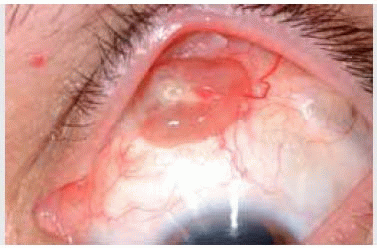
 Vascular Tumors and Related Lesions of the Conjunctiva
Vascular Tumors and Related Lesions of the ConjunctivaConjunctival Pyogenic Granuloma
General Considerations
There are a few important vascular tumor and related lesions that can occur in the conjunctiva, including pyogenic granuloma, lymphangioma, varix, capillary hemangioma, cavernous hemangioma, and Kaposi sarcoma (KS). In the authors’ clinical series of 1,643 conjunctival tumors, there were 63 vascular lesions, accounting for 4% of the 1,643 lesions (4).
Pyogenic granuloma is a common and well-known condition (1,2,3,4,5,6,7,8,9,10,11,12,13,14,15,16,17,18,19). In the authors’ series of 1,643 conjunctival tumors, the 11 pyogenic granulomas accounted for 18% of 63 conjunctival vascular lesions and for less than 1% of the 1,643 lesions (5).
The classification and terminology of pyogenic granuloma has been the source of considerable confusion. Some pathologists prefer to classify it as exuberant granulation tissue of “pyogenic granuloma type,” which is the term employed by our pathologists (Ralph C. Eagle, Jr, MD, personal communication, November 23, 2005). Others prefer the term “acquired capillary hemangioma, pyogenic granuloma type.” Some dermatologists have called a similar lesion an “acquired lobular capillary hemangioma” (16,17), which does not easily apply to the lesions seen in the conjunctiva. Until a more accurate name is agreed upon, we have chosen to continue to use the conventional term “pyogenic granuloma,” even though it is a misnomer. In actuality, it is a proliferative fibrovascular response (granulation tissue) to prior tissue insult by inflammation, surgery, or nonsurgical trauma (1,2,3,4,5,6,7,8,9,10,11,12,13,14,15,16,17). It is most commonly seen at a traumatic wound site or near a suture line after surgery for chalazion, pterygium, strabismus, or enucleation (7). It has been recognized at the site of a dermis fat graft used after enucleation (9). It can also occur as a primary response to a chalazion, even if there is no history of prior surgery. It has been recognized in patients who wear contact lenses, presumably from chronic inflammation or from retention of a “lost” lens (8). Rarely, it appears to be entirely primary, without any underlying cause or event.
Pyogenic granuloma is usually confined to the conjunctiva, but it has also occurred on the cornea (10,11). A report of 14 corneal pyogenic granulomas showed that there was usually an underlying cause and a precipitating event. Predisposing conditions included indolent corneal ulceration, dry eye syndrome, trachoma, trichiasis, alkali burn, multiple topical drug use, previous orbital irradiation, and ocular cicatricial pemphigoid. The precipitating event was usually a persistent epithelial defect secondary to those predisposing conditions (10). It has also occurred at the surgical site after corneal transplantation (11).
Clinical Features
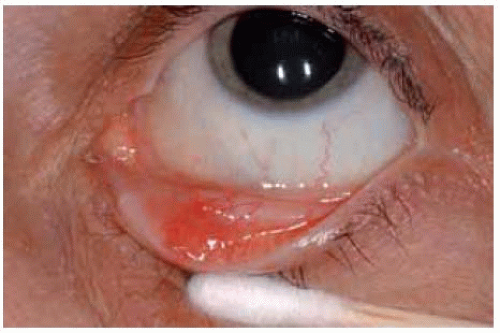
Clinically, pyogenic granuloma generally has a rapid onset and progression usually follows an apparent insult. It can assume any of several clinical variations. It is usually an elevated fleshy red-pink mass that often has a florid blood supply from the adjacent conjunctiva. The shape of the lesion can vary considerably from case to case, ranging from round to ovoid, broad based, and even mushroom shaped. Elevation of the margin of a pyogenic granuloma with a cotton-tipped applicator often reveals that the lesion is pedunculated, with an underlying stalk of blood vessels and connective tissue.
Pathology
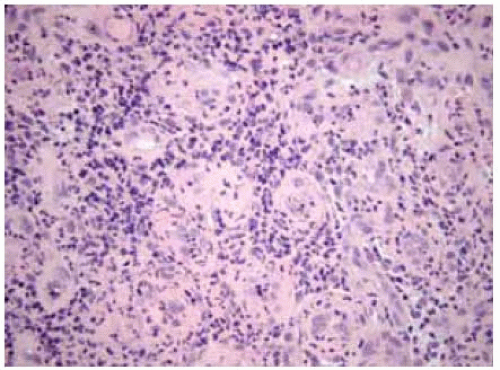
Microscopically, pyogenic granuloma is composed of granulation tissue with lymphocytes, plasma cells, scattered neutrophils, and numerous small-caliber blood vessels. As mentioned, it is often pointed out that the term “pyogenic granuloma” is a misnomer; the lesion is neither pyogenic nor granulomatous.
Management
Pyogenic granuloma sometimes responds to topical cortico-steroids, but many cases ultimately require surgical excision. We have found that shaving excision at the small base, followed by cautery and cryotherapy, is usually effective, but recurrence is not uncommon. In the rare case of recurrence and continued growth, low-dose brachytherapy with a radioactive plaque has been effective (12).
Selected References
1. Spencer WH. Conjunctiva. In: Spencer WH, ed. Ophthalmic Pathology. An Atlas and Textbook. 4th ed. Philadelphia: WB Saunders; 1996:83-84.
2. Shields CL, Shields JA. Overview of tumors of the conjunctiva and cornea. In: Foster CS, Azar DT, Dohlman CL, eds. Smolin and Thoft’s The Cornea. 4th ed. Philadelphia: Lippincott, Williams & Wilkins; 2005:735-755.
3. Shields JA, Shields CL. Tumors of the conjunctiva. In: Stephenson CM, ed. Ophthalmic Plastic, Reconstructive and Orbital Surgery. Stoneham, MA: Butterworth-Heinemann; 1997:253-271.
4. Shields CL, Shields JA. Tumors of the conjunctiva and cornea. Surv Ophthalmol 2004;49:3-24.
5. Shields CL, Demirci H, Karatza E, et al. Clinical survey of 1643 melanocytic and nonmelanocytic tumors of the conjunctiva. Ophthalmology 2004;111:1747-1754.
6. Ferry AP. Pyogenic granulomas of the eye and ocular adnexa: a study of 100 cases. Trans Am Ophthalmol Soc 1989; 87:327-347.
7. Fryer RH, Reinke KR. Pyogenic granuloma: a complication of transconjunctival incisions. Plast Reconstr Surg 2000;105:1565-1566.
8. Horton JC, Mathers WD, Zimmerman LE. Pyogenic granuloma of the palpebral conjunctiva associated with contact lens wear. Cornea 1990;9:359-361.
9. Liszauer AD, Brownstein S, Codere F. Pyogenic granuloma on a dermis fat graft in acquired anophthalmic orbits. Am J Ophthalmol 1987;15;104:641-644.
10. Cameron JA, Mahmood MA. Pyogenic granulomas of the cornea. Ophthalmology 1995;102:1681-1687.
11. DePotter P, Tardio DJ, Shields CL, et al. Pyogenic granuloma of the cornea after penetrating keratoplasty. Cornea 1992;11:589-591.
12. Gunduz K, Shields CL, Shields JA, et al. Plaque radiotherapy for recurrent conjunctival pyogenic granuloma. Arch Ophthalmol 1998;116:538-539.
13. Soll SM, Lisman RD, Charles NC, et al. Pyogenic granuloma after transconjunctival blepharoplasty: a case report. Ophthal Plast Reconstr Surg 1993;9:298-301.
14. Espinoza GM, Lueder GT. Conjunctival pyogenic granuloma after strabismus surgery. Ophthalmology 2005;112;1283-1286.
15. Akova YA, Demirhan B, Cakmakci S, et al. Pyogenic granuloma: a rare complication of silicone punctal plugs. Ophthalmic Surg Lasers 1999;30:584-585.
16. Mills SE, Cooper PH, Fechner RE. Lobular capillary hemangioma, the underlying lesion of pyogenic granuloma: a study of 73 cases from the oral and nasal mucous membranes. Am J Surg Pathol 1980;4:471-479.
17. Patrice SJ, Wiss K, Mulliken JB. Pyogenic granuloma (lobular capillary hemangioma): a clinicopathologic study of 178 cases. Pediatr Dermatol 1991;8:267-276.
18. Murphy BA, Dawood GS, Margo CE. Acquired capillary hemangioma of the eyelid in an adult. Am J Ophthalmol 1997;124:403-404.
19. Shields JA, Criss J, Mashayekhi A, et al. Vascular tumors of the conjunctiva. The 2006 Victor Curtin Lecture. In press.
Conjunctival Pyogenic Granuloma: Primary (Idiopathic) Type
In some cases, pyogenic granuloma can appear in the conjunctiva as a spontaneous lesion, without an evident cause. Some may be related to ruptured chalazion of which the patient was unaware; others may develop secondary to subclinical trauma or other insults.
Ferry AP. Pyogenic granulomas of the eye and ocular adnexa: a study of 100 cases. Trans Am Ophthalmol Soc 1989;87:327-347.
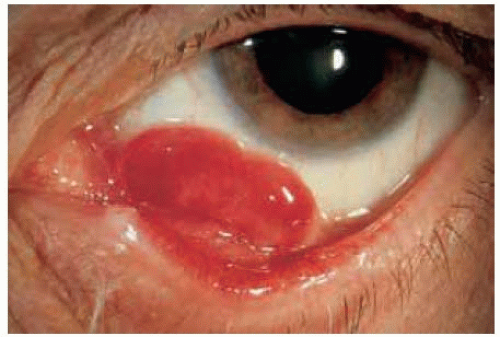 Figure 20.2. Spontaneous pyogenic granuloma arising from conjunctiva inferiorly in a 66-year-old woman. The lesion was very pedunculated and was connected by a stalk to the underlying conjunctiva. |
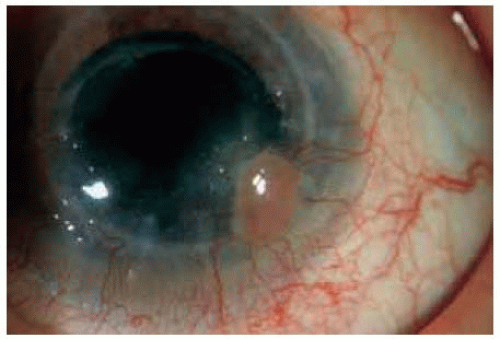
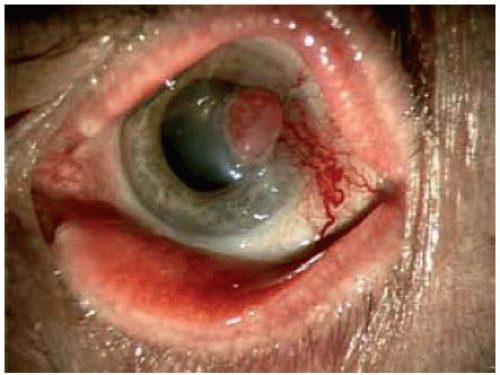 Figure 20.3. Pyogenic granulom a of the cornea. The etiology was uncertain. Note the dilated feeder vessels. |
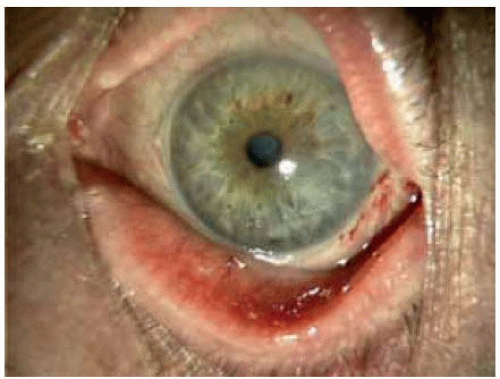 Figure 20.4. Appearance of eye shown in Figure 20.3, one year after superficial surgery to remove the lesion. The cornea is clear and the feeder vessels have mostly resolved. |
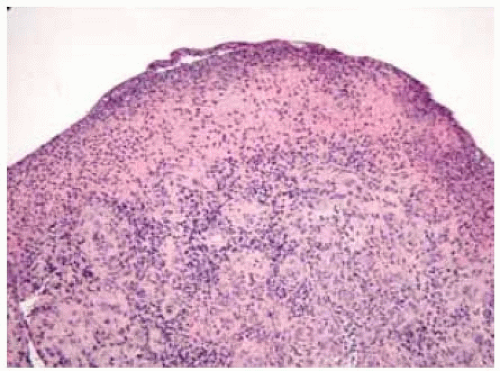 Figure 20.5. Pathology of pyogenic granulom a show ing compact inflammatory cells and granulation. (Hematoxylin-eosin 20.) |
Secondary Conjunctival Pyogenic Granuloma: Treatment With Plaque Radiotherapy
In many instances, pyogenic granuloma is due to an apparent underlying cause, such as prior ocular surgery, trauma, or ruptured chalazion. Surgical procedures that can be associated with the development of pyogenic granuloma include procedures for strabismus, pterygium, retinal detachment, and procedures like corneal transplant, and enucleation. In some instances, pyogenic granuloma can involve the cornea.
DePotter P, Tardio DJ, Shields CL, et al. Pyogenic granuloma of the cornea after penetrating keratoplasty. Cornea 1992;11:589-591.
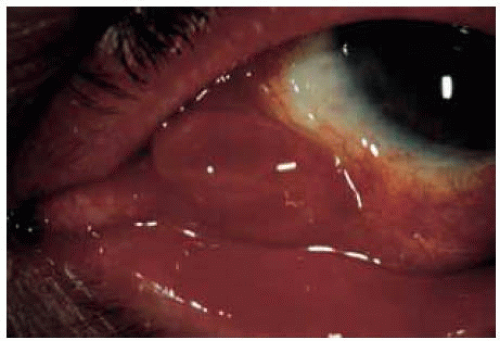
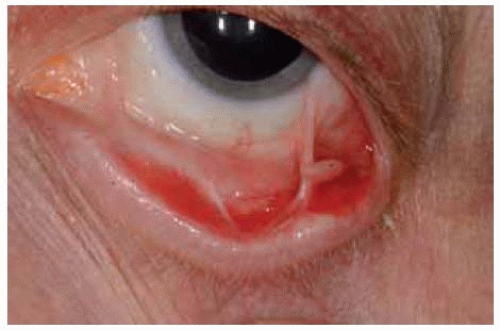 Figure 20.7. Pedunculated pyogenic granuloma that developed after uncomplicated surgical removal and cryotherapy of primary acquired melanosis of the inferior fornix. |
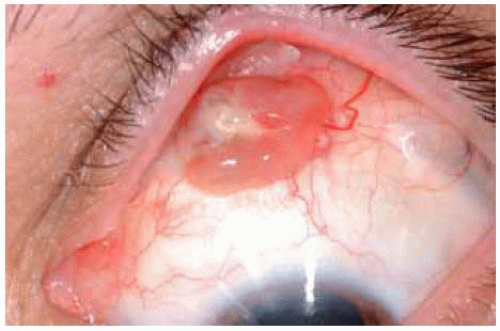 Figure 20.8. Pyogenic granuloma that developed as a reaction to scleral buckling procedure for rhegmatogenous retinal detachment. Note the exposed silicone band just posterior to the lesion. |
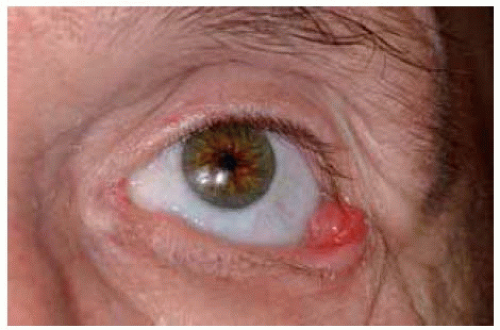 Figure 20.9. Pyogenic granuloma in lateral canthal region, that possibly developed from irritation by a slightly poor-fitting prosthesis after enucleation for uveal melanoma. |
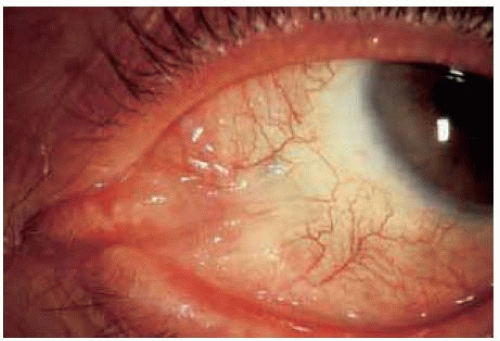 Figure 20.12. Appearance of same eye shown in Figure 20.11, one year after plaque radiotherapy. There has been no further recurrence after plaque brachytherapy. |
Conjunctival Lymphangiectasia and Lymphangioma
General Considerations
In some instances, the lymphatic channels in the conjunctiva are dilated and prominent, a condition called “lymphangiectasia.” When the vascular lesion forms a distinct mass, it is called a “lymphangioma” (1,2,3,4,5,6,7,8,9,10,11,12,13). Although it is usually a unilateral, sporadic occurrence, it has been recognized as part of Turner’s syndrome and Nonne-Milroy-Miege disease (1). In the authors’ clinical series of 1,643 conjunctival tumors, there were 15 lymphangiomas, accounting for 24% of conjunctival vascular lesions and for less than 1% of the 1,643 lesions (6).
Clinical Features
When there is bleeding into the lymph channels, it is called “hemorrhagic lymphangiectasia” (2). When lymphangiectasia assumes tumorous proportions, it is called “lymphangioma.” Conjunctival lymphangioma can occur as either a solitary conjunctival lesion or as multifocal conjunctival lesions. In most instances, the conjunctival lymphangioma represents a superficial component of a deeper diffuse orbital lymphangioma (8). The lymph channels in a lymphangioma may contain clear fluid (lymph), in which case it appears as a multiloculated, cystlike lesion. In such instances, a large cystic compound nevus of the conjunctiva may be clinically similar to lymphangioma (11). Usually, when it becomes clinically apparent in the first decade of life it has undergone bleeding into the cystoid spaces and appears as a multiloculated blue-red mass containing variable-sized, clear, dilated vascular channels (3,4,5,6). When this blood is present in many of the cystic spaces, the lesion has been called a “chocolate cyst” (3). At that stage, the lesion may resemble a cavernous hemangioma.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree