Strabismus
Alex V. Levin
Thomas W. Wilson
Stephen P. Kraft
David Smith
Linda Calpa
Strabismus can be classified into congenital or acquired forms, as well as comitant versus incomitant entities. Congenital strabismus is generally considered a misalignment that manifests within the first 6 months of life, while acquired forms have their onset after that time period. Comitant strabismus implies that the degree of misalignment is the same in all fields of gaze, contrasting with incomitant strabismus, in which the measured angle of the eye turn varies in the different fields of gaze.
Incomitant strabismus can vary in the horizontal or vertical plane, or both. If a horizontal misalignment (esotropia or exotropia) differs in the upgaze and downgaze positions, this leads to pattern strabismus (including A, V, Lambda, Y, or X patterns). A misalignment, either horizontal or vertical, that changes when shifting from the right to left gaze positions generates a horizontal incomitance. Finally, if a vertical misalignment (hypertropia or hypotropia) changes on fixating from upgaze to downgaze, this is termed a vertical incomitance.
Incomitant strabismus can be classified etiologically into innervational and mechanical forms. Innervational entities include innervation deficits (paresis or palsy), which can be supranuclear, nuclear, or infranuclear. Excess innervation of muscles may also occur. Mechanical causes imply restrictions due to problems within the orbit, and these can include abnormalities in the muscles, soft tissues, or bones, as well as lesions within the socket. Restrictions can be caused by congenital disorders or they can be acquired as a result of trauma, surgery, systemic disorders, or other problems.
I. Comitant Strabismus
a) Esotropia
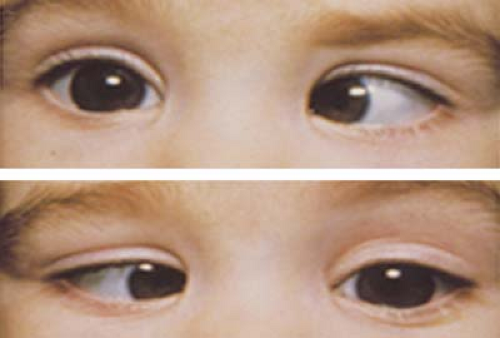
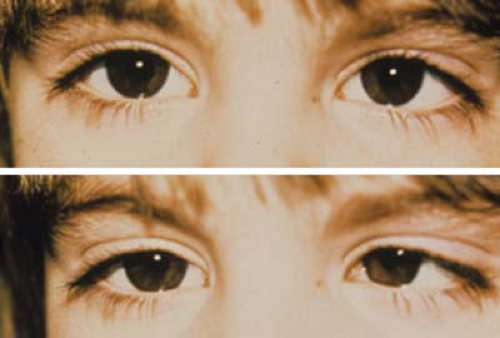
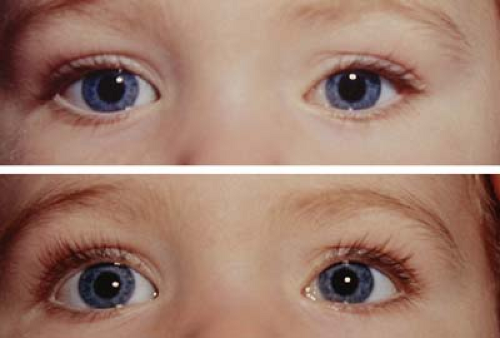
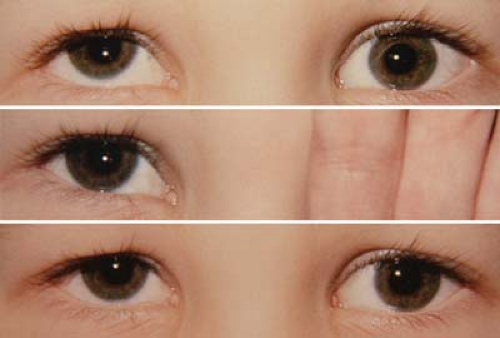
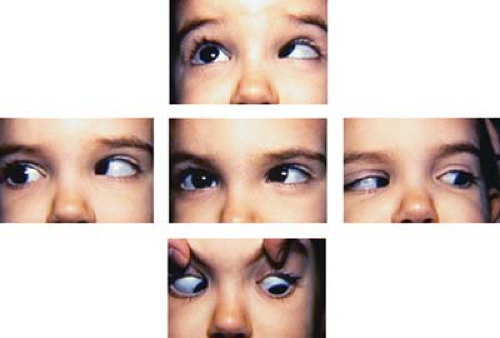 Figure 1.1 Infantile Esotropia Infantile esotropia, also referred to as essential infantile esotropia or by the older term congenital esotropia, presents as a manifest deviation with onset before 6 months of age. The angle of deviation is usually over 30 prism diopters. The eye movements are full in the vertical and horizontal planes except for mildly limited abduction of the right eye. As these children often cross-fixate, using the adducted eye to view the contralateral field rather than abducting the ipsilateral eye, it can be difficult to elicit full abduction. A rapid Doll head maneuver or patching the nontested eye may be required to elicit abduction. Infantile esotropia is also associated with inferior oblique overaction (note left eye in upgaze; also see Fig. 1.31), dissociated vertical deviation (Figs. 1.19 and 1.20), latent nystagmus, and, less commonly, manifest nystagmus. |
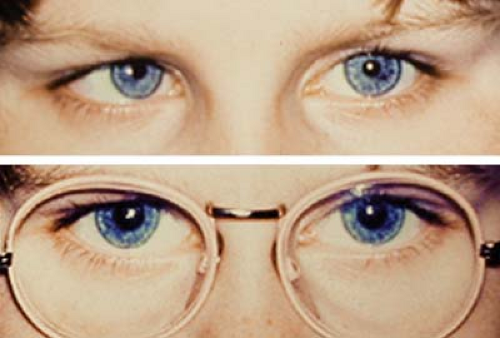
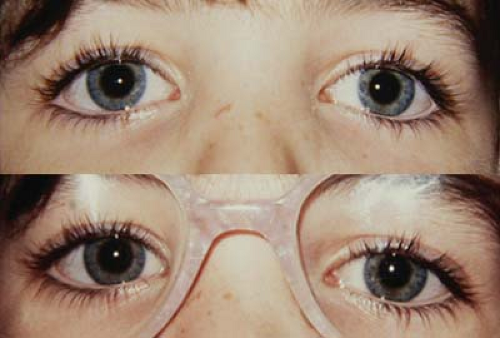
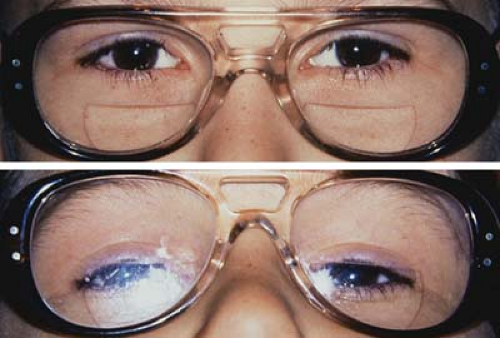 Figure 1.8 Bifocals Set Too Low The upper image shows the bifocal set several millimeters below the lower eyelids. The child is viewing a distance target with full hyperopic correction for his accommodative esotropia: The eyes are straight. The lower image shows the child fixating through the bifocal in the near position. While the add is effective in maintaining good alignment for the excess near deviation (convergence excess, see Fig. 1.6), the child has to use an awkward chin-up head posture to be able to use the bifocal segment. Figure 1.7 demonstrates proper spectacle construction for this disorder. |
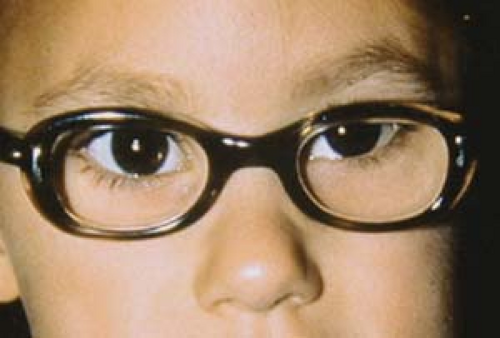
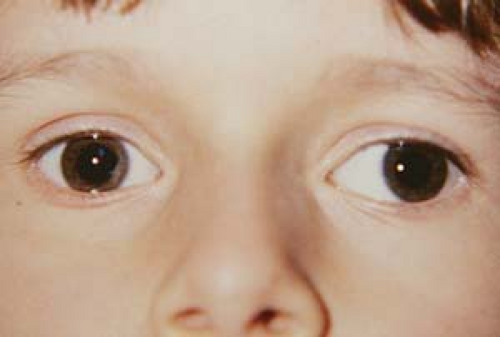
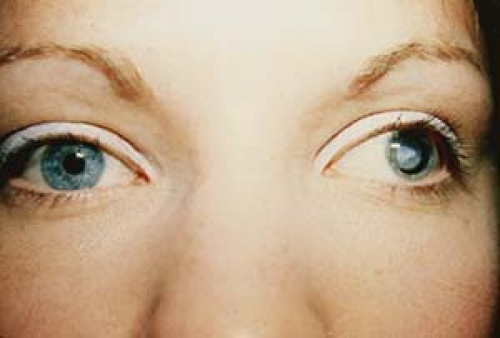
 Figure 1.10 Negative Angle Kappa In this photo the patient is fixating with her right eye. However, the light reflex in that eye is located slightly temporal within the pupil when compared to the centered reflex in the left eye, giving the child the appearance of a right esotropia. A cover test will show no movement of the right eye on covering the left eye, indicating that there is no strabismus. The off-centered light reflex persists under monocular conditions in the right eye. This is due to a negative angle kappa: A disparity between the visual axis (joining target and fovea) and the anatomic pupillary axis (joining midpupil to fovea). (Compare to Fig. 1.18, positive angle kappa.) |
b) Exotropia
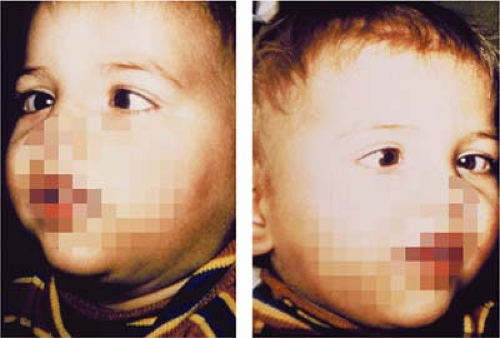
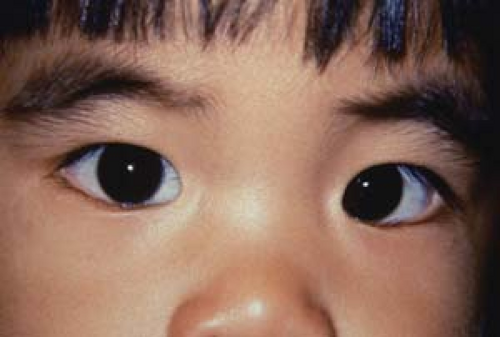
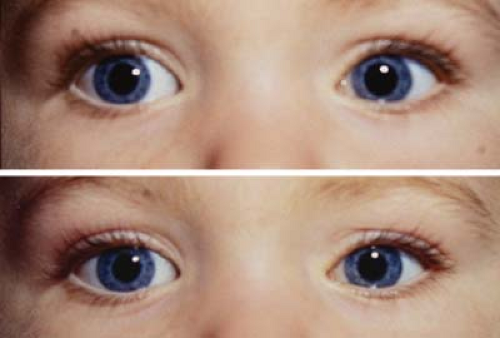
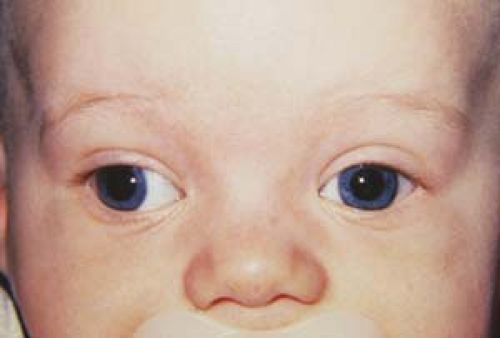 Figure 1.16 Infantile Exotropia The photo shows an infant with a large-angle right exotropia, which presented before the age of 6 months. Infantile exotropia, also known as essential or congenital exotropia, is much rarer than infantile esotropia (Fig. 1.1). The exodeviation is usually very large, almost always over 40 prism diopters. Infantile exotropia has also been reported in association with various neurologic and developmental disorders. |
II. Dissociated Deviations
a) Dissociated Vertical Deviation
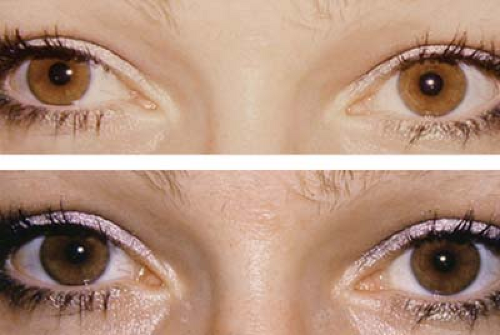
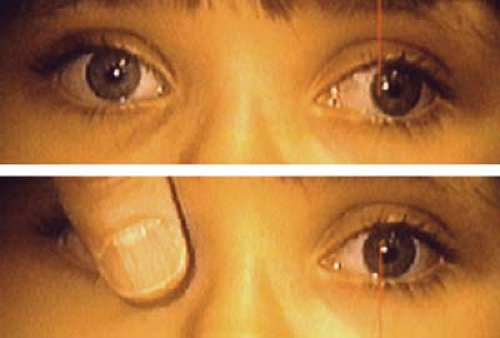
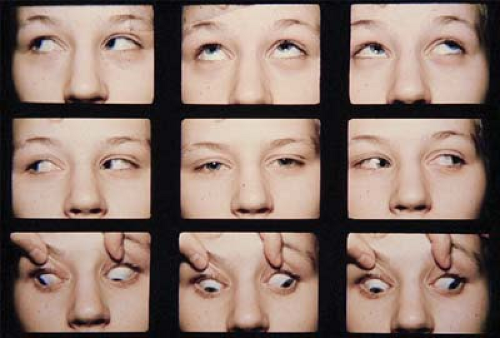
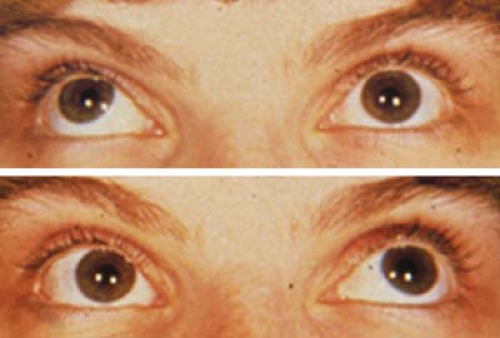 Figure 1.20 Bilateral Dissociated Vertical Deviation (DVD) The upper photo shows that when the patient fixates with the left eye the right eye drifts upward and outward. The lower photo shows that when she fixates with the right eye the left eye drifts upward and outward. Indirect ophthalmoscopy showed excyclotropia of the hyperdeviated eye in each instance. These findings confirm the presence of bilateral DVD. Note that there is never a hypotropia of the fixating eye when fixation is switched (Fig. 1.19). If a patient presents with a latent or manifest DVD in one eye, patching of the fellow eye for several minutes may bring out a bilateral DVD that was not apparent on initial examination. In side gaze, fixation by the adducting eye can be blocked by the nose, causing that eye to drift upward. To differentiate this from overaction of the inferior oblique (Fig. 1.31), a cross-cover test will fail to show a hypotropia of the abducting eye in DVD. |
b) Dissociated Horizontal Deviation
III. Incomitant Strabismus: Patterns
a) A-pattern Strabismus
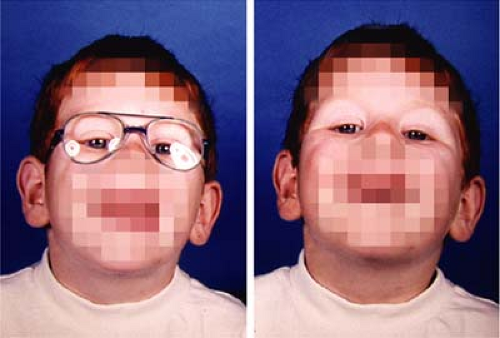 Figure 1.27 Head Posture with A-pattern Esotropia
Stay updated, free articles. Join our Telegram channel
Full access? Get Clinical Tree
 Get Clinical Tree app for offline access
Get Clinical Tree app for offline access

|