Chapter 106 Optic atrophy in infancy and childhood
Presentation
In childhood, optic nerve disorders occur in three main periods:
1. Prenatal: the result is usually a developmental disorder such as coloboma or optic nerve hypoplasia but an element of optic atrophy may occur when the cause occurs late in gestation.
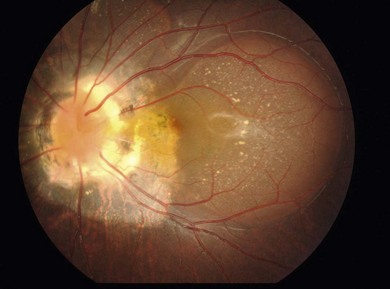
2. Perinatal: the developmental condition merges with optic atrophy1 and some cases have both a developmental optic disk anomaly and optic atrophy, as in Figures 106.1 and 106.2, due to loss of neurons at different times.
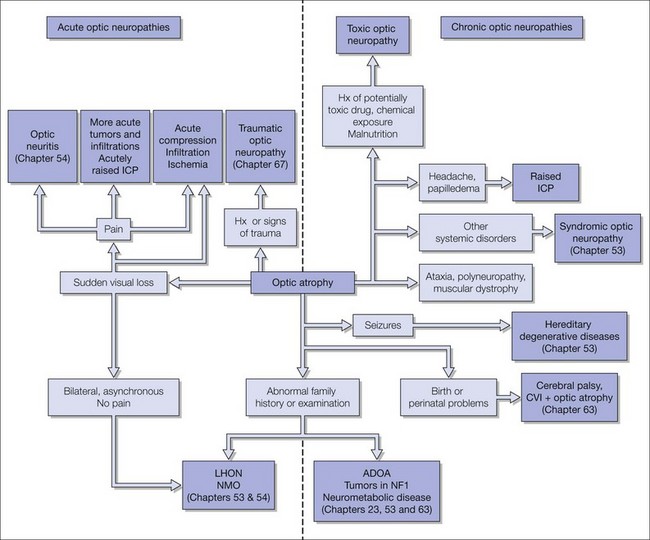
Causes (Fig. 106.3)
It is not possible to establish a cause in every case; the cause varies enormously between centers. A tertiary referral center sees cases referred to their neurology, neurosurgery, or metabolic departments2 while developmental centers see mainly cases associated with cerebral palsy. Prevalence is difficult to establish.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


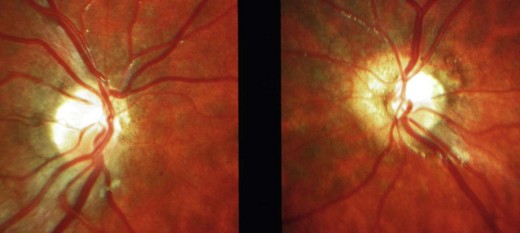
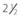 years old when his parents felt his vision became significantly worse. The optic disks are clearly hypoplastic but the temporal segments, which is where any surviving axons would be, are very pale. The inferior parts contain residual nerve fibers which can be best seen about
years old when his parents felt his vision became significantly worse. The optic disks are clearly hypoplastic but the temporal segments, which is where any surviving axons would be, are very pale. The inferior parts contain residual nerve fibers which can be best seen about 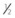 disk diameter away from the optic disk.
disk diameter away from the optic disk.