Purpose
To examine the in vivo morphologic properties of Salzmann nodular degeneration with ultra-high-resolution optical coherence tomography (OCT).
Design
Interventional case series.
Methods
setting: Single-center academic practice. study population: Nineteen eyes of 12 patients with Salzmann nodular degeneration were recruited to participate in the study. observational procedure: Subjects were imaged using novel, custom-built ultra-high-resolution OCT. Images were used to describe in vivo characteristics of subepithelial nodules. Morphometric measurements were made with custom-built software. Ultra-high-resolution OCT findings were compared with histopathologic findings in 3 patients. main outcome measures: Identifiable in vivo morphologic characteristics of Salzmann nodular degeneration with ultra-high-resolution OCT.
Results
Ultra-high-resolution OCT images demonstrate intraepithelial fibrous nodules with epithelial thinning and corneal surface elevation. The Bowman layer could be differentiated in 9 of 12 patients. The difference between the mean thickness of epithelium above the nodule and the thickness of normal epithelium was statistically significant ( P < .0001). The correlation between thickness of the epithelium and thickness of the nodule was statistically significant (r = −0.48; P < .0001). The correlation between thickness of the nodule and total surface thickness (thickness of the epithelium + thickness of the nodule) was statistically significant (r = 0.98; P < .0001). Ultra-high-resolution OCT findings were consistent with histopathologic results.
Conclusions
Ultra-high-resolution OCT can be used to noninvasively image the cornea in Salzmann nodular degeneration. This new imaging technique helps us to demonstrate different in vivo morphologic characteristics of Salzmann nodular degeneration.
Salzmann nodular degeneration is a noninflammatory, progressive corneal degeneration characterized by elevated, whitish-gray subepithelial nodules. The nodules are developed by fibrous overgrowth and may appear at any part of the cornea. Patients can present with unilateral or bilateral disease and the number of nodules can vary from 1 to many. It is most commonly seen in female subjects and the majority of the cases are reported in elderly patients. Although Salzmann nodular degeneration can be asymptomatic, it can cause severe pain, irritation, irregular astigmatism, and significant decrease in visual acuity.
Salzmann nodular degeneration may be associated with chronic or recurrent keratoconjunctivitis, surgical trauma, or corneal dystrophy. Salzmann nodular degeneration has been associated with Thygeson’s punctate keratitis, vernal keratitis, filamentary keratitis, chronic uveitis, phlyctenular keratitis, and epithelial basement membrane dystrophy. It can also develop after cataract extraction, ptergium excision, laser-assisted in situ keratomileusis, ocular trauma, and hard contact lens wear. In some cases a specific etiologic factor may not be confirmed. Manual removal, phototherapeutic keratectomy, penetrating keratoplasty, lamellar keratoplasty, or anterior keratectomy have been used in the treatment of symptomatic Salzmann nodular degeneration. Recurrence of the nodules can be seen after the surgical treatment of the degeneration.
Optical coherence tomography (OCT) is a signal acquisition technique used to get detailed images from light-scattering tissues. This method is widely used to analyze the structure of anterior and posterior segments of the eye. Ultra-high-resolution OCT is a new technique that allows visualization of the anterior segment structures with an axial resolution of 3 μm. The images with ultra-high-resolution OCT have the quality of a living biopsy, which allows noninvasive in vivo histologic analysis of the morphology of the cornea. This technique has been previously used to analyze the morphologic characteristics and the thickness of Descemet membrane. In this study we evaluated the in vivo morphologic structure of the cornea with ultra-high-resolution OCT in cases with Salzmann nodular degeneration. We described ultra-high-resolution OCT findings, clinical features, and histopathologic results.
Methods
Setting and Design
This interventional case series study took place at a single-center academic practice.
Study Population
Nineteen eyes of 12 patients with Salzmann nodular degeneration were recruited to participate in the study. All patients with Salzmann nodular degeneration who presented to our clinic between January 2, 2009 and June 30, 2010 were asked to participate in the study. Inclusion criteria were a diagnosis of Salzmann nodular degeneration and ability to provide written informed consent. Patients who did not want to give written consent were excluded from the study.
Data Collection
Digital slit-lamp pictures of the cornea were taken in all patients before ultra-high-resolution OCT imaging.
A novel, custom-built spectral-domain ultra-high-resolution OCT was used for the study. A 3-module superluminescent diode light source (Broadlighter, T840-HP; Superlumdiodes, Ltd, Moscow, Russia) was used with a center wavelength of 840 nm and a full width at half maximum bandwidth of 100 nm. The low-coherence light, after passing through a fiber pig-tailed isolator, was coupled into a fiber-based Michelson interferometer with a 2×2, 3-dB fiber coupler. The light was split into the reference arm and the sample arm. The sample light was connected to a light delivery system that has a telecentric design for imaging the anterior segment of the eye. An X–Y galvanometer scanner was used for delivering the sample light and collecting the reflected light from the eye.
In the detection arm, a spectrometer with a collimating lens (f = 50 mm), a 1200-line/mm transmission grating, and an achromatic imaging lens (f = 180 mm) were used. A linear-scan charge-coupled device (CCD) camera (Aviiva-M2-CL-2014, 2048 pixels with 14-μm pixel size operating in 12-bit mode; Atmel, San Jose, California, USA) senses the light and transfers images to the computer. Images were passed through an acquisition board in a computer workstation for signal processing and image display. The A-line (depth scan) rate of the OCT system was set to 24 kHz.
The calibrated axial resolution of the system was ∼4 ìm in the air and ∼3 ìm in the water or tissue with a refractive index of ∼1.39. The ultra-high-resolution OCT radial images were captured at 32 frames per scan. The width of the images varied from 8 to 16 mm according to the extent and the location of the degeneration. The image acquisition was performed relative to the center of the nodule. Custom-built software processed the raw data.
The ultra-high-resolution OCT image with the thickest nodule was selected for each patient and used for thickness measurements. Thickness of the epithelium and thickness of the nodule was measured every 0.1 mm at the entirety of the nodule. Mean thickness of the epithelium, mean thickness of the nodule, minimum thickness of the epithelium overlying the nodule, and maximum thickness of the nodule were calculated from these measurements ( Figure 1 ).
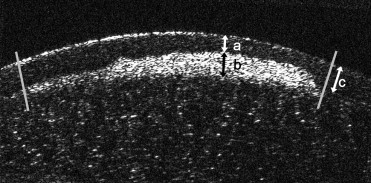
Thickness of the epithelium was measured between the surface of the cornea and superficial margin of the nodule. Thickness of the nodule was measured between the superficial margin of the nodule and the Bowman layer. In cases with indistinct Bowman layer (Patient 1 OU; Patient 2 OU; Patient 6 OS), the thickness of the nodule was measured between superficial and deep margins of the nodule. Total surface thickness was measured as the sum of thickness of the epithelium plus thickness of the nodule. The thickness of the normal epithelium was measured at the edge of the nodule at the nearest point to the center of the cornea ( Figure 1 ).
Three eyes of 3 patients who underwent surgical treatment with superficial keratectomy were examined histologically ( Table 1 ). All procedures were performed with topical anesthesia. The nodules were lifted with a beaver blade and peeled off with a forceps. The dissection plane was prepared in a planar fashion. Bandage soft contact lens was applied for healing and comfort. The specimens were fixed in 10% buffered formalin, dehydrated, and embedded in paraffin. Slides, sectioned at 7 μm, were stained with hematoxylin-eosin, Periodic acid–Schiff, and Gomori’s 1-step trichrome staining and analyzed using a microscope (Olympus Optical Co, Tokyo, Japan).
| No. | Age | Sex | Eye | Ocular History | Ocular Medications | Ocular Surgery | BSCVA | Refraction | ||
|---|---|---|---|---|---|---|---|---|---|---|
| OD | OS | OD | OS | |||||||
| 1 | 68 | F | OU | Dry eye, Fuchs‘ dystrophy, OU cataract | Topical cyclosporine 0.05%, ATD | Conjunctival biopsy | 20/30 | 20/20 | −0.25 +0.50 × 170 | +0.50 × 175 |
| 2 | 13 | M | OU | Ocular rosacea | Loteprednol | 20/20 | 20/20 | Plano | Plano | |
| 3 | 52 | F | OD | 20/20 | 20/15 | −1.00 plano | −0.50 plano | |||
| 4 | 70 | M | OU | EBMD, OS cataract | 20/25 | 20/50 | +4.00 +0.50 × 45 | +0.75 +6.00 × 55 | ||
| 5 | 69 | M | OD | PBK | Fluoromethalone | OD ECCE IOL (1999), OD PK + IOL exchange (1999) | 20/30 | 20/25 | −4.25 +6.00 × 0.75 | −0.75 +1.75 × 5 |
| 6 | 54 | F | OU | Rosacea, CL wear | ATD | OU PTK + superficial keratectomy (2008) a | 20/25 | 20/60 | −6.00 plano | −7.00 +1.00 × 25 |
| 7 | 79 | F | OS | Dry eye, OU cataract | ATD | OU Phaco | 20/20 | 20/20 | −2.00 +1.00 × 147 | −1.00 +1.50 × 45 |
| 8 | 82 | F | OU | OU cataract, OU dermatochalasis, OD CME | Nepafenac, prednisolone acetate | 20/40 | 20/30 | −0.50 +1.25 × 10 | +1.72 +2.00 × 180 | |
| 9 | 43 | M | OU | OU KCN, OD PK (1989) | OS PTK (for CL intolerance) | 20/20 | 20/40 | −7.50 +3.50 × 170 | −6.00 +8.00 × 10 | |
| 10 | 53 | F | OD | Sjögren disease, dry eye | ATD | Conjunctival biopsy (to eliminate CIN) + superficial keratectomy (2009) | 20/20 | 20/20 | −3.50 +1.50 × 180 | −2.25 plano |
| 11 | 82 | M | OD | Dry eye, OD ERM | ATD | OD CE + IOL (1992), OS Phaco + AC IOL (2006) + superficial keratectomy (2010) | 20/80 | 20/40 | +075 +3.50 × 150 | −1.75 +1.50 × 150 |
| 12 | 52 | F | OU | Dry eye | ATD | OD superficial keratectomy (2009) | 20/20 | 20/20 | +0.75 × 180 | +0.50 × 180 |
SPSS software version 15.0 (SPSS, Inc, Chicago, Illlinois, USA) was used for statistical analyses. Results are reported as means ± standard deviation. Differences between thickness measurements were tested for significance by the Mann-Whitney U test. Correlations between thickness measurements were examined with Pearson correlation analysis. P < .05 was considered significant.
Main Outcome Measure
Visualization of the in vivo morphologic characteristics of cases with Salzmann nodular degeneration was achieved with ultra-high-resolution OCT and the results were compared with clinical features and histopathologic results.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


