years to accomplish a full taper in some children. Although there are certainly risks of steroid-induced cataract or glaucoma, the risk of these complications from inadequately treated uveitis is even greater. Our experience with high dose and chronic topical steroid use actually shows a reduction in such complications and better vision outcomes (15).
Table 13.1 EVALUATION AND TESTING FOR PEDIATRIC UVEITIS | |||||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
and cataract were both observed at significant rates, and the authors recommend close monitoring of pediatric patients on this medication.
Table 13.2 THE SUN WORKING GROUP CLASSIFICATION OF UVEITIS (10) | |||||||||||||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| |||||||||||||||||||||||||||||||||||||||
considered. Secondary glaucoma may occur more frequently in children than in adults (19,20). In general, oral corticosteroids are reserved for short course (<14 days) as an acute intervention, to test for steroid responsiveness, or perioperatively. Although nonsteroidal anti-inflammatory medications (NSAIDs) may be a useful adjunct in managing the systemic symptoms of JIA, and there has been some suggestion of ocular benefit, they play a minor role in the management of pediatric uveitis (21).
is continued for 7 to 10 days thereafter, along with a topical regimen of frequent prednisolone acetate (q1-2h) and a cycloplegic agent.
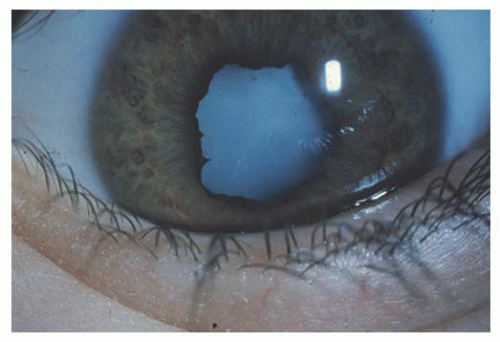
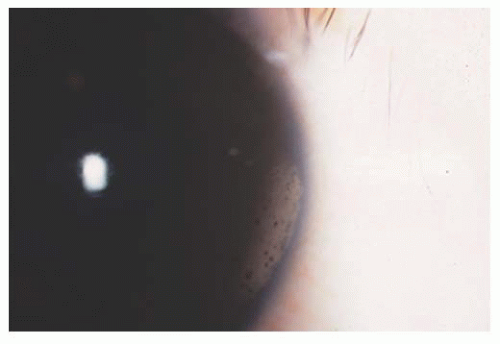 FIGURE 13.2. Typical band keratopathy of chronic pediatric anterior uveitis. Usually starts at medial and temporal limbus and then spreads over interpalpebral cornea. |
screening by ophthalmologists is advised only yearly (49,50). Acquired tenosynovitis of the superior oblique tendon (Brown syndrome) has been described (51).
TABLE 13.3 DIFFERENTIAL DIAGNOSIS OF ANTERIOR UVEITIS IN CHILDREN | |||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree