Flaps, Grafts, and Alloplastic Materials in Lid Reconstruction and Repair
W. Jackson Iliff
Elba M. Pacheco
This chapter was conceived to supplement the other excellent chapters in this text on lid reconstruction and orbital surgery by supplying some additional ideas and resources for the management of lid defects. Although it is not encyclopedic in scope, we hope it will supply both basic and more advanced techniques currently available that will improve our flexibility in difficult situations. Reports of new procedures appear at regular intervals. Most are based on the basic principles and techniques presented here. Some may go on to wide acceptance. Others, though occasionally useful and inventive, will remain as isolated case reports.
There are, of course, many ways to reconstruct a lid defect. Some can be repaired with flaps only, others with a combination of flaps and grafts, perhaps with the addition of alloplastic materials. Each individual reconstruction requires careful planning. Hopefully this chapter will supply alternatives. However, the goal is not to lead the surgeon step by step through each technique, although some will be illustrated. Basic suturing techniques and wound closure will not be covered. Instead, this material should lead, when necessary, to the appropriate resources in this or other texts or the original literature.
In association with planning the exact procedures necessary to reconstruct a given defect, a review of lid and adjacent anatomy, as well as anesthesia considerations and applicable general surgical ones is appropriate. Other chapters in this text cover general and local anesthesia1 and provide a good review of the anatomy.2,3 Other texts on oculoplastic surgery also provide expanded treatments of these topics, including harvesting some of the grafts to be mentioned here.4,5,6
FLAPS
A flap is a tissue structure, usually skin, or a combination of skin and muscle, that is relocated from its original site. In the lid, flaps may also include tarsus and conjunctiva as well as skin and muscle. The blood, and possibly the neural supply, remain intact and are not interrupted during the transfer. The recipient bed does not initially contribute to its nourishment. In the lids, the rich anastomosing network of vessels improves flap survival. Random flaps are generally dissected and moved more or less perpendicular to their blood supply or without regard to it; thus, they are more poorly vascularized than axial flaps, which are elevated parallel with and incorporate the supplying vessels. It is generally said that a random flap length may not exceed four times its width. In the early days of tissue transfer, without benefits such as microsurgical techniques and antibiotics, a one-to-one ratio was recommended, to be exceeded only if a vessel (thus an axial flap) was included in the dissection. In the lid, long flaps from the upper to lower lid, for instance, are truly part flap and part free graft, since these principles are routinely exceeded. So-called free flaps are not routinely used in lid reconstruction but may be in more complex facial, orbital, and maxillofacial procedures. Free or microvascular flaps are, in essence, free grafts that incorporate both an artery and vein, which are reanastomosed microsurgically to corresponding vessels in the recipient area, thus becoming tissue transferred with a direct vascular supply at the close of the procedure.
Skin, myocutaneous, and tarsoconjunctival flaps are most often used in lid reconstruction or for filling partial-thickness defects. Skin and myocutaneous flaps usually can supply tissue coverage for the entire anterior lamellae of the lid and can support grafts to the posterior portion of the lid. Tissue grafts or alloplastic materials can be used to add structural support under a flap during eyelid or orbital reconstruction. Mucosal flaps with or without tarsus may conversely rebuild the posterior lid and support a free skin graft anteriorly.
In addition to vascular supply, flaps are characterized by their shape. Four types are described: sliding, advancement, rotation, and transposition. A sliding flap is generally random (dissected without regard for the blood supply) and involves simple undermining of the area surrounding a defect to allow primary closure. The orientation of the flap is selected based on scar alignment. The skin and subcutaneous tissue is “slid” into position. An advancement flap is a more complicated flap in that the tissue to be “advanced” is incised on three sides to allow greater mobility. Closure is primary and generates no secondary defect. Examples include the Cutler-Beard flap to reconstruct the upper lid and the Hughes tarsoconjunctival flap for lower-lid repairs (discussed later.) The rotation flap is similar to an advancement flap in its basic construction in that a three-sided incision and elevation of tissue is performed. However, the defect to be filled is adjacent to the side of the flap rather than at its end, so that the flap is “rotated” into the defect. In doing so, a secondary defect is created opposite the primary. The secondary defect may be closed with a number of techniques, including primary closure if small enough, by developing sliding flaps (further undermining) perhaps with excision of small amounts of additional tissue to produce tension in a different direction, by additional smaller flaps or by a skin graft. Examples include the Tenzel semicircular flap and the Mustardé cheek rotation flap (both are discussed in more detail later in this chapter). The transposition flap moves tissue to a nonadjacent site. Small transposition flaps, like small rotation and advancement flaps, may be random. Larger (i.e., longer) flaps, as in the midforehead, more often need axial design for proper survival. Examples of transposition flaps are simple Z-plasties, rhomboid flaps, bilobed flaps, and the tarsoconjunctival flaps described by Hewes and Leone (see “Marginal Defects” section).
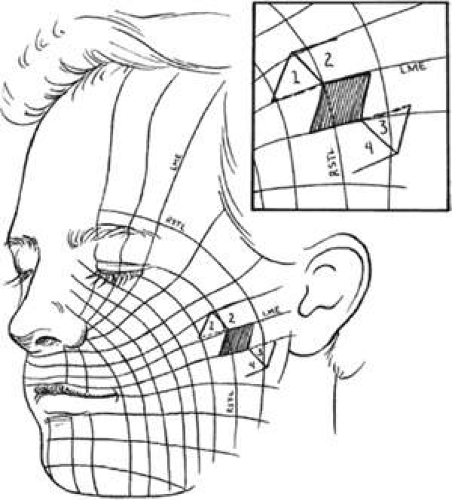
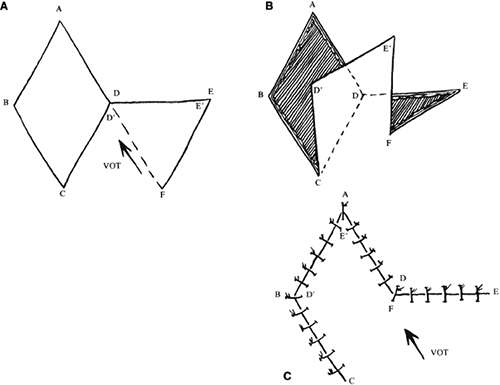
Optimal incision placement and flap design hinge on several important general considerations. The concept of the relaxed skin tension lines (RSTL) (Fig. 1) or Langer lines helps incision placement.7 Wrinkles and skin creases generally develop parallel to these lines as a result of the action of underlying musculature. Incisions ideally should be placed in pre-existing creases because they are best hidden in these areas and avoid development of scars that may be more visible. If placement within a crease is not possible, they should be parallel to the RSTL. The lines of maximum skin extensibility (LME) are perpendicular to the RSTL. The skin is most extensible (i.e., available for sliding, transposing) in the direction of the LME. Vectors of tension should be parallel to the LME. However, the LME in the lower eyelid is vertical and presents a special challenge during reconstruction. Balancing of horizontal and vertical forces is crucial to avoid retraction or ectropion. Once the possible graft or flap donor sites are identified (there are usually several), the site with the most available skin is identified by pinching it up and pushing and pulling the surrounding structures to judge possible distortion caused by closure. For instance, significant lower lid ectropion might be caused by one donor site and avoided by an alternate. This should be kept in mind when designing flaps and will be expanded further in the discussion of rhomboid flaps.
Defects That Do Not Involve the Lid Margin
The most common method of closing a skin defect is simple direct closure, perhaps with just a little undermining. Undermining produces a sliding flap. However, when the size of a defect or its proximity to another vital structure, such as lid margin, punctum, or canthus, makes primary closure difficult or produces an unwanted side effect, such as ectropion or lagophthalmos, a flap closure may be appropriate. Alternatively, skin grafts can be used and may be preferable, in difficult-to-close areas, such as the medial canthus. Lid skin, being thin and elastic, often allows direct closure with sliding or simple rotation or advancement flaps. Cheek and brow skin is much thicker and less mobile, requiring more extensive undermining and more frequent transposition.
Z-Plasty
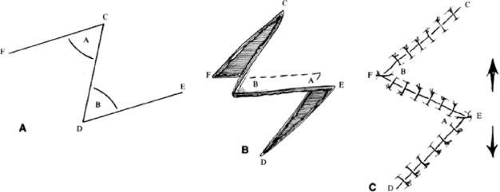
Z-plasty (Fig. 2), (as well as V-Y and Y-V) is one of the most basic techniques: it may be used in many simple as well as more complicated repairs. Z-plasty employs transposition of two flaps of skin, to elongate the skin along a given axis. Z-plasty involves marking and dissecting two triangular flaps, which are transposed. The center of the Z (Fig. 2 line CD) is aligned on the axis of an area to be lengthened (such as a contracted scar). Each arm of the Z is equal in length and forms angles from 30° to 90°, with angles of up to 60° being the most useful. Larger angles provide the most lengthening but are technically more difficult and are rarely useful. The greater the angle, the greater the percentage gain in length along the central axis; the longer the central member, the greater the actual increase in length.6(p14) A Z-plasty, in addition to being used in other reconstructions, can be used to lengthen a contracted scar, to realign a scar to fall in natural folds (along RSTL), or to make the scar less conspicuous by interrupting its continuity. Long scars can be revised by multiple Z-plasties along their length. Malpositioned structures, such as the brow or canthus, may be repositioned by including them in one of the flaps of a Z-plasty. Congenital epicanthal folds (see discussion later in this chapter) are also amenable to reconstruction by Z-plasty.
V-Y- and Y-V-Plasty
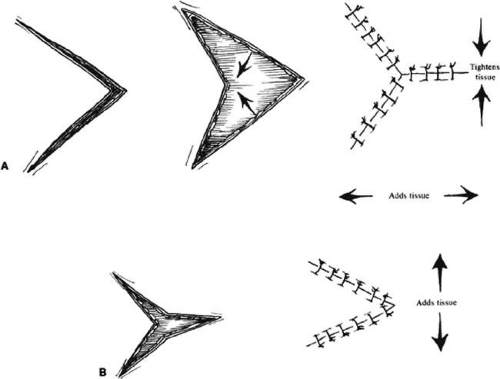
The Y-V and V-Y flaps (Fig. 3) are sliding flaps that also may be combined with other techniques. They may be used to close the donor site of another skin flap or to relieve tension on the lid margin, as from a tight scar. The flap is developed by making a V-shaped incision and recessing the central flap, closing to form a Y (Fig. 3A) or reversing the process by making a Y-shaped incision, advancing the flap to close as a V (Fig. 3B). The Y-V flap by itself or in combination with techniques such as the five-flap procedure (discussed later) can be useful in correction of epicanthal folds.
Subcutaneous Pedicle Flaps
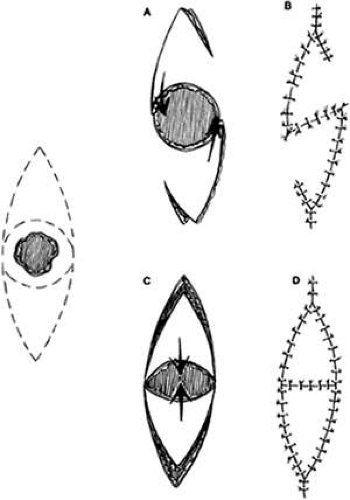
The subcutaneous pedicle flap is a flap of skin that is totally divided from surrounding skin but is left attached to the subcutaneous tissues for its blood supply. Adequate mobilization of the pedicle may allow greater mobility of the skin, and this flap usually combines the technique of V-Y closure. It may be used to close a number of defects in a fashion similar to the V-Y-S flap (Fig. 4A and B) described in the paragraph on medial canthal defects. The flap is elevated by incising all sides of a triangle and gently mobilizing the deep tissues. The skin may then be advanced to fill a defect, with closure of the secondary defect directly (Fig. 4C and D). Two opposing flaps may be elevated for larger defects. With adequate design, flaps such as the V-Y glabellar flap and variations of the median forehead flap (see “V-Y Glabellar Flap” section) can be developed with a subcutaneous pedicle and advanced to fill medial canthal, lower-lid, or cheek/nasolabial defects. This has the advantage of a one-stage procedure with a flap that can be shaped to lie flat without “dog-ears” of skin. The pedicle must be long enough to reach the recipient site without tension or kinking and to provide vascular elements sufficient to sustain the flap.8
Rhomboid Flaps and Variations
The rhomboid flap7 is very useful for reconstructing cheek defects. It can also be used with some medial canthal or brow and temple sites. Because the flap has a precise geometric design, its principles help us to understand the principles of flap design and transfer, and to execute other transposition flaps. Because of the rich vascularity of the cheek and relatively little concern of viability, random pattern flaps are the rule. They are raised at the level of the subdermal plexus, leaving a layer of subcutaneous tissue attached to the skin. Transposition skin flaps, such as the rhomboid flap, are designed adjacent to the defect and share all or part of one side of the defect.
The flap shapes may vary, for instance being oval rather than rectilinear, but can be thought of as having two sides, a distal end and a base. If spacing and lesion shape allow, and excessive removal of normal skin is avoided, the rhombic shape is marked around the lesion with two sides parallel to the LME. These lines run perpendicular to the RSTL (Fig. 1). As will be seen, the vector of traction will be roughly parallel to the LME if well constructed (Fig. 1 inset, Fig. 5), producing the easiest closure. The flap is ideally drawn with all sides and the short diagonal (Fig. 5A line D′F) equal in length. Essentially, the flap design represents two equilateral triangles base to base. The distal end of the flap (Fig. 5A line D′E′) forms a straight line extension of the short diagonal of the defect (Fig. 5A points BD). The sides of the flap, the edges of the defect, and the continuation of the short diagonal are all of equal length.
There are four possible donor sites for any given rhomboid defect, two on each side of the defect on the extension of the short diagonal. These can be mentally drawn on the defect to decide which is best (Fig. 1 inset). The vector of tension (VOT) is roughly parallel to the short diagonal of the flap (Fig. 5A). If the defect is properly positioned with two sides parallel to the LME, the VOT of two of the possible four flaps will be parallel to the LME (Fig. 1 inset: dotted lines, flaps 1 and 3). The other two possible flaps will have VOT roughly perpendicular to the LME or close to parallel to the RSTL, which is an undesirable condition (Fig. 1 inset: flaps 2 and 4). Either of the preferred flaps can be used, but proximity to other structures will usually make one preferable over the other. The surrounding skin is pushed, pinched, or pulled to assess the possible distortion produced by each flap and the most advantageous one picked.
The near corner of the flap base is adjacent to the defect (Fig. 5A point C). The far corner of the flap base is called the pivot point of the flap (Fig. 5A point F), and it is located the width of the flap away from the near corner. The pivot point in a classic transposition flap does not move, but this requires a longer flap for closure. However, with this type of rhomboid flap, the pivot point moves toward the junction of the short diagonals of the defect and the flap (Fig. 5A point D). This facilitates closure of the donor defect and eliminates the need for a longer flap. If there is adequate tissue and the flap is well designed, it closes nicely with little tension, and the VOT is parallel to the short diagonal of the flap (Fig. 5A pointsD′F). However, as is sometimes the case, the pivot point is not mobile enough to close the defect easily. In that case, the junction point of the short diagonals (Fig. 5A point D) must move toward the pivot point. For this to occur, a near side of the defect (Fig. 5A line AD) must elongate, the end of the defect (Fig. 5A point A) must move toward the pivot point (which tends to widen the defect), or the far side of the defect (Fig. 5A line ABC) must move toward the flap. These movements change the shape of the defect and the flap and will induce a second VOT in the axis of the short diagonal of the flap (Fig. 5C pointsD′F) as it is sutured in place. If this is excessive, flap viability is compromised.7 In addition, if the far side of the defect moves, it may distort adjacent structures, which is also undesirable; however, undermining the far side of the defect may allow closure with less tension if the pivot point is poorly mobile.
If the VOT is not ideal, it can be changed somewhat by extending or shortening the far side of the flap. By extending the far side of the flap (Fig. 5A line E′F), the pivot point is moved more toward the long axis of the defect (Fig. 5A points AC). As the pivot point moves, the VOT becomes more parallel to the long axis of the defect, and there is less tendency for the defect to widen. However, this also moves the pivot point (Fig. 5A point F) farther away from the junction of the short diagonals (Fig 5A point D), making it more difficult to close the donor defect.
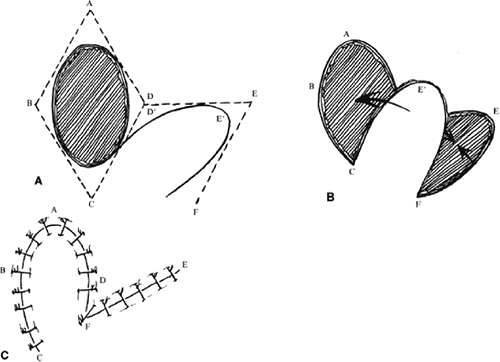
The concepts of the rhomboid flap may also be used with round, oval, and teardrop-shaped defects. For instance, with an oval defect, a rhombus may be drawn around the defect, the flap marked, and then an oval flap designed within the rhomboid to be transposed in a similar fashion (Fig. 6). The principles are the same. In this setting, however, there is somewhat more flexibility in the length of the far side of the flap and its angle with respect to the long axis of the defect. As noted, this allows some modification to the VOT. A longer far side of the flap (Fig. 6B line EF) and greater angle between the axis of the flap and the axis of the defect produce a VOT more parallel to the long axis of the defect. As seen in Figure 6A and B, the angle between lines AC and EC can be changed with oval defects, in contrast to true rhomboids. As the long axis of the flap rotates, the VOT rotates in the same direction. A VOT more perpendicular to the axis of the defect produces a tendency for the defect to increase in width with closure. A VOT more parallel tends to pull downward on the proximal side of the defect without tending to widen it.7
Bilobed Flaps
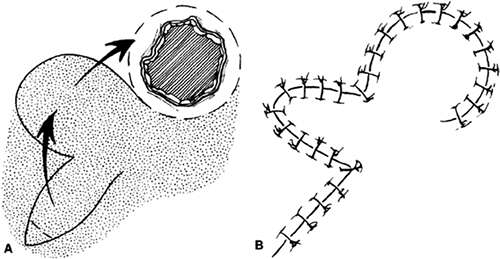
An additional variation on the rhomboid theme is the bilobed flap (Fig. 7). This flap can be used when it is believed that the flap necessary to close a given defect will leave a donor site too large to close primarily. An additional, smaller (about one half) flap is elevated adjacent to the donor defect and rotated at the same time, leaving a smaller secondary donor defect, which can be closed primarily. This can be used multiply in some areas of thick, inelastic skin, such as around the nose.
V-T Closure
Harvey and Corin9 described a simple closure of skin defects not involving the lid margin or lashes. In the typical case of a tumor overlying the tarsus, the lesion is excised by producing a base-up triangle. An infralash incision is performed medially and laterally, extending the base of the triangle as necessary with undermining to allow rotation of skin flaps into the defect. Closure gives horizontal rather than vertical tightening and produces little vertical scarring forces. Lesions close to the lid margin are effectively removed in cases where a vertical ellipse, an alternative closure, may be difficult.
Other
Larger defects in the anterior lamellae, both superior and inferior, can be closed with larger advancement myocutaneous flaps, as described by Anderson and Edwards.10 In the upper lid, they used classic advancement flaps, which may include portions of the brow if necessary to fill upper nasal brow defects. The flap is dissected widely and extends far temporally to allow sufficient advancement. In the lower lid, the flap has similar features to the Mustardé flap in that dissection can be carried temporally as far as the ear if necessary. In this case, however, only the anterior skin-muscle lamellae are moved. Flaps of this type can cover large defects if adequately developed.
Marginal Defects
Marginal defects can be traumatic in origin, such as from severe motor vehicle accidents with loss of tissue or from human, dog, or other animal bites. More commonly, perhaps, they are the result of excision of malignant tumors.
Techniques vary somewhat for upper and lower lids and depending on whether they are nasal or temporal. A combination of two or more may allow closure of a defect in a more advantageous way than a single one, even though the final result may be similar. For instance, a large (greater than 50%) defect in the nasal lower lid too large to be closed by a Tenzel semicircular flap11,12 might be closed by a Hughes-type tarsoconjunctival flap with a skin graft. This requires closing the central visual axis for up to 4 to 6 weeks (see later discussion.) This is undesirable, especially if it involves the only seeing eye. An alternative would be to use a rotation flap of the remaining lower lid moved nasally by performing a lateral canthotomy and cantholysis, thus creating a secondary defect laterally. The secondary defect may then be reconstructed with a rotation flap of tarsus and conjunctiva and a skin flap or graft from the upper lid. This produces a somewhat less objectionable lateral tarsorrhaphy, which will not obstruct vision as much and can be opened at a later time. As will be discussed further on in the chapter, Jordan et al.13 believe that nearly any defect bordered by remaining tarsus may be closed by their technique, which is a modification of the Tenzel flap. Yet a better approach might be a transposition flap of tarsus and conjunctiva from the upper lid, with a transposition skin flap or graft from the upper lid producing a reconstruction with no tarsorrhaphy.14,15 These techniques will be briefly illustrated, but there are many possible combinations to fit differing lids, locations, and sizes of defect.
We recommend becoming familiar with lateral and medial tarsal strip procedures and their modifications, as described by Anderson16,17 and others.18,19 These procedures are useful in a wide variety of oculoplastic operations, especially in some reconstructions. Direct closure of a lid defect has numerous advantages, including lack of obstruction of visual axis caused by sharing techniques, no need for tarsal substitutes (see grafts and alloplastic materials), no need for multistage procedures, a less complicated and quicker surgery, and good cosmesis. However, many times more complicated procedures are necessary.
Sliding/Rotation Flaps
Canthotomy and Cantholysis
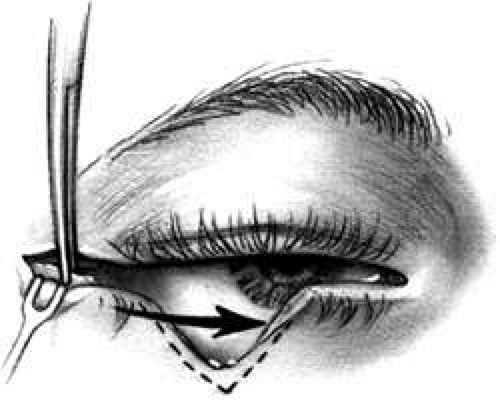
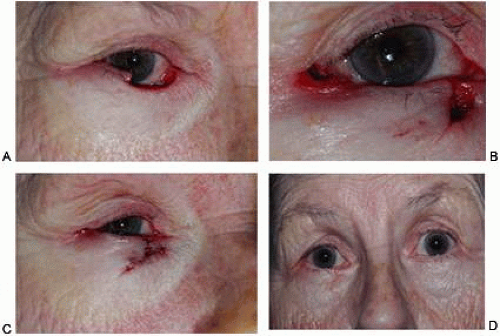
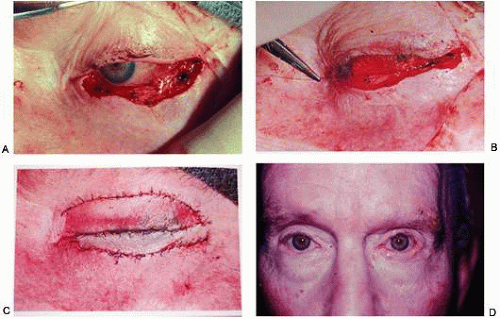
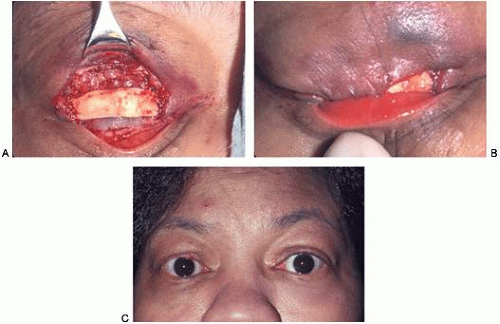
Lateral canthotomy and cantholysis, which can be applied to either the lower or upper lid, is probably the most useful technique in lid repair when simple primary closure is inadequate. This will allow closure of defects of 25% to 40% or slightly more if the lid is particularly lax. (Figs. 8 and 9A). The procedure is simple and is performed with straight, fairly heavy scissors. They are placed horizontally at the lateral canthal angle, and the skin, tendon, and conjunctiva are divided. If fine enough, these same or a smaller pair of scissors is placed on the tendon between the skin and conjunctiva superiorly or inferiorly, and the tendon is divided down to the orbital rim (Fig. 8). The lid can be felt to release and slide nasally when the tendon is completely divided (Fig. 9B). There are often several strands that fan inferiorly that need to be cut for complete release. If conjunctiva is divided, it can be closed or the open area left to re-epithelialize. The skin is closed laterally at the canthus (Fig. 9C). Many defects can be closed with this simple technique, which gives excellent cosmetic results (Fig. 9D).
If a canaliculus is nonfunctioning and can be sacrificed, a medial canthotomy and cantholysis can be performed in selected cases.20 This can also be combined with a similar lateral procedure to allow closure of central defects without sharing procedures or grafts.
Tenzel Rotation Flap
In the mid to late 1970s, Tenzel11 and later Tenzel and Stewart12 described the semicircular flap to reconstruct the central one half of the lid. The results of earlier operations in this area were not as satisfactory as the results with the Tenzel technique, which has since become popular. Jordan et al.13 reported on some modifications of this technique in a medium-sized series. They found that they were able to close defects of 50% to 70% of the central and medial margin and defects of almost any size if medial and lateral stumps of tarsus remained. Their modifications involve making a more vertical incision at the canthus, more extensive undermining laterally, and if necessary, division of the conjunctiva and lower-lid retractors to allow further mobilization of lid remnants. Their extensive lateral dissection has the disadvantage of possible injury to the facial nerve (cranial nerve VII).
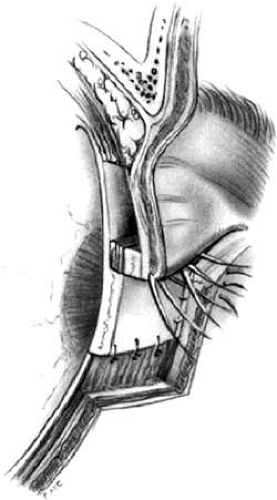
The semicircular flap technique as originally described11 involves making a skin and muscle incision at the lateral canthus, which curves superiorly and temporally in a semicircular fashion (Fig. 10). A lateral canthotomy and cantholysis are performed to slide the lateral portion of the lid nasally. Of course, this assumes there is a remnant of tarsus available laterally. If there is not, other procedures may be used, such as a sharing procedure from the upper lid with advancement or transposition flaps or a graft. Closing the primary defect with standard techniques may require removing a piece of conjunctiva inferiorly under the primary defect. Tenzel suggested using this tissue to reline the flap laterally. The semicircular skin flap stretches and moves into the area vacated by the tarsal remnant and forms the anterior lamellae of the lid in that area. With slight undermining and sliding, the semicircular flap temporally can be closed primarily. Small dog-ears (Burows triangles) of skin may need to be removed to achieve a flat closure.
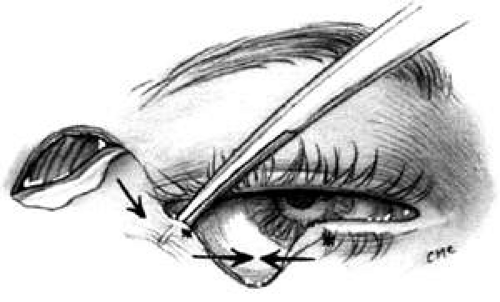 Fig. 10. Tenzel semicircular flap for closure of lower-lid defect. Inferior cantholysis to slide lid nasally. |
Especially with larger defects, the modification by Jordan et al.13 wherein they suggested a more vertical incision and inclusion of additional deep muscle by making a beveled incision would seem to provide some advantage and more lateral support to the new lid. However, the more extensive lateral dissection has the disadvantage of risking injury to the facial nerve. Indeed, as they pointed out, with larger procedures this becomes very similar to the well-known Mustardé rotation flap21 (see next section), although the dissection is more superior (temporal area rather than cheek).
As with the Tenzel11,12 flap, the modification of Jordan et al.13 can be used with upper-lid reconstructions as well. The semicircular flap or vertical incision is made inferiorly instead of superiorly, the superior limb of the canthal tendon is divided, the lid remnant is moved nasally, and the skin muscle flap is used to reconstruct the lateral portion of the lid. Careful closure laterally to reattach the new portion of lid to the remaining tendon of the lid is important for support and redevelopment of the canthal angle.
Jordan et al.13 also pointed out that their technique ends with apparent excess of tissue at the lid margin in the reconstructed area. This tissue will contract and smooth with time, which may help prevent a lid notch. With large defects, other procedures may be combined with the Tenzel-type flap. McCord et al.22 suggested the addition of a periosteal flap elevated from the lateral orbital rim to support the lateral part of the lid. Careful placement of this flap gives good upward support to the lateral lid. A strip about 5 mm in width, with a length appropriate for the defect size, is elevated from the rim and hinged at the orbital rim. It is sutured to the lid remnant nasally and effectively produces a new canthal tendon. The anterior lamella is reformed by the semicircular flap. The inner aspect is lined with elevated conjunctiva. If a large lateral defect is present, an ear cartilage graft (or, for that matter, a nasal chondromucosal, hard palate mucosa, or tarsoconjunctival flap or graft) can be used to reform the inner lamella laterally, with the semicircular flap to reconstruct the anterior lid. Both these modifications can be used with lateral defects that extend to the canthus, where there is no tarsal stump to advance.
Mustardé Cheek Rotation Flap
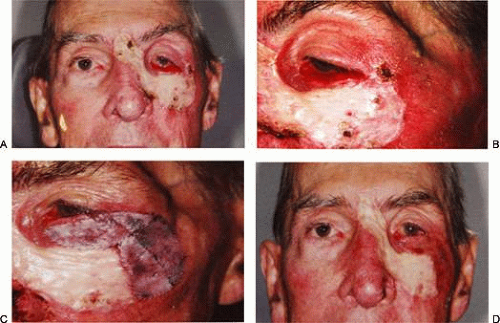
The Mustardé flap4,5,21 has the reputation of being a major operation. If necessary, it can be used to close big defects that are difficult to manage by other techniques. Although we perhaps see very large primary tumors less frequently now than in the past, recurrent lesions (especially morphea-type basal cell carcinoma) can be widespread by the time they are detected, resulting in large defects at the time of removal. Large skin grafts require the use of less than optimal donor sites (see “Grafts” section) or two or more sites. If possible, split-thickness grafts should not be used on the lids or face to avoid contraction (Fig. 11) (see section on split thickness skin grafts later in this chapter). A large flap, with grafts for the posterior lamella, may therefore be the best option and can give satisfactory results when well performed. However, the cheek rotation flap has the inherent disadvantage of producing an inferior vector of traction during healing, which is aggravated by gravitational forces; this makes ectropion or lid retraction with scleral show more likely. Other disadvantages include a large scar and the possible necessity of excising considerable amounts of normal tissue, since in addition to the lid defect from primary tumor excision, a large superiorly based triangle of skin with the nasal edge at the nasolabial fold will also need to be excised. However, Rao and Frank23 used this triangle of skin to fill a portion of the nasal defect developed by the excision of a tumor. In addition to decreasing the necessary size of the flap, this technique avoids the undesirable excision of normal tissue. Possible facial nerve damage from the dissection of the full-thickness musculocutaneous flap may also occur.
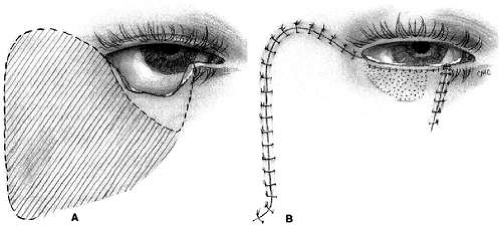
The flap (Fig. 12) is developed by outlining the area from the lateral canthus extending superiorly and temporally to or above the brow.4(p270),21 This helps to provide superior support to the lateral lid. Many illustrations of this procedure do not emphasize this point. The incision is extended laterally to just in front of the ear and then inferiorly over the jaw. The flap is extensively undermined prior to rotation. The posterior lamella of the lid is reformed by a variety of grafts, including autologous ear or nasal cartilage, tarsus, or hard palate mucosa or homologous and heterologous materials (see “Grafts” section) such as acellular dermis. The flap is rotated into position and the large redundant nasal triangle is trimmed or used for reconstruction. Trimming of the flap laterally may be necessary to avoid puckering. If the canthal tendons were removed, careful suturing of the graft and flap to remnants is necessary to provide good support to help prevent ectropion and lid displacement from the globe.
Tarsoconjunctival Flaps
Although many lid defects, even large ones, can be repaired by the relatively easy techniques of canthotomy with cantholysis or semicircular flaps, some defects may be best fixed with a sharing procedure from the opposite lid. Many have been described, including the classic Hughes5,24 and Cutler-Beard5,25 operations. Both have been modified, and we will present several examples.
Hughes Procedure and Modifications
In 1937, Hughes24 presented his first description of the now classic procedure to reconstruct the lower lid and emphasized in a later article the following concept: “When it is necessary to provide new lid structures nothing replaces lid tissue so well as lid tissue itself, both functionally and cosmetically.”26 The original technique involved splitting the upper lid into anterior (skin-muscle) and posterior (tarsoconjunctival) flaps. Because of possible instability or distortion of the lid margin or loss of lashes, this technique has been modified. The generally accepted technique places the incision in the tarsus about 4 mm above the margin, thus leaving the margin intact (Fig. 13).
After excision of the lower-lid lesion (Fig. 14A), the remaining lid segments are drawn toward each other to judge the minimal amount that must be borrowed from the opposite lid. The lid is everted on a retractor or over a plate. In the upper lid, a horizontal incision about 4 mm from the margin is made through tarsus. Vertical incisions are made to the superior tarsal border. The tarsoconjunctival flap is elevated, and the levator muscle of the upper eyelid and Müller muscle are dissected free. The conjunctiva is left attached and advanced with the tarsus to the lower lid, where the tarsus is sutured to the conjunctiva and lower-lid retractors inferiorly, and medially and laterally to the cut edges of the tarsus remaining in the defect (Fig. 13 and 14B). After thus repairing the posterior lamellae, the anterior can be reconstructed with a skin graft, a transposition flap from the upper lid (Fig. 14C), an advancement flap from the lower lid inferiorly (increased risk of producing ectropion), or a laterally based advancement flap, depending on the location of the defect and the laxity and availability of skin. Traditionally the tarsorrhaphy thus created is left in place for 4 to 8 weeks (Hughes suggested 3 months). However, several recent reports indicate that the pedicle can be safely divided sooner. McNabb et al.27 performed a prospective study opening the pedicle at 2 or 4 weeks and found no significant differences in lid position or complication rates. In 2002 Bartley and Messenger28 reported eight cases in which the pedicle was dehisced by trauma between 1 and 11 days after surgery. Though one repair was attempted, most were treated with antibiotic ointment only. All cases had a satisfactory result without loss of the grafts, though one required secondary surgery. Additionally, Leibovitch and Selva29 reported 29 cases in which the pedicle was divided at 1 week with no cases of flap or graft ischemia or necrosis. It would appear that in many cases, safe division of the pedicle can be carried out safely much sooner than previously thought.
After opening the lid, margins and donor site may require some trimming but will re-epithelialize rapidly. Some redness is expected and will fade in 6 months to a year. Care must be taken not to advance the levator tendon, or else lid retraction will result. This modification has an advantage over the original technique in that it does not violate the upper-lid margin or disturb the lashes. Hughes describes grafting lashes from the brow to the lower lid midway through healing. In many cases, a lower lid without lashes gives an acceptable appearance and avoids the possibility of misdirection with trichiasis, but grafting can be considered if cosmesis requires (see the discussion lash grafting below).
Although this basic technique was described and is best used for lower-lid reconstruction, a “reverse” Hughes procedure has been described for upper-lid reconstruction. Not surprisingly, Hughes reported this himself in his 1945 article26 on lid reconstruction. Several authors, including Leone30 and Mauriello and Antonacci,31 have presented their experience with this modification, which technically is similar to the procedure for lower-lid repair. Leone30 advanced residual tarsus and conjunctiva (basically a partial Hughes flap) and supplemented it with a reverse Hughes flap from the lower lid, the combination filling a large upper defect. As with the standard Hughes procedure and other lid-sharing techniques, the reverse Hughes flap employs tarsorrhaphy for eye closure, which they suggested remain for up to several months (see above discussion on timing of dividing the pedicle) (Fig. 15).
Jordan et al.32 and Irvine and McNab33 also reported using features of the classic Hughes operation to rebuild the central upper lid in patients in whom complete tarsal excision was not necessary. They found that if at least 3 mm of tarsus remained superiorly, it could be advanced to reform the lid margin with appropriate closure to the remaining lid fragments and could be covered with a graft or advancement flap. These procedures have the advantage of being one stage repairs without closing the lids.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree