Table 80.2 summarizes treatment options for open reduction with internal fixation (ORIF) for mandibular fractures in adult patients according to fracture location. Internal fixation can be classified as being rigid (reconstruction plates, lag screws), semirigid (miniplates), or nonrigid (interosseous wires). Most rigid and semirigid techniques obviate the use of postoperative IMF, and the occlusion may be guided with postoperative dental elastics when required. This is an especially important consideration among patients with epilepsy, diabetes, alcoholism, psychiatric disorders, or severe disability, who may not tolerate IMF. The classic indication for open reduction and rigid internal fixation is inability to reduce or stabilize the fracture with a closed technique. Other indications include associated midface fractures, associated condylar fractures, IMF is either contraindicated or not possible, to preclude the need for IMF for patient comfort, and to facilitate the patient’s return to work or other activities. The fundamental principles of rigid internal fixation include accurate anatomic reduction, stable internal fixation, early mobilization, and careful tissue handling with preservation of the neurovascular supply. The application of appropriately stable fixation varies depending on the location and severity of the fracture. Internal fixation is the application of sufficient hardware to prevent movement across the fracture site during function; however, this is not necessarily rigid internal fixation in many situations. Thus the concept of
load-bearing versus
loadsharing fixation merits review.
Load-bearing fixation is the application of hardware of sufficient rigidity to resist all functional forces until osseous union is achieved. When treating comminuted mandibular fractures, atrophic mandibular fractures, and those with segmental defects, load-bearing fixation is generally required. In contrast,
load-sharing fixation refers to the application of hardware that allows the functional load to be shared between the hardware and the apposed mandibular cortices after fracture reduction is achieved along the fracture site. The majority of mandibular fractures are adequately treated with load-sharing fixation.
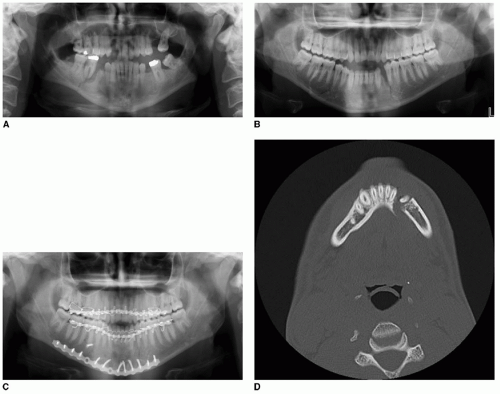
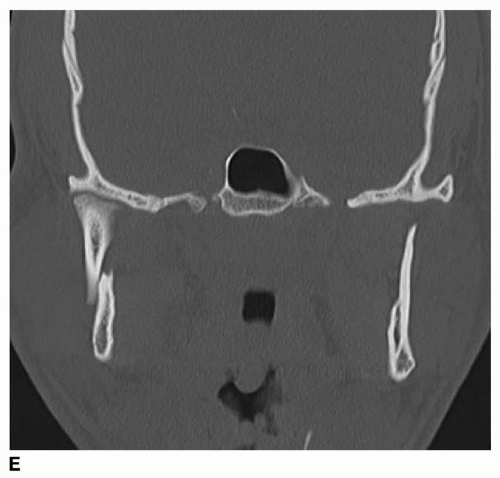
Comminuted fractures are defined as a fracture pattern in which a single anatomic region is broken into pieces. Comminuted fractures of the mandible have been treated in a variety of fashions, including closed reduction, external pin fixation, internal wire fixation, and ORIF with titanium plating systems (
8,
9,
10). Most nonunions in these fractures result from inadequate immobilization of comminuted fragments. Investigations have revealed that periosteal stripping during ORIF does not lead to increased infections as long as fragments are properly stabilized (
9,
10). Comminuted mandibular fractures treated with formal ORIF using reconstruction plates exhibit lower complication rates and decreased recovery time when compared to external pin fixation and closed reduction techniques (
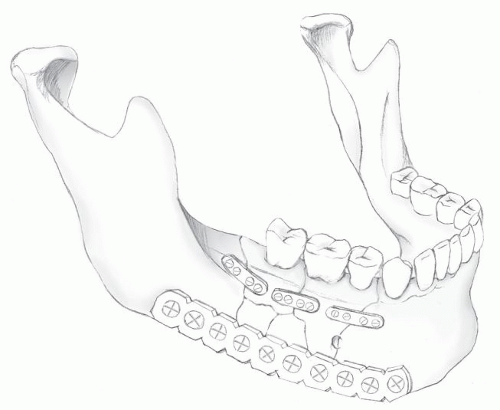
Fig. 80.8) (
9,
10).
In terms of soft tissue approaches, similar complication rates have been observed when comparing transoral versus extraoral reduction of mandible fractures (
11). The majority of mandibular fractures may be treated via the transoral approach, which allows direct occlusal visualization during reduction and internal fixation, eliminates facial scarring, and limits the risk of facial nerve injury. In many instances, posterior body, angle, ramus, and condyle fractures can be addressed through combined intraoral and extraoral approaches utilizing trocars to reduce external scars. The main advantage of the extraoral approach is enhanced visualization and access for complex or comminuted fractures. Extensive comminution or fractures in the severely atrophic mandible often require an external approach to appropriately address the fracture.