Chapter76 Special esotropias (acute comitant, sensory deprivation, myopia associated and microtropia)
Acute comitant esotropia
In a child presenting with sudden onset comitant esotropia a reason needs to be sought for loss of fusion at an age when binocular function is usually stable. This is commonly a benign condition, but children with intracranial pathology, particularly posterior fossa tumors, can present in this way.1,2
Children with acute onset comitant esotropia can be divided into three groups:3
1. Acute onset esotropia following artificial interruption of fusion. This can occur with patching for anisometropic amblyopia, but has also been described following patching for a corneal abrasion. Loss of fusion may be associated with uncorrected hypermetropia. It can also occur following visual loss in one eye (see below, Sensory esotropia).
2. Comitant esotropia of the “Franceschetti” type. This is an acute onset comitant esotropia with diplopia and good potential binocular co-operation. It may be intermittent at first. The accommodative element is usually minimal. In most patients no immediate cause can be found: in some an illness or shock may precede the onset.3
3. Comitant esotropia of the “Bielschowsky” type. These patients have up to 5 diopters (D) of myopia. There is uncrossed diplopia for distance, with fusion for near. The mechanism of the causal relationship between the myopia and esotropia is debated.
The decision on neuroimaging depends on the features of each case.4 The risk of underlying pathology must be balanced against the risks associated with the X-ray dose for a CT scan and a general anesthetic for CT or MRI imaging if required.
Features suggesting neurological disease include age of onset after the age of 5 years and distance diplopia prior to the onset of the esotropia. Diplopia at presentation indicates the absence of pre-existing suppression and an esotropia of recent onset and so higher risk. Suspicious features of the examination include a distance angle larger than the near angle, an increase in esotropia in lateral gaze, lateral rectus underaction, and nystagmus. Lack of fusion on testing with prisms or the synoptophore is more common where there is a brain lesion. An “A” esotropia may be associated with hydrocephalus secondary to an Arnold-Chiari malformation, a tumor, or aqueduct obstruction. Papilledema or optic nerve dysfunction as shown by reduced acuity or color vision or abnormalities of pupil responses mandate imaging.4 Visual fields and clinical electrophysiological testing may provide valuable information.
Initial treatment consists of full correction of any refractive error and treatment of amblyopia. If re-alignment is not achieved with refractive correction alone, then early surgery is indicated to realign the eyes before the potential for fusion is lost. As an alternative treatment botulinum toxin may result in the long-term re-establishment of high-grade stereoscopic function.5
Early re-alignment carries a good prognosis for re-establishing fusion. The failure to re-establish fusion may be an indicator of an underlying neurological problem.1 However, fusion following strabismus surgery has been reported in patients with a tumor.2 Patients with treated intracranial tumors and incomitant strabismus have a better chance of re-establishing fusion.6 In the absence of involvement of brainstem fusion centers, the duration of misalignment is a major prognostic factor for the re-establishment of binocular function. However, the timeframe for loss of fusion potential varies from child to child. Some older children have regained fusion after several years; in some younger children fusion potential is lost in a few months. Early surgery or botulinum toxin to re-establish alignment is likely to be beneficial even in children with (treated) intracranial tumors.
Sensory deprivation esotropia
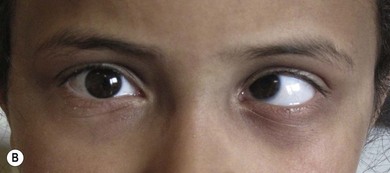
The visual cortex fuses the images from the two eyes into a single image. If the image from one eye is severely degraded or lost, fusion cannot occur. In adults, divergence is common,7 but in children an eye with poor vision and absent binocular function will commonly become convergent, perhaps because they are hyperopic. Sensory esotropia may occur with early onset conditions (monocular congenital cataract or optic nerve anomalies; Fig. 76.1), or with later acquired visual loss (trauma; Fig. 76.2). Correction of hypermetropia in the fixing eye has a variable effect on reducing the deviation and should be undertaken before surgery is considered.