Purpose
To evaluate the prevalence of intermediate-stage age-related macular degeneration (AMD) in patients with acquired immunodeficiency syndrome (AIDS).
Design
Cross-sectional study of patients with AIDS enrolled in the Longitudinal Study of the Ocular Complications of AIDS.
Methods
Intermediate-stage AMD was determined from enrollment retinal photographs by graders at a centralized Reading Center, using the Age-Related Eye Disease Study grading system. Graders were masked as to clinical data.
Results
Of 1825 participants with AIDS and no ocular opportunistic infections, 9.9% had intermediate-stage AMD. Risk factors included age, with an odds ratio (OR) of 1.9 (95% confidence interval [CI] 1.6, 2.3, P < .001) for every decade of age; the prevalence of AMD ranged from 4.0% for participants 30–39 years old to 24.3% for participants ≥60 years old. Other risk factors included the human immunodeficiency virus (HIV) risk groups of injection drug use (OR = 2.4, 95% CI 1.5, 3.9, P < .001) or heterosexual contact (OR = 1.9, 95% CI 1.3, 2.8, P = .001). Compared with the HIV-uninfected population in the Beaver Dam Offspring Study, there was an approximate 4-fold increased age-adjusted prevalence of intermediate-stage AMD.
Conclusions
Patients with AIDS have an increased age-adjusted prevalence of intermediate-stage AMD compared with that found in a non-HIV-infected cohort evaluated with similar methods. This increased prevalence is consistent with the increased prevalence of other age-related diseases in antiretroviral-treated, immune-restored, HIV-infected persons when compared to non-HIV-infected persons.
Age-related macular degeneration (AMD) is the leading cause of late-onset visual impairment and blindness in persons over 65 years of age. Age-related macular degeneration is staged as early, intermediate, or late. Small drusen are the hallmark of early-stage AMD; intermediate-stage AMD consists of extensive medium-size drusen or any large drusen, with or without pigment changes. Late-stage AMD is defined by either choroidal neovascularization or geographic atrophy. In the United States, it is estimated that ∼1.2 million persons have neovascular AMD; 970 000 have geographic atrophy; and 8 million have intermediate-stage AMD.
Antiretroviral-treated, immune-restored, human immunodeficiency virus (HIV)-infected persons have a marked reduction in opportunistic infections and a substantially increased lifespan compared to those from the era before modern combination antiretroviral therapy. However, despite the improved immune function and increased lifespan, antiretroviral therapy does not fully restore health. Compared to similarly-aged, non-HIV-infected peers, antiretroviral-treated, immune-restored, HIV-infected persons have a substantially shortened lifespan, largely owing to an increased risk of non–acquired immunodeficiency syndrome (AIDS) diseases associated with aging. These diseases include cardiovascular disease, non-AIDS cancers, metabolic diseases, and neurocognitive decline, and collectively suggest that antiretroviral-treated, immune-restored HIV infection is associated with an “accelerated/accentuated aging” phenotype. Therefore, we undertook to evaluate whether persons with AIDS had an increased prevalence of AMD, using retinal photographs taken at enrollment in the Longitudinal Study of the Ocular Complications of AIDS (LSOCA) cohort.
Methods
The Longitudinal Study of the Ocular Complications of AIDS was a prospective, observational cohort study of patients with AIDS in the era of modern combination antiretroviral therapy. Enrollment began on September 1, 1998 and was completed on July 31, 2011. Eligible persons had AIDS diagnosed according to the 1993 Centers for Disease Control and Prevention revised criteria for the diagnosis of AIDS. Recruitment occurred at 19 clinical centers throughout the United States, typically located in large urban centers with a large HIV-infected population.
Participants with and without ocular opportunistic infections were recruited. At enrollment all participants gave a detailed medical and HIV-related disease history; relevant findings were confirmed from the medical record. Wide-field retinal photographs were taken on all participants at enrollment, as previously described. Laboratory testing at enrollment included hematology and blood chemistry, lymphocyte subset analysis for CD4+ T cells, the amount of circulating HIV RNA in the blood (HIV load), and the presence of antibodies to hepatitis C.
Approval for the study and its procedures was obtained from the institutional review boards of the individual participating clinical centers and the 3 resource centers (chairman’s office, coordinating center, and reading center). Written informed consent was obtained from all participants. The study was conducted in accordance with the Declaration of Helsinki.
Grading of Retinal Photographs
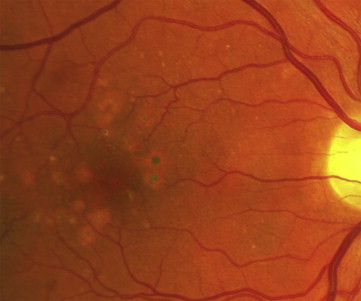
Photographs were graded by graders at the Studies of the Ocular Complications of AIDS (SOCA) Reading Center at the University of Madison, Wisconsin from stereoscopic color photographs of the macula obtained at the baseline visit. Photographers and camera systems were certified for SOCA photographic procedures by Reading Center personnel. Images were graded either from 35 mm film, mounted in typical slide mounts and viewed on a light box with a Donaldson 5X stereoscopic viewer, or from digital images displayed on calibrated computer monitors and viewed with a stereoscopic viewer (PS Manufacturing, Portland, Oregon, USA). The Early Treatment Diabetic Retinopathy Study grid, measuring 7.2 mm on the retina, was placed on film slides using an acetate overlay sized for the camera type and degree of view. Digital image grading employed software tools to calibrate and locate the grid. Approximately 10% of the images were digital. Fundus photographs were graded for the features of intermediate-stage AMD, including the presence, size, and area of drusen and the presence and area of pigmentary abnormalities. Grading questions and procedures employed the Age Related Eye Disease Study (AREDS)-2 system for classifying AMD from retinal photographs. Graders were masked as to clinical information. The primary outcome of interest was intermediate-stage AMD, defined as at least 1 large druse (>150 μm using modern estimates of the average disc size or >125 μm using the traditional estimate) or extensive medium-sized drusen with or without pigment abnormalities ( Figure ). Quality control was provided by a resampling and regrading of 10% of the photographs by the reading center project ophthalmologist (R.P.D.). Because drusen are difficult to evaluate in the face of extensive retinal necrosis and scarring from cytomegalovirus (CMV) retinitis, eyes with ocular opportunistic infections were not graded, and these participants were not included in the study. The primary outcome was intermediate-stage AMD.
Statistical Methods
Continuous variables were categorized into clinically meaningful categories or quartiles. Variables with moderate to large (>10%) amounts of missing data included a category for missing. The association of unadjusted participant characteristics with prevalence of intermediate-stage AMD was assessed using the χ 2 test (or Fisher exact test for small n’s). Adjusted independent effects were assessed with a stepwise model selection procedure using Akaike’s Information Criterion logistic regression. The candidate set included all unadjusted participant characteristics except individual antiretroviral drugs. Odds ratios and confidence intervals were estimated using Wald’s test. All statistical analyses were conducted with SAS/STAT version 9.3 (SAS Institute, Inc, Cary, North Carolina, USA) and Stata version 12.0 (Stata Statistical Software: Release 12, 2011; StataCorp LP, College Station, Texas, USA) software packages.
Comparison With the Beaver Dam Offspring Study
In order to compare the prevalence of intermediate-stage AMD among patients with AIDS to that seen in the non-HIV infected population, the prevalence of intermediate-stage AMD in LSOCA was compared to the published data from the Beaver Dam Eye Study, which also were obtained from grading retinal photographs at the same institution as the SOCA Reading Center and used similar grading protocols. Comparisons were stratified by age and adjusted for age and sex. In addition, because the Beaver Dam Offspring Study was a study of white participants, a comparison also was made with white participants in the LSOCA study.
Results
Characteristics of the Study Population
Of the 2392 participants enrolled in LSOCA, 535 had an intraocular opportunistic infection (primarily CMV retinitis), and 32 did not have enrollment photographs; 1825 had enrollment photographs and no intraocular infections and form the study population. Characteristics of the study population are listed in Table 1 . The group had a mean age of 43.4 years and was 80.7% male. The plurality of participants were white, non-Hispanic (45.4%), but 37.7% were African American, and 13.3% were Hispanic. The largest transmission category for HIV infection was participants with male-to-male sexual contact (54.3%); 14.1% had injection drug use and 26.0% heterosexual transmission as the transmission category for HIV infection. The median nadir CD4+ T cell count prior to enrollment was 44 cells/μL (25th, 75th percentiles, 11 cells/μL, 113 cells/μL), the median enrollment CD4+ T cell count was 198 cells/μL (25th, 75th percentiles, 81 cells/μL, 360 cells/μL). At enrollment 84.9% of participants were receiving combination antiretroviral therapy, and 93.6% had received combination antiretroviral therapy prior to or at enrollment. Comorbidities associated with aging included diabetes in 8.7%, hypertension in 20.9%, and cardiovascular disease in 13.7%.
| Characteristic | Result |
|---|---|
| Number of participants | 1825 |
| Demographics | |
| Age (y) | |
| Mean | 43.4 |
| Standard deviation | 8.8 |
| Sex (%) | |
| Male | 80.7 |
| Female | 19.3 |
| Race (%) | |
| White, non-Hispanic | 45.4 |
| African American | 37.7 |
| Hispanic | 13.3 |
| Other | 3.6 |
| HIV transmission category (%) | |
| Male-to-male sexual contact | 54.3 |
| Injection drug use | 14.1 |
| Heterosexual contact | 26.0 |
| Other | 5.6 |
| Duration of AIDS at enrollment (y) | |
| Median | 4.3 |
| 25th, 75th percentile | 1.6, 7.3 |
| Smoking (%) | |
| Current | 18.0 |
| Former | 28.4 |
| Nonsmoker | 31.3 |
| Missing | 22.3 |
| Immunology and virology | |
| Enrollment CD4+ T cells (cells/μL) | |
| Median | 198 |
| 25th, 75th percentile | 81, 360 |
| Nadir CD4+ T cells (cells/μL) | |
| Median | 44 |
| 25th, 75th percentile | 13, 113 |
| Enrollment HIV load (log 10 [copies/mL]) | |
| Median | 2.7 |
| 25th, 75th percentile | 1.9, 4.6 |
| Maximum prior HIV load (log 10 [copies/mL]) | |
| Median | 5.3 |
| 25th, 75th percentile | 4.7, 5.7 |
| HIV treatment | |
| Highly active antiretroviral therapy at enrollment a (%) | |
| Yes | 84.9 |
| No | 15.1 |
| Highly active antiretroviral therapy prior to or at enrollment (%) | |
| Yes | 93.6 |
| No | 6.4 |
| Comorbidities | |
| Diabetes (%) | |
| No | 91.3 |
| Yes | 8.7 |
| Hyperlipidemia (%) | |
| No | 78.4 |
| Yes | 21.6 |
| Renal impairment (elevated serum creatinine) (%) | |
| No | 93.9 |
| Yes | 6.1 |
| Hypertension (%) | |
| No | 79.1 |
| Yes | 13.7 |
| Cardiovascular disease (%) | |
| No | 86.3 |
| Yes | 13.7 |
| Hepatitis C infection (%) | |
| Seronegative | 66.4 |
| Seropositive | 19.0 |
| Missing | 14.6 |
a Highly active antiretroviral therapy = combination therapy including at least 1 potent antiretroviral drug (eg, a protease inhibitor).
Prevalence of and Risk Factors for Intermediate-Stage Age-Related Macular Degeneration
The prevalence of intermediate-stage AMD in the entire study population was 9.9%. The associations of demographic, immunologic, and virologic comorbidity and antiretroviral treatment risk factors with intermediate-stage AMD in the univariate analysis are listed in Table 2 . Age was a significant risk factor, with prevalences ranging from 4.0% for participants aged 30–39 years to 24.3% for participants 60 years of age and over ( P < .0001). Smoking was associated with intermediate-stage AMD, with current smokers having a higher prevalence (13.7%) than former smokers (9.1%) and “never-smokers” (8.2%) ( P = .02). Participants whose risk for HIV infection was either injection drug use (14.4%) or heterosexual contact (12.0%) had a greater prevalence of AMD than did men who had sex with men (7.7%) or other risk groups (5.6%) ( P = .003). Diabetes (14.4% vs 9.4%, P = .04), hypertension (13.9% vs 8.8%, P = .003), and cardiovascular disease (14.0% vs 8.9%, P = .02) all were associated with intermediate-stage AMD.
| Characteristic | Number | % With AMD a | P Value |
|---|---|---|---|
| Overall | 1825 | 9.9 | |
| Age (y) | <.0001 | ||
| <30 | 98 | 8.2 | |
| 30–39 | 499 | 4.0 | |
| 40–49 | 794 | 9.3 | |
| 50–59 | 364 | 16.8 | |
| ≥60 | 70 | 24.3 | |
| Sex | .30 | ||
| Male | 1472 | 9.5 | |
| Female | 353 | 11.3 | |
| Race & ethnicity | .15 | ||
| White, non-Hispanic | 828 | 8.2 | |
| African American | 688 | 11.6 | |
| Hispanic | 243 | 9.9 | |
| Other | 66 | 12.1 | |
| Smoking history | .02 | ||
| Current | 329 | 13.7 | |
| Former | 518 | 9.1 | |
| Never | 571 | 8.2 | |
| Enrollment cohort (year of enrollment) | .36 | ||
| 1998–2000 | 663 | 8.8 | |
| 2001–2004 | 721 | 10.0 | |
| 2005–2012 | 441 | 11.3 | |
| Time since AIDS diagnosis (y) | .37 | ||
| Quartile 1 (<1.55) | 445 | 10.1 | |
| Quartile 2 (1.55–4.33) | 457 | 7.9 | |
| Quartile 3 (4.34–7.25) | 448 | 10.0 | |
| Quartile 4 (>7.25) | 450 | 11.3 | |
| HIV transmission category | .003 | ||
| Male-to-male sexual contact | 991 | 7.7 | |
| Injection drug use | 257 | 14.4 | |
| Heterosexual contact | 474 | 12.0 | |
| Other | 103 | 5.6 | |
| Enrollment CD4+ T cells (cells/μL) | .98 | ||
| <100 | 519 | 10.2 | |
| 100–199 | 389 | 10.3 | |
| 200–499 | 664 | 9.6 | |
| ≥500 | 238 | 9.7 | |
| Nadir CD4+ T cells (cells/μL) | .25 | ||
| <50 | 953 | 9.0 | |
| ≥50 | 845 | 10.7 | |
| Enrollment HIV load (log 10 [copies/mL]) | .26 | ||
| <2.6 | 627 | 8.3 | |
| 2.6–3.0 | 305 | 10.8 | |
| ≥3.0 | 786 | 10.7 | |
| Maximum prior HIV load (log 10 [copies/mL]) | .98 | ||
| <2.6 | 47 | 10.6 | |
| 2.6–3.0 | 49 | 10.2 | |
| ≥3.0 | 1645 | 9.8 | |
| HIV treatment | |||
| Highly active antiretroviral therapy b | .21 | ||
| No | 276 | 12.0 | |
| Yes | 1548 | 9.5 | |
| Nucleoside transcriptase inhibitor | .27 | ||
| No | 208 | 12.0 | |
| Yes | 1616 | 9.6 | |
| Non-nucleoside transcriptase inhibitor | .24 | ||
| No | 1117 | 9.2 | |
| Yes | 707 | 10.9 | |
| Protease inhibitor | .09 | ||
| No | 703 | 11.4 | |
| Yes | 1121 | 8.9 | |
| Integrase inhibitor | .70 | ||
| No | 1781 | 9.8 | |
| Yes | 43 | 11.6 | |
| Chemokine receptor 5 antagonist | .42 | ||
| No | 1818 | 9.9 | |
| Yes | 6 | 0 | |
| Fusion inhibitor | .48 | ||
| No | 1795 | 9.8 | |
| Yes | 29 | 13.8 | |
| Comorbidities | |||
| Diabetes | .04 | ||
| No | 1666 | 9.4 | |
| Yes | 159 | 14.4 | |
| Hyperlipidemia | .87 | ||
| No | 1428 | 9.9 | |
| Yes | 393 | 9.7 | |
| Renal impairment (elevated serum creatinine) | .73 | ||
| No | 1714 | 9.8 | |
| Yes | 111 | 10.8 | |
| Hypertension | .003 | ||
| No | 1442 | 8.8 | |
| Yes | 382 | 13.9 | |
| Cardiovascular disease | .02 | ||
| No | 1258 | 8.9 | |
| Yes | 200 | 14.0 | |
| Hepatitis C infection (seropositive) | .65 | ||
| No | 1211 | 9.8 | |
| Yes | 347 | 10.7 |
a Percentage with intermediate-stage AMD reported.
b Highly active antiretroviral therapy = combination therapy including at least 1 potent antiretroviral drug (eg, a protease inhibitor).
Neither combination antiretroviral therapy nor the use of any class of antiretroviral drugs at enrollment was associated with intermediate-stage AMD ( Table 2 ). Details of the relationship of individual antiretroviral drugs to intermediate-stage AMD are listed in the Supplemental Table (available at AJO.com ). The only individual antiretroviral drug statistically associated with intermediate-stage AMD was adefovir (33.3% in those taking it vs 9.7% in those not taking it, P = .01); however, only 15 participants were taking adefovir, and only 5 participants taking it had intermediate-stage AMD, so adefovir use had a minimal impact on the prevalence of AMD in this population. There was no association of the use of antiretroviral therapy prior to enrollment, the use of any class of antiretroviral drugs, or the use of any specific antiretroviral drugs prior to enrollment with the prevalence of intermediate-stage AMD at enrollment (data not shown).
The multiple regression analysis of risk factors for intermediate-stage AMD is listed in Table 3 . Age was strongly associated with intermediate-stage AMD with an odds ratio of 1.9 for every decade of age (95% CI 1.6, 2.3, P < .001). HIV transmission category remained a risk factor with injection drug use (odds ratio 2.4, 95% CI 1.5, 3.9, P = .01) and heterosexual contact (odds ratio 1.9, 95% CI 1.3, 2.8, P = .001) associated with intermediate-stage AMD as compared to participants whose HIV risk factor was male-to-male sexual contact. There was no evidence of effect modification between HIV risk group and sex on the risk of intermediate-stage AMD (interaction P = .18, data not shown).



