Glaucoma
Alex V. Levin
J. Raymond Buncic
Elise Héon
Glaucoma may manifest at any time during childhood. Congenital and infantile glaucoma usually involves a primary dysgenesis of the trabecular meshwork system, whereas later onset often implies a secondary malfunction of aqueous outflow. The primary childhood glaucomas, congenital/infantile and juvenile, have a genetic basis, which is currently being elucidated. Other forms of glaucoma associated with congenital malformation of the anterior segment such as the Axenfeld-Rieger spectrum and aniridia, also have a genetic basis. Virtually every anterior segment dysgenesis leaves the patient with a lifelong risk of developing glaucoma.
Some children acquire glaucoma as a result of other events. Aphakic glaucoma is one of the most common causes of pediatric glaucoma. Any child who has cataract surgery is at lifelong risk and must be screened for glaucoma periodically. Some aphakic children may also have a goniodysgenesis, perhaps indicating that there is more to the malformation complex than just the cataract. Other theories for the development of aphakic glaucoma include barotrauma at the time of surgery, communication of the anterior chamber with the vitreous, and genetic predisposition. The average onset time for developing glaucoma is approximately 8 years after cataract surgery. The effect of intraocular lens implantation is not yet clear, but early indicators suggest that this procedure will not reduce the incidence of glaucoma significantly, particularly in the first 2 years of life.
Trauma can also result in glaucoma through direct damage to the aqueous outflow system, inflammation, hyphema, or secondary ghost cell glaucoma. Other causes of secondary glaucoma include infection such as congenital rubella syndrome, uveitis, and the use of steroids. Glaucoma may be an isolated ocular disorder or associated with a wide variety of systemic diseases and syndromes. This chapter focuses on isolated glaucoma. The reader is referred elsewhere in this atlas for discussion of those ocular and systemic disorders that are associated with glaucoma, such as Sturge-Weber syndrome and neurofibromatosis type 1 (Chapter 23: Phakomatoses) and aniridia and Axenfeld-Rieger syndrome (Chapter 6: Iris and Pupils).
The most common cause of visual loss in patients with glaucoma is amblyopia. However, left untreated, the glaucoma itself will result in optic neuropathy with visual field and acuity loss. Early identification, aggressive treatment, and careful periodic follow-up are the cornerstones of a successful outcome.
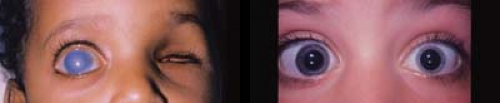 Figure 10.1 Primary Congenital Glaucoma—Buphthalmos Elevated intraocular pressure in the eye of a child less than 2 to 3 years old results in stretching of the pliant sclera and cornea such that the corneal size and axial length increase. Rarely, this can also occur later, in the first 5 to 7 years of life. Buphthalmos will also be reflected in an increasingly myopic refraction. In microphthalmic eyes, the corneal diameter and axial length may be increasing pathologically, even though the absolute values are below the age-matched normative data. Likewise, excessive loss of hyperopia (e.g., in an aphakic eye) can also be a sign of excessive ocular growth due to glaucoma. In the left image, the child’s left eye was enucleated (photograph provided by John Ainsworth, Hospital for Sick Children fellow, 1994). In the right image, the child has left microphthalmia with a buphthalmic right eye that was also previously microphthalmic.
Stay updated, free articles. Join our Telegram channel
Full access? Get Clinical Tree
 Get Clinical Tree app for offline access
Get Clinical Tree app for offline access

|