Hematology
Alex V. Levin
Thomas W. Wilson
David Smith
Abnormalities in the hematologic system will often have associated ocular diseases or findings. All four major components of the blood (serum, red blood cells, white blood cells, and coagulation factors) have been implicated as the underlying cause of vision loss and eye disease. The maintenance of ocular health depends upon the hematologic system.
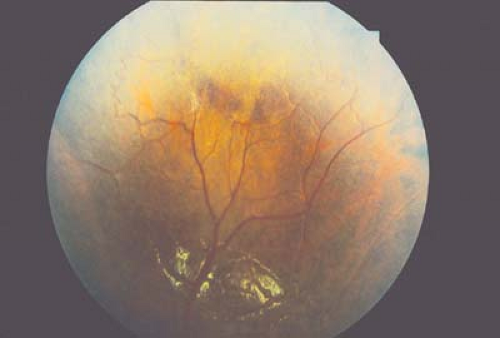
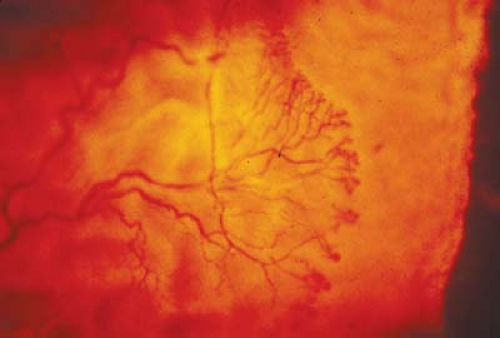
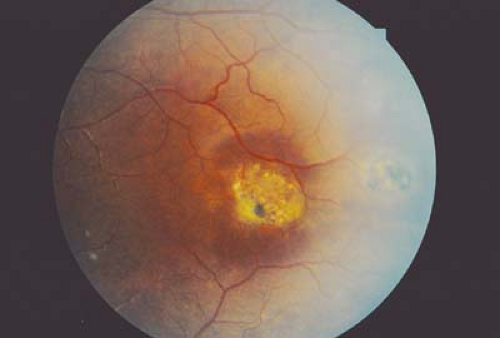
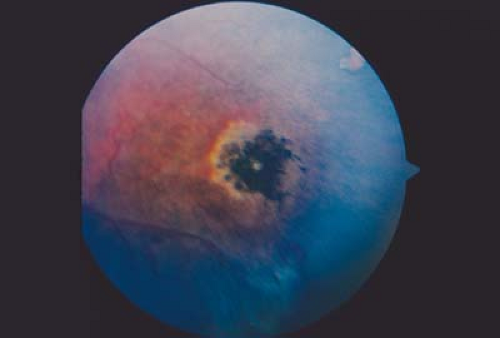
Anemia and abnormalities of red blood cell function and morphology will lead to mild to severe ischemia within the eye. Mild ischemia will be manifested as cotton wool spots (ischemia of the nerve fiber layer), microaneurysms, and scattered hemorrhages throughout the retina. Severe ischemia will lead to neovascular proliferation and the potential for significant vision loss from extensive hemorrhage or tractional retinal detachment.
Proliferation of the white blood cells in lymphoma and leukemia will have direct (invasion in ocular tissues) and indirect (increased risk of infection due to immunosuppression) effects on the visual system. White blood cell abnormalities have been reported in the ataxia telangiectasia (telangiectatic conjunctival vessels, progressive ataxia, decreased IgA, and decreased T-cell–mediated immunity) and Chediak-Higashi (albinism and defective chemotaxis and degranulation of neutrophils) syndromes.
Abnormalities of coagulation will often have associated conjunctival and retinal hemorrhages. The retinal hemorrhages of coagulopathies are typically few in number and located in the posterior pole. Disorders of blood serum including hyperviscosity can cause retinal venous disease.
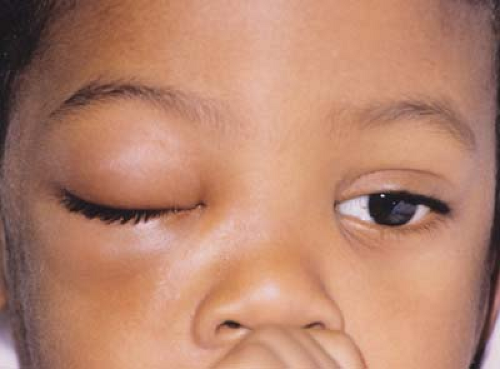 Figure 18.5 Sickle Cell Disease— Orbital Bone Infarction
Stay updated, free articles. Join our Telegram channel
Full access? Get Clinical Tree
 Get Clinical Tree app for offline access
Get Clinical Tree app for offline access

|