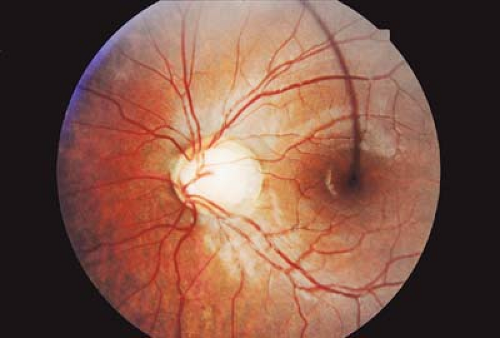
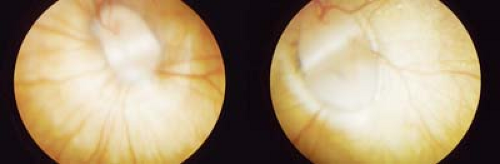
Optic Nerve
Alex V. Levin
Thomas W. Wilson
J. Raymond Buncic
Agnes Wong
Wai-Ching Lam
The optic nerve arises as an outpouching of the anterior neural tube. The optic stalk, formed at the fourth week of gestation, is continuous with the forebrain at one end and the optic vesicle at the other. The optic vesicle, derived from neuroectoderm, forms the neurosensory retina and retinal pigmented epithelium. As early as the sixth week of gestation, ganglion cells in the optic vesicle become the first retinal cells to differentiate and their axons begin to reach the formative occipital cortex by the eighth week. Neural crest cells form the optic nerve sheath. Abnormalities of this process cause congenital anomalies of the optic nerve and optic disc.
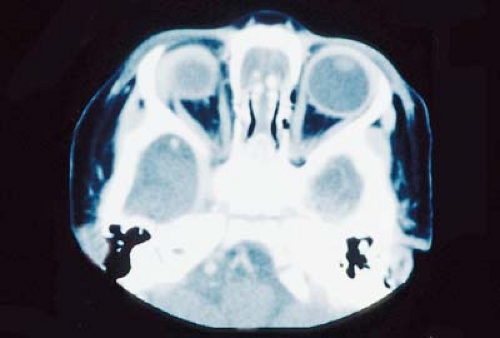
Optic nerve function is often affected by underlying systemic illness or by local processes, including compression, inflammation, or the effects of other intracranial disease. The optic nerve may respond to the many pathologic processes by becoming edematous, hyperemic, or, with time, atrophic. Loss of optic nerve fiber is more readily appreciated in children because of visible changes in the normally thick nerve fiber layer in children. Congenital anomalies of the optic nerve may also be associated with underdevelopment of the macula.
Although sophisticated evaluation such as optical coherence tomography, Doppler ultrasound, and neuroimaging are helpful, any physician can assess the optic nerve using the ophthalmoscope.
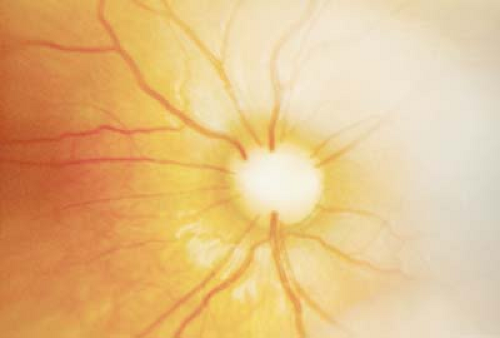
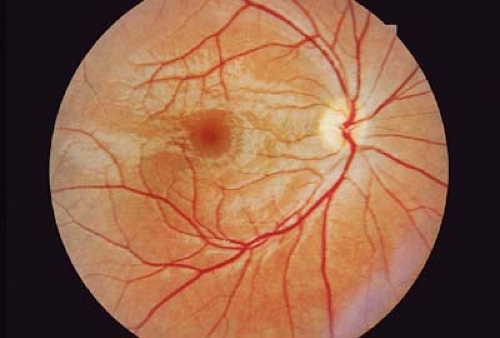 Figure 9.1 Normal Nerve Fiber Layer This photograph demonstrates a normal optic nerve and macula. The nerve fiber layer is thickest in the perifoveal area. The thickness is demonstrated by the relationship of the retinal blood vessels usually buried within the retina and overlying light reflexes. The central reflexes form a doughnut-shaped mound, with a perifoveal inner circular reflex and an outer reflex where the curvature of the macula evens out. Within the fovea, the nerve fiber layer is absent, thus highlighting the healthy surrounding circular macular mound (mound of Buncic) of the thick nerve fiber layer. Flattening of this mound indicates loss of thickness of the retinal nerve fiber layer and decrease in the number of axons into the optic nerve (Figs. 9.15 and 9.21). |
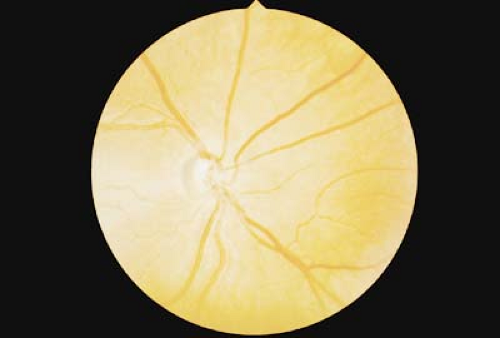
