Techniques of Phacoemulsification
Mark Packer
INTRODUCTION
The principle technical features of phacoemulsification include:
1. construction of watertight, self-sealing corneal incisions;
2. successful completion of an intact, round, centered capsulorrhexis with a diameter smaller than that of the intended intraocular lens (IOL) optic;
3. gentle and efficient ultrasound power modulation to protect the capsule, iris, and cornea;
4. fastidious cortical cleanup resulting in a clean capsular bag; and
5. a traumatic IOL insertion through an incision of 1.5 to 2.4 mm.
Phacoemulsification (phaco) has thus come to refer to all of the techniques and technology required for the fragmentation and extraction of the crystalline lens through a small corneal incision and the implantation of an IOL, resulting in immediate visual rehabilitation and reduced need for optical correction. The first three steps, including corneal incisions, capsulotomy, and phacofragmentation may today be performed by using either a blade, or forceps, or ultrasound, or femtosecond laser.
From the time of its introduction in the late 1960s, phaco evolved into a highly effective method of cataract extraction. Incremental advances in surgical technique and the simultaneous redesign and modification of technology permitted increased safety and efficiency. Among the advances that shaped modern phaco are incision construction, continuous curvilinear capsulorrhexis (CCC), cortical cleaving hydrodissection and hydrodelineation, and nucleofractis techniques.
United States patent 3,589,363, filed July 25, 1967, lists Anton Banko and Charles D. Kelman as inventors of “an instrument for breaking apart and removal of unwanted material, especially suitable for surgical operations such (as) cataract removal, including a handheld instrument having an operative tip vibrating at a frequency in the ultrasonic range with an amplitude controllable up to several thousandths of an inch.1” Even recently, the fundamental mechanisms by which the system known as phacoemulsification operates remained controversial. While some authors have described the surgical advantages of a unique type of cavitational energy, others have denied any role for cavitational energy in phacoemulsification.2
INCISION CONSTRUCTION AND ARCHITECTURE
Since 1992 when Fine described the self-sealing temporal clear corneal incision the availability of foldable IOLs has furthered the trend away from scleral tunnel incisions to clear corneal incisions.3 Rosen demonstrated by topographical analysis that clear corneal incisions 3 mm or less in width do not induce significant astigmatism.4 This finding led to increasing interest in T-cuts, arcuate cuts, and limbal relaxing incisions for managing preexisting astigmatism at the time of cataract surgery. Surgeons recognized many other advantages of the temporal clear corneal incision, including better preservation of preexisting filtering blebs and options for future filtering surgery, increased stability of refractive results because of decreased effects from lid blink and gravity, ease of approach, elimination of the bridle suture and iatrogenic ptosis, and improved drainage from the surgical field via the lateral canthal angle.
Surgeons originally adopted single plane incisions utilizing a 3.0 mm diamond knife. After pressurizing the eye with viscoelastic through a paracentesis, the surgeon placed the blade on the eye so that it completely applanated the eye with the point of the blade positioned at the leading edge of the anterior vascular arcade. The knife was advanced in the plane of the cornea until the shoulders, 2 mm posterior to the point of the knife, touched the external edge of the incision. Then the point of the blade was directed posteriorly to initiate the cut through Descemet’s membrane in a maneuver known as the dimple-down technique. After the tip entered the anterior chamber, the initial plane of the incision was reestablished to cut through Descemet’s in a straight-line configuration.
Williamson was the first to utilize a shallow 300 to 400 µm grooved clear corneal incision.5 Langerman6 later described the single hinge incision, in which the initial groove measured 90% of the depth of the cornea anterior to the edge of the conjunctiva. Surgeons employed adjunctive techniques to combine incisional keratorefractive surgery with clear corneal cataract incisions. Osher described the construction of arcuate keratotomy incisions at the time of cataract surgery for the correction of preexisting corneal astigmatism. Kershner7 used the temporal incision by starting with a nearly full-thickness T-cut through which he then made his corneal tunnel incision. Finally, the recommendation of limbal relaxing incisions by Gills and Gayton8 and Nichamin9 advanced the ultimately most popular means of reducing preexisting astigmatism.
Following phacoemulsification, lens implantation, and removal of residual viscoelastic, stromal hydration is performed in order to seal the incisions by gently irrigating balanced salt solution (BSS) into the stroma at both edges of the incision with a 26- or 27-gauge cannula. An intraoperative Seidel test may be used to ensure sealing. Studies of sequential optical coherence tomography (OCT) of postoperative clear corneal incisions have demonstrated that the edema from stromal hydration lasts up to one week.10
Clear corneal incisions, by nature of their architecture and location, are associated with unique complications. Chemotic ballooning of the conjunctiva may occur from irrigating fluid streaming into an inadvertent conjunctival incision. In this case, the conjunctiva may be snipped to permit decompression. Incisions that are too short can result in an increased tendency for iris prolapse and poor sealability. A single suture may be required in order to secure the wound. On the other hand, a long incision may result in striae in the cornea that compromised the surgeon’s view during phaco. Coarse manipulation of the phacoemulsification tip may result in epithelial abrasions or tears in Descemet’s membrane, compromising self-sealability. Of greater concern has been the potential for incisional burns.11 When incisional burns develop in clear corneal incisions there may be rapid contraction of tissue and loss of self-sealability. Suture closure of the wound may induce excessive astigmatism.
Literature supports the view that suboptimal construction of clear corneal incisions may lead to poor coaptation, inadequate sealing and ingress of bacteria, thereby increasing the risk of acute postoperative bacterial endophthalmitis.12 However, four large published series have found no greater likelihood of infection with corneal versus other types of incisions.13,14,15,16 Regardless of the type of incision, the principle remains that appropriate incision construction and watertight closure are obligatory. Besides poor wound closure, other significant findings have been associated with higher risk of postoperative infection, including posterior capsule rupture, vitreous loss, older age, prolonged surgery, immunodeficiency, active blepharitis, lacrimal duct obstruction, inferior incision location, and male gender.17
CONTINUOUS CURVILINEAR CAPSULORRHEXIS
Implantation of the IOL in an intact capsular bag facilitates the permanent rehabilitative benefit of cataract surgery. For many years, surgeons considered a “can-opener” capsulotomy satisfactory for both planned extracapsular cataract extraction and phaco. However, in 1991, Wasserman and associates performed a postmortem study that showed that the extension of one or more V-shaped tears toward the equator of the capsule produced instability of the IOL and resulted in IOL malposition.18 Gimbel and Neuhann popularized CCC in the late 1980s.19,20,21
The basic principles of manual CCC include the following:
1. The continuous capsular tear should be performed in a stable anterior chamber under viscoelastic pressurization.
2. The tear should be initiated at the center of the capsule so that the origin is included within the circle of the tear.
3. The continuous tear may proceed either clockwise or counter-clockwise in a controlled and deliberate fashion, the surgeon regrasping with the forceps or repositioning the point of the cystotome/bent needle on the inverted flap to control the vector of the tear.
A tear that begins moving peripherally or radially is a signal that a condition exists that requires immediate attention. Further progress of the tear should be stopped and the depth of the anterior chamber assessed. Frequently, the cause of the peripheral course of the tear is shallowing of the anterior chamber. Adding more viscoelastic to deepen the anterior chamber opposes the posterior pressure, making the lens capsule taut, widening the pupil, and permitting inspection of the capsule.
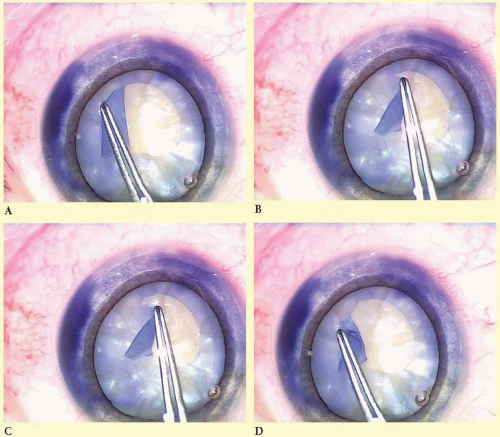
One important technique for redirection of the capsulorrhexis has been described by Little et al.22 In this technique, in order to rescue the capsulorrhexis from a peripheral tear-out, the force applied to the capsular flap is reversed, but maintained in the plane of the anterior capsule. It is necessary to first unfold the capsular flap so that it lies flat against the lens cortex as it did prior to being torn. Force can then be applied with the capsule forceps holding the capsular flap as near to the root of the tear as possible and pulling backwards, in a retrograde direction along the circumferential path of the completed portion of the capsulorrhexis. Traction should be applied in the horizontal plane of the capsule and not upward. The initial pull should be circumferentially backward, and then, while holding the flap under tension, directed more centrally to initiate the tear. The forward progress of the capsulorrhexis will uniformly and predictably redirect toward the center of the capsule (Fig. 7.1). In the event that the capsule will not tear easily and the entire lens is being pulled centrally, this rescue maneuver should be abandoned to avoid a wrap-around capsular tear or zonular dialysis. Alternate rescue techniques such as completing the capsulorrhexis from the opposite direction or making a relieving cut in the flap edge and continuing in the same direction represent reasonable alternatives.
The use of trypan blue to stain the anterior capsule in the absence of a good red reflex constitutes an important adjunctive technique for capsulorrhexis construction. The dye may be injected into the chamber through a paracentesis under air. The air and residual dye are then exchanged for viscoelastic. Despite the absence of a red reflex the capsule is easy to see.
The technique of CCC has provided important advantages both for cataract surgery and IOL implantation. Because endolenticular or in situ phaco must be performed in the presence of an intact continuous capsulotomy opening, the capsulorrhexis has served as a stimulus for modification of phaco techniques. Because the edge of a well-constructed rhexis completely overlaps the edge of the IOL, it insures positional stability and enhances refractive predictability.
HYDRODISSECTION AND HYDRODELINEATION
Hydrodissection has traditionally meant the injection of fluid into the cortical layer of the lens to separate the nucleus from the cortex and capsule. Following the adoption of capsulorrhexis, hydrodissection became a critical step to mobilize, disassemble, and remove the nucleus. Fine first described cortical cleaving hydrodissection, which is designed to cleave the cortex from the capsule and leave the cortex attached to the epinucleus.23 Cortical cleaving hydrodissection often eliminates the need for cortical cleanup as a separate step in cataract surgery.
In this technique, the anterior capsular flap is initially elevated with a 26-gauge blunt cannula. Firm and gentle continuous irrigation results in a fluid wave that cleaves the cortex from the posterior capsule. The lens bulges forward because fluid is trapped by equatorial cortical-capsular connections. Depressing the central portion of the lens with the side of the cannula forces the fluid around the equator and lyses the cortical-capsular connections. Adequate hydrodissection is demonstrated by rotation of the nuclear-cortical complex. The demonstration of free rotation of the lens within the capsule represents a critical step in phacoemulsification.
Hydrodelineation describes separation of the epinuclear shell from the endonucleus by irrigation. The epinucleus acts as a protective cushion within which phacoemulsification forces can be confined. Further, the epinucleus keeps the bag on stretch throughout the procedure, making capsule rupture less likely.
To perform hydrodelineation, a 26-gauge cannula is placed in the nucleus, off-center to either side, and directed at an angle downward and forward toward the central plane of the nucleus. When the nucleus starts to move, the endonucleus has been reached. At this point, the cannula is directed tangentially to the endonucleus, and a to-and-fro movement of the cannula is used to create a tunnel within the epinucleus. The cannula is backed out of the tunnel approximately halfway, and gentle but steady pressure on the syringe allows fluid to enter the distal tunnel without resistance. A circumferential golden or dark ring will outline the endonucleus.
Occasionally, an arc will result and surround approximately one quadrant of the endonucleus. In this instance, the procedure can be repeated in multiple quadrants until a golden or dark ring verifies complete circumferential separation of the nucleus.
NUCLEOFRACTIS TECHNIQUES
The recognition that the lens nucleus could be divided and removed from within the protective layer of the epinucleus while preserving the capsulorrhexis influenced the development of a plethora of phaco techniques.
Divide and Conquer
In the divide and conquer technique originally described by Gimbel,24 a deep crater is sculpted into the center of the nucleus including the posterior plate. However, phaco fracture, a technique actually described by Shepherd, is often referred to as “divide and conquer.”25 In this technique the surgeon sculpts a groove parallel to the incision one and a half to two times the diameter of the phaco tip, with the tip in a bevel-up position, using moderate power and low vacuum. Using the phaco handpiece and a second instrument, the surgeon then rotates the nucleus 90 degrees and sculpts a second groove perpendicular to the first. Sculpting continues until the red reflex is seen at the bottom of the grooves. A bimanual cracking technique is used to create a fracture through the nuclear rim in the plane of one of the grooves. The nucleus is then rotated 90 degrees, and additional fractures are made until four separate quadrants are isolated. A short burst of phaco power with increased vacuum is then used to embed the phaco tip into one quadrant which is pulled into the center for emulsification. The second instrument can help elevate the apex of the quadrant to facilitate its mobilization.
Phaco Chop
Nagahara first introduced the phaco chop technique by using the natural fault lines in the lens nucleus to create cracks without creating prior grooves (Presentation at the American Society of Cataract and Refractive Surgery Film Festival, 1993). The phaco tip is embedded in the center of the nucleus after the superficial cortex is aspirated. In horizontal chopping, a second instrument, the phaco chopper, is then passed to the equator of the nucleus, beneath the anterior capsule, and drawn to the phaco tip to fracture the nucleus. The two instruments are separated to widen the crack. In vertical chopping a sharp-tipped instrument is inserted directly into the nucleus beside the embedded phaco needle and the two instruments are again separated as in horizontal chopping. The nucleus is rotated and this procedure is repeated until several small fragments are created, which are then emulsified.
Power Modulations
Fine described the “choo-choo chop and flip” technique in 1998 and subsequently correlated the reduction of ultrasound energy made possible by power modulations with superior uncorrected visual acuity on the first postoperative day.26,27 Effective phaco time (EPT), absolute phaco time (APT), and cumulative dissipated energy (CDE) became standard metrics for consumption of ultrasound energy. Although EPT, APT, and CDE cannot be compared across different machines made by different manufactures, when using the same machine they can be compared from one case to the next as a sign of surgical safety and efficiency.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree