Chapter 78 Special forms of comitant exotropia
Introduction
Exodeviations in children can be comitant or non-comitant. Non-comitant exodeviations result from either innervational causes, i.e. third nerve paresis and Duane’s syndrome, or mechanical causes, such as tumors or trauma (see Chapters 82 and 83).
Infantile exotropia
Introduction
Infantile exotropia is an exodeviation that develops within the first few months of life and persists. While infantile esotropia is generally defined as having its onset by age 6 months, the term infantile exotropia is used for exodeviations that first manifest up to 1 year of age.1–6 It can be a primary disorder or secondary to an ocular or systemic problem.
Primary infantile exotropia, unrelated to a systemic or ocular disorder, is rare, roughly 1 per 30 000 births.7 In primary strabismus in infancy, for every case with exotropia there are between 150 and 300 cases with esotropia.8 Intermittent exotropia can manifest by age 12 months, and it may represent a large minority of cases of exotropia seen before age 1 year (see Chapter 77).6 Infantile exotropia is often associated with ocular or systemic disorders. It is seen with ptosis, albinism, ocular motor apraxia (saccadic initiation failure), optic nerve anomalies, and with diseases that lead to vision loss, including retinoblastoma, retinoschisis, iridolenticular abnormalities, and cataracts.8–10 Exotropia can be a feature of several congenital strabismus syndromes, including third nerve palsies, Duane’s syndrome, congenital fibrosis of the extraocular muscles, and strabismus fixus8,9 (see Chapter 82). It is described in association with many systemic disorders including prematurity, cerebral palsy, seizure disorders, hydrocephalus, craniofacial syndromes, and various chromosomal anomalies.1,4,5,8,10,11
Ocular or systemic disorders are more common in infantile exotropias than in esotropias, and infants with constant exotropia have a much stronger chance than those with intermittent exotropia of having a coexisting problem.5,9 The incidence of systemic anomalies may also be positively correlated with the size of the angle of deviation:5 it is prudent to consider a neurodevelopmental assessment of a child with infantile exotropia.
Etiology
Vergence abnormalities
Exodeviations appear in over one-third of healthy neonates, while esodeviations are rare.12,13 Mostly, they are transient and resolve by 6 months as the vergence system matures.13 Therefore, primary infantile exotropia may be an arrested development of the convergence system.
Abnormal convergence may be a primary or secondary phenomenon. There may be a primary convergence deficit in the convergence system, or it may arise from defective cortical binocular development.14 Disruption of binocular connections in the immature visual cortex potently disrupts development of vergence, leading to strabismus and to functional deficits, loss of fusion, asymmetric monocular smooth pursuit, and asymmetric monocular motion perception.14 The asymmetries are characterized by better tracking and detection of targets when they are followed from the temporal to the nasal visual field than when they are tracked in the reverse direction. This directional asymmetry should lead to infantile esotropia, rather than exotropia. Therefore, the severity of a primary or secondary convergence system deficit must override the other abnormal processes such that divergence is predominant. The identical pursuit asymmetry seen in infantile esotropia also occurs in infantile exotropia (L Tychsen, personal communication, 2001).
Anatomic factors
An asymmetry in the structure of the lateral and medial rectus muscles occurs with the length–tension curve of the lateral rectus showing more stiffness than the medial rectus and the diameter of the lateral rectus may be congenitally larger than normal, allowing it to “overpower” the medial rectus.8 Finally, orbital dysmorphism, as in craniofacial syndromes, can produce a divergent positioning of the eyes.
Clinical features
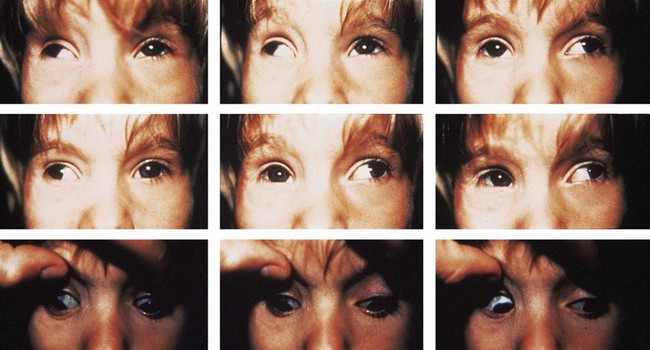
Infantile exotropia occurs by 12 months of age.1,3,8 It can have a wide range of angles, from 20 to 90 prism diopters (PD), with most cases more than 35 PD7,9,11,15 (Fig. 78.1). The angle is usually stable initially, increasing slowly.6 Amblyopia occurs in up to 25%, usually caused by strabismus rather than anisometropia.8 It responds to the usual treatments (see Chapter 70). There is a normal distribution of refractive errors.7,8 If the deviation is large, an “X” pattern strabismus is common, as also seen in adults with large angle exotropia who have a tight lateral rectus syndrome. The deviation is larger in upgaze and downgaze than in the primary position with mild limitation of adduction in one or both eyes and upshoots and downshoots in adduction (see Fig. 78.1) which have been ascribed to contracture with overactions of the oblique muscles, to sideslip of the lateral rectus around the globe (a “leash effect”), or to the globe having more room to elevate and depress when it is not fully adducted.8,16,17 Alternatively, there may be “A” or, more commonly, “V” patterns.1,4,7,11,15 Latent nystagmus, dissociated vertical deviations, and inferior oblique overactions may occur, as with infantile esotropia, but less frequently.1,3,4,6
Examination
Some pertinent points must be noted in the evaluation of infantile exotropia.
1. The general behavior and physical features of the child may suggest a systemic or orbital association.
2. Anterior and posterior segment disorders can be associated with infantile exotropia. A cycloplegic refraction is vital.
3. The examiner must observe the corneal light reflexes to rule out a positive angle kappa that gives a false appearance of exotropia:8 the cover test will confirm a true exodeviation rather than a pseudo-exotropia (see Chapters 7 and 72).
4. When the angle is large, the examiner needs to use two prisms oriented base-in and split between the two eyes to get an approximation of the total angle, whether the angle is measured by the Krimsky or prism and alternating cover methods (see Chapter 72).
5. The examiner should search for features of the infantile strabismus complex including dissociated vertical deviations and oblique muscle overactions. Optokinetic testing may detect monocular nasal–temporal motion asymmetries.
Management
Non-surgical therapy
Infantile exotropia usually requires surgery after any refractive errors and amblyopia have been treated. Although the angle of the deviation is generally stable, the strabismus angle may reduce with occlusion.1
Botulinum toxin injections have been used for infantile esotropia, but there are no reports on series of cases of the rarer infantile exotropia and success rates range from 50% to 70%, with bilateral, not unilateral, lateral rectus injections.18,19 Most had intermittent exotropia: the success rates for exotropia over 35 to 40 PD was much lower, and, since most infantile exotropias are larger than this, botulinum toxin may be less successful than surgery for deviations over 35 PD.
Surgery
Timing
Patients with primary infantile exotropia should be approached in the same manner as those with infantile esotropia where the general consensus among pediatric ophthalmologists for many years was to align the eyes before the age of 24 months to achieve optimal motor and sensory results.2,3,7,20 In recent years, earlier surgery has been favored in the belief that it is more effective in reversing the binocular vision and vergence deficits. Evidence suggests that the optimal “window” for treating infantile esotropia may be the first 8 to 10 months of life21 but whether it is applicable to infantile exotropia is not known. The consensus still favors realigning the eyes before 24 months of age. Once the diagnosis of infantile exotropia is confirmed and any refractive error or amblyopia is corrected, the child should be followed for a few weeks to be sure the angle of the strabismus is stable.
Surgical planning
Strabismus surgery techniques for exotropia are described in Chapter 85, but there are some specific recommendations for surgical treatment of infantile exotropia:
1. The aim in primary infantile exotropia is to create an esotropia in the immediate postoperative period, as in most exotropias in older children and adults.1,7 This principle also applies to children with infantile exotropia and developmental delay or cerebral palsy, as the postoperative drift is usually in the divergent direction whether they originally had esotropia or exotropia immediately after surgery.8 For either category, the best result in a single operation seems to require an immediate postoperative angle in the range of 10 to 14 PD, which is slightly larger than is usually targeted for later-onset intermittent exotropia.
2. The strategy generally involves weakening (usually recession) of one or both lateral rectus muscles, as they are often tight. If the near exotropia is larger than that at distance, then a strengthening (usually a resection) of a medial rectus muscle should be included.8
3. Strabismus angles under 40 PD can usually be successfully treated with surgery on two horizontal muscles, either bilateral lateral rectus recessions or a unilateral lateral rectus recession with a medial rectus resection.1 Treatment of angles over 40 PD may require “supramaximal” amounts of recessions or resections if surgery is limited to two muscles. Alternatively, surgery of more “regular” dosages can be planned on three or four horizontal muscles.1,3,4,7,11,15,20 Another strategy involves large recessions of both lateral rectus muscles combined with simultaneous injections of botulinum toxin into the two muscles.
4. Surgery for any coexisting dissociated vertical deviations or oblique overactions can be planned for the same sitting or for subsequent surgery, as in infantile esotropia.
Results
The success rates for infantile exotropia surgery are not high. Reoperation rates are as high as 50% of patients: undercorrections are more common than overcorrections.1,3,11,15,20
Young children who are aligned before age 24 months develop peripheral fusion in up to 50% of cases: some may show gross stereopsis.1,11,15,20 The best binocular outcomes reported are monofixation syndromes.6 Realigning patients with infantile exotropia after age 2 years can lead to stable long-term results, but sensory fusion is rarely achieved after this age.7,8
Monofixational exotropia
Introduction
The monofixation syndrome is characterized by fixation with the fovea of only one eye under binocular conditions.8,22 Sensory features include intact peripheral fusion, preserved gross stereopsis and, frequently, amblyopia of the non-foveating eye. The motor features include manifest heterotropia of under 8 PD, a larger heterophoria, and preserved convergence and divergence fusional amplitudes.22–24 Some cases show no heterotropia on cover test: they are termed monofixational phorias. Some show a heterotropia without a heterophoria: these are sometimes termed microtropias (see Chapter 76).22
In most cases of monofixation syndrome, if there is a small angle heterotropia, it is an esotropia, and any associated heterophoria is an esophoria. However, about 20% have an exotropic orientation for the tropia and the phoria.22,23,25–28 Most cases of monofixational exotropia are secondary, either associated with anisometropia or following surgery for exotropia. However, a monofixation syndrome may underlie some cases of intermittent exotropia and its true nature may only become evident after surgery for the total exodeviation.23,29
Most cases of monofixational exotropia, by virtue of intact vergence amplitudes, retain a stable long-term small exotropia under binocular conditions. In a minority, fusion control is disrupted and the exophoria becomes predominant: this is termed a decompensated monofixational exotropia.22,23,25
Etiology
Primary monofixation exotropia
Patients with the primary form have a deficit in fovea-to-fovea correspondence: they cannot attain bifoveal fusion.22 This may be an hereditary error in foveal correspondence that may exceed the capability of Panum’s fusional space to compensate for it, leading to suppression of the less dominant fovea.8 Alternatively, there may be a reversal of the normal dominance of the nasal over the temporal hemifield. As a result, any degree of foveal disparity can lead to a facultative scotoma on the temporal side of the fovea rather than in its usual location on the nasal side.8,24,30
A primary monofixational exotropia can decompensate because of an acute illness or chronic fatigue and the “all or none” suppression in exodeviations is less flexible than that in esodeviations.30,31 If the latent heterophoria begins to manifest, then the strong hemiretinal suppression mechanism may increase the propensity for the exodeviation to decompensate.8,31
Secondary monofixational exotropia
The majority of secondary forms in children result from surgery for constant or intermittent exotropia.26 Monofixation after surgery suggests a pre-existing defect in bifoveal fusion, and this may underlie a minority of cases of seemingly typical intermittent exotropia.22,25,26,29 Anisometropia is a less common cause but, as an obstacle to bifoveal fusion, it leads to suppression of the less dominant fovea. Finally, a unilateral macular lesion can lead to a progressive manifest exotropia; small lesions can result in a small scotoma with the attributes of a monofixation syndrome.8
Secondary monofixation exotropia has the same propensity for deterioration as the primary form. There is an abnormal binocular state, and any loss of the “peripheral fusion lock” allows the heterophoria to manifest. If the control deteriorates then the hemiretinal suppression adaptation may take over and increase the likelihood that the exotropia becomes constant.31
Clinical features
Motor features
Most patients with a monofixation syndrome show a heterotropia of 2 to 8 PD under binocular conditions. Up to one-third of cases will show no shift on cover test: most commonly in the form secondary to anisometropia.8,22
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree