CHAPTER 99 Benign and Malignant Tumors of the Nasopharynx
The nasopharynx (NP) is an embryologic confluence of the end of the nasal structures and the beginning of the pharynx. It is also bounded superiorly by the ectodermal origins of the cranial base and upper cervical spines posteriorly. For this reason, a large range of pathologies occur in this small confine (Table 99-1). Because of the NP capacity for tumor growth and expansion, the symptoms in general arise late. Thus they can reach significant sizes before presentation because of the diagnostic inaccessibility of the NP area.
Table 99-1 Benign and Malignant Tumors of the Nasopharynx
Diagnostic Approach for Nasopharyngeal Masses
Squamous Papilloma
This benign epithelial tumor is common in the anterior and posterior nasal space. The epithelial changes of such a tumor may be inverting at the basal membrane, whence they are termed “Schneiderian” or “inverting” papilloma. The presentation is unusually incidental for lesions of the nasopharynx (which is not common), and diagnosis should be done with a biopsy. The base of the lesion should be completely removed with a margin of normal tissue. The use of powered instrumentation is helpful in difficult recesses of the nasopharynx. Further detail on the management of inverting papilloma of the nose and paranasal sinuses is available in Chapters 49 and 99.
Craniopharyngioma
Craniopharyngiomas are histologically benign tumors that arise developmentally from Rathke’s pouch. They usually present with symptoms similar to pituitary tumors (endocrine and visual disturbances), but occasionally they may present with nasal symptoms such as nasal obstruction due to extension into the nasopharynx. In children, these lesions have been known to mimic presentation similar to adenoidal hypertrophy.14 Treatment is surgical excision with or without radiation therapy. The gamma knife has been used as the primary treatment.
Angiofibroma
Growth Patterns
The tumor mass is locally infiltrative and usually has a wide-based attachment to the NP and to its surrounding related anatomy. JNA is a slow-growing vascular tumor arising in the area of the sphenopalatine foramen at the root of the pterygoid process on the lateral nasal wall. The tumor expands laterally via the pterygopalatine fossa to the infratemporal fossa but has no resistance to growth into the NP and choanal space and thereby may expand into the anterior nasal cavity and all the related sinuses. It can have intracranial extensions into the middle and anterior cranial fossae, although this is uncommon. It can also extend bilaterally to the maxillary sinuses and superiorly to the cranial skull base. Because JNA commonly occurs in young males, this has prompted studies related to the androgen receptor (AR) and estrogen receptor (ER) in the tumor tissue. A recent study suggests a stronger relationship to ER positivity, which may provide a platform for ER modulators in the management of JNA.1
Pathologic Features
The gross pathology usually shows a sessile, lobulated, rubbery dark red to tan gray mass that can be large in size. Mucosal ulceration is uncommonly seen and the tumor is unencapsulated and composed of an admixture of vascular tissue and fibrous stroma. The vessel walls lack elastic fibers and have incomplete or absent smooth muscle that will account for their tendency to bleed.2
Clinical Features
Although JNA is typically diagnosed between the ages of 10 and 25 in males, many case reports exist for female patients and also in patients who are in the later decades of life. JNA patients present with nasal obstruction (usually unilateral), epistaxis, blood-stained sputum, and serous otitis media. Less common symptoms include nasal discharge, facial swelling, proptosis, sinusitis, and anosmia. The duration of symptoms is usually long and often mild and innocuous. JNA cases occurring in sites other than the NP have been reported. The next commonest site, the maxillary sinuses, is associated with a greater proportion of females.3
Diagnosis
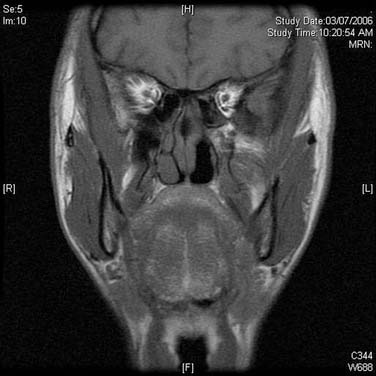
On endoscopic examination, JNA presents as a rubbery vascular mass protruding into the anterior nasal space and may have excessive bleeding on contact. A CT scan with contrast will show an enhancing soft tissue mass arising from the NP or lateral wall of the nose. Although the pterygopalatine fossa may be widened by the tumor (Fig. 99-1), bone erosion is not present in general. MRI will show a vascular tumor with flow voids within the mass and enhances on gadolinium. MR angiography will be the least invasive form of vascular imaging that will show the feeding vessels arising from the branches of the external carotid system. The authors have found the MRI with contrast to be more useful for follow-up evaluation (Fig. 99-2). The use of 99mTc-RBC single photon emission computed tomography has been suggested to be accurate in the diagnosis of JNA.4 However, final proof of diagnosis is histologic.
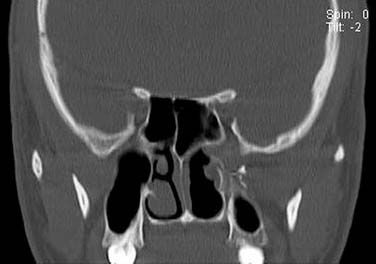
Figure 99-1. Computed tomography showing the widening of the left sphenopalatine foramen from a juvenile angiofibroma.
Staging
In 1984 Chandler and colleagues5 proposed a staging system (Table 99-2) on the basis of clinical and CT assessment. This staging system is logical and easy to understand and it is useful for reporting. Due to the large anatomic region of stage 3, Sessions and Radkowshi have suggested refining stage 3. However, none of the systems has been used extensively for comparing outcomes because published case series have usually been of small numbers.
Table 99-2 The 2002 UICC TNM Staging of Nasopharyngeal Carcinoma
| T Classification | |
| Tx | Primary tumor unable to be assessed |
| T0 | No evidence of tumor |
| T1 | Confined to nasopharynx |
| T2a | Extends to nasal cavity, oropharynx |
| T2b | Tumor extends to parapharyngeal space |
| T3 | Tumor involves sinuses, orbit, skull base, hypopharynx |
| T4 | Intracranial or infratemporal involvement |
| N Classification | |
| N0 | No nodal involvement |
| N1 | Ipsilateral lymph nodes < 6 cm |
| N2 | Bilateral lymph nodes < 6 cm |
| N3 | Lymph node > 6 cm; supraclavicular node |
| M Classification | |
| M0 | No distant metastasis |
| M1 | Distant metastasis (includes mediastinal nodes) |
| Stage Classification | |
| Stage I | T1N0M0 |
| Stage II | T1N1M0, T2N0M0, T2N1M0 |
| Stage III | T3N0-2M0, T1-2N2M0 |
| Stage IVa | T4, any NM0 |
| Stage IVb | any TN3M0 |
| Stage IVc | any T, any N, M1 |
TNM, tumor node metastasis; UICC, Union Internationale Contre Cancre.
Management
For extension outside the NP into the paranasal sinuses, a Le Fort type 1 osteotomy will allow an inferior approach to the maxillary and ethmoid sinuses as well as the pterygopalatine canal. For lesions involving the infratemporal fossa or large lesions involving the majority of the sinuses, a facial translocation approach affords a large window of access. The facial translocation involves the rotation of the facial cheek flap as a single osteoplastic unit with the underlying maxilla rotated laterally after osteotomies to the maxillary nasal, orbital maxillary, and zygomatic arches. The senior author has also incorporated the entire nose and cheek as a single rotation based laterally. This allows for excellent access to the infratemporal fossa and hemostatic options in the event of bleeding. A lateral infratemporal fossa approach has been recently used as reported by Tyagi and colleagues.6
Endoscopic sinus surgery techniques have advanced significantly over the past 2 decades and have allowed the intranasal access and nasal anatomy to be approached in an extremely competent fashion. Several authors have published their experience of successful endoscopic resection of such tumors. Several reports of endoscopic resection have reasonable follow-up durations (13 patients in 23 months) and low recurrence rates (8%).7 Combination approaches of type 3 JNA with open and endoscopic approaches have also reported good success but of shorter-term results.8 For larger lesions such as stage 3A disease, Hofmann and colleagues have reported successful endoscopic resection with long-term results (52 months) in a series of 21 patients and have reported that extension to the medial aspect of infratemporal fossa and retromaxillary space was not a contraindication to an endonasal endoscopic approach.
Preoperative embolization of the tumor mass is used by some to reduce intraoperative bleeding. However, the risk of recurrence has been highlighted with the use of preoperative embolization.9 In extensive tumors where the feeding vessels come from the internal carotid system, a laser-assisted extracranial-intracranial bypass has been used before the definite surgery in order to prevent neurologic deficits.10
Recurrence rates have been reported to be as high as 35% depending on the length of follow-up. For patients with recurrent disease, the options remain for observation alone, revision surgery, or radiation. Radiation has been used for treatment of JNA, especially those that recur after surgery and those with intracranial extension where clearance of margins may be difficult. Cummings and colleagues11 reported a series of 56 patients treated with 3000 cGY. However, issues of impact on growth centers, cataract formation, and osteoradionecrosis have been reported, as have cases of malignant transformation.12 For these various reasons, observation, sometimes followed by involution with aging or repeat surgery, is an option in the presence of recurrence. In patients who cannot undergo surgery, recalcitrant cases of tumor recurrence despite several repeat resections and inaccessible recurrences may be considered for radiation therapy with full disclosure of possible long-term, late effects (e.g., radiation-induced malignancy, carotid artery damage). Park13 recently reported using the gamma knife with good success for a case of recurrent intraorbital JNA.
Adenoid Cystic Carcinoma of the Nasopharynx
Adenocystic carcinoma of the sinonasal tract constitutes 20% of all adenoid cystic carcinomas of the head and neck. They, along with other tumors of salivary gland origin, arise from the minor salivary glands in this region. Those of the NP are not common but can be insidious and slow growing.14 The lesion can extend from the nasopharynx into the anterior skull base and can present as bilateral nasal lesions. In the latter, there is a need to differentiate this from simple bilateral nasal polyps. Patients with either condition may present with simple nasal obstruction with hyposmia. Other accompanying symptoms do not usually occur, unless palpable neck metastasis is detectable at presentation. Otitis media with effusion may exist if the eustachian tube is involved. These tumors have the propensity for perineural spread and thus MR imaging is important in the pretreatment evaluation. The primary treatment of such lesions is surgical resection. However, proximity of the nasopharynx to the sphenoid, and, hence, the internal carotid arteries and intracranial structures, plus their propensity for centrifugal spread along nerves, may preclude complete removal. Postoperative radiotherapy is important in local control of such lesions.
Nasopharyngeal Carcinoma
Nasopharyngeal carcinoma (NPC) is unique in its epidemiologic pattern. It is common in certain ethnic groups, with the highest incidence in southern China, Hong Kong, and southeast Asia. The majority of patients with NPC are diagnosed with advanced disease. However, over the past 20 years, the survivals of these patients have improved.15 This has been attributed to the combined use of chemotherapy and radiation to treat the patients with advanced disease.16 Furthermore, with the advent of improved techniques in radiation, the side effects, which plagued long-term survivors in the past, may be reduced.17,18 The strategy in the management of NPC is to find novel methods of early detection and develop improved techniques of effective primary treatment with the focus on reducing morbidity from the treatment. In this chapter we describe the epidemiology, etiology, pathology, clinical features, staging, treatment, and prognosis of NPC.
Epidemiology
The highest incidence of NPC is recorded in Guangzhou, China, where the age-adjusted incidence rate is reported to be more than 30 per 100,000.19 Hong Kong has a rate of 20.2 per 100,000 in males and 7.8 per 100,000 in females.15 Patients who are affected by NPC are ethnic Chinese with an ancestry from the southern part of China. In southern China the two main ethnic subgroups are the Cantonese and the Fujians. In Hong Kong the vast majority of the population is Cantonese. In Singapore the overall incidence in males from 1998 to 2002 was 10.8 per 100,000.20 This lower rate may be in part accounted for by the demographics of Singapore, which unlike China, Hong Kong, and Taiwan, has a more heterogeneous population. The population in Singapore is approximately 70% Chinese, with the remaining major ethnic groups being Malays and Indians. The majority of the NPC patients in Singapore are Chinese (Fujians and Cantonese).21 The incidence of NPC in Singaporean male Chinese is 12.5 per 100,000. These incidence rates in southern China, Hong Kong, and southeast Asia are among the highest in the world and have remained stable for many years. However, in the most recent review of the latest trend in the incidence of NPC, both Singapore and Hong Kong have reported a significant decrease for the first time after many years of stable rates.15 Why there was a fall in incidence is unclear, but one theory advanced to account for this is the change in dietary habits.22,23 Other ethnic groups, with rates that are reported to be intermediate to high, include the Eskimos,24,25 Polynesians, and indigenous Mediterranean population.26 NPC is not common in whites. In North America the highest incidences are seen in the ethnic Chinese who are first-generation immigrants.23 Subsequent-generation immigrants have a lower incidence, although it is still higher than the other ethnic groups. Overall, these incidence rates are lower than those in southern China and southeast Asia. This pattern of decreasing incidence rates seen in emigrant Chinese is a well-known phenomenon. It is likely that with migration, there is over time a greater variation in the gene pool arising from factors such as intermarriage, although the adoption of different dietary habits cannot be discounted. The epidemiologic pattern indicates that NPC occurs commonly in Chinese. This will suggest the possibility of a genetic link or a shared habit such as dietary intake.