Chapter 123 What is a sensible screening program in paediatric ophthalmology?
Why screening is important in pediatric ophthalmology
Young children do not report reliably changes in vision to one or both of their eyes. There are a limited range of professionals who are able to perform an eye examination on children, and this number is possibly reducing. For these reasons many pediatric eye disorders present late. A need for screening is recognized and has led to the detection by screening of over 50% of pediatric eye conditions affecting the child’s sight, usually by pediatricians or family doctors.1
What is screening?
“Screening is the systematic application of a test or inquiry to identify individuals at sufficient risk of a specific disorder to benefit from further investigation or direct preventive action, among persons who have not sought medical attention on account of symptoms of that disorder”.2 Screening detects individuals within a population who have a disease before they develop signs or symptoms. Alternatively, screening can be used to detect a risk factor for future or asymptomatic disease.
When is screening appropriate?
Criteria for the value and feasibility of screening programs were created by the World Health Organization (Box 123.1)3,5. These fall into groups:
Box 123.1 World Health Organization criteria for screening
1. The condition should be an important health problem.
2. There should be a treatment for the condition.
3. Facilities for diagnosis and treatment should be available.
4. There should be a latent stage of the disease.
5. There should be a test or examination for the condition.
6. The test should be acceptable to the population.
7. The natural history of the disease should be adequately understood.
8. There should be an agreed policy on whom to treat.
9. The total cost of finding a case should be economically balanced in relation to medical expenditure as a whole.
10. Case-finding should be a continuous process, not just a “once and for all” project.
Types of screening
Targeted screening
A test or examination is offered to a population at increased risk of a disease or complication.
Screening vs. active surveillance
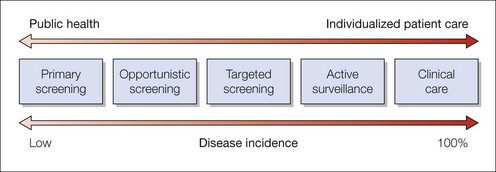
The prevalence of underlying disease in primary screening is low; for example, hundreds of neonatal red reflex examinations will be needed to detect an abnormality and WHO guidelines need to justify screening. When the chance of positive findings within a targeted population is high, then active surveillance is used instead of screening (Fig. 123.1).
Genetic screening
The special and changing nature of genetics screening is recognized in program assessment criteria.4 As costs reduce there is increasing pressure from individuals, families, patient support groups and commercial interests for testing in specific gene disorders or for gene markers of complex traits.5
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree