Acyclovir (9-[2-hydroxyethoxymethyl] guanine) has proved to be an extremely safe and effective agent and is a drug of choice for most forms of HSV and VZV infections. Its availability in topical, oral, and IV preparations allows its use in a wide range of clinical situations. However, its poor oral absorption has spurred the development of valacyclovir and famciclovir.
Mechanism of Action, Pharmacology, and Toxicity
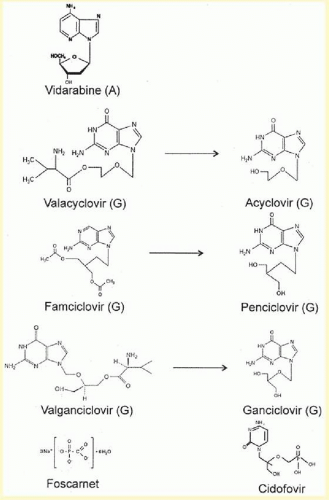
An acyclic analog of guanosine (see
Fig. 37.2), acyclovir is the prototype of a generation of specific antiviral drugs that are activated by a viral thymidine kinase to become potent inhibitors of viral DNA polymerase.
91 The drug inhibits in vitro, in order of decreasing effect, HSV-1 and HSV-2, VZV, Epstein-Barr virus (EBV), human herpesvirus 6 (HHV-6), and CMV.
92 (In vivo it does have some activity against CMV.
93) Its in vitro activity is 160 times greater than that of vidarabine.
94 However, acyclovir’s antiviral spectrum is limited to the herpesvirus group. It has no significant activity against vaccinia.
61 Acyclovir must be phosphorylated to the nucleotide form, acyclovir triphosphate to exert its antiviral activity. It is first selectively phosphorylated to acyclovir monophosphate by viral thymidine kinase produced only in infected cells. Cellular kinases then convert acyclovir monophosphate to the triphosphate form.
95 Acyclovir triphosphate is found in HSV-infected cells at concentrations 40 to 100 times greater than in uninfected cells.
96 That the drug is functional predominantly in infected cells explains its very low toxicity. Human CMV is relatively insensitive to acyclovir because it does not encode for viral thymidine kinase and is, therefore, inhibited only with a median inhibitory dose (ID
50) similar to that of the host’s cells.
92 Acyclovir triphosphate is both an irreversible inhibitor of, and a substrate for, viral DNA polymerase
97 and has a greater affinity for viral DNA polymerase than for cellular DNA polymerase. In addition, the incorporation of acyclovir triphosphate into a growing DNA chain results in chain termination because it lacks a 3′ hydroxyl group and, therefore, no attachment point for the next link. Because EBV, which does not produce herpes-directed thymidine kinase, is sensitive in vitro to acyclovir, additional mechanisms of action may exist.
98,
99Acyclovir can be administered topically (although not formulated for ophthalmic use in the United States), intravenously, and orally. The dosage is timed to achieve drug levels in the extracellular fluid that are greater than the ID
50 for HSV types 1 and 2 (mean, 0.1 to 1.6 µM) and VZV (mean, 3 to 4 µM).
91,
92,
100 However, antiviral activity is actually due to intracellular levels of acyclovir triphosphate. With IV dosing, the serum half-life is about 3 hours in adults with normal renal function. At a dosage of 5 mg per kg three times a day, serum concentrations are well above the ID
50 for HSV-1 and HSV-2, but trough levels fall below the ID
50 of many VZV isolates.
101 However, a dosage of 10 mg per kg three times a day provides trough levels sufficient for most VZV infections.
100,
101 Acyclovir is 15% protein bound, and the volume of distribution is 70%, corresponding to total body water.
102 The cerebrospinal fluid level is 50% that of plasma.
103 Seventy percent of acyclovir is excreted unchanged in the urine through filtration and secretion
102; therefore, the dosage must be adjusted in the presence of renal failure. Acyclovir is readily hemodialyzable.
