9 Glaucoma
Anatomy/physiology
Ciliary body (CB)
Functions
Outflow Pathways
Trabecular meshwork (traditional pathway)
The pore size of the meshwork decreases towards Schlemm’s canal:
Angle Structures
Visible only by gonioscopy because of total internal reflection at the air/cornea interface (Figure 9-1)
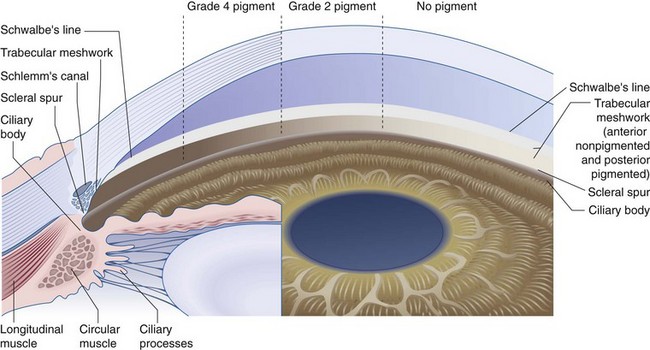
Figure 9-1 Composite drawing of the microscopic and gonioscopic anatomy.
(From Becker B, Shaffer RN: Diagnosis and Therapy of the Glaucomas, St Louis, Mosby, 1965.)
Angle Abnormalities
Cyclodialysis cleft
Optic Nerve (Figure 9-2)
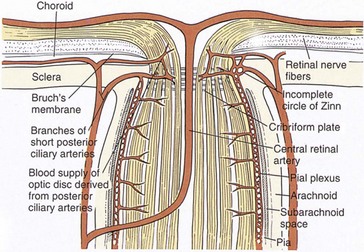
Figure 9-2 Vascular supply and anatomy of the anterior optic nerve.
(From Hart WM Jr: In Podos SM, Yanoff M [eds]: Textbook of Ophthalmology, vol 6, London, Mosby, 1994.)
4 layers of optic nerve head based on blood supply:
Testing
Intraocular Pressure
Goldmann equation
IOP = F/C + EVP relates 3 factors important in determination of IOP
Tonometry
IOP measurement can be performed with a variety of devices (tonometers)
Indentation
Applanation
Gonioscopy
Classification systems
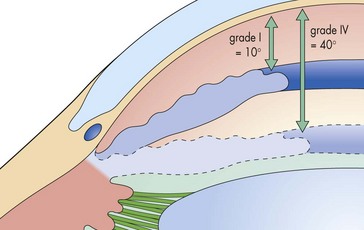
Figure 9-3 Shaffer’s angle-grading system.
(From Fran M, Smith J, Doyle W: Clinical examination of glaucoma. In Yanoff M, Duker JS [eds]: Ophthalmology, 2nd edn. St Louis, Mosby, 2004.)
Visual Fields
Central field tests points only within a 30° radius of fixation
Types
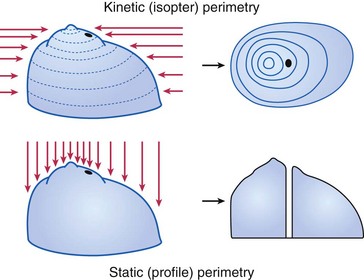
Goldmann (kinetic and static)
Humphrey (static)
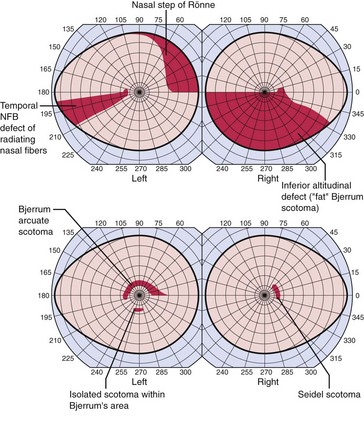
VF defect
a scotoma is an area of partial or complete blindness
Optic Nerve Head (ONH) Analyzers
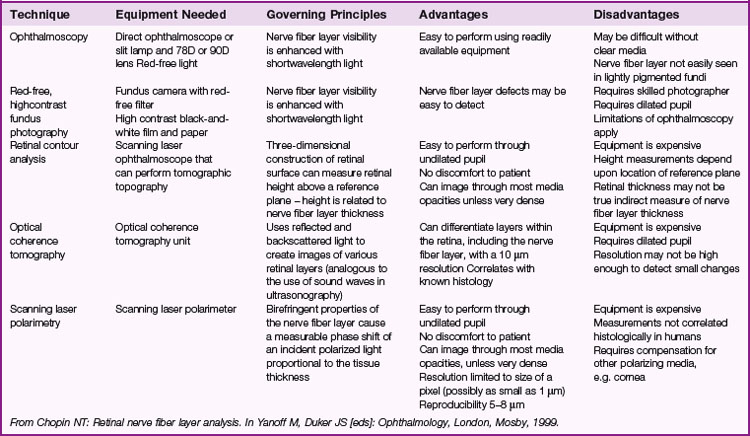
Various digital and video cameras that capture ONH image; computer then calculates cup area in an attempt to objectively quantify ONH appearance (Table 9-1)
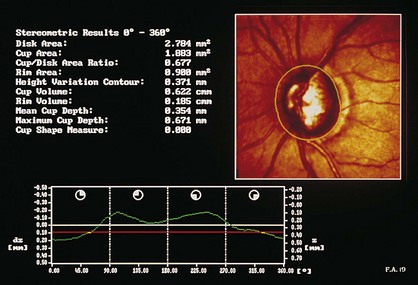
Confocal scanning laser ophthalmoscopy (CSLO; Heidelberg retinal tomograph [HRT]; TopSS)
low-power laser produces digital 3D picture of ON head by integrating coronal scans of increasing tissue depth; indirectly measures nerve fiber layer (NFL) thickness (Figures 9-6, 9-7)
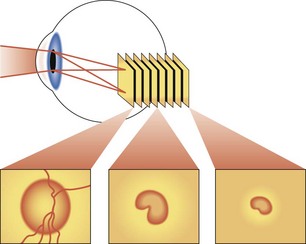
Figure 9-6 Confocal scanning laser ophthalmoscopy.
(Adapted from Schuman JS, Noeker RJ: Imaging of the optic nerve head and nerve fiber layer in glaucoma. Ophthalmol Clin North Am 8:259–279, 1995.)
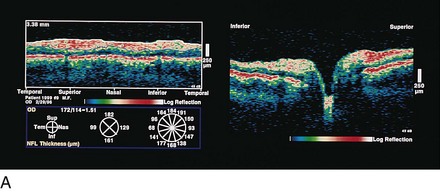
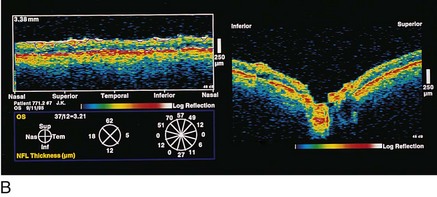
Optical coherence tomography (OCT)
measures optical backscattering of light to produce high-resolution, cross-sectional image of the NFL (Figure 9-8)
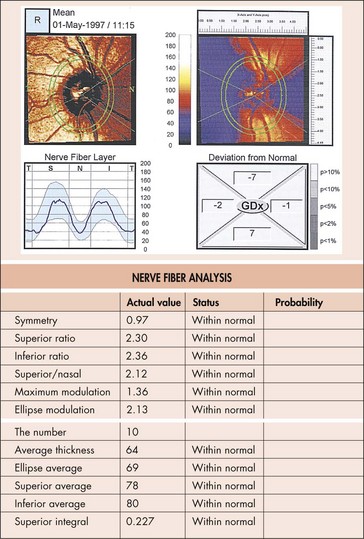
Scanning laser polarimetry (SLP; Nerve Fiber Analyzer, GDx)
uses a confocal scanning laser ophthalmoscope with an integrated polarimeter to detect changes in light polarization from axons to measure the NFL thickness; quantitative analysis of NFL thickness to detect early glaucomatous damage (Figure 9-9)
Pathology
Glaucoma
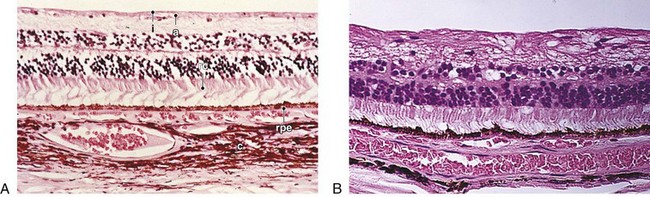
Dropout of ganglion cells, replacement of NFL with dense gliotic tissue and some glial cell nuclei; partial preservation of inner nuclear layer with loss of Müller’s and amacrine cells (normal 8–9 cells high; in glaucoma, 4–5 cells high); earliest histologic changes occur at level of lamina cribrosa; advanced cases may show backward bowing of lamina or ‘beanpot’ appearance (Figures 9-11, 9-12)
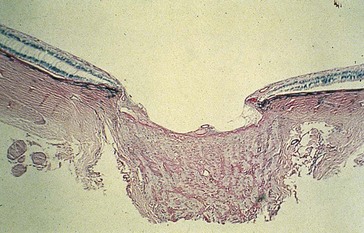
Figure 9-11 POAG demonstrating cupping of the optic nerve head.
(From Yanoff M, Fine BS: Ocular Pathology, 5th edn. St Louis, Mosby, 2002.)