 Orbital Lymphoid Tumors and Leukemias
Orbital Lymphoid Tumors and LeukemiasOrbital Non-Hodgkin Lymphoma
General Considerations
Lymphoid tumors range from low-grade lymphoid hyperplasias to highly malignant lymphoma. The classification of lymphoid tumors is complex, discussed in textbooks and articles, and beyond the scope of this textbook. The Revised European American Lymphoma (REAL) classification and its updated version by the World Health Organization is preferred by many authorities (1). Lymphoma can affect any part of the eye and adnexa. The low-grade mucosa-associated lymphoid tissue (MALT) lymphomas, which can also occur in the orbit, are discussed in the conjunctival section. Non-Hodgkin lymphoma of B-cell lineage is the most common type in the orbit (2,3,4,5,6,7,8,9,10,11,12,13,14,15,16,17,18,19,20,21,22,23,24,25,26,27). Less common orbital lymphoid lesions like Burkitt lymphoma, T-cell lymphoma, plasmacytoma, and leukemias are also discussed.
Non-Hodgkin lymphoma in the orbit and ocular adnexa can be divided into benign (benign reactive lymphoid hyperplasia [BRLH]), intermediate, or malignant categories. It is difficult to determine clinically whether a particular lesion is benign or malignant and histopathologic evaluation is necessary to accurately categorize these lesions. For reasons of brevity, the term “lymphoma” is used here to describe all of these variations.
In general, orbital lymphoma has rather characteristic clinical, radiographic, and pathologic features. It generally occurs in older individuals, and is the most common malignant orbital tumor of older patients, accounting for 24% of all orbital malignancies in patients .59 years old (4). Orbital lymphoma can be confined to the orbit or it can be a part of systemic lymphoma. Although estimates vary, it is estimated that the incidence of systemic lymphoma among patients with orbital lymphoma is approximately 50%. Orbital lymphoma may be more common in immunosuppressed patients (20).
An unusual form of orbital lymphoma is being seen as a manifestation of post-transplant lymphoproliferative disorder (PTLD) and orbital involvement can develop before systemic involvement is recognized (27).
Clinical Features
Orbital lymphoma typically presents as a painless, slowly progressive, unilateral or bilateral anterior orbital mass that can often be palpable through the eyelid or conjunctiva as a rubbery mass. It is important in such cases to inspect the conjunctiva for a typical fleshy (salmon patch) infiltration and to check the uveal tract for iris or choroidal infiltration that, if present, strongly suggests that the orbital lesion is lymphoma.
Diagnostic Approaches
The patient with a suspected orbital lymphoma should undergo a thorough systemic evaluation to detect and determine the extent of any associated systemic lymphoma. With regard to the orbital lesion, computed tomography (CT) and magnetic resonance imaging (MRI) disclose an ovoid or elongated mass that tends to mold to adjacent orbital structures and shows moderate enhancement with contrast agents. It is usually confined to soft tissue; bone involvement is uncommon. It can occur anywhere in the orbit and is commonly confined to the lacrimal gland. Lymphoid tumors that arise in the lacrimal gland should be differentiated from primary epithelial tumors of the lacrimal gland. Lymphoid tumors generally have an oblong, ovoid, or pancake contour and mold to the globe and orbital bones, usually without producing a bony fossa or bony erosion. In contrast, epithelial tumors of the lacrimal gland tend to have a more rounded contour and tend to compress the bone, producing a fossa or sometimes actual bone destruction.
Pathology
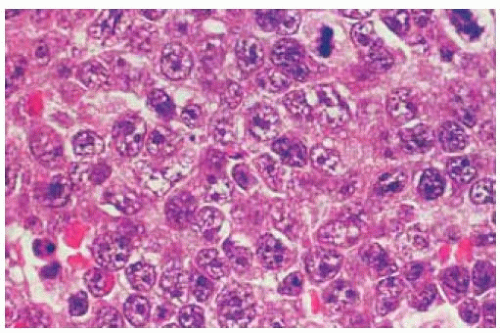
Most benign or malignant orbital lymphomas are of the B-cell type, classified histopathologically as extranodal marginal-zone, B-cell lymphoma according to the REAL classification (13). BRLH is characterized by a polymorphous array of small round lymphocytes and plasma cells. Mitotically active germinal centers are frequently present.
The intermediate form is a borderline between BRLH and frank malignant lymphoma. It is composed of monomorphous sheets of lymphocytes. In contrast with reactive lymphoid hyperplasia, the nuclei are somewhat larger, prominent nucleoli are sometimes present, and abortive follicles may be observed.