91,
99Absorption of orally administered acyclovir is slow and incomplete, with bioavailability of 15% to 30%. Peak plasma levels are reached in 1.5 to 2 hours.
92 Steady-state levels after administration of 200 mg orally every 4 hours range from 1.4 to 4.0 µM (mean, 2.5 µM).
104 Although these levels are inhibitory for HSV-1 and HSV-2, they are near or below the ID
50 of VZV, which is one-tenth as sensitive as HSV-2 to acyclovir.
100,
101 However, 800 mg orally five times a day yields peak and trough serum levels of 6.9 and 3.5 µM, respectively, which have a better clinical effect on VZV.
91,
105,
106,
107Topical acyclovir 3% ophthalmic ointment has the best corneal penetration of any topical antiviral drug. It penetrates intact corneal epithelium to achieve aqueous levels well within the therapeutic range for HSV-1 and HSV-2.
38Clinically significant intraocular concentrations of acyclovir are also achieved following oral or IV administration. When 400 mg is given orally five times a day, tear
108,
109 and aqueous
110 acyclovir levels are produced in excess of the ID
50 of HSV-1. The intravitreal acyclovir level 2 hours after an IV dose of 13 mg per kg was within the therapeutic range for HSV-1 and HSV-2, VZV, and EBV.
111 Intravitreal concentrations of 8.8 to 11.0 µM may result from IV acyclovir dosages of 5 mg per kg three times a day.
101 Subconjunctival injections of 25 mg result in clinically significant aqueous and vitreous levels
112 but cause subconjunctival crystals.
Experimentally, topical acyclovir has no detrimental effect on regenerating corneal epithelium or on the healing of epithelial or stromal wounds. Nevertheless, a compilation of published clinical trials of topical acyclovir did not discover a statistically significant decrease in ocular adverse reactions compared with the other available antiviral drugs.
113 One randomized trial found a significantly decreased frequency of superficial punctate keratopathy in acyclovir recipients compared with IDU recipients.
114 Other, less common reported complications include burning or stinging, tearing, follicular conjunctivitis, palpebral allergy, and punctal stenosis.
113 In patients with ARN who received acyclovir in the infusion fluid during vitrectomy at doses of 10 to 40 µg, there was no evidence of retinal toxicity, but one patient developed a posterior subcapsular cataract.
115Acyclovir is a remarkably safe drug when used systemically for periods as long as 5 years.
116 Toxic effects are predominantly associated with high doses (more than 5 mg per kg) of the IV formulation.
117 The pH of the IV formulation is 11, and concentrated solutions are caustic. Local irritation, phlebitis, and vesicular lesions may result from subcutaneous infiltration.
118,
119 Such reactions can be circumvented by infusing acyclovir at a concentration no greater than 6 mg per mL.
120 Acyclovir’s major adverse effect is on renal function. This is due to crystallization and deposition of the drug in the kidneys of patients who are dehydrated or have preexisting renal insufficiency.
121 Renal dysfunction can be avoided by infusing acyclovir slowly over 1 hour and administering 1 L of fluid with each gram of the drug.
120 Oral acyclovir has rarely been associated with renal dysfunction.
122 Nausea, vomiting, and abdominal pain can occur and probably represent a direct toxic effect on the gastrointestinal tract.
117 There is one report of diarrhea, presumably caused by the presence of lactose in oral acyclovir tablets, which responded to oral lactase administration.
123 Reports of CNS toxicity (lethargy, confusion, obtundation, tremor, myoclonus, hallucinations, and coma) or psychiatric disturbances have occurred, mainly in association with the use of the IV formulation or with other neurotoxic agents or in the presence of renal disease.
122,
124,
125,
126,
127,
128Hypersensitivity reactions, typically transient maculopapular rashes near infusion sites, occur in less than 1% of patients.
120 Acyclovir can be incorporated into DNA, which has raised some concern over its possible mutagenicity. There is no significant evidence that acyclovir is a carcinogen.
129,
130 At much higher than clinically relevant doses, acyclovir has been teratogenic in animals,
131 but other animal studies indicate that it is not a significant teratogen.
91,
132 Although acyclovir does cross the placenta, there is no clinical evidence indicating teratogenicity.
133,
134,
135 Although its safety in pregnant women has not been established, it is often prescribed during pregnancy for treatment of genital herpes.
136A Danish population-based historical cohort study showed no increased risk of major birth defects associated with the exposure of acyclovir or valacyclovir in the first trimester.
124
Systemic Uses
Acyclovir is safe and effective for most HSV and VZV infections. IV acyclovir is the first-line treatment of HSV encephalitis and should be started as soon as the disease is suspected clinically. It can reduce mortality from 70% to nearly 20%. The recommended dosage is 10 to 15 mg per kg every 8 hours for at least 14 to 21 days to avoid relapse.
134 In immunocompromised patients, a longer treatment duration may be required.
137 IV acyclovir is effective in the treatment of neonatal HSV infections,
83 and oral long-term suppressive therapy results in improved neuro-developmental outcomes and fewer skin recurrences.
138 A number of placebo-controlled, double-blind clinical trials have demonstrated the therapeutic efficacy of oral or IV acyclovir in the treatment of primary genital HSV infections.
139,
140,
141,
142 Topical therapy is of minimal benefit
142 The recommended oral dosage is 200 mg five times daily or 400 mg three times daily for 7 to 10 days.
136,
140Oral acyclovir for 5 days is modestly effective in treating genital or orolabial HSV recurrences in immunocompetent adults.
143,
144 However, chronic oral acyclovir reduces the frequency of recurring genital HSV infection.
144 Doses of 400 mg twice daily are convenient and well tolerated.
116,
145,
146 Unfortunately, following completion of acyclovir therapy, patients may return to their previous pattern of recurrent infection. Topical acyclovir 5% cream slightly decreases the duration of an episode of orolabial herpes.
143 Oral acyclovir started within 3 days of onset of herpetic gingivostomatitis in young children significantly shortens the course of the disease.
147 However, high dose, short course (1 day) therapy of recurrent herpes labialis with oral valacyclovir or famciclovir is preferred in immunocompetent adults.
143Systemic acyclovir in various regimens can successfully prevent and treat mucocutaneous HSV infections in immunosuppressed patients.
148,
149,
150,
151,
152,
153,
154 However, recurrences commonly occur following the cessation of therapy.
Acyclovir is also of established benefit in the treatment of VZV infections in immunocompromised patients when given intravenously for 7 days at a dosage of 10 to 12 mg per kg every 8 hours.
155,
156,
157,
158,
159,
160 The indications for using acyclovir to treat VZV infections in immunocompetent adults and children with nonophthalmic disease are less obvious. IV acyclovir benefits adults when administered within 72 to 96 hours of the onset of symptoms.
156,
158 Oral acyclovir, given as 400 mg five times a day, is clinically ineffective in VZV infections in immunocompetent patients.
105,
161 However, higher doses of up to 800 mg five times a day have had some benefit when initiated within 48 to 72 hours of exanthem and are of proven efficacy in treating herpes zoster ophthalmicus (HZO).
161,
162,
163,
164,
165,
166 A meta-analysis of four placebo-controlled trials of oral acyclovir 800 mg five times daily for 7 or 10 days concluded that acyclovir accelerates pain resolution, especially in those aged 50 or older.
167 Treatment should be strongly considered for those over 50 years of age or with moderate to severe pain and definitely for ophthalmic zoster. Some consider therapy optional in young patients with uncomplicated disease.
Studies suggest that high-dose oral acyclovir, if given within 24 hours of exanthem, reduces the severity and duration (by 1 day) of primary varicella infections (chickenpox) in normal children,
168,
169 adolescents,
170 and adults.
171 It is not known if this affects the subsequent risk of herpes zoster or if it is cost-effective to treat all patients to shorten slightly the duration of a generally self-limited disease. Treatment should be strongly considered in older patients, who tend to have more severe disease than young children.
171 The American Academy of Pediatrics recommends the treatment of varicella with oral acyclovir (20 mg per kg to a maximum of 800 mg four times a day) in patients over 13 years of age, children receiving aerosolized corticosteroids, and children older than 1 year with chronic cutaneous or pulmonary conditions.
172 Treatment of infected household contacts might also be considered.
173Prophylactic high-dose IV or oral acyclovir may reduce the likelihood and severity of CMV infections in CMV-seronegative renal and CMV-seropositive bone marrow-transplant recipients.
174,
175 Trials of acyclovir in the treatment of established CMV infections, on the other hand, have shown no consistent benefit in immunosuppressed patients.
176,
177,
178,
179 In acute systemic EBV infections (e.g., infectious mononucleosis), acyclovir temporarily suppressed oropharyngeal EBV replication and excretion. However, the slight clinical benefit does not justify the routine use of acyclovir for this condition.
180,
181 High-dose oral acyclovir can cause temporary regression of EBV-induced oral hairy leukoplakia in HIV-infected patients.
182 A meta-analysis concluded that the evidence for a beneficial effect of acyclovir in severe EBV infections is inconclusive but that its use might be considered as an adjunct to corticosteroids.
181Although there is some evidence that Bell’s palsy may result from inflammation of the facial nerve in the temporal bone caused by HSV,
183 whether there is a definitive benefit from the addition of oral acyclovir to corticosteroids remains controversial. Randomized controlled studies have provided conflicting results.
184,
185 A meta-analysis suggested that, although ineffective as single agents, antivirals may provide a small additional benefit to corticosteroids when used in combination.
186
Resistance
There are at least three mechanisms of resistance to acyclovir. The most common mutation is loss of synthesis of viral thymidine kinase so that acyclovir is not phosphorylated to its active form.
92 A second type of mutation induces thymidine kinase with altered substrate specificity that phosphorylates thymidine but not acyclovir. Finally, a mutation of the viral DNA polymerase gene induces altered DNA polymerase that is not sensitive to inhibition by acyclovir triphosphate.
Acyclovir-resistant HSV and VZV mutants are uncommon in immunocompetent patients.
255,
291 Isolates of HSV-1 in the United Kingdom obtained from 40 primary ocular infections in immunocompetent patients showed reduced sensitivity in 7.5% and acyclovir-resistance in 2.5%. Sensitivity to IDU and vidarabine was retained.
292 However, a second British study found no resistance of HSV-1 viruses, although one HSV-2 isolate was resistant in vitro to all antiviral agents tested.
293 Resistance to acyclovir is more common in immunodeficient patients.
255,
294 This is especially so in patients with AIDS or transplantation patients receiving treatment for 2 weeks or more.
65,
255,
295,
296,
297 Although many thymidine kinase-deficient HSV mutants appear less neurovirulent and less efficient in establishing ganglionic latency,
298 they may cause progressive and severe mucocutaneous disease in immunocompromised patients, especially those with AIDS.
65,
66,
294,
295 Some of these patients have been successfully treated with foscarnet or cidofovir that do not rely on phosphorylation by thymidine kinase.
65,
299,
300,
301 Continuous IV infusion of high-dose acyclovir can also be effective.
302,
303 For ulcerative cutaneous lesions, topical trifluridine, topical IFN-α2 alone or in combination with topical trifluridine,
303 topical foscarnet,
304 or topical cidofovir gel and topical imiquimod
305 have also been used successfully in some patients.
Acyclovir-resistant VZV has caused hyperkeratotic skin lesions in HIV-infected patients after long-term oral acyclovir suppressive therapy.
255 The viral isolates had deficient or altered thymidine kinase function. Subtherapeutic doses or inadequate courses of acyclovir may have been factors in the development of acyclovir resistance in these cases. Foscarnet may be effective in treating acyclovir-resistant VZV.
300