Chapter 83 Cranial nerve and eye muscle palsies
Congenital IIIrd nerve palsy: classification
Bilateral
A. Congenital cranial dysinnervation disorder (CCDD) (see Chapter 82). This is the commonest cause of bilateral congenital IIIrd nerve palsy. Inherited genetic mutations lead to primary maldevelopment of either the IIIrd (CFEOM1) or the IIIrd and IVth cranial nerve nuclei (CFEOM2). Clinical features include bilateral ptosis and symmetrically reduced elevation and adduction. High resolution MRI shows cranial nerve hypoplasia.1
B. Rarely, sporadic bilateral infranuclear congenital IIIrd nerve palsy has been described usually in association with extensive neurodevelopmental anomalies.
Unilateral congenital IIIrd nerve palsy
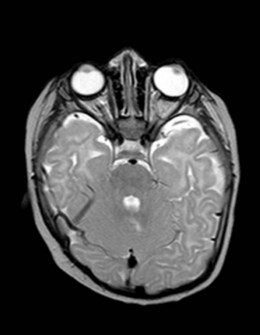
A. Clinical features suggesting pre- or perinatal peripheral IIIrd nerve damage, viz. variable IIIrd nerve innervated muscle involvement and signs of misdirection regeneration. The palsy may be isolated or associated with additional perinatal neurologic damage (Fig. 83.1).2
B. With features suggesting a primary nuclear maldevelopment, viz. bilateral partial ptosis and contralateral superior rectus palsy. A hypoplastic peripheral IIIrd nerve may be seen on MR imaging and specific genetic mutations known to be associated with CCDD identified.
C. Unilateral congenital IIIrd nerve palsy has also been reported in:
Acquired IIIrd nerve palsy
Most cases are unilateral and likely to occur in a clinical context that helps establish the etiology.2
Infection
A. Bacterial meningitis. In neonates, due to group B streptococcal infection (also Escherichia coli/listeria with brain stem encephalitis), it may be complicated by unilateral or bilateral IIIrd; recovery is likely to be poor. Cerebral visual impairment is also common (see Chapter 56). IIIrd nerve palsy can also occur in infantile or childhood meningitis.
B. TB meningitis. This can present with or be complicated by unilateral or bilateral progressive IIIrd nerve palsy.
C. Para-infectious palsy. A presumed immune-mediated pathology is responsible for cases described after, for example, influenza vaccination or MMR (measles, mumps, rubella) vaccination. The condition can be recurrent.
D. Viral meningitis. Causal viruses include herpes simplex, Epstein-Barr virus, cytomegalovirus, and herpes zoster virus.
Tumor
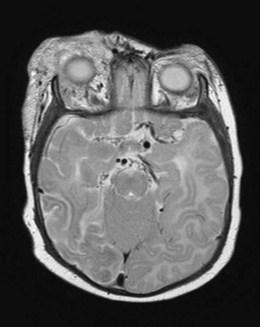
Intracranial and intraorbital tumors can present with signs including a IIIrd nerve palsy, usually progressively worsening (Fig. 83.3). External compression, direct involvement of the nerve (e.g. by schwannoma), infiltration, or malignant meningitis may be responsible. Compression can be anywhere along the course of the nerve (e.g. brainstem glioma or parasellar tumor). Raised intracranial pressure may be a contributory or primary cause.
Additional neuro-ophthalmic signs should be sought to help localize the pathology: neuro-imaging is mandatory.1
Rare causes
Vascular
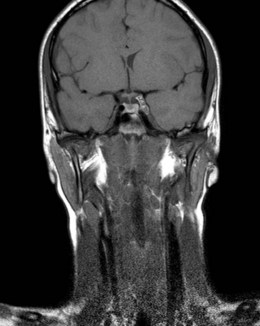
A. Aneurysmal compression. This may occur in the first or second decade due to posterior communicating artery aneurysm: also (usually with a VIth nerve palsy) due to intracavernous internal carotid artery aneurysm in, for example, Loewys-Dietz syndrome (Fig. 83.4).
B. Vasculitis. Cases have been described secondary to Kawasaki’s disease with or without aseptic meningitis and raised intracranial pressure, also polyarteritis nodosa.
C. Vascular malformation. A hemorrhage in a brain stem cavernoma or other vascular malformation can present with a partial IIIrd nerve palsy.
Ophthalmoplegic migraine
This is a diagnosis of exclusion after full investigation.3 It cannot be made on clinical grounds alone. The syndrome is not certainly due to migraine. The diagnostic criteria are:
• Childhood onset IIIrd nerve palsy associated with headache, photophobia/photopsia, and nausea.
• Pupillary involvement and usually a complete palsy.
• Neuroimaging normal except for enlargement and gadolinium enhancement of the cisternal portion of the IIIrd nerve on MRI (not invariable).4 The cerebrospinal fluid (CSF) is normal.
• Steroid responsive (but self-limiting without treatment).
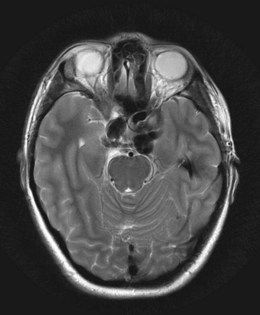
The differential diagnosis includes schwannoma, hemangioma, and lymphoma. The condition may be recurrent (Fig. 83.5).
It characteristically affects the IIIrd nerve but can affect the IVth or VIth.
Inflammatory
Fascicular IIIrd nerve palsy may occur in ADEM (acute disseminated encephalomyelitis) and in childhood onset multiple sclerosis (MS).5
Idiopathic/cryptogenic
Despite full investigation, a small proportion of childhood onset IIIrd nerve palsies remain unexplained. It is important to be prepared to reinvestigate if new signs develop; ocular myasthenia, for example, can present as a unilateral pupil sparing IIIrd nerve palsy with negative antibodies and normal electromyography.6
IVth nerve palsy
Congenital palsy
This is the commonest congenital cranial nerve palsy and the commonest cause of hypertropia in children.7 It is usually unilateral.
• An abnormal head posture (AHP) – possibly detectable from early infancy onwards. This consists of a tilt and turn of the head away from the side of the lesion (for differential diagnosis, see Box 83.1).8
• Without the AHP, a hypertropia of the affected eye which increases in adduction and reduces in abduction. This is associated with ipsilateral inferior oblique overaction/superior oblique underaction and contralateral superior rectus underaction/inferior rectus overaction.
• The Parks’ three step test is a useful way of identifying the primary underacting muscle (see Chapter 80).