Chapter 13 Management of the Patient with Atopic Skin Disease
Introduction
Atopic dermatitis, also called atopic eczema or simply eczema, has been described since the days of Hippocrates. Eczema literally means to “boil over.” This is an apt description of the smoldering itch and inflammation that characterize this skin disease. Since the advent of formal diagnostic criteria in 1980, it has become clear that atopic dermatitis is an extremely common, multifactorial disease.1 The cause remains unknown but both genetic and environmental factors contribute to the clinical phenotype. The incidence of atopic dermatitis (AD) is rising globally, and the medical, psychosocial, and financial burden imposed is considerable. While the persistent inflammation and itch often resolve during the childhood years, cutaneous hyperirritability and susceptibility to allergy and infection persist in many. Eighty percent of all patients with occupational skin disease are atopic.2 Longitudinal studies have shown that symptoms of AD recur or persist in up to 60%, implying that we do our patients no favors by asserting that they will “grow out of it.”3
Epidemiology
Atopic dermatitis, along with asthma and hayfever, comprises one-third of the “atopic triad.” Though deemed “atopic” 20–60% of patients do not have IgE-mediated sensitivity to allergens or a positive family history of atopy.4 This led to recent nomenclature revision by the Nomenclature Review Committee of the World Allergy Organization.5 Up to 30% of patients with AD continue the “atopic march” to develop asthma, and 35% will eventually develop hayfever.6 AD is a pediatric disease. Sixty percent are diagnosed by 1 year of age and 90% by 5 years of age. There is no race or gender predilection. The prevalence varies widely from less than 2% in China to greater than 20% in Japan, Australia, and England.7,8 In a study in 2000 of Oregon schoolchildren, Laughter et al found a 17.2% incidence of AD.9 This contrasts with prevalence rates around 5% in the USA in the 1950s. Many candidate genes have been investigated though none explain all cases. Schultz Larsen demonstrated 0.72 concordance in monozygotic twins and 0.23 in dizygotes.10 Children with two affected parents have a 60–80% chance of developing AD. This risk drops with one or neither parent having AD, asthma, or hayfever, and markedly so if there is no atopic family history. In a longitudinal study Ben-Gashir et al noted that children living in an urban area with onset of AD accompanied by asthma, allergic rhinitis, or both during the first year of life, had more severe disease independent of other risk factors.11
Birth order studies have found a higher incidence of AD in first born children. AD rates have also been found to be lower in households with two or more farm animals, and early childhood exposure to typical infections.12 These results have suggested that some degree of exposure to antigen at an early age may induce immunologic tolerance and aid the discriminatory capability of the developing immune system. The “hygiene hypothesis,” which posits that excessively clean environments prevent exposure to such early priming antigens, has been used to explain some of these findings.13,14 These data point to significant environmental mediation of disease expression.
The impact of AD on families is often underestimated. Validated quality of life indices can provide a more accurate assessment of the impact of disease on patients and families.15 An Australian study comparing the impact of chronic diseases on children and families found that caring for a child with moderate to severe AD was significantly more stressful than caring for a child with insulin-dependent diabetes.16 Sleep loss due to itch plays a large part in this daily burden and can have wide repercussions on school performance, interpersonal confidence, social relationships both inside and outside of the family unit, and personal health. Polysomnographic studies have documented frequent nighttime awakening, reduced non-REM sleep, and poor sleep efficiency in patients with AD.17 The out of pocket costs of this disease are comparable to those of asthma.18,19
Classification
Atopic dermatitis has been classified in various ways though the most useful are by severity. Severity can be mild, moderate, or severe based upon body surface area involved, degree of itch, and signs of disease including erythema, papulation, lichenification, and excoriation. Validated scoring instruments such as the EASI (Eczema Area and Severity Index) and SCORAD (SCORing of Atopic Dermatitis) are available but are rarely used outside of clinical trials.20 In a UK survey of 1760 children from 1 to 5 years, 84% were categorized as mild, 14% moderate, and 2% severe.21
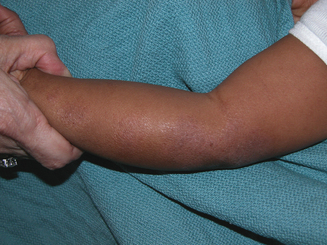
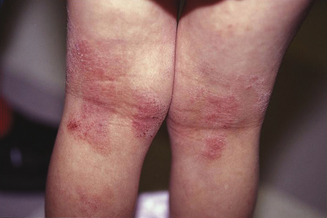
Atopic dermatitis can be categorized based upon age of presentation. Atopic dermatitis can present differently in infants and small children. Infantile eczema, though histologically indistinguishable from childhood and adult eczema, often affects a more extensor and facial distribution (Figure 13.1). Skin folds including the axilla and groin are typically spared in AD, however in infants there is frequent overlap with seborrheic dermatitis which has intertrigenous involvement. As children age the more classic flexural presentation predominates (Figure 13.2). Adult-onset eczema is uncommon and may have more follicular and nummular features.22,23 Other eczema “types” such as “nummular,” “papular,” “follicular,” or “palmoplantar” refer to the prevailing morphology or distribution in a given patient. These subtypes have similar histology and putative triggers.
An older classification scheme, utilized primarily in Europe, describes AD as either extrinsic or intrinsic. Extrinsic AD represents the 60–80% of patients who have an atopic family history, elevated IgE, and positive allergy tests. These patients would qualify as having “atopic dermatitis” under the revised nomenclature described above. The remaining 20–40% do not have these features, though clinically their disease is identical. This population is labeled “intrinsic AD.” These distinctions highlight the immunologically heterogeneous nature of atopic dermatitis.
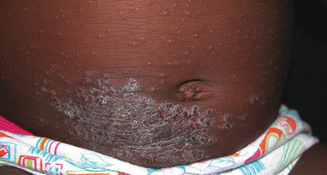
Allergic contact dermatitis, irritant contact dermatitis, and contact urticaria are three related skin conditions that are frequently confused with AD. All three occur with greater frequency in patients with AD, but do not necessarily have the same triggers or natural history. Allergic contact dermatitis (ACD) is a delayed-type hypersensitivity reaction to an external substance. Common causes of ACD in atopic patients include fragrance, nickel (Figure 13.3), latex, lanolin, Neosporin, rubber accelerators, preservatives such as formaldehyde or formaldehyde releasers, parabens, and, rarely, steroid molecules themselves (e.g., budesonide). Contact urticaria is an immediate-type hypersensitivity reaction that presents within minutes to hours after exposure (e.g., fish) and resolves completely within 24–48 hours. Irritant contact dermatitis, a nonimmunologic reaction, is due to either frequent wetting and drying (e.g., perioral rash in drooling infants) without sufficient emollient use, or the harsh effects of certain foods on the skin (e.g., citrus). Each of these conditions present with an itchy rash possibly in response to a food or environmental stimulus; however, treatment and natural history may vary so it is useful to distinguish these different cutaneous reaction patterns from typical eczema.
Anatomy/Physiology
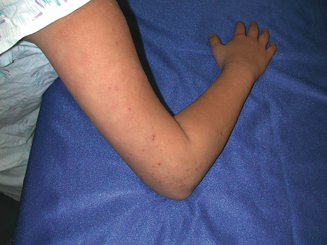
The skin is divided into three layers: epidermis, dermis, and subcutis. Atopic dermatitis is a papulosquamous skin disease and as such affects primarily the epidermis and papillary (superficial) dermis. Related conditions can present with additional findings affecting more focal cutaneous structures. Keratosis pilaris (Figure 13.4) occurs quite commonly in patients with atopic dermatitis and presents with scaly hyperkeratotic papules typically affecting the hair follicles of the upper extensor arms. Keratosis pilaris specifically affects the follicular ostia and adnexal unit, sparing the remainder of the epidermis. Ichthyosis vulgaris affects the stratum corneum or outer layer of the epidermis and the plate-like scale commonly found on the shins reflects this retained, xerotic outer skin layer. Pityriasis alba reflects diminished pigmentation within melanosomes distributed throughout the epidermis, presumably in response to the cutaneous inflammation associated with AD. Less commonly patients with AD develop an ocular deformity called keratoconus. Keratoconus is found in some patients with chronic periocular dermatitis and conjunctivitis. Asthma and rhinoconjunctivitis are also common in patients with AD and are detailed elsewhere.
Pathophysiology
The cause of AD is unknown. In the prevailing model, genetically predisposed individuals develop epidermal inflammation in response to environmental and/or emotional stimuli, presumably leading to the characteristic itch and rash of AD. The final common pathway of all types of eczema histologically is epidermal spongiosis with a mixed lymphohistocytic papillary dermal infiltrate. Cutaneous inflammation in AD is T cell mediated and there are demonstrable barrier and immunologic abnormalities. Patients have increased transepidermal water loss that manifests as xerotic, scaly skin. Biochemical analysis has shown deficiencies in certain components of the epidermal envelope including ceramide. The so-called “acid mantle,” a zone of lower pH found in normal skin that may alter bacterial attachment, is disrupted. Clinically it has long been noted that patients with AD are prone to staphylococcal skin infections whereas patients with psoriasis, another skin disorder notable for an abnormal barrier, are not. It has recently been shown that skin biopsies from lesional AD skin have decreased levels of the innate antimicrobial peptide beta-defensin, in contrast to normal or elevated levels found in lesional psoriatic skin.24 This deficiency could explain the relatively heightened skin infection risk in AD.
In addition to these barrier abnormalities, AD patients have well-described immunologic alterations including elevated IgE and eosinophil counts. AD patients have an abnormal T-helper 2 (Th2) mediated immune response as reflected by increased numbers of specific T cells producing interleukin (IL) 4, IL-5, and IL-13, and diminished interferon gamma (IFN-γ). IL-4 is involved in IgE isotype switching and IL-5 promotes eosinophilia which could explain these clinical features. This Th2 predominance may be due to preferential apoptosis of circulating Th1 cells.25 Skin biopsies have demonstrated elevated IL-4, IL-5, and IL-13 in both acutely affected and unaffected skin.26 Conversely biopsies taken from chronic lesions show increased amounts of IFN-γ, IL-5, IL-12, and GM-CSF (granulocyte macrophage colony stimulating factor).27 The factors governing the evolving inflammatory response have not been elucidated, but the chemokine MIP4/CCL18 may play a regulatory role.28 The clinical significance of this “biphasic” response is unclear but the effector cells appear to be FcRI expressing IgE epidermal dendritic cells including Langerhans cells (LC) and inflammatory dendritic epidermal cells (IDEC), both of which have been demonstrated in lesional AD skin.29
Diagnosis
▪ History
Atopic dermatitis does not usually present a diagnostic challenge. Affected patients typically present in the first year of life with focal or widespread itch and rash. Parents often suspect but cannot pinpoint an association with either a food or environmental trigger. Occasionally there is an obvious association with certain foods such as dairy products or eggs. Parents may report associated sleep loss and irritability. Gastrointestinal symptoms are less common but may present with cramping, nausea/vomiting, diarrhea, or blood in the stool. Particularly in cases of infantile eczema, the possibility of an underlying immunodeficiency must be considered. Several immunodeficiency states including hyper IgE syndrome and Wiskott–Aldrich syndrome may present with intractable eczema. The timing of presentation is similar to typical eczema which may delay diagnosis. Failure to thrive, hair loss, petechiae, or unusual type or number of extracutaneous infections in an infant with severe eczema should trigger a complete immunologic work up. Other differential considerations in this setting include severe combined immunodeficiency (SCID), Bruton’s agammaglobulinemia, and Netherton’s syndrome.30 Box 13.1 outlines a more complete differential diagnosis for AD.
BOX 13.1 Differential diagnosis of atopic dermatitis
Cutaneous T-cell lymphoma (CTCL)
Acrodermatititis enteropathica
When the diagnosis of AD is not clear cut, diagnostic criteria should be considered (Box 13.2). Hanifin described four major criteria including itch, family history of eczema, asthma, or hayfever, typical distribution of either extensor/facial dermatitis in an infant or flexural dermatitis in a child or adult, and a waxing and waning course.1 Three of these four major criteria plus three or more minor criteria need to be present to make a diagnosis of AD. The minor criteria include the related conditions mentioned above (keratosis pilaris, pityriasis alba), physical findings such as lip cheilitis, nipple eczema, xerosis, centrofacial pallor, a distinctive fold beneath the lower eyelids (Dennie–Morgan folds), keratoconus, and white dermographism, as well as serologic abnormalities, elevated IgE, and elevated eosinophil counts that may help when the diagnosis is uncertain. Several groups including a working party in the UK have attempted to modernize the original criteria.31 In addition to establishing a concrete diagnosis, every effort should be made to identify relevant allergic and nonallergic triggers. Foods that are most commonly associated include eggs, cows’ milk, peanuts, soy, wheat, seafood and shellfish. A recent meta-analysis of food sensitization and atopic diseases found few good studies upon which to guide our recommendations from the over 2000 that have been performed. Tarini et al identified nine such studies, five of which had a positive association between AD and early solid food exposure. The other four studies did not identify such an association. The authors concluded that there may be a slightly increased risk of developing AD but not other atopic conditions with early introduction of solid food.32 Zutavern found no increased risk if solids were delayed for 6 months, but could not rule out an increased risk if solid food is introduced prior to 4 months of age.33 Patient history should include family members with atopy, duration of breastfeeding, age of onset of skin disease, maternal and infant diet history, nature of skin reactions suspected in relationship to diet, and response to interventions or withdrawals. All medications should be reviewed. There have been reports of an increased incidence of atopic disease in association with early medication ingestion.34