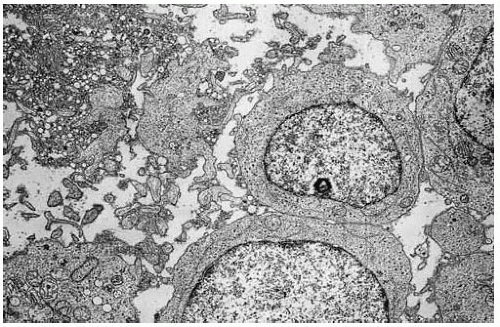
Malignant non-Hodgkin lymphoma is characterized by more anaplastic cells with larger cleaved nuclei, more nuclear pleomorphism, and frequent prominent nucleoli. Lymph follicles and endothelial cell proliferation are absent or less evident. As mentioned, many orbital/adnexal lymphoid tumors are derived from MALT (20,26).
Management
Management of suspected orbital lymphoma is individualized to each case. An excisional or incisional orbital biopsy is generally advisable and the best approach to biopsy is determined by imaging studies. Prior communication with a pathologist is important so that the excised tissue can be appropriately processed for immunohistochemistry and flow cytometry. The surgeon should remove as much of the orbital tumor as possible, attempting to avoid damage to vital orbital structures.
A physical examination and laboratory and imaging studies should be done to rule out systemic lymphoma. If the patient has known systemic lymphoma and the orbital lesion is located anteriorly beneath the skin, a fine-needle biopsy can help to establish the orbital diagnosis, thus avoiding an open biopsy. If systemic lymphoma is present and chemotherapy is advised, then the orbital lesion can usually be followed with no further treatment. If no systemic lymphoma is found, then the orbital lymphoma can be treated with local orbital radiotherapy (1,10,11,23,27). About 2,000 to 2,500 cGy is given for more benign lesions and about 3,500 to 4,000 cGy for malignant lesions. In most cases, radiotherapy appears to be safe and effective (10). Even if evaluation for systemic lymphoma
is negative, the patient should have yearly or biyearly follow-up for the development of systemic lymphoma.
is negative, the patient should have yearly or biyearly follow-up for the development of systemic lymphoma.
Orbital MALT lymphoma requires special mention because of the recent revelations regarding its relationship to gastric MALT lymphoma and Helicobacter pylori and Chlamydia species. There is currently interest in treating some cases of MALT lymphoma of the conjunctiva and orbit with antibiotics directed toward these organisms.
Selected References
1. Armitage JO, Mauch PM, Harris NL, et al. Non-Hodgkin’s lymphomas. In: DeVita VT Jr, Hellman S, Rosenberg SA, eds. Cancer. Principles and Practice of Oncology. 6th ed. Philadelphia: Lippincott, Williams & Wilkins; 2001: 2265-2272.
2. Shields JA, Bakewell B, Augsburger DG, et al. Classification and incidence of space-occupying lesions of the orbit. A survey of 645 biopsies. Arch Ophthalmol 1984;102:1606-1611.
3. Shields JA, Shields CL, Scartozzi R. Survey of 1264 patients with orbital tumors and simulating lesions: the 2002 Montgomery Lecture, part 1. Ophthalmology 2004;111:997-1008.
4. Demirci H, Shields CL, Shields JA, et al. Orbital tumors in the older adult population. Ophthalmology 2002;109:243-248.
5. Knowles DM, Jakobiec FA. Orbital lymphoid neoplasms: a clinicopathologic study of 60 cases. Cancer 1980;46:576-589.
6. Knowles DM II, Jakobiec FA. Ocular adnexal lymphoid neoplasms: clinical, histopathologic, electron microscopic, and immunologic characteristics. Hum Pathol 1982;13:148-162.
7. Yeo JH, Jakobiec FA, Abbott GF, et al. Combined clinical and computed tomographic diagnosis of orbital lymphoid tumors. Am J Ophthalmol 1982; 94:235-245.
8. Jakobiec FA, Yeo JH, Trokel SL, et al. Combined clinical and computed tomographic diagnosis of lacrimal fossa lesions. Am J Ophthalmol 1982;94: 785-807.
9. Nicolo M, Truini M, Sertoli M, et al. Follicular large-cell lymphoma of the orbit: a clinicopathologic, immunohistochemical and molecular genetic description of one case. Graefes Arch Clin Exp Ophthalmol 1999;237: 606-610.
10. Bolek TW, Moyses HM, Marcus RB Jr, et al. Radiotherapy in the management of orbital lymphoma. Int J Radiat Oncol Biol Phys 1999;44:31-36.
11. Restrepo A, Raez LE, Byrne GE Jr, et al. Is central nervous system prophylaxis necessary in ocular adnexal lymphoma? Crit Rev Oncol 1998;9:269-273.
12. Kennerdell JS, Flores NE, Hartsock RJ. Low-dose radiotherapy for lymphoid lesions of the orbit and ocular adnexa. Ophthal Plast Reconstr Surg 1999;15:129-133.
13. Coupland SE, Krause L, Delecluse HJ, et al. Lymphoproliferative lesions of the ocular adnexa. Analysis of 112 cases. Ophthalmology 1998;105:1430-1441.
14. Adkins JW, Shields JA, Shields CL, et al. Plasmacytoma of the eye and orbit. Int Ophthalmol 199620:339-343.
15. Liesegang TJ. Ocular adnexal lymphoproliferative lesions. Mayo Clin Proc 1993;68:1003-1010.
16. Park KL, Goins KM. Hodgkin’s lymphoma of the orbit associated with acquired immunodeficiency syndrome. Am J Ophthalmol 1993;116:111-112.
17. Font RL, Laucirica R, Patrinely JR. Immunoblastic B-cell malignant lymphoma involving the orbit and maxillary sinus in a patient with acquired immune deficiency syndrome. Ophthalmology 1993;100:966-970.
18. Font RL, Shields JA. Large cell lymphoma of the orbit with microvillous projections (“porcupine lymphoma”). Arch Ophthalmol 1985;103:1715-1719.
19. Shields JA, Cooper H, Donoso LA, et al. Immunohistochemical and ultrastructural study of unusual IgM lambda lymphoplasmacytic tumor of the lacrimal gland. Am J Ophthalmol 1986;101:451-457.
20. Cockerham GC, Jakobiec FA. Lymphoproliferative disorders of the ocular adnexa. Int Ophthalmol Clin 1997;37:39-59.
21. Bairey O, Kremer I, Rakowsky E, et al. Orbital and adnexal involvement in systemic non-Hodgkin’s lymphoma. Cancer 1994;73:2395-2399.
22. Medeiros LJ, Harris NL. Lymphoid infiltrates of the orbit and conjunctiva. A morphologic and immunophenotypic study of 99 cases. Am J Surg Pathol 1989;13:459-471.
