 Benign Tumors of the Eyelid Epidermis
Benign Tumors of the Eyelid EpidermisThere are many benign tumors and pseudotumors of the epidermis that are discussed in textbooks on dermatology. Many of these lesions can occur on the skin of the eyelid. This section discusses those that have a tendency to develop on the eyelids and that are better known to ophthalmologists and ophthalmic pathologists.
Eyelid Squamous Papilloma
General Considerations
Squamous papilloma is a nonspecific term used to designate several different conditions characterized clinically by a wartlike lesion and histopathologically by benign hyperplasia of squamous epithelium. Therefore, it is not a specific clinicopathologic entity. However, ophthalmologists and ophthalmic pathologists have come to use the term clinically and histopathologically to characterize the condition described herein. Squamous papilloma is one of the most common eyelid lesions. It usually occurs in middle-aged or elderly individuals and can assume several clinical configurations (1,2,3,4,5). This eyelid lesion is quite different from the conjunctival infectious papilloma, which generally occurs in younger people and has a fleshy, pink-red color. It is discussed later, under the topic of conjunctival lesions.
Clinical Features
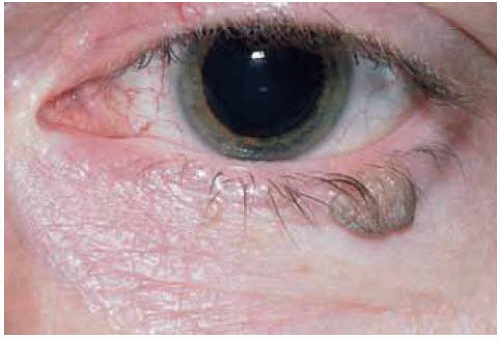
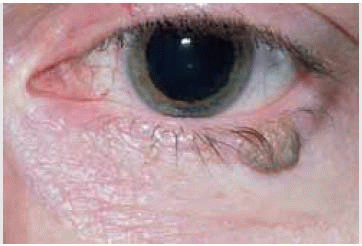
Clinically, eyelid squamous papilloma can be sessile, pedunculated, solitary, or multiple, and is usually of similar color to the adjacent skin (1,2,3). However, it can sometimes be pigmented, particularly in dark-skinned individuals. Sessile papilloma is broad based and slightly elevated, and often has a smooth surface. In contrast, pedunculated papilloma is more elevated and generally has a rough, convoluted, cerebriform surface. A rough keratin crust can often be palpated on the surface of the lesion (keratotic papilloma or “wart”). Eyelid papilloma tends to have a gradual onset and to progress slowly. Abrupt onset and more rapid growth suggests another diagnosis.
Differential Diagnosis
The differential diagnosis includes melanocytic nevus, basal cell carcinoma, seborrheic keratosis, fibroma, and verruca vulgaris. In our experience, a sessile papilloma can be remarkably similar clinically to amelanotic melanocytic nevus or a nonulcerated basal cell carcinoma.
Pathology
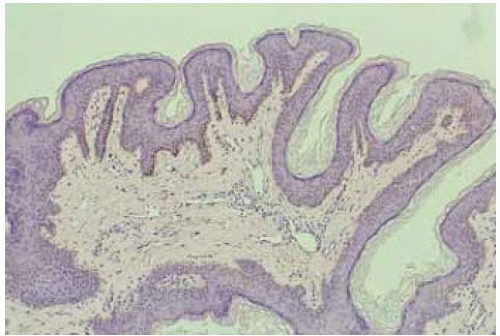
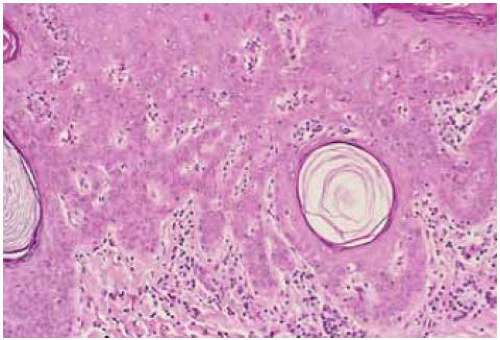
Microscopically, eyelid papilloma is composed of vascularized fibrous connective tissue covered by acanthotic epithelium. The more pedunculated lesions have fingerlike projections of fibrovascular connective tissue lined by epidermis with hyperkeratosis and acanthosis.
Management
Prognosis
The prognosis for eyelid papilloma is excellent. Unlike the inverted squamous papilloma that develops in lacrimal drainage system, the eyelid papilloma has little or no malignant potential.
Selected References
1. Font RL. Eyelids and lacrimal drainage system. In: Spencer WH, ed. Ophthalmic Pathology. An Atlas and Textbook. 4th ed. Philadelphia: WB Saunders; 1996:2227.
2. Older JJ. Eyelid Tumors. Clinical Diagnosis and Surgical Treatment. 2nd ed. New York: Raven Press; 2003:47.
3. Geist CE. Benign epithelial tumors. In: Albert DM, Jakobiec FA, eds. Principles and Practice of Ophthalmology. Philadelphia: WB Saunders; 2000:3353-3354.
4. Beckman H, Fuller TA, Boyman R, et al. Carbon dioxide laser surgery of the eye and adnexa. Ophthalmology 1980;87:990-1000.
5. Wohlrab TM, Rohrbach JM, Erb C, et al. Argon laser therapy of benign tumors of the eyelid. Am J Ophthalmol 1998;125:693-697.
Eyelid Squamous Papilloma
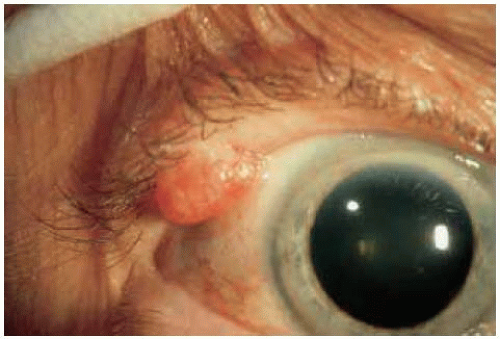 Figure 1.1. Sessile papilloma located on the upper eyelid margin of a 63-year-old woman. It appears as a pink lesion with a smooth surface. |
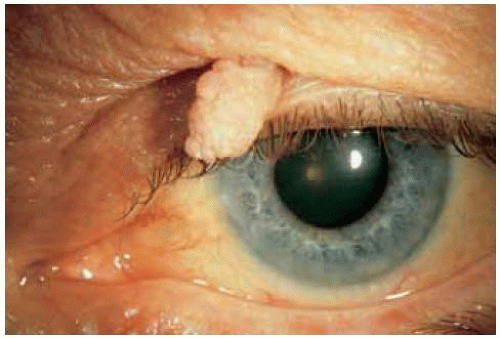
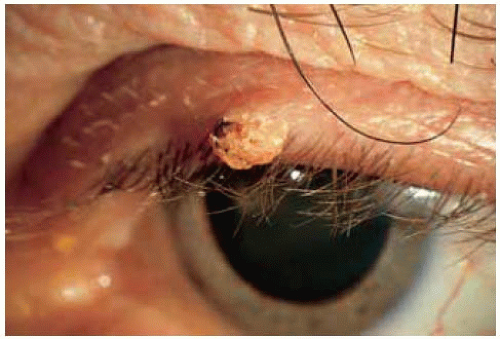 Figure 1.2. Slightly pedunculated papilloma in the upper eyelid of a 72-year-old man. Note the rough, irregular surface of the lesion. |
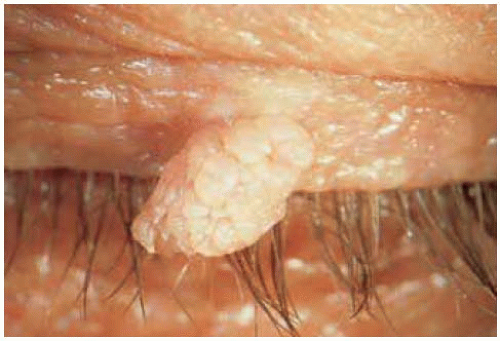 Figure 1.4. Close view of lesion shown in Figure 1.3 depicting the corrugated surface. |
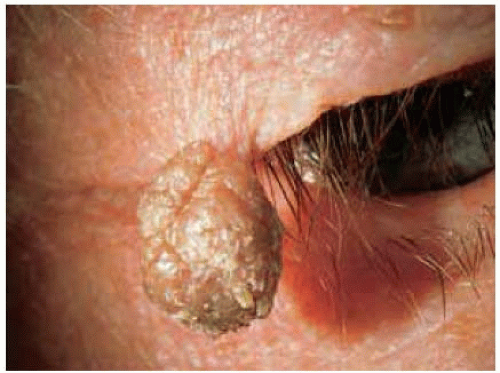 Figure 1.5. Markedly pedunculated papilloma arising from the lateral portion of upper eyelid in an 80-year-old man. |
Eyelid Seborrheic Keratos
General Considerations
Seborrheic keratosis (SK; basal cell papilloma; seborrheic wart) is a common, benign, cutaneous lesion that frequently occurs on the chest and back, but is also common on the face and periocular region of older individuals (1,2,3,4,5,6,7,8,9,10,11,12,13,14). It develops in hair-bearing areas of skin and does not occur on the palms, soles, or mucous membranes. It is generally a solitary lesion, but multiple lesions can occur and may have an autosomal-dominant inheritance pattern. The sudden appearance of multiple SKs, or rapid growth of pre-existing SKs, may herald the onset of internal malignancy, particularly gastrointestinal adenocarcinomas. This is called the “sign of Leser-Trelat”(5,6).
Clinical Features
Clinically, SK first appears as a minimally elevated hyperpigmented, tan to brown plaque. With time, it may become more elevated, and even assume a dome configuration (1,2,3,4,5). SK can occasionally be more pedunculated and resemble a pedunculated papilloma. Although SK is usually asymptomatic, it can cause pruritus or local irritation, particularly in areas of friction. It usually has a rough surface with irregular fissures. It is usually discrete and movable, and has been compared to a button stuck on the surface of the skin. A clinical variant of SK, known as dermatosis papulosa nigra, is characterized by multiple, deeply pigmented, elevated papules found in the malar region and periocular area in black individuals (7,8).
Differential Diagnosis
Pathology and Pathogenesis
Histopathologically, SK has been classified into six distinct types; many lesions have combinations of these types (10). The acanthotic type is the most common. All types of SK are characterized by hyperkeratosis, papillomatosis, and acanthosis, mainly a proliferation of basal cells. A characteristic feature is the presence of intraepithelial keratin cysts (horn cysts or pseudohorn cysts) that should not be confused with the pearl cysts, which are often present in squamous cell carcinoma. These cysts gradually coalesce and migrate superficially, forming a rough surface to the lesion (3).
The pathogenesis of SK is uncertain, but age, sun exposure, and hereditary tendency may be predisposing factors. SK apparently arises from the follicular infundibulum and seems to involve an aggregation of immature epidermal keratinocytes (10).
Management
Treatment is generally observation or excision, depending on the clinical circumstances (4,11,12,13,14). In the eyelid area, a lesion can be removed for cosmetic considerations or because of interference with wearing of glasses. Removal can be accomplished by curettage, shaving excision flush with the skin surface, or standard full-thickness excision of the skin epidermis and dermis down to the subcutaneous tissue, followed by primary closure. The tarsus does not need to be removed. Light freezing with liquid nitrogen has been advocated for smaller flat lesions (1). There is a slight tendency for local recurrence after excision.
Prognosis
Prognosis for SK is generally excellent, but its uncommon occurrence as multiple eruptive lesions can herald development of gastrointestinal adenocarcinoma (sign of Leser-Trelat) (6). The cutaneous lesion itself probably has no malignant potential.
Selected References
1. Griffith DG, Salasche SJ, Clemons DE. Cutaneous Abnormalities of the Eyelid and Face. New York: McGraw-Hill, 1987:200.
2. Font RL. Eyelids and lacrimal drainage system. In: Spencer WH, ed. Ophthalmic Pathology. An Atlas and Textbook. 4th ed. Philadelphia: WB Saunders; 1996:2229-2235.
3. Kobalter AS, Roth A. Benign epithelial neoplasms. In: Mannis MJ, Masai MS, Huntley AC, eds. Eye and Skin Disease. Philadelphia: Lippincott-Raven; 1996:348-350.
4. Geist CE. Benign epithelial tumors. In: Albert DM, Jakobiec FA, eds. Principles and Practice of Ophthalmology. 2nd ed. Philadelphia: WB Saunders; 2000:3353-3357.
5. Ostler HB, Maibach HI, Hoke AW, et al. Diseases of the Skin and the Eye. Philadelphia: Lippincott Williams & Wilkins; 2004:179.
6. Ellis DL, Yates RA. Sign of Leser-Trelat. Clin Dermatol 1993;11;141-148.
7. Hairston MA Jr, Reed RN, Derbes VJ. Dermatosis papulosa nigra. Arch Dermatol 1964;89:655.
8. Spott D, Wood M, Healon G. Melanoacanthoma of the eyelid. Arch Dermatol 1972;105;898.
9. Foley P, Mason G. Keratotic basal cell carcinoma of the upper eyelid. Aust J Dermatol 1995;36:95-96.
10. Kirkham N. Tumors and cysts of the epidermis. In: Elder D, Elenitsas R, Jaworsky C, et al., eds. Lever’s Histopathology of the Skin. 8th ed. Philadelphia: Lippincott-Raven; 1997:689-690.
11. Scully J. Treatment of seborrheic keratosis. JAMA 1970;213:1498.
12. Beckman H, Fuller TA, Boyman R, et al. Carbon dioxide laser surgery of the eye and adnexa. Ophthalmology 1980;87:990-1000.
13. Doxanas MT, Iliff WJ, Iliff NT, et al. Squamous cell carcinoma of the eyelids. Ophthalmology 1987;94:538-541.
14. Griffith DG, Salasche SJ, Clemons DE. Cutaneous Abnormalities of the Eyelid and Face. New York: McGraw-Hill; 1987:202-203.
Eyelid Seborrheic Keratosis
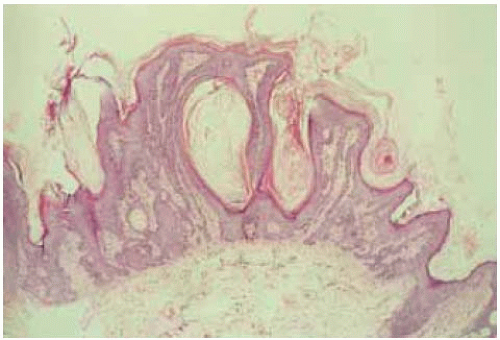 Figure 1.11. Histopathology of hyperkeratotic variant of SK, demonstrating acanthosis and hyperkeratosis. (Hematoxylin-eosin 50.) |
Eyelid Seborrheic Keratosis: Clinical Variations
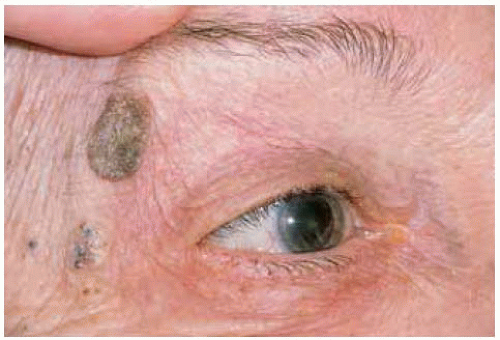
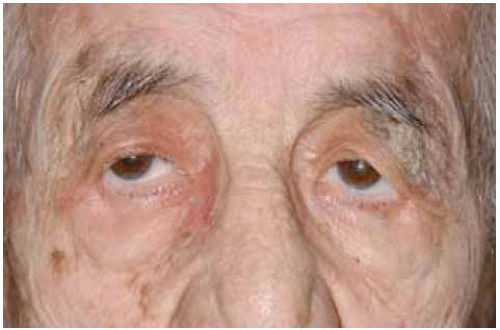 Figure 1.13. Extensive diffuse seborrheic keratosis on left upper eyelid of elderly man. There is a coincidental sebaceous cyst on medial aspect of same eyelid. |
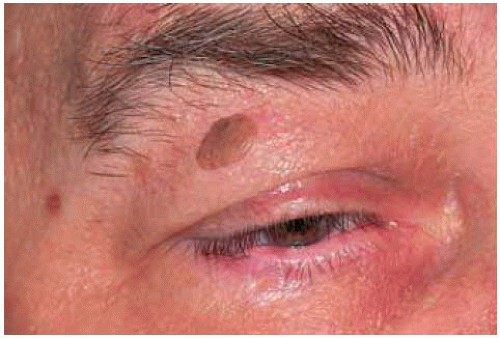
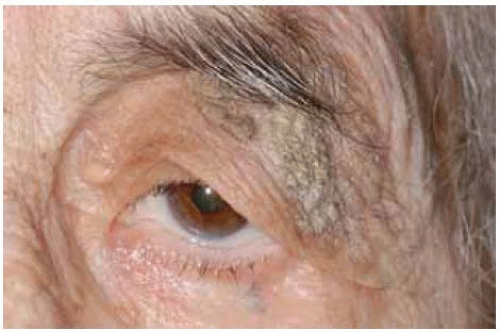 Figure 1.14. Close up view of lesion shown in Figure 1.13.
Stay updated, free articles. Join our Telegram channel
Full access? Get Clinical Tree
 Get Clinical Tree app for offline access
Get Clinical Tree app for offline access

|