Effective immune responses to foreign antigens require cells to “traffic” through tissues. Chemokines (chemotactic cytokines) are critical mediators that provide the trafficking signals to immune cells. These are low-molecular-weight proteins, of which more than 50 have been identified to date; they have been classified into subgroups based on their amino acid sequence. Although there is some overlap in the function of these cytokine species, they can also be classified functionally into those that promote neutrophil recruitment (eg, IL-8); T helper-1 (Th1) lymphocyte recruitment and activation (macrophage inflammatory protein-1β [MIP-1β]); monocyte-macrophage recruitment (monocyte chemotactic protein-1 [MCP-1]); and eosinophil recruitment (eotaxin).
Many chemokines have been identified as playing important roles in corneal inflammation. A brief tabulation of some important soluble mediators involved in immune and inflammatory responses of the cornea and ocular surface appears in Table 6-1.
Immunoregulation of the Ocular Surface
Immunoregulation of the ocular surface occurs through tolerance and regulation of the innate and adaptive arms of the ocular immune response. The normal, uninflamed conjunctiva contains polymorphonuclear leukocytes (neutrophils); lymphocytes (including regulatory T cells [Treg cells], which dampen the immune response); macrophages; plasma cells; and mast cells. In addition, the conjunctival stroma has an endowment of dendritic antigen-presenting cells (APCs). The epithelium contains a special subpopulation of dendritic APCs known as Langerhans cells, which are capable of both antigen uptake and priming (sensitizing) of naive (antigen-inexperienced) T lymphocytes. Hence, these dendritic cells serve as the sentinel cells of the immune system of the ocular surface. In addition to containing immune cells, the conjunctiva has a plentiful supply of blood vessels and lymphatic vessels, which facilitate the trafficking of immune cells and antigens to the draining lymph nodes, where the adaptive immune response is generated. This occurs through the recruitment of Treg cells, which return to the ocular surface to modulate and suppress the local immune response (Fig 6-1).
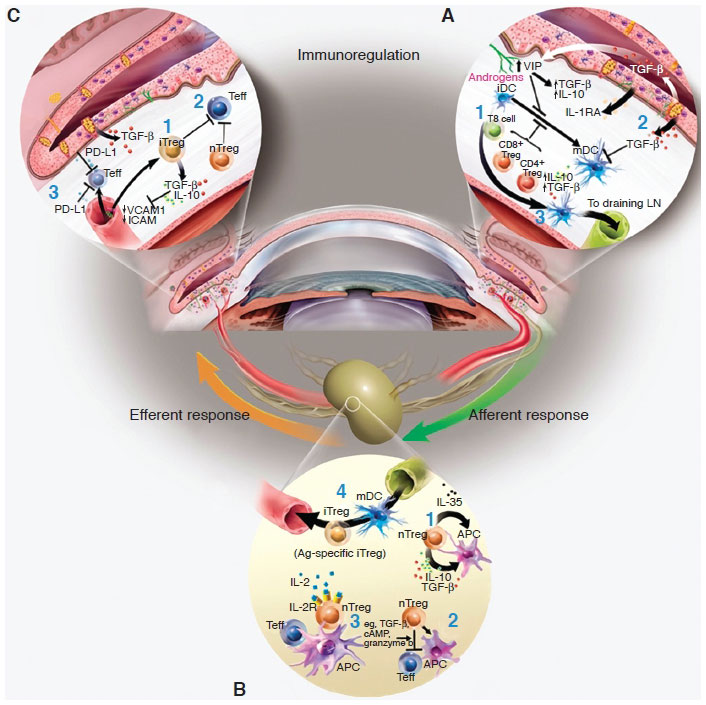
Figure 6-1 A, Immunoregulation of the ocular surface: The ocular surface tissues contain a variety of soluble and cellular factors to reduce inflammation-induced pathology in the lacrimal functional unit. Those implicated in immunoregulation within the ocular surface tissues include the following: (1) Natural regulatory T cells (nTreg cells) (eg, CD4+, CD8+, and natural killer T cells), which include many of the conjunctival intraepithelial lymphocytes, are thought to dampen or inhibit the inflammatory/autoimmune response on the ocular surface. (2) The anti-inflammatory cytokine transforming growth factor β (TGF-β) is present on the ocular surface and has profound suppressive effects on resident dendritic cell (DC) maturation in the cornea; proliferation, differentiation, and survival of autoreactive T cells; and regulatory T cell (Treg cell) differentiation and maintenance. The activity of the potent acute-response, proinflammatory cytokine interleukin-1 (IL-1) is modulated by the IL-1 receptor antagonist (IL-1RA), which is expressed and secreted by corneal and conjunctival epithelial cells. Vasoactive intestinal peptide (VIP) also seems to be protective; VIP secreted by sensory nerve endings in the cornea increases production of TGF-β and IL-10 and inhibits expression of the proinflammatory cytokines and chemokines, IL-1β, tumor necrosis factor α, interferon-γ, and chemokine (C-X-C motif) ligand 2. Hormones are also implicated in curbing inflammation and maintaining homeostasis. In addition, the corneal epithelium expresses vascular endothelial growth factor (VEGF) receptor-1 to sequester VEGF and reduce neovascularization. (3) Antigen-presenting cells (APCs) bearing self-antigen derived at the ocular surface may migrate to the regional lymph nodes to induce antigenspecific Treg cells (iTreg cells). B, Immunoregulation in the lymphoid organs: nTreg cells may exert their immunosuppressive function through (1) release of soluble factors (eg, TGF-β, IL-10); (2) cell–cell contact, which disables pathogenic effector T cells (Teff cells) and/or APCs; and/or (3) competition for soluble factors (eg, IL-2). (4) iTreg cells may use similar mechanisms to inhibit cells bearing or responding to autoantigens. It is possible that these Treg-dependent mechanisms may also function within the ocular surface tissues. C, Other peripheral immunoregulatory mechanisms: additional mechanisms also limit access and effector function of autoreactive T cells within the ocular surface tissues: (1) TGF-β and (2) nTreg and iTreg cells are thought to suppress infiltrating autoreactive lymphocytes, and (3) lowlevel expression of integrins in endothelial cells of the healthy ocular surface, coupled with expression of the programmed death ligand-1 (PD-L1), negatively regulates activated T cells within the ocular surface tissues. (Modified with permission from Stern ME, Schaumburg CS, Dana R, Calonge M, Niederkorn JY, Pflugfelder SC. Autoimmunity at the ocular surface: pathogenesis and regulation. Mucosal Immunol. 2010;3(5):425–442.)
The normal, uninflamed cornea, like the conjunctiva, is endowed with dendritic cells. Like those in the conjunctiva, the dendritic cells in the corneal epithelium are called Langerhans cells. They are located primarily in the corneal periphery and limbus. These APCs are in an activated, mature state (expressing class II major histocompatibility complex [MHC] antigens and costimulatory molecules) and hence are capable of efficiently stimulating T cells. In addition to these dendritic cells (Fig 6-2), small numbers of lymphocytes are present in the peripheral epithelium and anterior stroma of the cornea. A highly regulated process, mediated by vascular endothelial adhesion molecules and cytokines, controls the recruitment of the various leukocyte subsets from the intravascular compartment into the limbal matrix. Immune responses are also mediated by Treg cells in the regional lymph nodes and perhaps at the local level as well.