23. Lee SW, Suh CO, Kim GE, et al. Role of radiotherapy for primary orbital lymphoma. Am J Clin Oncol 2002;25:261-265.
24. Tranfa F, Di Matteo G, Strianese D, et al. Primary orbital lymphoma. Orbit 2001;20:119-124.
25. Lauer SA. Ocular adnexal lymphoid tumors. Curr Opin Ophthalmol 2000;11:361-366.
26. Malek SN, Hatfield AJ, Flinn IW. MALT lymphomas. Curr Treat Options Oncol 2003;4:269-279.
27. Douglas RS, Goldstein SM, Katowitz JA, et al. Orbital presentation of posttransplantation lymphoproliferative disorder: a small case series. Ophthalmology 2002;109:2351-2355.
Orbital Non-Hodgkin Lymphoma: Clinical, Computed Tomography, and Magnetic Resonance Imaging Features
Orbital lymphoma has rather characteristic clinical and radiographic features that should strongly suggest the diagnosis.
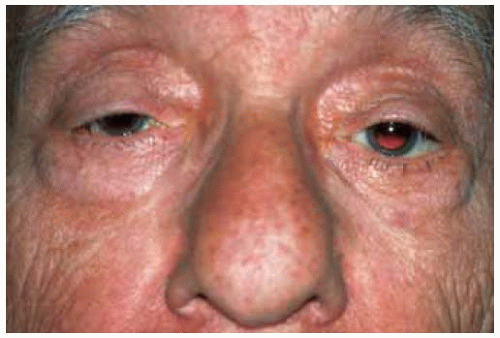
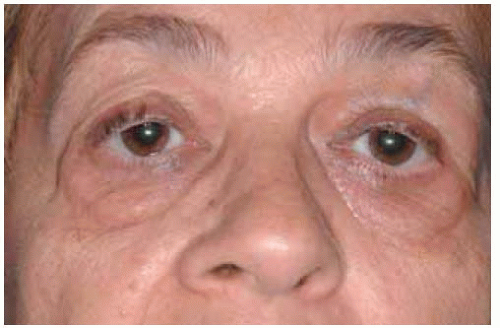
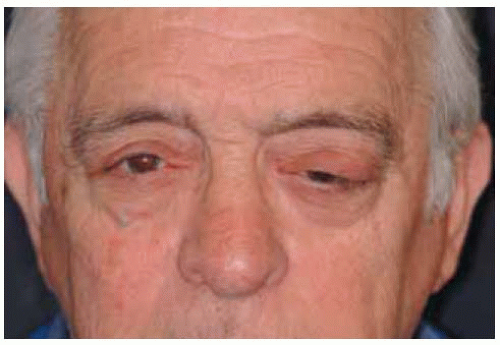
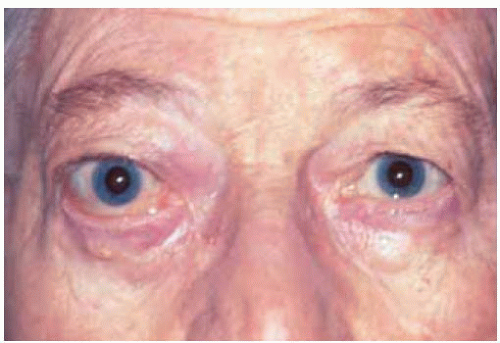 Figure 39.1. Slight proptosis of the right eye in a 90-year-old man with no prior history of lymphoma. |
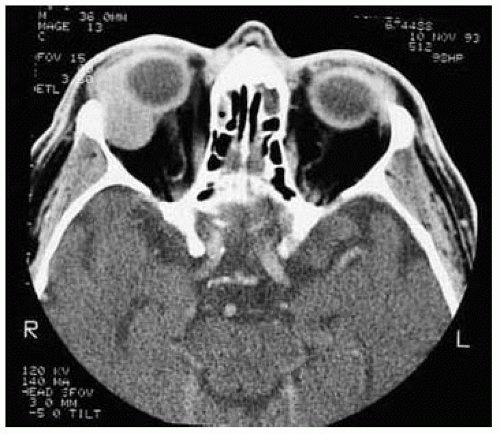
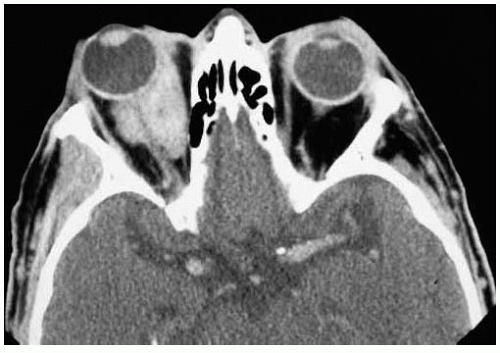 Figure 39.2. Axial computed tomography of patient shown in Figure 39.1. Note the characteristic diffuse orbital mass that molds to the globe and optic nerve. In such a case, incisional biopsy can be done under local anesthesia. |
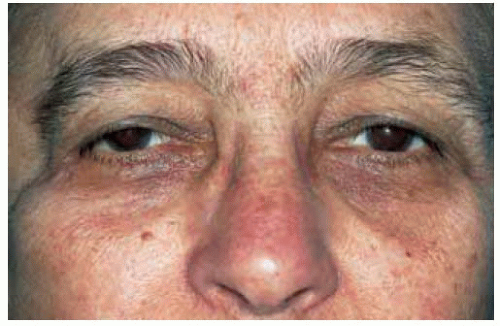
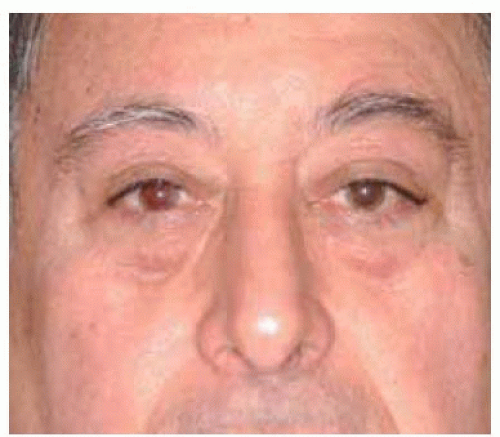
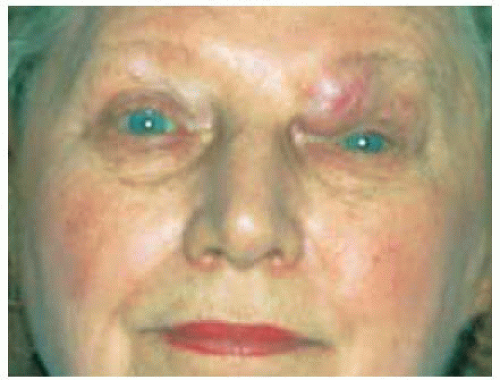
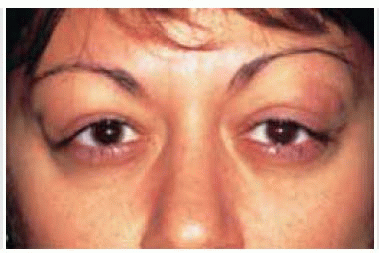
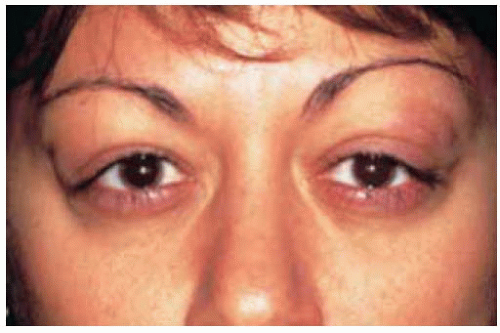 Figure 39.3. Bilateral lacrimal gland involvement by lymphoma. Note the superotemporal orbital fullness bilaterally in this 37-year-old woman. |
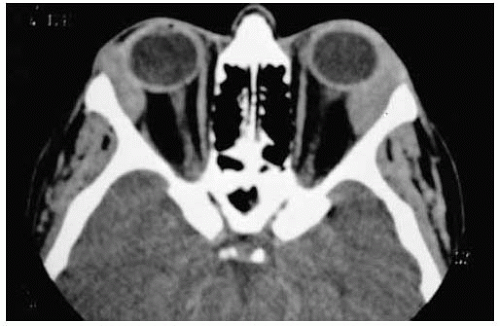 Figure 39.4. Axial computed tomography of patient shown in Figure 39.3 showing the bilateral orbital masses that affect the lacrimal glands and mold to the globe and orbital bone. |
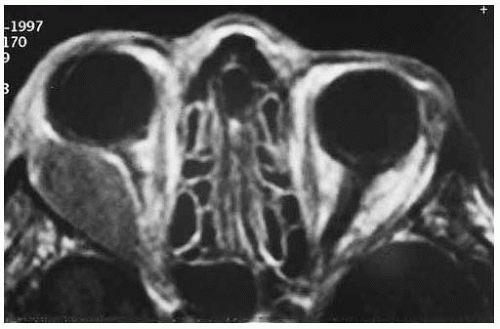 Figure 39.6. Axial magnetic resonance imaging of patient shown in Figure 39.5 in T1-weighted image of patient shown in Figure 39.5 showing diffuse ovoid mass in temporal aspect of the right orbit. |
Orbital Non-Hodgkin Lymphoma: Clinical Variations and Pathology
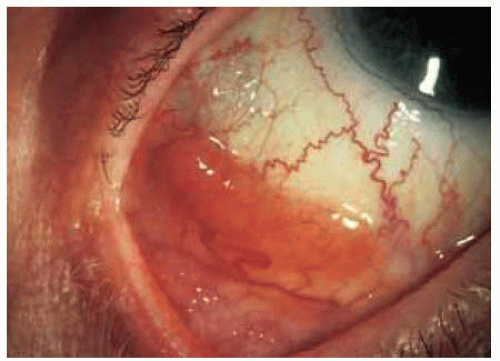
In a patient with suspected orbital lymphoma, it is important to perform a complete ocular examination. The finding of typical lymphoma of the conjunctiva or uveal tract should strongly suggest that the orbital lesion is lymphoma.
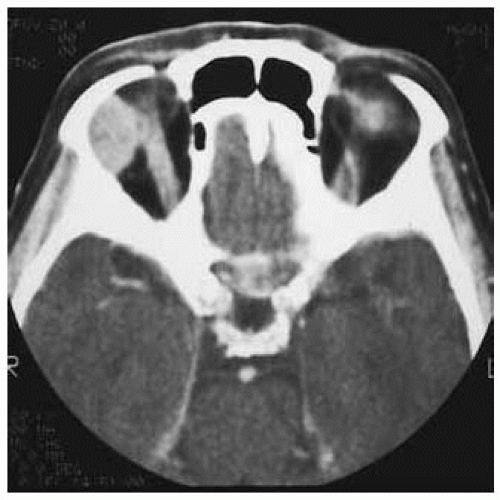 Figure 39.8. Axial computed tomography showing ovoid mass in superotemporal aspect of orbit in patient seen in Figure 39.7. |
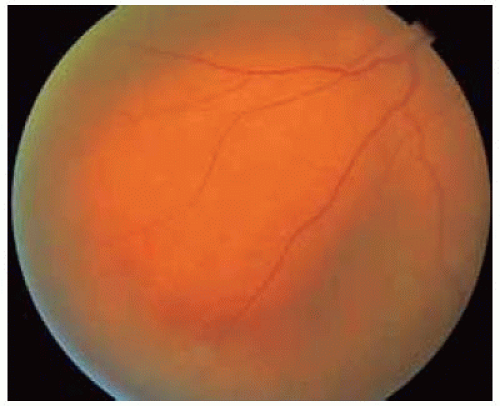 Figure 39.10. Yellow-orange lymphoid infiltrate in choroid inferotemporally in same patient. The patient declined treatment and the orbital, conjunctival, and choroidal lesions enlarged very slowly. |
Orbital Lacrimal Gland Lymphoma: Clinical and Magnetic Resonance Imaging Correlations
Lymphoma can occur anywhere in the orbit and it seems to have a slight predilection for the lacrimal gland. Like other orbital lymphomas, it can be unilateral or bilateral and isolated or part of systemic lymphoma. It usually presents as a painless, slowly growing, anterior orbital mass that is often visible or palpable through the skin. Imaging studies like computed tomography and magnetic resonance imaging are invaluable in making the diagnosis and determining the approach to biopsy. Cases are shown, each of which was confirmed histopathologically.
