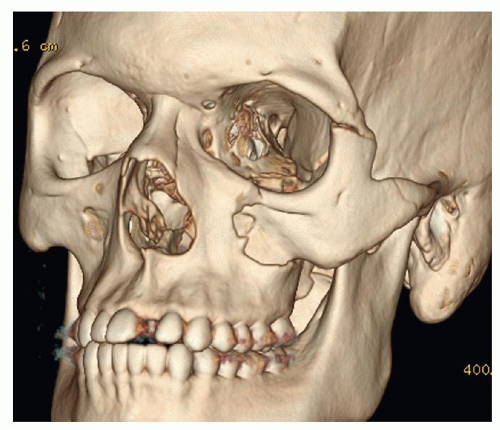
Orbital Fractures
Clinton D. Humphrey
David J. Kriet
OVERVIEW
Orbital fractures occur both as isolated injuries and in conjunction with additional maxillofacial fractures or multisystem trauma. Patients with an orbital injury require initial evaluation by the emergency department (ED) physician and in some cases activation of the trauma team following current Advanced Trauma Life Support (ATLS) protocols (see Chapter 74). The identification of orbital fractures during the initial ED workup should lead to a request for facial trauma surgeon consultation. Computed tomography (CT) scanning is standard for confirming or identifying fractures. Fractures of the zygomaticomaxillary complex (ZMC), orbital rim, medial orbital wall, and orbital floor are most commonly encountered. Fractures of the superior orbit occur less frequently and are often associated with frontal sinus fractures and intracranial involvement. Naso-orbital-ethmoid (NOE) fractures tend to be associated with complex midfacial and maxillary trauma (see Chapter 81). The management of NOE fractures differ from the management of most orbital fractures and is discussed in detail elsewhere. The surgeon’s prompt evaluation of orbital fractures is indicated once life-threatening injuries have been addressed and the patient is stabilized. Ophthalmology consultation is appropriate in selected cases (1). Certain indications and ideal timing for orbital fracture repair remain controversial. Surgical intervention should restore preinjury appearance and function.
ANATOMY
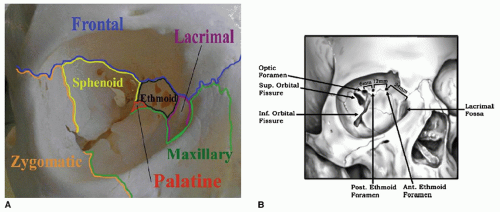
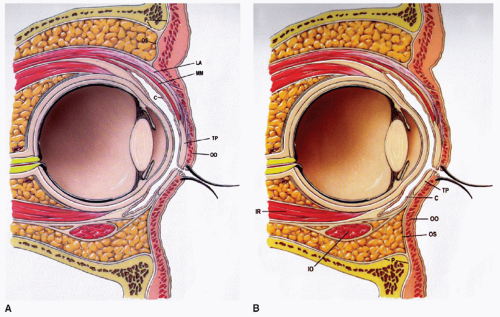
The orbital skeleton contains contributions from the frontal, sphenoid, lacrimal, ethmoid, maxillary, zygomatic, and palatine bones. The supraorbital rims are entirely comprised of the frontal bone. Laterally, the frontal bone articulates with the zygoma. More posteriorly, within the orbit, the zygoma also articulates with the greater wing of the sphenoid. Portions of both the zygoma and maxilla make up the infraorbital rim and, along with a small contribution from the palatine bone, the orbital floor. The medial orbit is a complex confluence of the ethmoid lamina papyracea, lacrimal bone, maxilla, and nasal process of the frontal bone. The bony orbit and locations of the optic foramen, ethmoid artery foramina, and orbital fissures are shown in Figure 82.1A. Moving posteriorly, the anterior ethmoid artery, posterior ethmoid artery, and optic nerve are located approximately 24, 36, and 42 mm, respectively from the anterior lacrimal crest Figure 82.2B. Upper and lower eyelid layers are detailed in Figure 82.2 (2).
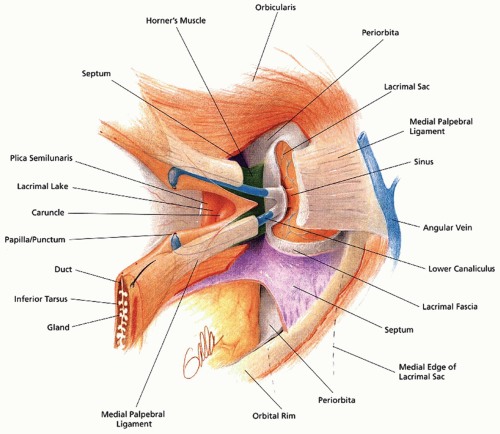
The lateral canthal tendon consists of two limbs. A thin anterior limb blends with the orbicularis oculi muscle fibers and periosteum of the lateral orbital rim; a thicker posterior limb attaches to Whitnall tubercle of the zygoma. The medial canthal tendon attaches via two limbs as well. A thicker limb extends to the anterior lacrimal crest and a thinner limb containing Horner muscle to the posterior lacrimal crest. Intimately related to the medial canthal tendon is the lacrimal system. Upper and lower puncta begin 5 to 7 mm lateral to the canthus and continue as a common canaliculus into the lacrimal sac located between the anterior and posterior limbs of the medial canthal tendon within the lacrimal fossa. The sac empties into the inferior meatus via the nasolacrimal duct. Figure 82.3 demonstrates the complex relationship between the lacrimal drainage apparatus and the medial canthal tendon. The lacrimal gland is located along the superolateral orbit within the upper lid and divided into a larger orbital portion and a smaller palpebral portion by the lateral horn of the levator aponeurosis. Anteriorly, the gland’s orbital portion is in contact with the orbital septum (3, 4).
Extraocular muscles include the two oblique and four rectus muscles. The course of the superior oblique muscle brings it into nearly direct contact with the periorbita of the orbital roof and medial wall at the trochlea. The inferior
oblique is in proximity to the orbit at its origin just posterior to the inferomedial orbital rim, lateral to the superior end of the nasolacrimal canal, and occasionally from the fascia over the lacrimal sac. The superior, inferior, lateral, and medial rectus muscles originate from the annulus of Zinn. All of the extraocular muscles insert directly onto the sclera.
oblique is in proximity to the orbit at its origin just posterior to the inferomedial orbital rim, lateral to the superior end of the nasolacrimal canal, and occasionally from the fascia over the lacrimal sac. The superior, inferior, lateral, and medial rectus muscles originate from the annulus of Zinn. All of the extraocular muscles insert directly onto the sclera.
DEMOGRAPHICS AND ETIOLOGY
Orbital fractures requiring treatment commonly occur secondary to blunt trauma incurred during violent assaults, accidental injury (falls, sports injuries, work-related), or motor vehicle accidents. While these fractures occur at any age, young males are most often affected. The most typical injury patterns among all patients are isolated blow-out fractures of the orbital floor and fractures of the ZMC. ZMC fractures by definition involve the orbital floor and lateral orbital wall (5). Isolated trapdoor type fractures of the floor are more common in the pediatric age group than in adults (6, 7). Orbital roof fractures occur with high-energy injuries that often produce concomitant intracranial sequelae.
Orbital Blow-Out Fractures
The majority of orbital floor blow-out fractures occur medial to the infraorbital nerve and inferior orbital fissure with preservation of a medial strut extending posteriorly off of the nasomaxillary buttress and adjacent to the lacrimal bone (Fig. 82.4). Two wall fractures involving both the orbital floor and the medial wall are less common but must be identified preoperatively as reconstruction is exponentially more challenging, especially if the medial strut is disrupted. In both orbital floor and medial wall fractures, an intact posterior shelf of maxillary or palatine bone will be preserved that must be identified for stable and anatomic implant placement (Fig. 82.5). In medial wall
fractures, there is usually a stable superior shelf of frontal bone above the level of the anterior and posterior ethmoid arteries. These arteries indicate to the surgeon the level of the cribriform plate and skull base.
fractures, there is usually a stable superior shelf of frontal bone above the level of the anterior and posterior ethmoid arteries. These arteries indicate to the surgeon the level of the cribriform plate and skull base.
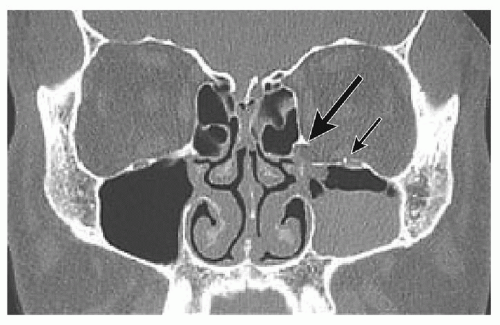 Figure 82.4 A medial strut extending posteriorly from the vertical nasomaxillary buttress is typically preserved following an orbital blow-out fracture. This strut is a useful landmark for orientation and provides a stable anteromedial shelf for implant placement when attempting repair. (From Farwell DG, Sires BS, Kriet JD, et al. Endoscopic repair of orbital fractures: use or misuse of a new approach. Arch Facial Plast Surg 2007;9(6):427-433, with permission). |
Yano et al. presented a simple classification system for blow-out fractures, separating them into “linear,” “punched-out,” and “burst” fractures. Linear fractures were minimally dislocated. Punched-out and burst fractures referred to fractures involving respectively less than half or more than half of the wall (orbital floor or medial) (8). Unfortunately, this classification system and alternatives offered by others generally do not correlate well with the likelihood of developing enophthalmos or persistent diplopia (8, 9). Further, any classification system based on radiologic findings alone is unlikely to reliably predict these sequelae and the need for surgical intervention.
Zygomaticomaxillary Complex Fractures
Classic “tripod,” or tetrapod, fractures of the ZMC involve medial rotation of the zygoma at the arch due to blunt trauma at the lateral aspect of the malar eminence. Significant dislocation results in disruption of the horizontal buttresses at the infraorbital rim and zygomatic arch. The vertical zygomaticomaxillary and zygomaticofrontal buttresses are disrupted as well. Rotation of the body of the zygoma causes displacement along the lateral orbital wall at the zygomaticofrontal and zygomaticosphenoid suture lines (Fig. 82.6). The orbital floor is disrupted by an extension of the orbital rim fracture that runs posteriorly along the zygomaticomaxillary suture line and adjacent to the infraorbital nerve. Infraorbital anesthesia or dysesthesia is present in almost 25% of cases (10).
Zingg proposed a classification system that would stratify ZMC fractures based on concise description of the anatomic sites involved. Type A fractures are isolated to the zygomatic arch, lateral orbital rim, or infraorbital rim alone. Type B fractures are classic monofragment tetrapod fractures as previously described that involve disruption of all four zygomatic articulations. Type C fractures are more complicated tetrapod fractures in which there is comminution of the zygoma. This system does guide treatment somewhat as closed reduction was appropriate for select type A and B ZMC fractures, and open reduction was always indicated for type C fractures in a series of over 1,000 cases (10).
Orbital Roof Fractures
Orbital roof fractures are uncommon with an estimated incidence of 1% to 9% of all facial fractures (11). In adults, they are most commonly produced as a result of a highenergy impact such as a motor vehicle accident. In children, fractures may occur as an extension of a linear frontobasal fracture with falls being the most common etiology. One must maintain a high index of suspicion for intracranial injuries manifesting as pneumocephalus, cerebrospinal fluid (CSF) leaks, or encephalocele formation in patients with orbital roof fractures (12).
Biomechanics and Pathophysiology
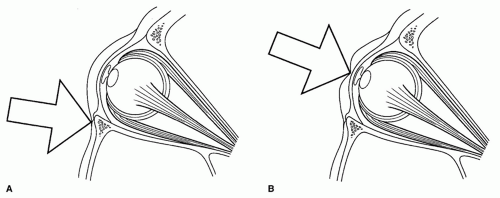
The pathophysiology for most facial fractures is straightforward in that the fracture occurs at the site of impact. For example, ZMC fractures result from impact sustained at the prominent malar eminence. Orbital blow-out fractures occurring in the absence of an infraorbital rim fracture are unique because the fracture-producing force is transmitted indirectly. Two popular, but not mutually exclusive, theories have traditionally been used to explain the mechanism of these blow-out injuries. The first, bone conduction (or buckling) theory, was originally described by Le Fort (13) and maintains that force is transmitted through the thicker bone of the rim into the thinner bone of the floor, resulting in a fracture of the floor but maintaining an intact rim. The bone conduction theory does not as adequately explain how isolated medial wall blow-out fractures might occur. Alternatively, the hydrostatic theory suggests that impact to the globe results in increased intraorbital pressure that fractures the orbital floor and/or medial wall at the weakest points (14). Figure 82.7 illustrates both theories. A third hypothesis—a modification of the hydrostatic theory— proposes that it is displacement of and direct contact of the globe with the orbital floor or medial wall that results in the fracture. A cadaver study by Rhee et al. in 2002 provides strong support for the hydrostatic theory by demonstrating that increased pressure within the orbit in the absence of rim impact results in blow-out fractures. This study also suggested that direct contact of the deformed globe with the orbital floor or medial wall is not required for fracture (15). Despite this evidence bolstering the pure hydrostatic theory, each of these mechanisms could potentially play at least some role in the clinical setting.
EVALUATION
All trauma patients should initially be stabilized and evaluated according to ATLS protocol by an ED physician or the trauma team. Patients with severe orbitofacial trauma, decreased visual acuity, and/or double vision should be evaluated by the facial trauma surgeon acutely and admitted to the hospital if warranted. Conversely, discharge from the ED and follow-up within 3 to 5 days for outpatient evaluation is appropriate for carefully selected patients. Periorbital edema will decrease in the interval, making the examination less difficult and offering an improved assessment of potential enophthalmos. Comprehensive screening CT scans have become increasingly common in complex trauma cases. Identification of orbital fractures on these screening CT scans is often the impetus for consulting the facial trauma surgeon. In the event that fractures are initially discovered on physical exam or noted on plain films or a head CT, a fine cut (less than 2 mm) maxillofacial scan with axial, coronal, and sagittal reconstructions is indicated. Axial images are useful in evaluating medial
wall fractures. Coronal images provide excellent views of the orbital floor, medial wall, and roof. Sagittal images are helpful in assessing the position of the stable posterior shelf. When available, three-dimensional reconstructions are useful for gaining a broad overview of fracture patterns and fragment orientation.
wall fractures. Coronal images provide excellent views of the orbital floor, medial wall, and roof. Sagittal images are helpful in assessing the position of the stable posterior shelf. When available, three-dimensional reconstructions are useful for gaining a broad overview of fracture patterns and fragment orientation.
The availability of a high-quality screening CT scan should not preclude the facial trauma specialist from obtaining a detailed history and performing a thorough physical examination. The historian should inquire about mechanism of impact, previous eye surgery, double vision, numbness, preinjury vision status, and use of anticoagulant medications or other comorbid factors. The physical examination begins with assessing pupillary response and visual acuity. The use of a pocket-sized Snellen chart is helpful for performing an initial vision check. Most smartphones are now able to display such a chart, making the documentation of visual acuity feasible in most circumstances. Color perception is another useful bedside test. Patients with traumatic optic neuropathy may perceive a bright red object (e.g., light shining through the closed eyelid) as a dull brown. While the facial trauma surgeon may not have access to a slit lamp for funduscopic examination, the anterior chamber should be inspected for the presence of hyphema (Fig. 82.8). If available, a Naugle exophthalmometer can easily be used in the clinic to objectively determine the presence and degree of enophthalmos (Fig. 82.9). Extraocular movements (EOMs) are assessed, observing for symmetry and the presence of diplopia during the exam. It is not uncommon to note some diplopia at the extremes of gaze, especially after a fracture causes substantial edema in the affected eye. The status of other cranial nerves, particularly the facial and trigeminal, is determined. Anesthesia or dysesthesia in the distribution of the infraorbital branch of the trigeminal frequently occurs in association with orbital fractures. Likewise, paresis in the buccal branch of the facial nerve can be seen. It is imperative that any neural deficits be documented preoperatively. The combined findings of neurologic injury and an upper eyelid hematoma in a child should raise suspicion for the less common orbital roof fracture (16). The zygomatic arches, zygomaticofrontal sutures, infraorbital rims, and nasal bones are palpated for tenderness or step-offs. The zygomaticomaxillary buttresses are most effectively palpated intraorally. Occlusion and midface stability are also scrutinized.
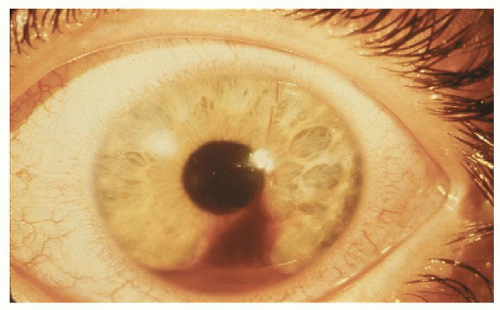 Figure 82.8 Visible hyphema (blood in the anterior chamber of the eye) shown in a patient. Hyphema is most frequently caused by blunt trauma. (Photograph courtesy of Michael P. Grant, MD.) |
 Figure 82.9 A Naugle exophthalmometer can be used to objectively measure enophthalmos. This exophthalmometer is stabilized on the supraorbital and infraorbital rims. |
Indications for ophthalmologic evaluation in patients with orbital fractures remain controversial. Some advocate for an immediate and comprehensive ophthalmologic evaluation of every patient with an orbital fracture. In many institutions, this is difficult to achieve and probably unnecessary. At a minimum, it is advisable that the facial trauma surgeon document EOM, pupillary response, and an objective exam of visual acuity prior to any surgical intervention. A prospective study by Grant (17) has demonstrated that up to 30% of patients with orbital fractures have significant ocular injury that could lead to at least partial loss of vision if undiagnosed. Another study by Mellema et al. on the incidence of ocular injuries in patients with orbital fractures demonstrated that severe ocular injuries are extremely uncommon when patients are visually asymptomatic. Surprisingly, changes in visual acuity alone are a poor predictor of ocular injury. Pain, double vision, flashes of light (photopsias), blind spots (scotomata), and floaters are more sensitive indicators. The presence of any of these symptoms including changes in visual acuity is a clear indication for immediate consultation of an ophthalmologist (1).
INDICATIONS FOR SURGICAL MANAGEMENT
Many orbital fractures require intervention to return the patient to preinjury appearance and functional status. Modern approaches are safe and aesthetically acceptable when performed properly. Selecting the most appropriate surgical approach will optimize exposure and increase
the likelihood of successful treatment. Most orbital fractures do not require urgent intervention and can be repaired within 2 weeks. Resolving soft tissue may uncover enophthalmos and allow transient diplopia to resolve (18). Decreased swelling also facilitates improved surgical exposure. If any ocular injury is suspected, we obtain ophthalmology consultation after complex orbital trauma prior to surgical intervention. Evidence of hyphema, ocular rupture, or other globe injury should delay internal orbital approaches until an ophthalmologist can address the injury (19).
the likelihood of successful treatment. Most orbital fractures do not require urgent intervention and can be repaired within 2 weeks. Resolving soft tissue may uncover enophthalmos and allow transient diplopia to resolve (18). Decreased swelling also facilitates improved surgical exposure. If any ocular injury is suspected, we obtain ophthalmology consultation after complex orbital trauma prior to surgical intervention. Evidence of hyphema, ocular rupture, or other globe injury should delay internal orbital approaches until an ophthalmologist can address the injury (19).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree