Theory and Practice of Spectacle Correction of Aniseikonia
Eleanore Z. Thill
Aniseikonia, a term coined by Dr Walter Lancaster in 1932, is an anomaly of binocular vision in which the ocular images are unequal in size, shape, or both. (The ocular image is the final impression received in the higher cortical centers, involving the retinal image with modifications imposed by anatomic, physiologic, and perhaps psychological properties of the entire binocular visual apparatus.) In general, aniseikonia is associated with a false stereoscopic localization and an apparent distortion of objects in space.1 Aniseikonia can be the cause of asthenopia, diplopia, suppression, poor fusion, headaches, vertigo, photophobia, amblyopia, and strabismus.
The differences in size may be overall—that is, the same in all meridians—or meridional, in which the difference is greatest in one meridian and least in the meridian 90 degrees away. The effect of aniseikonia on space perception is usually dramatic, especially when meridional magnification is involved. This is particularly true when the horizontal meridian is involved, since horizontal disparities are the basis for the stereoscopic perception of depth.1
Aniseikonia was thoroughly researched at Dartmouth College in Hanover, NH, from 1920 to 1945 under the leadership of Adelbert Ames. Brought together at the time were some of the leading scientists of the day, including Hermann M. Burian, Paul Boeder, Robert Bannon, Walter B. Lancaster, Arthur Linksz, and Kenneth N. Ogle. Although their studies were involved with all binocular anomalies, they were particularly interested in aniseikonia.
The most obvious cases of aniseikonia, those with anisometropia, are discussed here, but one must bear in mind that there are many cases on record of patients with emmetropia or isometropia who had aniseikonia that, when corrected, relieved that patient of symptoms. These cases are further proof that aspects other than retinal image size are involved in aniseikonia. Factors such as retinal element distribution, differences in number of radiation fibers, possible modification at the synapses, and indeed the physiology of the entire neurovisual system play a part in the final perceived image size.
One study reported objective evidence of the benefits of aniseikonic correction.2 An immediate reproducible increase in amplitude of both steady-state and transient binocular visual evoked responses (VERs) was demonstrated when aniseikonic correction was included in a patient’s spectacle correction. In addition, after this patient wore the aniseikonic correction for 3 months, she reported a lessening of subjective complaints. There was great improvement in visual comfort, decreased frequency of headaches, and an increased ability to read for extended periods. The case history also suggested that the frequency of her intermittent exotropia had decreased. Additionally, there was now no indication of suppression at the patient’s normal reading distance, and stereoacuity had increased from 100 to 30 seconds of arc.
THRESHOLDS OF ANISEIKONIA
Tolerances for aniseikonia vary from patient to patient; some apparently are able to tolerate rather large amounts, and others have severe symptoms with much smaller levels. It is when the difference in image size or meridional distortions approaches the patient’s tolerance that the symptoms of aniseikonia become manifest and troublesome. We may define clinical aniseikonia as the amount of aniseikonia that must be corrected to eliminate the patient’s symptoms.
Clinical aniseikonia usually occurs when the difference in image size between the two eyes approaches 0.75%. Meridional distortions are more poorly tolerated, especially when they are oblique (not horizontal or vertical). Oblique meridional aniseikonia causes a rotary deviation between the fused images of vertical lines in the two eyes; this is termed declination. Declination becomes clinically troublesome when it approaches 0.3 degrees.
INCIDENCE OF ANISEIKONIA
The estimation of the incidence of aniseikonia varies with the investigator and with the population studied. According to the Dartmouth College study, which spanned 15 years, aniseikonic lenses were prescribed for 4% of the population of Hanover. In their follow-up study, the researchers found that about 75% of these patients declared they had benefited from the correction, which would indicate that 3% of the general population need and benefit from the correction of an aniseikonia.
Gillott, in England, examined a cross section of a community and found 8% to have a significant aniseikonia, associated with symptoms.3 Ewalt, who used eikonometry for a lengthy period, suggested the clinically significant incidence to be about 2%.4 Duke-Elder said that some degree should be expected in 20% to 30% of people who wear spectacle correction.5
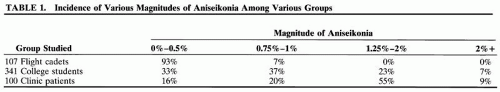
A study of different groups shows differences in occurrence. Burian and Triller showed that the composition of the group influences the incidence (Table 1)6.
EFFECTS ON VISUAL FUNCTIONING
Different authors show a similarity in the nature of symptoms and their frequencies.4,7 Symptoms, in order of their frequency of occurrence, are local eye discomfort (tiring), headaches, difficulty reading, photophobia, poor depth perception, vertigo, nausea, motility difficulty, nervousness, and physical fatigue.
AXIAL VERSUS REFRACTIVE ANISOMETROPIA
Although aniseikonia can be measured using an instrument such as the American Optical Space Eikonometer, these instruments are not widely available. Remole and Robertson list several direct comparison tests using equipment usually found in the refracting room, such as Brecker’s device.8 Another direct comparison test, the Awaya NAT (New Aniseikonia Test) is available from Binocular Vision Quarterly.*9 It consists of a booklet containing a series of red and green half moons (dissociated with red and green spectacles) differing in size from 1% to 24%.8
We suspect aniseikonia may be present in cases of anisometropia. Anisometropia may be divided into two major categories: axial, in which the difference between the two eyes is due to a difference in their axial lengths, and refractive, in which the ametropic difference between the two eyes occurs as a result of differences in corneal or lens power, or position of crystallin lens.
Clinical rules for applying these concepts are as follows:
If the anisometropia is 2 D or more, assume it is axial.10
If the anisometropia is less than 2 D or is in cylinder only, assume it is refractive. Astigmatism is classified as a cause of refractive aniseikonia if it is found in only one eye, if the power needed is greater in one eye than the other, or if the axes in each eye differ from one another.
RETINAL IMAGE SIZE
IN UNCORRECTED REFRACTIVE AMETROPIA
If we start with a hypothetical emmetropic eye and make it ametropic by changing only the power of its cornea or lens (refractive ametropia), this uncorrected eye now receives a blurred image. The size of this uncorrected image is changed only minimally, the myopic eye having a slightly smaller image by 0.25% per diopter and the hyperopic eye having a slightly larger image by 0.25% per diopter.
IN CORRECTED REFRACTIVE AMETROPIA
Correcting refractive ametropia with spectacles placed at the anterior focal point (about 15 mm from the cornea) causes the resultant image to be clear but now different in size from the emmetropic eye by 1.5% per diopter, smaller in myopia and larger in hyperopia. Placing the lens closer to the cornea than 15 mm will result in less minification for the minus lens or less magnification for the plus lens. Placing the refractive correction on the cornea (contact lenses) gives the least change in image size from the uncorrected state in refractive ametropia. If contact lenses can be tolerated and the ametropia is of refractive nature, it is possible that no other correction for aniseikonia may be necessary.
IN UNCORRECTED AXIAL AMETROPIA
Let us consider the case of our hypothetical emme-tropic eye, this time made ametropic by varying only the axial length. This eye then receives a blurred image but with a significant change in image size as well. The axially myopic eye has a larger image by about 1.50% per diopter and the axially hyperopic eye has a smaller image by 1.5% per diopter.
IN CORRECTED AXIAL AMETROPIA
Placing the correcting lens at the anterior focal point of the eye (about 15 mm from the cornea) again causes a 1.5% per diopter change in size of the image from what it was when uncorrected, just as in the previously discussed refractive case, with the minus lens decreasing the size by 1.5% per diopter and the plus lens increasing the size by 1.5% per diopter. However, the uncorrected axial image size as stated above is larger in myopia and smaller in hyperopia. (KnapP′s law: in the axially ametropic eye, if the correcting lens is placed before the eye so that the second principal plane of the lens coincides with the anterior focal point of the eye, the size of the image on the retina will be the same as if the eye were emmetropic11).
Theoretically, although axial ametropes would not need aniseikonic correction if the correcting lenses were placed at the anterior focal point, these patients often can be made far more comfortable by judicious use of the techniques we will discuss. Studies show that sometimes minification is needed for axially myopic eyes and magnification is needed for axially hyperopic eyes,12,13,14,15,16 just as in the case of the refractive ametrope.
The reasoning behind this is as follows: whereas the retinal image of the corrected eye may be the same as in emmetropia as stated in KnapP′s law, the final image received in the higher cortical centers is different because the retinal elements have been either scattered or condensed through stretching or shrinking of the retina associated with the change in axial length. For example, when the axial length of the eye increases, the retina must also stretch so that the retinal element population is decreased for a given area, thereby causing the patient to perceive a smaller image since fewer retinal elements are being stimulated. The opposite occurs for hyperopia caused by an axially shortened eye.
ESTIMATING THE AMOUNT OF ANISEIKONIA
The guidelines given by the Dartmouth studies for estimating the amount of aniseikonia were as follows: If the difference in image size associated with anisometropia is primarily of refractive origin, we can expect it to be about 1.5% per diopter of anisometropia, but since the anisometropia may be partly axial, an estimate of 1% per diopter is more useful clinically. The eye requiring the more myopic, or less hyperopic, correction would be expected to require the magnification.
PRESCRIBING ANISEIKONIA LENSES
When deciding which spectacle lens to modify it is important to realize that the size and shape of the final image does not matter; it is only important that the images of each eye match each other. In designing lenses, instead of magnifying the image of one eye it may be easier to minify the image in the other eye. In doing so, it may be possible to thus present to the patient a more cosmetically acceptable pair of spectacles, or perhaps lenses that are more easily manufactured and therefore less costly.
The total magnification of a lens (Mt), in percent, is found by adding the magnification in percent from its power (Mp) and the magnification in percent from its shape (Ms):
(eq 1)