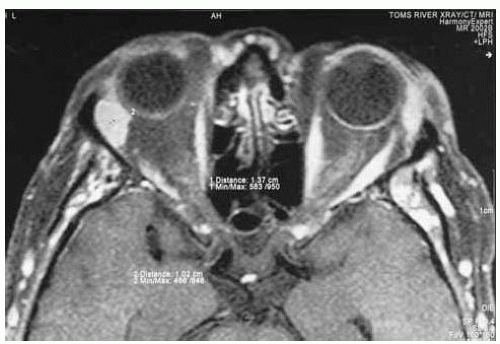 Figure 39.14. Axialm agnetic resonance imaging in T1-weighted image and gadolinium enhancement of patient shown in Figure 39.13. Note the moderatelyen larged right lacrimal gland and mildly enlarged left lacrimal gland. |
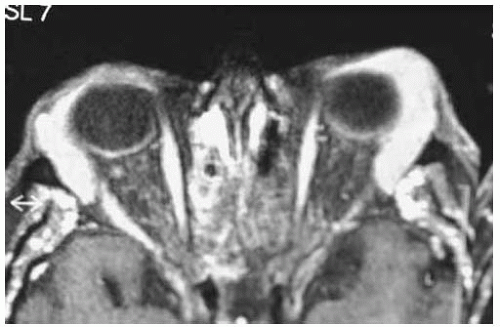 Figure 39.16. Axial magnetic resonance imaging in T1-weighted image and gadolinium enhancement of patient shown in Figure 39.15. Note how the mass molds to the globe and orbital bones. |
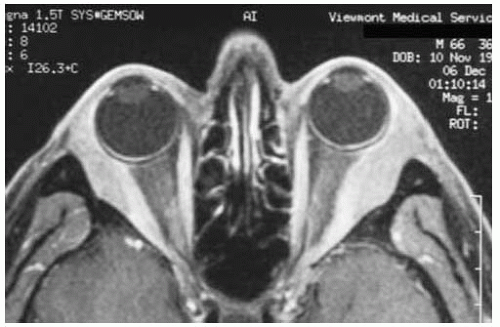 Figure 39.18. Axial magnetic resonance imaging in T1-weighted image and gadolinium enhancement of patient depicted in Figure 39.17 showing bilateral elongated masses extending from the lacrimal glands along the lateral rectus muscles. |
Orbital Non-Hodgkin Lymphoma: Diagnosis and Management
In most instances, a biopsy is indicated for suspected orbital lymphoma. If there is no known lymphoma, an open biopsy is done using the most accessible approach as determined by axial and coronal computed tomography or magnetic resonance imaging. Small anterior circumscribed tumors should be excised completely if possible. Large nonresectable tumors should have incisional biopsy, still removing as much of the tumor as possible. If the patient has known lymphoma that has already been diagnosed and staged, a fine-needle aspiration biopsy can be performed to confirm the orbital diagnosis. The orbital tumor can respond to either irradiation or chemotherapy.
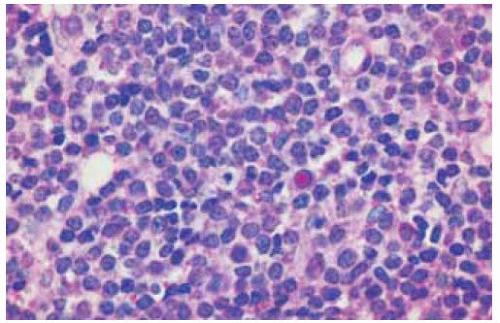
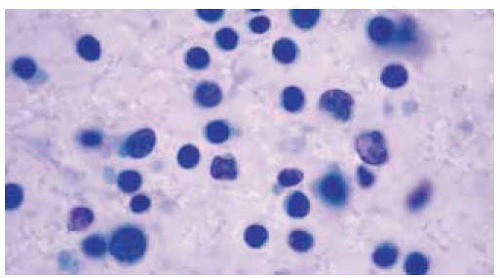 Figure 39.22. Cytology of fine-needle aspiration biopsy of patient shown in Figure 39.21. Note the large and small lymphocytes. Diagnosis was low-grade malignant lymphoma. (Papanicolau 300.) |
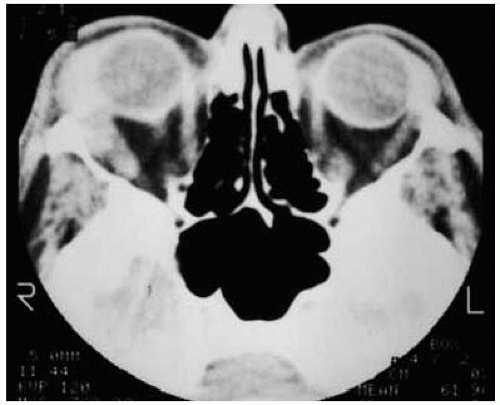 Figure 39.23. Response of orbital lymphoma to irradiation. Axial computed tomography shows a diffuse right temporal orbital mass in a 70-year-old man. |
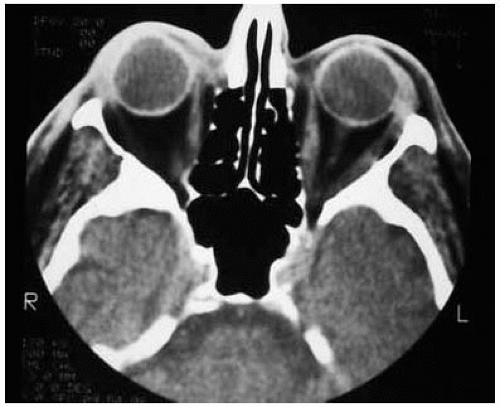 Figure 39.24. Postirradiation axial computed tomography of patient shown in Figure 39.23 demonstrating complete regression of the tumor. |
Orbital Lymphoma: Atypical Form
Most orbital lymphomas are typical non-Hodgkin B-cell lymphoma (1). However, unusual variants do occur. An example is shown of a large cell lymphoma with microvillous projections. This rare form of lymphoma may be confused with an epithelial tumor with light microscopy and even with electron microscopy (2).
Cutaneous T-cell lymphoma (mycosis fungoides) can also affect the orbit (3). It appears to be much more aggressive than B-cell lymphoma and can grow rapidly and destroy the eye. Most patients who develop orbital T-cell lymphoma already have systemic T-cell lymphoma (mycosis fungoides). The treatment is similar to that described for B-cell lymphoma. The prognosis is guarded.
Selected References
1. Shields JA. Lymphoid tumors and leukemias. In: Shields JA, ed. Diagnosis and Management of Orbital Tumors. Philadelphia: WB Saunders; 1989: 41-42.
2. Font RL, Shields JA. Large cell lymphoma of the orbit with microvillous projections (“porcupine lymphoma”). Arch Ophthalmol 1985;103:1715-1719.
3. Meekins B, Proia AD, Klintworth GK. Cutaneous T-cell lymphoma presenting as rapidly enlarging ocular adnexal tumor. Ophthalmology 1985;91;1288-1293.
Orbital Lymphoma: Atypical Forms: Large Cell Lymphoma With Microvillus Projections and Cutaneous T-Cell Lymphoma
1. Font RL, Shields JA. Large cell lymphoma of the orbit with microvillous projections (“porcupine lymphoma”). Arch Ophthalmol 1985;103:1715-1719.
2. Meekins B, Proia AD, Klintworth GK. Cutaneous T-cell lymphom a presenting as rapidly enlarging ocular adnexal tumor. Ophthalmology 1985;91;1288-1293.
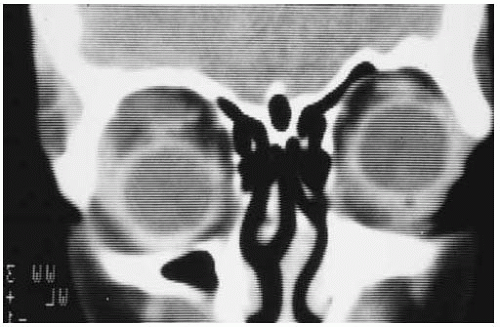 Figure 39.26. Coronal computed tomography showing superotemporal orbital mass in patient seen in Figure 39.25. There was bone erosion evident on many sections. |
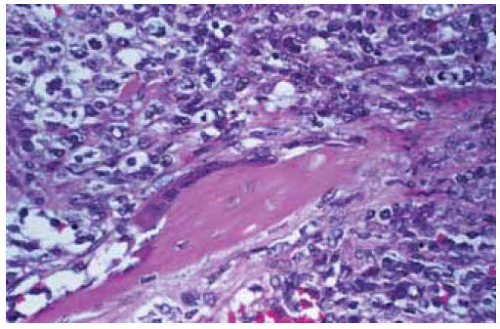 Figure 39.27. Histopathology showing anaplastic tumor cells. The diagnosis could not be determined on the basis of light microscopy. (Hematoxylin-eosin 100.) |
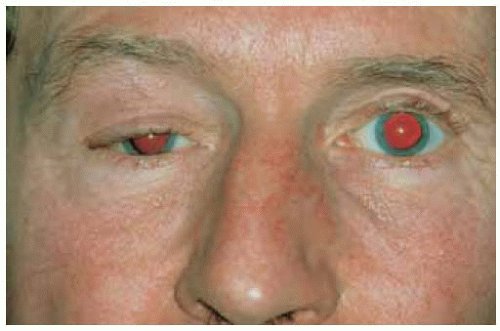
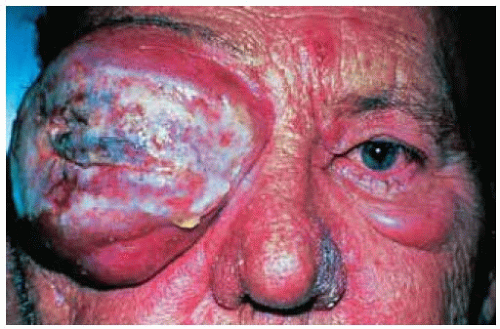 Figure 39.29. Massive orbital involvement and destruction of the eye by aggressive T-cell lymphoma (mycosis fungoides). (Courtesy of Gordon Klintworth, MD.) |
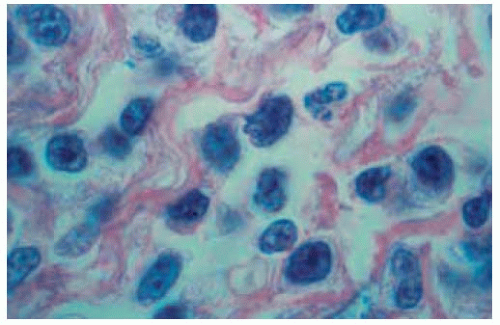 Figure 39.30. Histopathology of lesion shown in Figure 39.29 demonstrating malignant T cells. (Hematoxylin-eosin 400.) (Courtesy of Gordon Klintworth, MD.) |
Orbital Plasmacytoma and Lymphoplasmacytoid Tumo
General Considerations
Tumors composed of pure plasma cells (plasmacytomas) or those composed of B lymphocytes and plasma cells (lymphoplasmacytoid tumors) are closely related to the various lymphomas already discussed (1,2,3,4,5,6,7,8,9,10,11,12,13,14,15,16,17,18,19,20,21,22,23,24,25). The plasma cell is actually a B lymphocyte that produces large amounts of immunoglobulin. Lymphoplasmacytoid tumors are closer in the spectrum to lymphoma. Plasmacytoma is a tumor composed predominantly of plasma cells and is closer in the spectrum to multiple myeloma. Multiple myeloma is a plasma cell neoplasm characterized by plasma cell infiltration of bone marrow and by monoclonal immunoglobulin (Bence-Jones protein) in the serum. A solitary form of extramedullary plasma cell tumor usually occurs in the upper respiratory tract, gastrointestinal tract, or lymph nodes. It is relatively rare in the orbit, where it can occur as a soft tissue or bony lesion (1,2,3,4,5,6,7,8,9,10,11,12,13,14,15,16,17,18,19,20,21,22,23,24). Plasmacytoma can involve the orbit as a solitary lesion or as part of multiple myeloma. The majority of patients with solitary plasmacytoma will eventually develop multiple myeloma. In the authors’ clinical series, the six cases of plasmacytoma accounted for 4% of all orbital lymphoid tumors and for ,1% of all orbital tumors (2).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree