Purpose
To report 5 cases of inadvertent posterior capsule staining with trypan blue during phacoemulsification.
Design
Retrospective, observational case series.
Methods
Five cases of posterior capsule staining with trypan blue were identified from cataract surgeries performed at an academic institution. All 5 eyes underwent phacoemulsification with use of iris retractors. The surgical videos from each case were reviewed to better understand the mechanisms and risk factors for posterior capsule staining with trypan blue and techniques to avoid this complication.
Results
No eyes had clinical evidence of zonular pathology during their preoperative examination. Only 1 patient reported a possible childhood history of trauma to both eyes. One eye had uveitis, requiring posterior synechialysis. All 5 cases involved the use of iris retractors. No other intraoperative complications occurred, and the intraocular lens was successfully placed in the capsular bag in all cases. All eyes had resolution of posterior capsule staining by postoperative day 8.
Conclusions
Inadvertent posterior capsule staining with trypan blue can occur in eyes that appear structurally normal. The use of iris retractors may facilitate posterior capsule staining by allowing the posterior flow of trypan blue under the iris and through the zonules to the posterior capsule. Surgeons should consider techniques to minimize the risk of posterior capsule staining, particularly in cases involving the use of iris retractors.
Trypan blue is a vital dye used to stain the anterior lens capsule for better visualization during cataract surgery. Several cases of posterior capsule or vitreous staining with trypan blue during phacoemulsification have been reported in the literature. All of these cases involved eyes with suspected or known zonular weakness, including eyes with a history of trauma, previous surgery, or pseudoexfoliation syndrome. We report a series of 5 eyes with posterior capsule staining associated with the use of iris retractors.
Methods
This observational case series includes eyes of 5 patients who underwent otherwise uncomplicated phacoemulsification surgery ( Table ) at a single academic institution. The Johns Hopkins Hospital Institutional Review Board approved this retrospective review of patient data, and the study was HIPAA compliant. Although 1 of the 5 patients reported a possible history of trauma to both eyes in childhood, no eyes had any evidence of zonular pathology noted on preoperative examination or at any time during surgery. One of the 5 eyes had a history of uveitis and underwent synechialysis prior to cataract extraction. In all 5 cases, iris retractors were used to enlarge the pupil or to stabilize a floppy iris.
| Patient | Demographics | Pertinent History | Outcome | Fellow Eye Surgery |
|---|---|---|---|---|
| 1 | 74-year-old AAF | Chronic narrow-angle glaucoma s/p laser PI OU | Clear capsule by POD 8; final BCVA 20/20 | Trypan; no retractors |
| 2 | 83-year-old WF | Salzmann corneal dystrophy | Clear capsule by POD 8; final BCVA 20/25 | Retractors; no trypan |
| 3 | 78-year-old AAM | Possible childhood trauma OU; terazosin use | Clear capsule by POD 8; final BCVA 20/40 | No trypan; no retractors |
| 4 | 42-year-old AAF | Uveitis; s/p posterior synechialysis | Clear capsule by POD 8; final BCVA 20/25 | Trypan placed under viscoelastic; retractors |
| 5 | 71-year-old WM | Tamsulosin use | Clear capsule by POD 8; final BCVA 20/30 | Trypan placed before retractors |
Trypan blue capsule staining was performed after placement of iris retractors, and the same staining technique was used in all 5 cases. Trypan blue was injected into the anterior chamber under an air bubble and then irrigated with balanced salt solution, followed by a dispersive viscoelastic ( Figure 1 , Top left). The trypan blue was noted to flow under the iris, and in some cases, reflux of trypan was observed prior to hydrodissection ( Figure 1 , Top center, Top right).
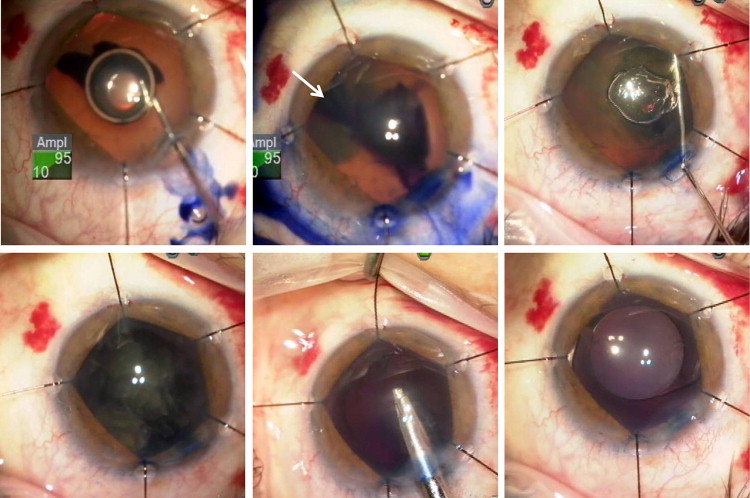
Results
In all 5 cases, the posterior capsule was noted to be stained with trypan blue during nuclear and cortical removal, causing loss of the red reflex and consequent difficulty visualizing the posterior capsule for the remainder of the surgery ( Figure 1 , Bottom left, Bottom center). Despite the poor visualization, none of the eyes had posterior capsular rupture or any other intraoperative complication, and the intended lens implant was successfully placed in the capsular bag ( Figure 1 , Bottom right). The posterior capsule staining persisted on postoperative day 1 but resolved by postoperative day 8 in all cases, with no long-term complications.
Cataract surgery was also performed in the fellow eye in all 5 patients, and none of these surgeries resulted in posterior capsule staining with trypan blue ( Table ). Trypan blue was used in 3 of the 5 fellow-eye cases, 1 of which did not involve the concomitant use of iris retractors. In 1 case involving both trypan blue and retractors, the trypan blue was placed under a dispersive viscoelastic (Patient 4). In the final case (Patient 5), the pupil was sufficiently dilated to use trypan blue before placement of iris retractors to stabilize the floppy iris.
On review of operative records for the 3-year period during which these 5 cases occurred, a total of 491 cataract surgeries were performed, 71 of them involving trypan blue, and 22 of them involving both trypan blue and iris retractors. We therefore observed posterior capsule staining in 7% of all cases involving trypan blue (5/71) and in 23% of cases involving both trypan blue and iris retractors (5/22).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


