,31 The contractions may be prolonged but are usually brief, resembling hemifacial spasm. The spasms are painful, and patients may break teeth, develop temporomandibular joint disease, or bite their tongue. Electrodiagnostic investigations have demonstrated peripheral motor nerve demyelination. The EMG does not show denervation. Ephaptic transmission, which refers to the concept of an artificial synapse between contiguous nerves caused by the lateral spread of extraaxonal current through the interstitium, is one possible mechanism. Treatment includes botulinum toxin and carbamazepine, which is the most successful oral medication.
CAVERNOUS SINUS
Masses or inflammation in the superior orbital fissure or cavernous sinus may affect the ophthalmic and maxillary divisions of the trigeminal nerve as well as the oculomotor, trochlear, abducens, and sympathetic nerves. Trobe and associates32 reported pain and impaired sensation in one of seven patients with meningiomas and in four of nine with aneurysms in the cavernous sinus. Trigeminal neurinoma or schwannoma can occur anywhere along the nerve and has also been reported in the cavernous sinus.33
Inflammation in the cavernous sinus has been called the Tolosa-Hunt syndrome.34,35,36 Pain is a prominent feature and may precede signs of involvement of the other nerves. It is typically described as a constant “boring” ache behind the eye. Loss of sensation in the ophthalmic more than the maxillary dermatomes is frequent. Corticosteroids can help with both pain and the speed of cranial nerve recovery. In a related condition called orbital pseudotumor, the inflammation occurs more anteriorly in the actual orbit, rather than in the cavernous sinus. The distinction between Tolosa-Hunt syndrome and orbital pseudotumor may be difficult to make; the underlying immunopathologic deficit perhaps being the same.
Cranial polyneuropathy is a condition of multiple cranial nerve palsies.36,37 Involvement is not limited just to the cavernous sinus, as in the Tolosa-Hunt syndrome. The abducens nerve is the one most often affected, but any combination is possible, with the exception of the olfactory nerve. Causes include the Guillain-Barré syndrome, infections, tumors, carcinomatous meningitis, sarcoidosis, collagen vascular disease, and idiopathic causes. A retrospective review by Juncos and Beal36 found the trigeminal nerve to be involved in 5 of 14 cases of idiopathic cranial polyneuropathy they analyzed. Face and head pain were almost invariable, and corticosteroids provided symptomatic benefit.
MIDDLE CRANIAL FOSSA
Tumors at the base of the skull (chondroma, sarcoma, chordoma, meningioma, and nasopharyngeal tumors) can involve the trigeminal nerve, producing pain or a sensory deficit. In most cases, other cranial nerves are also affected.
Facial pain occurring with an oculosympathetic paresis is termed Raeder’s paratrigeminal neuralgia syndrome.38 When this is associated with ocular motor nerve involvement, a mass lesion is usually present in the middle cranial fossa. This syndrome is discussed in more detail later in the section on Facial Pain.
GASSERIAN GANGLION
The gasserian ganglion can be affected by infection or tumor. It is a frequent site of varicella zoster reactivation, and the ophthalmic division is most commonly involved.
Herpes zoster ophthalmicus behaves like zoster infections elsewhere in the body. The incidence increases with age. Pain, often severe, may precede, be concurrent with, or follow the vesicular skin eruption. Occasionally no skin lesions occur; this is referred to as zoster sine herpete. The vesicular eruption usually involves only one dermatome, but severe systemic eruptions can occur (the latter appear most often in immunocompromised persons or in persons with malignancy). Fever, malaise, headache, and lymphadenopathy may be present at the onset. Fifty percent of cases have ocular involvement, which can be predicted if vesicles appear on the lid margin or if Hutchinson’s sign is present.39,40 In 1886, Hutchinson noted that when the nasociliary branch to the tip of the nose is affected, intraocular involvement is likely. Ocular changes include conjunctivitis, episcleritis, scleritis, keratitis, iritis, chorioretinitis, optic neuropathy, glaucoma, ocular motor palsies, and Horner’s syndrome.39,41,42 On rare occasions, a contralateral hemiplegia may occur (Fig. 7).39,43,44,45 A virus-induced angiitis of cerebral vessels has been shown by angiography and pathology in several cases. Although patients with neoplastic or other debilitating diseases are predisposed to the development of herpes zoster infections, a neoplasm is discovered in less than 1% of otherwise healthy persons with cutaneous zoster.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree