CHAPTER 208 Foreign Bodies of the Airway and Esophagus
Foreign bodies in the airway, pharynx, and esophagus continue to be a diagnostic and therapeutic challenge for practicing otolaryngologists. Despite improvement in public awareness and emergency care, foreign bodies result in approximately 150 deaths per year in children secondary to asphyxiation.1 Most deaths occur before hospital intervention.
Before the 20th century, bronchotomy was the method of choice for airway foreign body removal. Most patients with foreign body aspiration died from the initial event, the attempt at removal, or complications thereof. Although intubation of the airway was suggested at the time of Hippocrates, Killian in 1895 was the first to use a hollow tube to evaluate the tracheobronchial airway.2 He used this technique to remove a bone from the right main bronchus in 1897, becoming the first to perform endoscopic removal of an airway foreign body.
Endoscopic illumination was initially used in esophagoscopy and was incorporated into a bronchoscope by Jackson,2 who revolutionized the field of bronchoesophagography with the development of instruments and techniques for foreign body removal. The principles he and his son developed3 were paramount in reducing the mortality associated with airway foreign bodies and are still the basis of foreign body removal today.
Before the mid-1850s, the most common management for suspected esophageal foreign body impaction was to attempt to push the object into the stomach. Various instruments, including curved hooks, forceps, and even a walking cane, were used. Dupuytren was reported to pinch the neck of patients vigorously to crush a food impaction in the cervical esophagus, allowing it to pass to the stomach.2 The first esophagoscope used in 1890 by Mackenzie was later improved by Jackson, Ingals, and Mosher. The earliest rigid esophagoscopies for foreign body extraction by Jackson and Ingals were performed on awake patients in a sitting position. Because anesthesia risks have decreased, and instrumentation for endoscopic removal of esophageal foreign bodies has improved, these procedures are now performed with the patient supine and under general endotracheal anesthesia.
Epidemiology
The incidence of airway and esophageal foreign bodies has not changed significantly, but the safety in removal has increased dramatically. Most aerodigestive foreign bodies are esophageal—85% as reported by Hsu and colleagues.4 Most airway foreign body aspirations occur in patients younger than 15 years old. In this age group, choking-related episodes treated in the emergency department number approximately 29.9 per 100,000 population.1 The highest incidence occurs between 1 and 3 years of age; 25% of patients are younger than 1 year.5–9 The reasons toddlers are most susceptible are (1) they lack molars necessary for proper grinding of food; (2) they have less-controlled coordination of swallowing, and immaturity in laryngeal elevation and glottic closure; (3) there is an age-related tendency to explore the environment by placing objects in the mouth; and (4) they are often running or playing at the time of ingestion.10 Older children and adolescents may have an anatomic abnormality11 or a neurologic impairment.12 Accidental aspiration or ingestion of objects tends to be twice as common in boys. Vegetable matter is seen in approximately 70% to 80% of airway foreign body ingestions; the most common are peanuts in the United States, watermelon seeds in Egypt,13 and pumpkin seeds in Greece.14 The percentage of aspirated and ingested metallic foreign bodies, especially safety pins, has decreased, primarily because of the widespread use of disposable diapers. Plastic pieces constitute approximately 5% to 15% of airway foreign bodies; plastic pieces tend to remain longer because they are inert and radiolucent.
The most common esophageal foreign bodies are coins (75% of cases).5–9 Meat and vegetable matter impactions are less common in children. Round objects, trinkets, disk batteries, and sharp objects constitute less than 20% of impacted esophageal foreign bodies. The duration of impaction before endoscopic removal is less than 24 hours in most patients, more than 1 week in 6%, and of unknown duration in 10%.6,7
Of patients with multiple esophageal foreign body impactions, 80% have an esophageal anomaly on further evaluation.6 Of patients with recurrent esophageal foreign bodies, 19% have esophageal anomalies that previously required surgical repair.
Location
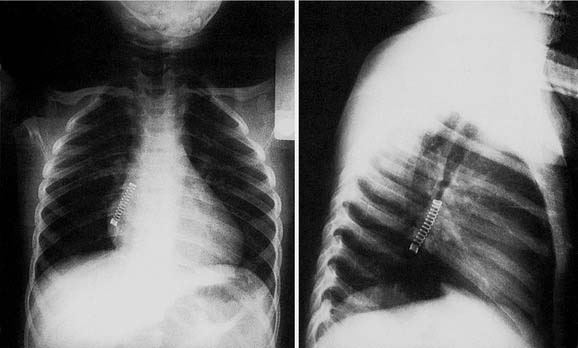
Most airway foreign bodies become lodged in the bronchi because their size and configuration allow passage through the larynx and trachea (Fig. 208-1). Larger objects become impacted in the larynx or trachea, sometimes causing complete obstruction, which is an acute emergency. Bronchial foreign bodies are more common in the right main bronchus in adults, which is thought to be caused by the position of the carina to the left of the midline and its lesser angle of divergence from the tracheal axis.15 Several authors report airway foreign bodies in children with equal frequency in the right and left main bronchi, with no clear explanation for this occurrence.2,16,17
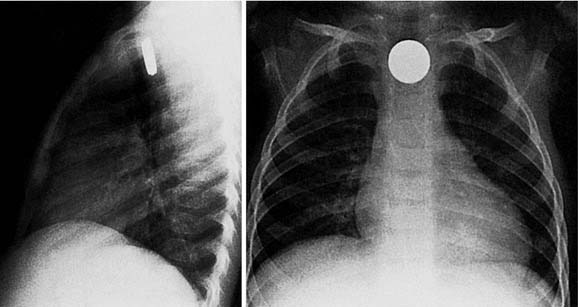
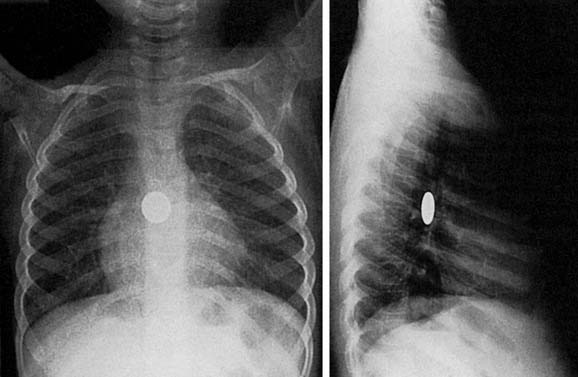
Most esophageal foreign body impactions occur in the cervical esophagus just below the cricopharyngeus muscle (Fig. 208-2).5,6,8 Another 4% to 5% of esophageal foreign bodies become lodged at the midesophagus or distal esophagus, often caused by extraluminal compression by the aortic arch or left main bronchus (Fig. 208-3). Esophageal foreign body impactions also can occur above an esophageal stricture.6
Acute Airway Obstruction
Complete airway obstruction resulting from a foreign body is an absolute emergency. Food (e.g., hot dogs, candies) and nonfood objects (e.g., toys, balloons) commonly become lodged in the larynx and trachea. Increased public awareness, availability of emergency personnel, and the widespread use of the Heimlich maneuver have greatly reduced the mortality of acute obstruction.18 The most important factor in reducing mortality is recognition of the person in acute airway distress. Coughing and gagging indicate partial obstruction. Older children and adults may signal choking by grasping the neck.
The Committee on Accident and Poison Prevention of the American Academy of Pediatrics developed guidelines in accord with the American Red Cross and the American Heart Association for management of choking victims.19 For infants, rescue breaths and chest compressions are recommended. Children older than 1 year require gentle abdominal thrusts while supine. Older children and adults are positioned standing, sitting, or recumbent for the Heimlich maneuver. Back blows or abdominal thrusts in individuals with only partial obstructions could lead to complete obstruction and are not recommended.
Symptoms
There are three clinical phases of foreign body aspiration.15 The initial phase consists of choking, gagging, and paroxysms of coughing or airway obstruction that occur at the moment of aspiration. The choking, gagging, and coughing subside during the asymptomatic phase when the foreign body becomes lodged, and the reflexes fatigue. The asymptomatic phase can last hours to weeks. Complications occur in the third phase, when obstruction, erosion, or infection causes hemoptysis, pneumonia, atelectasis, abscess, or fever.
Laryngeal Foreign Bodies
A foreign body in the larynx may constitute an airway emergency that requires lifesaving first aid before transport to the hospital. Irregular foreign bodies or orientation in the sagittal plane may produce only partial obstruction, allowing adequate air movement around the obstruction. Resulting laryngeal edema can lead to complete obstruction. Typically, these patients have symptoms of obstruction and hoarseness. Some symptoms can mimic croup.3 Delayed diagnosis may lead to complications.
Tracheal Foreign Bodies
Patients with tracheal foreign bodies are seen in similar fashion, but typically do not have hoarseness. Jackson and Jackson3 described three signs associated with tracheal foreign bodies: the “asthmatoid wheeze,” the “audible slap” produced from foreign body contact with the trachea, and the “palpable thud” over the trachea. As with laryngeal foreign bodies, edema can progress to complete obstruction.
Bronchial Foreign Bodies
Of airway foreign bodies, 80% to 90% are found in the bronchi.20 These patients typically have a triad of cough, wheezing, and decreased breath sounds. One large series reported that 65% have the classic triad,17 but 95% have at least one finding.16
The asymptomatic phase may give a false sense of security that the problem has resolved and lead to a delay in diagnosis. Chest auscultation may reveal decreased breath sounds or wheezing. Sudden onset of wheezing is particularly suggestive of a bronchial foreign body, especially if unilateral, but may be a subtle finding.21 Occasionally, bronchial foreign bodies can cause respiratory compromise as a result of swelling of dried vegetable matter (e.g., dried beans and peas) or edema around the object, producing complete obstruction and lobar collapse. Movement of the foreign body from one main bronchus to the other produces respiratory distress, resulting from obstruction of the previously normally ventilating lung.
Esophageal foreign body impaction is most frequently associated with vomiting, odynophagia, dysphagia, and ptyalism.5–8 If the ingestion is witnessed, gagging or choking may be reported. A large foreign body may cause symptoms of airway obstruction and cough caused by compression or irritation of the upper airway. In long-standing esophageal foreign body impaction, fever and other symptoms of respiratory infection may be present.6
Radiographic Evaluation
Laryngotracheal Foreign Bodies
Airway films—high-kilovolt posteroanterior and lateral soft tissue radiographs of the neck—are the radiographic examination of choice to identify laryngeal and tracheal foreign bodies. Chest radiographs are ordered before intervention. Neck films may show subglottic narrowing. Esclamado and Richardson20 reported that 92% of patients with tracheal foreign bodies had abnormal neck radiographs, whereas 50% had normal chest films. When such children do not respond rapidly to medical management, foreign body aspiration must be ruled out.
Bronchial Foreign Bodies
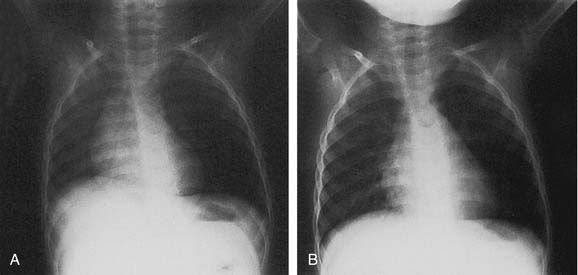
During normal respiration, the airway dilates with inspiration and contracts on expiration. This respiratory cycle can be altered by the presence of bronchial foreign bodies.22 Small objects may cause no radiographic abnormalities. Foreign bodies that obstruct mainly on expiration generate a check-valve effect, resulting in hyperinflation of the affected side and mediastinal shift to the opposite side (Fig. 208-4). This is a typical early finding. A ball-valve effect is produced later when foreign bodies obstruct on inspiration and open on expiration, producing atelectasis on the affected side and a mediastinal shift toward the affected side (Fig. 208-5). When the object completely obstructs the bronchus, a stop-valve effect occurs, leading to consolidation of the lobe involved.
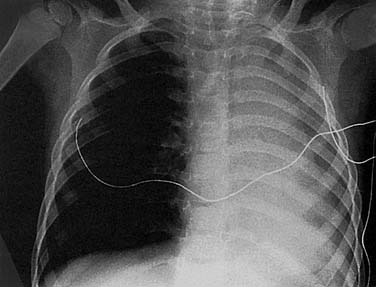
Figure 208-5. Anteroposterior chest film of left lobar collapse secondary to candy corn in the left main bronchus.
Inspiratory and expiratory chest films can aid in the diagnosis, showing hyperinflation on expiratory films or atelectasis on inspiratory films. In younger children who cannot cooperate, lateral decubitus films may help. The dependent lung should collapse normally, but remains inflated in bronchial obstruction. Fluoroscopic evaluation is of little benefit; decreased diaphragmatic movement on the side of the obstruction is helpful in only 50% of cases.16 Simultaneous biplane fluoroscopy is used for extraction of radiopaque foreign bodies in the lung periphery.
Radiographic findings often suggest but do not diagnose foreign body aspiration. Asthma and mucous plugging can simulate foreign body aspiration. Mu and associates23 reported that 35% of patients having normal radiographic studies were later found to have bronchial foreign bodies. Other studies show the lack of sensitivity or specificity of radiographs in diagnosing airway foreign bodies.24,25 In cases of suspected foreign bodies, endoscopic evaluation is important because negative radiographs are not enough to rule out the presence of a foreign body.24