Chapter 66 Accidental trauma in children
Epidemiology
The number of serious eye injuries in children has been estimated at 11.8 per 100 000 per year.1 At least 35% of serious eye injuries occur in children; the majority occur in children under the age of 12.2 Eye injuries account for 8–14% of total injuries in children3 and are the most common cause of unilateral blindness in children. Aside from vision loss, significant disfigurement may accompany a serious eye injury. Several factors place a child at risk for serious accidental eye injury:4 age between 0 and 5 years, male gender, and a lack of parental supervision. Non-compliance with optical correction and patching is an important factor after childhood perforating anterior eye injury.5 Amblyopia may limit recovery of vision in children under 7 years of age, even in eye injuries that would carry a good prognosis in older individuals.
Ophthalmic trauma caused by amniocentesis and birth injury
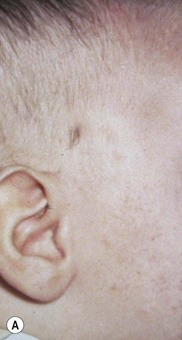
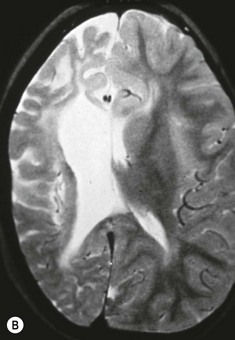
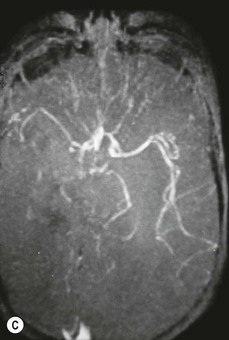
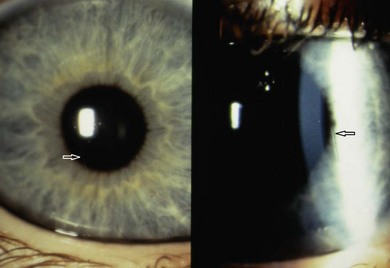
Eye injuries occur in association with amniocentesis (Fig. 66.1). Of five cases of presumed ophthalmic amniocentesis injury,6 one had a hemianopia and gaze palsy, two had presumed needle perforation of the eye resulting in a peaked pupil in one case and chorioretinal scar in the other. In the remaining two one showed a small leukoma, and one a limbal scar. After amniocentesis, non-pigmented anterior iris cysts adherent to the posterior cornea and with peripheral anterior synechiae are possibly a result of injury with the amniocentesis needle. Congenital aphakia with retinal scar has also been described following in utero perforation of the globe.
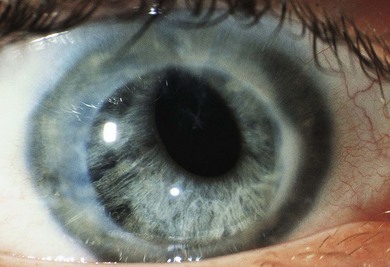
Ocular adnexal injuries occur, albeit rarely, after episiotomy. The possibility of ruptured globe caused by childbirth is discussed below. Forceps should be suspected as the cause of a congenital corneal abnormality in which vertical ruptures in Descemet’s membrane (Fig. 66.2) occur with a contralesional occipital depression caused by the other arm of the forceps (Chapter 33).
Eyelid and lacrimal system trauma
In eyelid margin laceration, careful reapproximation of the margins of the eyelid is essential. The etiology is sharp or blunt trauma to the lid margin. Injuries to the canalicular system will occur if the medial eyelid margin is injured, either of the upper or lower lid commonly caused in children by dog bites.7 They require intubation with silastic tubing passed through both ends of the canaliculus and into the nose or the use of a monocanalicular stent. With deeper injuries, we close deep edges of the wound with fine grade absorbable suture and close the more superficial edges of the wound with fine suture. With dog bite injuries additional problems may be an inferior oblique palsy or restrictive type of ocular motor problem. We close the laceration, as described above, followed later by strabismus management as required.
Anterior segment trauma
Subconjunctival hemorrhage (see Chapter 31)
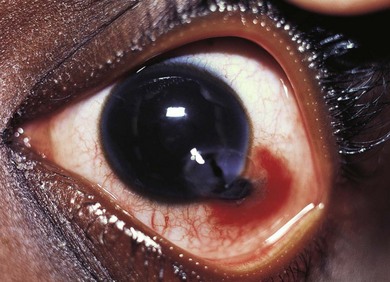
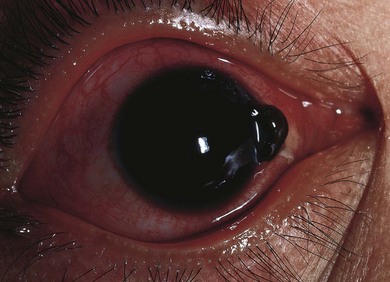
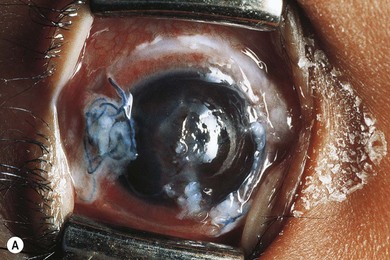
Subconjunctival hemorrhages associated with trauma indicate the need for a thorough search for a more serious eye injury (Fig. 66.3). The hemorrhage may mask a penetrating injury; look carefully for other signs of penetrating injury (e.g. uvea in a laceration, distorted pupil, lower intraocular pressure).
Corneal abrasion
The differential diagnosis for corneal abrasion includes viral (e.g. herpes simplex, adenovirus) keratitis and corneal basement membrane disease and dystrophies. Herpes infection is usually suggested by a dendritic appearance, while basement membrane disease occurs in older children and adults and is recurrent, with no history of trauma (see Chapter 15).
Eye wall injuries
Etiology
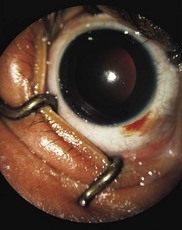
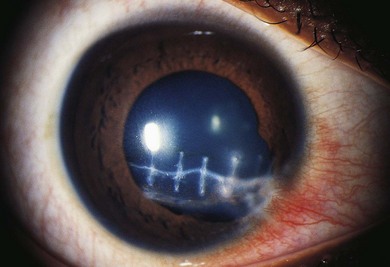
In simple lacerations, the eye is cut with a sharp object (Figs 66.4–66.7). Very young children usually suffer injury when they fall on a sharp object. Older children may suffer eye wall lacerations from glass (particularly when they wear spectacles), and projectiles.
Predisposition (“brittle corneas”)
Certain eyes may be more likely to rupture with relatively minor trauma. In Ehlers-Danlos syndrome, defective collagen cross-linkage leads to scleral and corneal weakness (Fig. 66.8); in Ehlers-Danlos with blue sclera (due to scleral thinning), hyperextensible skin, and hypermobile joints, spontaneous corneal rupture can occur, and in the brittle cornea, blue sclera and joint hyperextensibility syndrome, spontaneous rupture of the globe may occur. Such patients may have red hair and develop keratoglobus, and, unlike Ehlers-Danlos syndrome, they have normal levels of lysyl hydroxylase. Osteogenesis imperfecta consists of blue sclera, deafness, and bone fractures. Children with this syndrome may also be more prone to corneal rupture from minor trauma.
Globe rupture
When a globe is ruptured, it is pushed or squeezed so hard that the eye wall breaks under pressure. The results usually are devastating, with partial or complete expulsion of intraocular contents. Expulsion is facilitated due to the increase in intraocular pressure followed by sudden decompression through a hole in the wall of the eye. Events that can cause ruptured globes usually involve encounters with large, blunt objects. In many countries, sporting impacts and automobile crashes (airbag injuries) are major causes of globe rupture in older children.8 Globe rupture is more common in boys than girls, reflecting the nature of the cause. Eyes are more likely to be ruptured or lacerated in areas where the sclera or cornea are thinnest: under the rectus and superior oblique muscle insertions and the corneoscleral limbus are thin.
Anterior versus posterior laceration
Anterior locations of injuries carry a better prognosis, so long as the injury does not also cut the retina. Injuries anterior to the pars plana (5 mm posterior to the limbus) will not cut the retina, and therefore carry a better prognosis. If a cataract occurs with an anterior laceration, the prognosis for recovery of vision is not as good.9 Posterior injuries cut the retina and often result in a complicated retinal detachment, with a far worse prognosis.
Management
Prevention
The use of safety glasses in monocular children is valuable, especially at times of particular risk.
Imaging
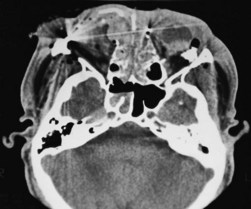
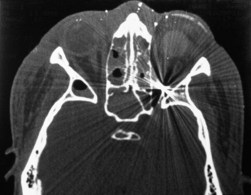
In many cases, a CT scan of the orbits (Figs 66.9 and 66.10) will help to identify the location of expected or unexpected intraocular foreign bodies, and ultrasound biomicroscopic evaluation also can be helpful to detect zonular deficiency, angle recession, iridodialysis, lens dislocation, and iridocorneal adhesions.10