Purpose
To investigate the repeatability of tear meniscus measurements using anterior segment swept-source optical coherence tomography (OCT) and the relationship of tear meniscus measurements with tear film breakup time and Schirmer test results.
Design
Prospective, observational, cross-sectional study.
Methods
We enrolled 26 healthy subjects (26 eyes; 20 men and 6 women; mean age, 36.5 ± 6.8 years) at the University of Tokyo School of Medicine, Tokyo, Japan, in this study. Examinations were conducted in the following sequence: anterior segment vertical raster scans by swept-source OCT, tear film breakup time, and Schirmer test. Each subject underwent OCT measurements twice by the same grader, and the central upper and lower tear menisci height and area and the lower tear meniscus volume were examined. Each OCT image was evaluated by 2 masked graders using the software calipers.
Results
The average upper and lower tear meniscus heights were 231 ± 78 μm and 256 ± 57 μm, respectively, and the average upper and lower tear meniscus areas were 18 829 ± 7823 μm 2 and 21 903 ± 8173 μm 2 , respectively. The average tear meniscus volume was 0.1327 ± 0.051 mm 3 . The intergrader intraclass correlations for all the parameters were more than 95%. The OCT tear meniscus measurements and the Schirmer test scores were correlated significantly ( P < .05, Spearman nonparametric correlation analysis). However, tear film breakup time was not correlated significantly with any of the parameters of tear menisci ( P > .05).
Conclusions
Anterior segment swept-source OCT is a noninvasive and practical method that can be used for quantitative evaluation of tear fluid.
The tear meniscus is a thin strip of tear fluid at the upper and lower lid margins of the eyelid. The tear meniscus retains tear fluid by its internal negative pressure and holds approximately 75% to 90% of the total tear volume of the exposed ocular surface. The Schirmer test, the cotton-thread test, and tear film breakup time (TBUT) are the conventional methods that reflect tear fluid status in terms of its secretion, drainage, and evaporation. However, there have been concerns about the poor repeatability, poor correlations with the symptoms, and invasiveness of the tests. Consequently, noninvasive tear meniscus evaluation is an essential requirement for diagnosis of dry eye and other diseases associated with tear fluid anomaly.
Several techniques, including slit-lamp evaluation with a graticule scale, optical pachymetry, videokeratography, and video meniscometery, have been used to assess the tear meniscus. Recently, anterior segment optical coherence tomography (OCT) has been used increasingly because it is a practicable method for measuring the tear meniscus.
Fourier-domain swept-source anterior segment OCT with a wavelength of 1310 nm (SS-1000; Tomey Corp, Nagoya, Japan) allows 3-dimensional imaging in addition to cross-sectional imaging of the anterior segment of the eyes. This OCT system allows higher speed of data acquisition, greater imaging depth, and wider observable range, which is reported to yield high repeatability and reproducibility of anterior ocular biometric measurements. Further, the 3-dimensional imaging of a newly installed system in the SS-1000 made it possible to measure the tear meniscus height, area, and volume. In this study, we aimed to investigate the repeatability of SS-1000 for tear meniscus measurements and to examine the relationship of these tear meniscus measurements with tear fluid parameters in normal subjects.
Methods
Patient Population
This study followed the tenets of the Declaration of Helsinki; the prospective protocol-driven study was approved by the Institutional Review Board of the University of Tokyo School of Medicine, Tokyo, Japan; and written informed consent to participate in research protocol was obtained from all subjects. The observational cross-sectional study population consisted of 26 healthy right eyes of 26 Japanese subjects (20 men and 6 women). The exclusion criteria were presence of ocular diseases, history of intraocular surgeries including refractive surgeries, TBUT of fewer than 5 seconds, Schirmer values of less than 5 mm, instillation of any kind of eye drops in the previous 24 hours, contact lens wear within 2 weeks, and any use of systemic medication.
Tear Meniscus Measurements
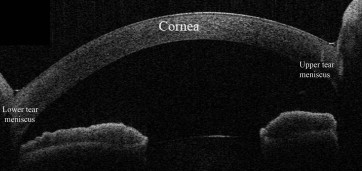
Anterior segment imaging using the SS-1000 with custom 16 vertical raster scans at 1-mm intervals was performed for all subjects. This custom scan mode, which we referred to as the tear meniscus mode, was used to obtain a total of 16 cross-sectional images of the anterior segment with width of 16 mm and length of 16 mm. A scan with angle of 90 degrees visualizes both upper and lower tear meniscus simultaneously ( Figure 1 ). The acquisition time for all scans is 0.3 seconds. The OCT image consists of 512 A-scans, with an axial resolution of approximately 8 μm and a transverse resolution of approximately 30 μm. Subjects were asked to look straight at a fixation light with no background illumination and were allowed to blink spontaneously during the examination. The right eyes were examined, but the contralateral eyes were maintained open while capturing the image. All subjects underwent OCT examination 1 second after blinking. Stable ambient room light was maintained during the examination. After 15 minutes, the same examiner (R.F.) repeated the scan for 17 subjects who consented to repeat the examination procedure. The upper and lower tear meniscus height, upper and lower tear meniscus area, and lower tear meniscus volume were evaluated using the SS-1000 by 2 masked graders (R.F.,T.U.).
First, the original OCT images were magnified by 300% to measure the tear meniscus. Both the upper and lower tear meniscus height values were measured manually using the software calipers on the vertical scan image across the central cornea. The central cornea in this case refers to the apex of the cornea, in which this OCT focuses automatically while capturing the image. Second, outlines of both the upper and lower tear meniscus at the central cornea, which consisted of the corneal surface, lid margin, and tear meniscus surface, were plotted manually using the software calipers ( Figure 2 ). At least 9 points were used for the plotting of each image. The area within the plotted lines, the tear meniscus area, was calculated automatically by the program, and the resulting tear meniscus area value was divided by the refractive index of balanced salt solution (1.343) to correct the refraction at the air–meniscus interface. Finally, the central 11 images of 10 mm in width were selected among the 16 images. The lower tear meniscus area of each image was identified as mentioned above, and the tear meniscus area of 11 consecutive images was integrated automatically by the program to calculate the tear meniscus volume. Again, the calculated value was corrected using 1.343 ( Supplemental Figure at AJO.com ). Because the program required consecutive images to calculate the volume, the upper tear meniscus volume could not be evaluated because the presence of eyelashes rendered it difficult to visualize the entire upper tear meniscus adequately.
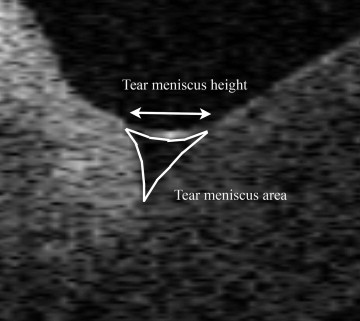
Examinations
The other ophthalmic examinations were slit-lamp microscopy, fluorescein staining, TBUT, and Schirmer test without local anesthesia. A fluorescein sodium strip was wetted with a drop of nonpreservative buffered saline solution and was instilled in the inferior palpebral conjunctiva. The TBUT measurement was obtained twice, and the mean value of the measurements was calculated. Fluorescein staining of the ocular surface also was recorded as described previously. Fluorescein staining scores ranged between 0 and 9 points. Five minutes after the TBUT test, the Schirmer test was performed without anesthesia. A dry Schirmer test strip (Showa Yakuhin Kako Co, Tokyo, Japan) was placed over the lower lid margin on the conjunctival sac at the lateral one third of the eyelid. After 5 minutes with the subject’s eyes closed, the strip was removed and the amount of wetting was recorded in millimeters.
Statistical Analysis
The intergrader repeatability and interimage repeatability of the tear meniscus height, area, and volume were analyzed. Further, the intraclass correlation coefficient (ICC) and coefficient of variation (CV) for the tear meniscus measurements were evaluated. ICC has been advocated as a statistic for assessing the agreement or consistency between 2 methods of measurement. The CV shows the extent of variability in relation to the mean of the population. It is defined as the ratio of the standard deviation to the mean, multiplied by 100 to be expressed as a percent. Correlations between the tear meniscus measurements and tear fluid parameters including TBUT and Schirmer values were analyzed using the Spearman nonparametric correlation analysis.
Results
The average upper and lower tear meniscus heights were 231 ± 78 μm and 256 ± 57 μm, respectively, and the average upper and lower tear meniscus areas were 18 829 ± 7823 μm 2 and 21 903 ± 8173 μm 2 , respectively. The average tear meniscus volume was 0.1327 ± 0.051 mm 3 . The mean TBUT value was 9.73 ± 3.53 seconds, and the mean Schirmer test score was 20.42 ± 11.13 mm. The average fluorescein score was 0.73 ± 1.15 points.
Statistically significant correlations were present between the upper and lower tear meniscus height ( P = .003, r = 0.574) and the upper and lower tear meniscus area ( P = .006, r = 0.541). Predictably, tear meniscus height was correlated significantly with tear meniscus area in both the upper and lower tear meniscus ( P < .001 and r = 0.794, and P < .001 and r = 0.819, respectively). Moreover, the lower tear meniscus height and tear meniscus volume values showed greater significant correlation ( P < 0.001, r = 0.830).
Table 1 shows the intergrader and the interimage repeatability as ICC and CV for each tear meniscus measurement. The intergrader repeatability, measured as the ICC, was more than 95% for all the tear meniscus parameters, showing excellent repeatability. Although the interimage repeatability was slightly inferior, particularly that of the upper tear meniscus assessment, our findings indicated acceptable reliability of OCT measurements.
| TMH | TMA | TMV | |||
|---|---|---|---|---|---|
| Upper | Lower | Upper | Lower | ||
| Intergrader ICC (%) | 96.6 | 97.6 | 95.1 | 97.0 | 96.9 |
| Intergrader CV (%) | 19.4 | 10.7 | 28.4 | 18.9 | 18.9 |
| Interimage ICC (%) | 69.4 | 78.3 | 63.8 | 83.2 | 71.3 |
| Interimage CV (%) | 25.0 | 19.7 | 34.4 | 36.8 | 34.7 |
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


