The dazzling panorama of new diagnostic laboratory techniques allows for the identification and characterization of cells, proteins, and histopathologic specimens and even for ultrastructural analysis of very small samples obtained by paracentesis. Diagnostic paracentesis of the eye (keratocentesis of the anterior chamber fluid) and vitreous biopsy (paracentesis of the vitreous fluid in the posterior segment of the eye) have definite value in the following scenarios:
Immune complexes and antibodies associated with Behçet’s disease may be found. Polymerase chain reaction (PCR) analysis has suggested the presence of DNA from the infection. Tumor cells may be identified when a malignant infiltration of the eye (e.g., large cell lymphoma, leukemia, retinoblastoma, malignant melanoma) masquerades as a uveitis, or by the presence of tumor cell enzymes and antigens (
Table 35.1).
1,2Although keratocentesis had been advocated historically as a treatment for active uveitis, it lost the attention of ophthalmologists until 1919, when Bruckner
3 first examined the aqueous humor for diagnostic purposes. Laboratory techniques were revolutionized in the 20th century in areas such as: (1) evaluating very small aliquots of fluid (0.2 to 0.3 mL of aqueous or vitreous), and (2) identifying specific microbial organisms and the predominance of other cell types, antibodies, and proteins in these fluids (
Figs. 35.1,
35.2,
35.3,
35.4,
35.5,
35.6). These advancements have led to the development of diagnostic paracentesis for sight-threatening ocular inflammations that are difficult to diagnose. Witmer
4 and O’Connor
5 have provided strong evidence that samples of the aqueous humor reflect the antibodyproducing capabilities of the iris and ciliary body, particularly when more specific antibody per unit of gamma globulin can be found on the aqueous humor than in the blood of the same patient.
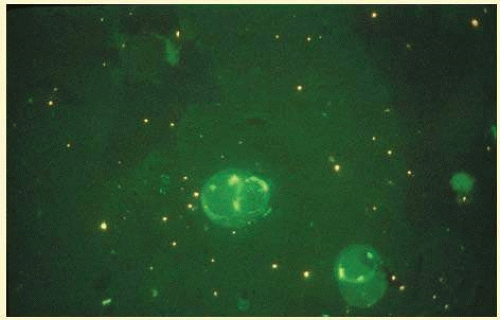
6,7,8 These determinations may be highly significant when one considers the fact that diseased tissue is being bathed in an antibody-containing fluid that is elaborated locally. For instance, in the case shown in
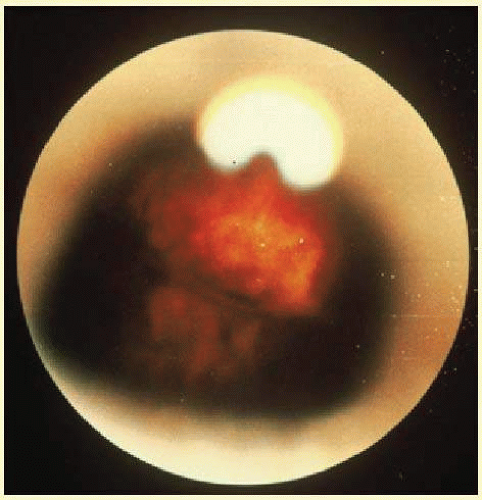
Figure 35.1, the immunofluorescent antibody titer to toxoplasmosis is four times greater in the vitreous aspirate at the time of vitrectomy for repair of retinal detachment than in the plasma. These same considerations have long been recognized in syphilis of the central nervous system, wherein specific antibodies may be present in the cerebrospinal fluid but not in the blood. This is also the case with an unusual presentation of ocular coccidioidomycosis
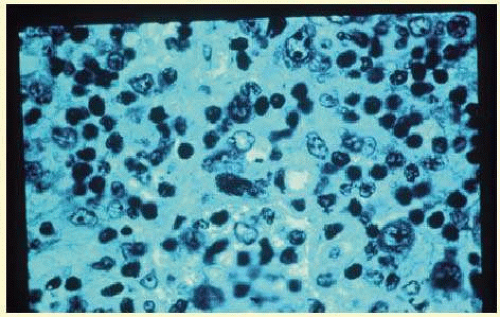
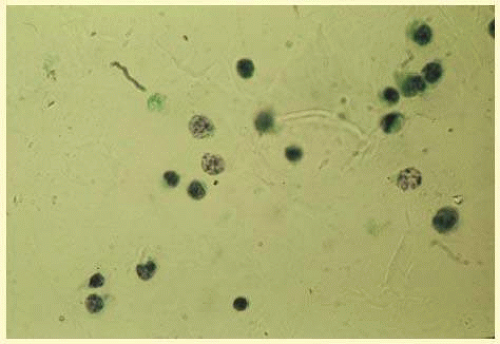
9 or toxocariasis. Many forms of uveitis are characterized by specific types of inflammatory cells. Usually, however, one encounters mixtures of cell types in any given specimen, with the relative percentages of lymphocytes and polymorphonuclear leukocytes varying. There may be unusual number of eosinophils, or macrophages laden with lens material. Thus, an enumeration of the cells and a careful analysis of their structure can be useful as a diagnostic aid (
Figs. 35.7,
35.8,
35.9,
35.10,
35.11,
35.12,
35.13,
35.14,
35.15,
35.16,
35.17,
35.18,
35.19 and
35.20).
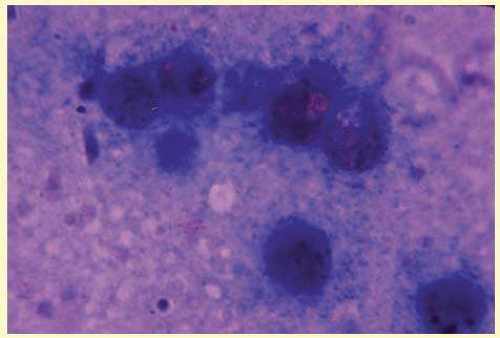
Figure 35.15 demonstrates eosinophils that were aspirated from the anterior chamber of a patient with Toxocara canis endophthalmitis.
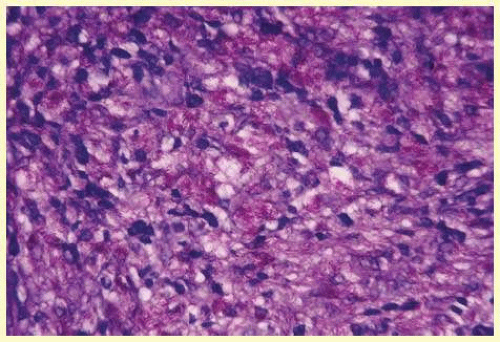
Figure 35.12 demonstrates malignant cell infiltrate from the vitreous, showing the stained presence of monoclonal light chains being elaborated in the cytoplasm. Interleukin-10, detectable in the vitreous of intraocular lymphoma patients, is also directly indicative of both the clinical activity and the number of malignant cells as observed by cytopathology.
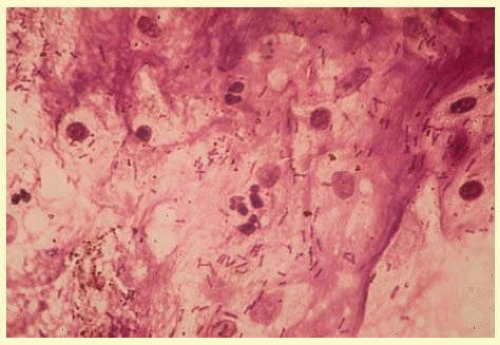
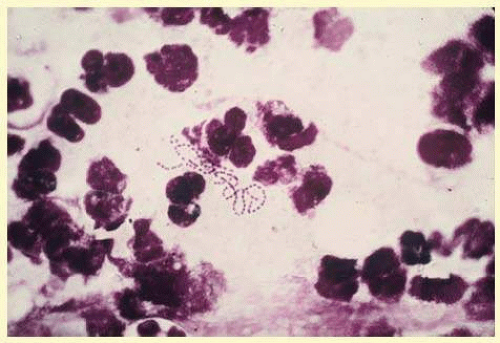
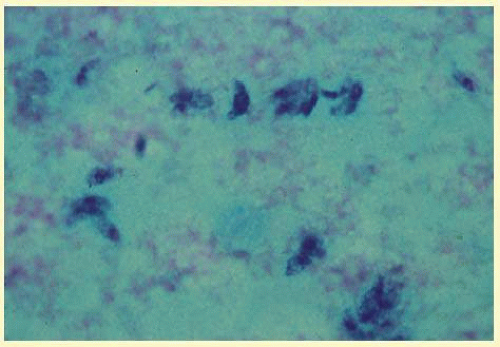
Precise identification and culture of bacterial and fungal pathogens from both the aqueous humor and the vitreous fluid can be obtained. Gram’s stain and Giemsa’s stain smears of centrifuged specimens from the aqueous humor and the vitreous humor frequently demonstrate the bacterial or fungal causative agent. Attempts to isolate bacteria and fungi and to identify them on Gram’s stain or Giemsa’s stain smears have been most rewarding in the following cases: (1) postoperative endophthalmitis, (2) infection after a penetrating injury of the eye, (3) drug abuse patients with endogenous endophthalmitis (
Figs. 35.21,
35.22,
35.23,
35.24 and
35.25), (4) patients receiving hyperalimentation, and (5) patients who are immunocompromised as a result of exogenous immunosuppressive agents.


 Get Clinical Tree app for offline access
Get Clinical Tree app for offline access