Chapter 109 My little girl tells me she sees strange things
Introduction
I have made a short mnemonic which I find helpful when dealing with such cases. “OSCE” stands for:
1. O-ptical (refractive, optic media).
3. C-erebral (neurologic, psychologic/functional, psychiatric.
4. E-fferent (motor, e.g. nystagmus, superior oblique neuromyokymia, or accommodation spasm) causes.
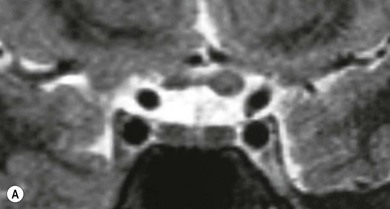
This should ensure the approach to the evaluation of the problem is complete (Table 109.1). This can usually be achieved by appropriate history taking followed by a clinical examination, but may require ancillary investigations and referral to other specialists (Box 109.1). It has to be remembered that not all cases have a definitive diagnosis made (Fig. 109.1) and that even apparently bizarre symptoms can arise from organic disease (Fig. 109.2).
Table 109.1 Systematic approach to children who complain of seeing peculiar things
| Systematic approach (mnemonic “OSCE”) | |
| O-ptical | Refractive |
| Optic media (red reflex) | |
| S-ensory (visual pathway) | Anterior segment |
| Posterior segment | |
| Optic nerve, chiasma, optic tract, visual cortex | |
| C-erebral | Neurologic |
| Psychologic/functional | |
| psychiatric | |
| E-fferent (motor) | Extraocular movement exam (nystagmus, superior oblique myokymia) |
| Lid movements (myokymia) | |
| Accommodation (loss/spasm) | |
Typical peculiar visual complaints are broken up into individual visual symptoms and presented from common to rare. There are excellent reviews of this subject.1–8
Entoptic phenomena
Entoptic phenomena are visual perceptions from sources within the eye rather than the outside world. Most are harmless curiosities which are usually not perceived or ignored, but may be noticed by a bright young child. They are noticed under special viewing or light conditions. Most people will have experienced some of them at some point in their life. Clinicians use them to assess the presence of gross retinal and optic nerve visual function when no direct fundal view is possible due to dense medial opacities. On the other hand, children with very poor sight will often rub and poke their eyes to stimulate entoptic phenomena (oculodigital sign; see Chapter 59).