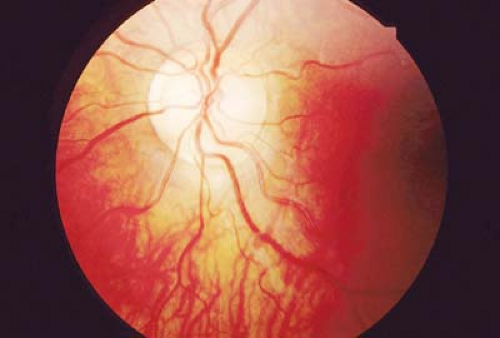 Figure 9.7 Megalopapilla Megalopapilla is a larger than normal optic disc. The cup-to-disc ratio is often increased, although there is no increased risk for pediatric glaucoma. Visual acuity and visual field are usually normal except for an enlarged blind spot. The cause of this disorder is unknown, although familial megalopapilla has been rarely described. It is not associated with coloboma (Fig. 9.4). |
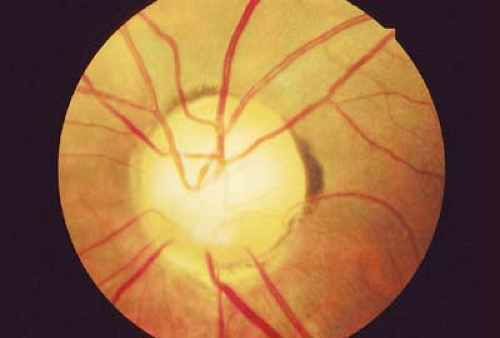
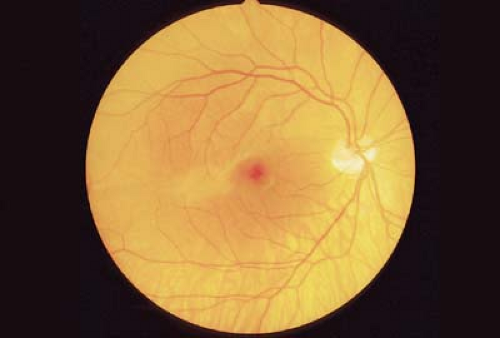 Figure 9.9 Congenital Tilted Disc The tilted disc syndrome is a nonhereditary, usually bilateral disorder of the optic nerve. The optic disc is elevated superotemporally and depressed inferonasally, with an inferior scleral crescent. The disc is oval in shape and its long axis tends to be oriented obliquely. There is usually associated situs inversus (Fig. 9.10) of the retinal vessels. A pseudobitemporal hemianopia may be observed. This is considered to be a refractive scotoma related to regional myopia localized to the inferonasal retina. The hemianopia does not respect the vertical meridian and is reduced or eliminated with the use of minus lenses. |
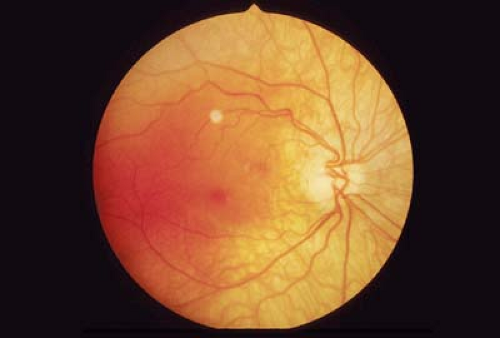 Figure 9.10 Situs Inversus Situs inversus is a variation of the course of the temporal retinal blood vessels. Normally, the temporal retinal blood vessels are directed temporally. In situs inversus, however, the temporal blood vessels course nasally first before turning temporally. Situs inversus is associated with tilted disc syndrome (Fig. 9.9) but can occur in entirely normal eyes. Retinal traction can cause a secondary acquired situs inversus. Primary congenital situs inversus has no visual significance. |
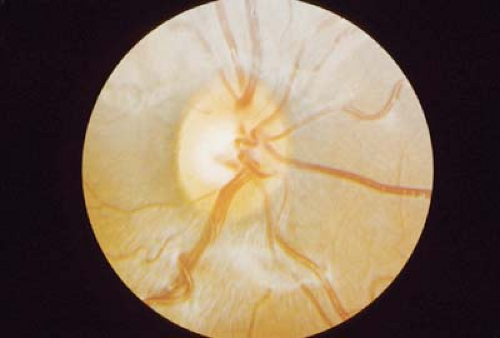 Figure 9.11 Prepapillary Vascular Loops Prepapillary vascular loops are extensions of the normal retinal blood vessels into the vitreous. They often have a spiral configuration but do not extend to the posterior capsule and are therefore differentiated from persistent hyperplastic primary vitreous (Chapter 7: Lens, Figs. 7.14 and 7.15). These loops are remnants of the primitive hyaloid vascular system. The majority of the loops are arterial and can be associated with retinal artery occlusion. Otherwise the loops are entirely benign.
Stay updated, free articles. Join our Telegram channel
Full access? Get Clinical Tree
 Get Clinical Tree app for offline access
Get Clinical Tree app for offline access

|