Phakomatoses
Alex V. Levin
Thomas W. Wilson
Agnes Wong
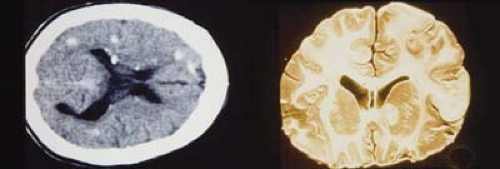
The phakomatoses are a group of diseases that have cutaneous, central nervous system, and ocular manifestations. They often present with dermatologic and ocular manifestations, which subsequently lead to diagnosis of the underlying brain involvement. Significant vision loss can occur due to involvement of either the central nervous system or the eyes, or both.
At least three of the major phakomatoses—neurofibromatosis, tuberous sclerosis, and von Hippel-Lindau—share a common genetic basis: Mutation of a tumor suppressor gene leads to local cellular proliferations in the forms of tumor or skin changes. These three disorders are autosomal dominant in inheritance and demonstrate variable expression, though penetrance approaches 100%. As a result, the detection of affected family members may require extensive investigations, including neuroimaging and abdominal ultrasound. When counseling for autosomal dominant disorders, one must remember that even though each child of an affected parent carries a 50% risk of being affected, the severity of the disease may be very different between the parent and the child. Ataxia telangiectasia is the only autosomal recessive phakomatosis.
Some of the phakomatoses, such as Sturge-Weber syndrome, appear to be sporadic with only very rare reports of familial occurrence. This suggests a somatic (postzygotic) mutation resulting in localized affectation of the field of tissues that are the descendants of the mutated cell. Such disorders would only be heritable if the somatic change also affects the patient’s sperm or eggs. As the manifestations of these disorders are largely confined to the head and neck, gonadal involvement is uncommon.
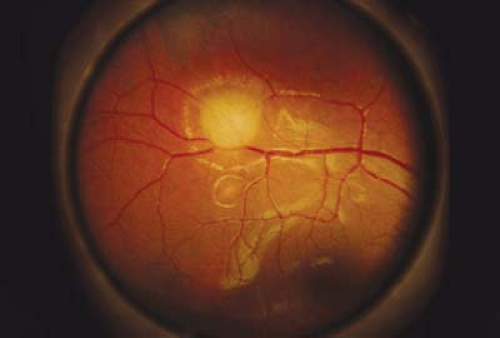
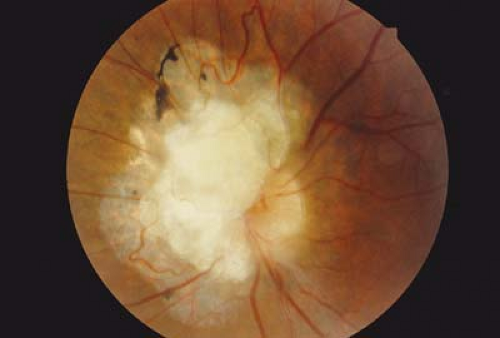
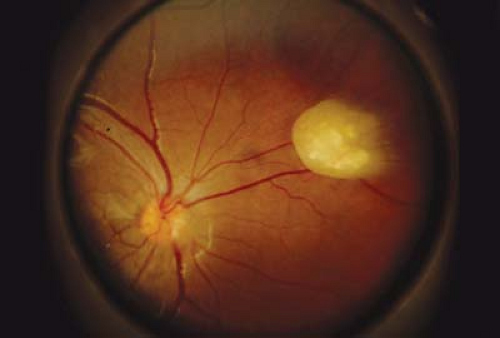 Figure 23.7 Tuberous Sclerosis— Retinal Astrocytic Hamartoma As the lesion matures, it becomes more opaque and eventually calcifies. In all phases, the differential diagnosis must include retinoblastoma (Chapter 8: Retina and Vitreous, Figs. 8.42, 8.43, 8.44, 8.45, 8.46, 8.47, 8.48, 8.49, 8.50, 8.51, 8.52 and 8.53). It can be differentiated from retinoblastoma based on its smooth surface, the absence of associated vascular abnormalities, exophytic growth, or vitreous seeding; and the presence of other systemic manifestations. Eyes have unfortunately been enucleated due to an incorrect suspicion of retinoblastoma. |
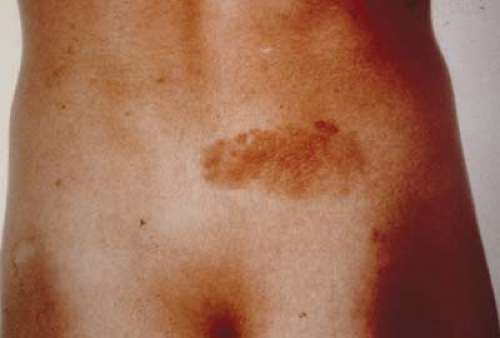
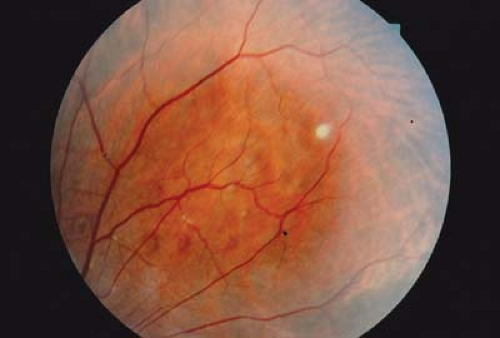 Figure 23.9 Tuberous Sclerosis—Retinal Pigmentary Lesion Areas of depigmentation may occur in the retinal periphery or midperiphery. The discrete lesion represents an area of decreased melanosome size and decreased melanin concentration similar to ash leaf spots (Fig. 23.4) of the skin. The lesion involves the retinal pigmented epithelium. It is benign, may be multiple, usually does not have an ash leaf mulberry appearance, and does not involve the overlying sensory retina. These lesions are visually insignificant. They are not diagnostic of tuberous sclerosis, as small hypopigmented lesions can be due to a variety of causes and may even be seen in normal children. |
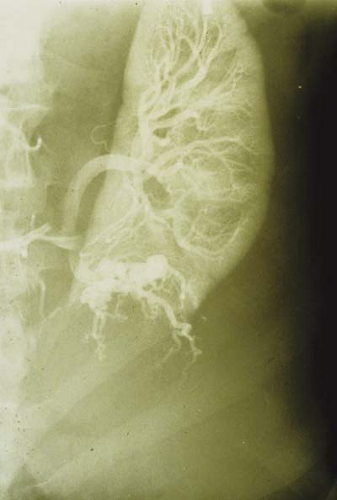 Figure 23.10 Tuberous Sclerosis—Renal Cyst
Stay updated, free articles. Join our Telegram channel
Full access? Get Clinical Tree
 Get Clinical Tree app for offline access
Get Clinical Tree app for offline access

|