Eyelid
6.1 PTOSIS
Symptoms
Drooping upper eyelid, visual loss often worse with reading and at night.
Signs
(See Figure 6.1.1.)
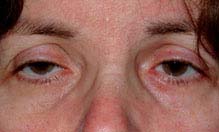
FIGURE 6.1.1. Ptosis.
Critical. Drooping upper eyelid.
Other. Concerning associated signs include anisocoria, diplopia, ocular motility defecits, headache, or neck pain. See individual entities.
Etiology
NOTE: Although the vast majority of ptosis is of benign etiology, five entities must be ruled out in every single case by careful examination.
1. Horner syndrome.
2. Third cranial nerve (CN) palsy (complete, partial, or aberrant CN III regeneration).
3. Myasthenia gravis.
4. Superior eyelid or orbital malignancy.
5. Chronic progressive external ophthalmoplegia (CPEO) (particularly Kearns–Sayre syndrome. See 10.12, Chronic Progressive External Ophthalmoplegia).
 Myogenic: Congenital myogenic ptosis is present at birth with poor levator function and a poor or absent lid crease due to dysgenesis of the levator muscle, fibrosis, and its replacement with adipose tissue. A poor Bell phenomenon, lagophthalmos in downgaze, and upgaze limitation may indicate a double elevator palsy. Acquired myogenic ptosis is uncommon and may be seen with muscular dystrophy and CPEO.
Myogenic: Congenital myogenic ptosis is present at birth with poor levator function and a poor or absent lid crease due to dysgenesis of the levator muscle, fibrosis, and its replacement with adipose tissue. A poor Bell phenomenon, lagophthalmos in downgaze, and upgaze limitation may indicate a double elevator palsy. Acquired myogenic ptosis is uncommon and may be seen with muscular dystrophy and CPEO.
 Aponeurotic: This is characterized by a high or absent eyelid crease, moderate degree of ptosis, good levator function (10 to 15 mm). May worsen in downgaze. Levator stretching or dehiscence can be due to normal aging, repetitive eye rubbing, use of rigid contact lenses, or previous intraocular surgery.
Aponeurotic: This is characterized by a high or absent eyelid crease, moderate degree of ptosis, good levator function (10 to 15 mm). May worsen in downgaze. Levator stretching or dehiscence can be due to normal aging, repetitive eye rubbing, use of rigid contact lenses, or previous intraocular surgery.
 Neurogenic: Third cranial nerve palsy (often complete ptosis, never an isolated abnormality; congenital, compressive, vasculopathic, see 10.5, Isolated Third Nerve Palsy); Horner syndrome (subtle upper and lower eyelid ptosis, see 10.2, Horner Syndrome); myasthenia gravis (variable ptosis, worsens with fatigue, see 10.11, Myasthenia Gravis); Marcus Gunn jaw-winking syndrome (ptotic eyelid elevates with jaw movement); ophthalmoplegic migraine; multiple sclerosis.
Neurogenic: Third cranial nerve palsy (often complete ptosis, never an isolated abnormality; congenital, compressive, vasculopathic, see 10.5, Isolated Third Nerve Palsy); Horner syndrome (subtle upper and lower eyelid ptosis, see 10.2, Horner Syndrome); myasthenia gravis (variable ptosis, worsens with fatigue, see 10.11, Myasthenia Gravis); Marcus Gunn jaw-winking syndrome (ptotic eyelid elevates with jaw movement); ophthalmoplegic migraine; multiple sclerosis.
 Mechanical: Retained contact lens in upper fornix; upper eyelid inflammation (chalazion, giant papillary conjunctivitis, posttraumatic or postsurgical edema) or neoplasm.
Mechanical: Retained contact lens in upper fornix; upper eyelid inflammation (chalazion, giant papillary conjunctivitis, posttraumatic or postsurgical edema) or neoplasm.
 Traumatic: History of eyelid laceration with levator transection, contusion injury to the levator, tethering or ischemia within an orbital roof fracture, late dehiscence or cicatricial changes.
Traumatic: History of eyelid laceration with levator transection, contusion injury to the levator, tethering or ischemia within an orbital roof fracture, late dehiscence or cicatricial changes.
 Pseudoptosis: Contralateral eyelid retraction or proptosis, ipsilateral enophthalmos, hypertropia, microphthalmia, phthisis bulbi, dermatochalasis, brow ptosis, chalazion or other eyelid tumor, eyelid edema, blepharospasm, Duane syndrome.
Pseudoptosis: Contralateral eyelid retraction or proptosis, ipsilateral enophthalmos, hypertropia, microphthalmia, phthisis bulbi, dermatochalasis, brow ptosis, chalazion or other eyelid tumor, eyelid edema, blepharospasm, Duane syndrome.
Work-Up
1. History: Determine the onset and duration of ptosis. Present since birth? Acute onset? Old photographs (e.g., driver’s license) and family members’ opinions are useful adjuncts to the history. History of surgery in either eye? Orbital or eyelid trauma (orbital blow-out fractures resulting in enophthalmos can mimic ptosis)? Variability with fatigue? Associated with headache or neck pain? Any history of autoimmune disease (lupus, Sjogren syndrome) or corneal abnormalities (may predispose the patient to postoperative exposure keratopathy)?
2. Mandatory documentation: Must carefully check and document pupillary size and extraocular motility, even if normal. If anisocoria is present, measurements should be documented under light and dark conditions. Additional pharmacologic testing may be indicated (see 10.1, Anisocoria). If extraocular muscle dysfunction is noted, additional testing with prism bars may be indicated.
3. Complete orbital examination of both eyes: Measure and compare margin–reflex distance, levator function (full upper eyelid excursion while preventing frontalis muscle assistance), upper eyelid crease position of both eyes. Is there lagophthalmos? Associated lower eyelid “ptosis” (elevation of ipsilateral lower eyelid) is often seen in Horner syndrome. Proptosis or eyelid lag may masquerade as contralateral ptosis. Exophthalmometry measurements are useful. Any sign of aberrant eyelid movements like jaw-winking, variability and/or fatigue, orbicularis weakness, eyelid retraction with adduction and/or infraduction? Palpate the superior orbit to rule out a mass or superior orbital rim deformity.
4. Complete ocular examination: Determine if there are associated pupillary or extraocular motility abnormalities. Flip upper eyelid to examine conjunctival surface and superior fornix. Dilated fundus examination to look for pigmentary changes in adolescents and young adults who present with ptosis, poor levator function, and external ophthalmoplegia (possible Kearns–Sayre syndrome).
5. Corneal protective mechanisms. Document the presence or absence of preoperative lagophthalmos, orbicularis function, Bell phenomenon, and tear production. Check the cornea carefully for any abnormalities or dystrophies, which may predispose the patient to postoperative keratopathy.
6. Other tests
—Ice test: Apply ice pack to ptotic eye for 2 minutes and reassess the degree of ptosis. Improvement with ice is highly suggestive of myasthenia gravis.
—Neosynephrine test: Instill one drop of 2.5% phenylephrine in the ptotic eye(s) and reassess the degree of ptosis. Patients with improvement of ptosis after 5 to 7 minutes may be good candidates for ptosis correction by an internal approach.
—Cocaine, apraclonidine, and hydroxyamphetamine tests. See 10.2, Horner Syndrome.
7. Imaging studies: In very select cases where a systemic or neurologic cause is suspected:
—Computed tomography (CT) or magnetic resonance imaging (MRI) of orbit if a superior orbital mass is suspected.
—Emergent CT/computed tomography angiogram (CTA) or MRI/magnetic resonance angiogram (MRA) of the head and neck if carotid artery dissection is suspected in a patient with a painful Horner syndrome. Imaging of the head alone is inadequate. See 10.2, Horner Syndrome.
—Emergent CT/CTA, MRI/MRA, or conventional angiography if intracranial aneurysm causing a third cranial nerve palsy with pupillary involvement or a partial third cranial nerve palsy is suspected. See 10.5, Isolated Third Nerve Palsy.
—Chest CT if myasthenia gravis is suspected to rule out thymoma. See 10.11, Myasthenia Gravis.
8. Ancillary studies:
—Urgent ECG and cardiology consult if Kearns–Sayre syndrome is suspected. These patients can have heart block, resulting in sudden death.
—If myasthenia gravis is suspected, acetylcholine receptor antibody testing, single- fiber electromyography (including the orbicularis muscle), and/or edrophonium chloride testing under monitored conditions may be indicated. See 10.11, Myasthenia Gravis.
—If severe dry eye is found, consider an autoimmune work-up to rule out lupus and Sjogren syndrome.
Treatment
1. Depends on the underlying etiology (see 10.2, Horner Syndrome; 10.5, Isolated Third Nerve Palsy; 10.11, Myasthenia Gravis).
2. Nonsurgical options: Observation. Taping upper lids open and eyelid crutches attached to glasses in neurogenic and myogenic ptosis. Management of chalazion with warm compresses and/or excision, eyelid and/or orbital neoplasms with excision.
3. Surgical options: Transcutaneous levator advancement, transconjunctival levator advancement, frontalis muscle suspension, Müller muscle resection. Surgical approach depends on preoperative evaluation and the underlying etiology of ptosis.
Follow-Up
1. Congenital: Close follow-up is required to monitor for the presence of amblyopia, caused either by occlusion or by refractive error secondary to induced corneal astigmatism, abnormal head positioning, and exposure keratopathy.
2. Traumatic: Observation for 6 months before considering surgical intervention.
3. Neurologic: Reevaluate based on particular entity.
4. Postoperative (after ptosis repair).
Acute: Monitor for infection and hemorrhage.
Subacute: Monitor for exposure keratopathy and for asymmetry that may require postoperative readjustment. Mild lagophthalmos is common for 2 to 3 weeks after surgical repair and usually resolves.
Chronic: Monitor for ptosis recurrence and exposure keratopathy.
6.2 CHALAZION/HORDEOLUM
Symptoms
Acute or chronic eyelid lump, eyelid swelling, tenderness.
Signs
(See Figure 6.2.1.)
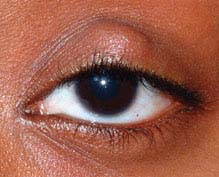
FIGURE 6.2.1. Chalazion.
Critical. Visible, or palpable, well-defined subcutaneous nodule in the eyelid. In some cases, a nodule cannot be identified.
Other. Blocked meibomian orifice, eyelid swelling and erythema, localized eyelid tenderness, associated blepharitis or acne rosacea. May also note “pointing” of mucopurulent material.
Definitions
Chalazion: Area of focal inflammation within the eyelid secondary to the obstruction of a meibomian gland or gland of Zeis.
Hordeolum: Acute infection; can be external (stye: abscess of gland of Zeis on lid margin) or internal (abscess of meibomian gland). Usually involves Staphylococcus species and occasionally evolves into a preseptal cellulitis.
Differential Diagnosis
 Preseptal cellulitis: Eyelid and periorbital erythema, edema, and warmth. See 6.10, Preseptal Cellulitis.
Preseptal cellulitis: Eyelid and periorbital erythema, edema, and warmth. See 6.10, Preseptal Cellulitis.
 Sebaceous carcinoma: Suspect in older patients with recurrent chalazia, eyelid thickening, or chronic unilateral blepharitis. See 6.11, Malignant Tumors of the Eyelid.
Sebaceous carcinoma: Suspect in older patients with recurrent chalazia, eyelid thickening, or chronic unilateral blepharitis. See 6.11, Malignant Tumors of the Eyelid.
 Pyogenic granuloma: Benign, deep-red, pedunculated lesion often associated with chalazia, hordeola, trauma, or surgery. May be excised or treated with a topical antibiotic–steroid combination such as neomycin/polymixin B/dexamethasone q.i.d. for 1 to 2 weeks. Intraocular pressure must be monitored if topical steroids are used.
Pyogenic granuloma: Benign, deep-red, pedunculated lesion often associated with chalazia, hordeola, trauma, or surgery. May be excised or treated with a topical antibiotic–steroid combination such as neomycin/polymixin B/dexamethasone q.i.d. for 1 to 2 weeks. Intraocular pressure must be monitored if topical steroids are used.
Work-Up
1. History: Previous ocular surgery or trauma? Previous chalazia or eyelid lesions?
2. External examination: Palpate the involved eyelid for a nodule.
3. Slit-lamp examination: Evaluate the meibomian glands for inspissation and evert the eyelid to rule out other etiologies.
Treatment
1. Warm compresses for 10 minutes q.i.d. with light massage over the lesion.
2. Consider a topical antibiotic if lesion is draining or for associated blepharitis (e.g., bacitracin or erythromycin ointment b.i.d.). Consider systemic therapy with doxycycline 100 mg b.i.d. for its antibacterial and anti-inflammatory actions.
3. If a hordeola worsens, consider incision and drainage and management as per preseptal cellulitis (see 6.10, Preseptal Cellulitis).
4. If the chalazion fails to resolve after 3 to 4 weeks of appropriate medical therapy and the patient wishes to have it removed, incision and curettage are performed. Occasionally, an injection of steroid (e.g., 0.2 to 1.0 mL of triamcinolone 40 mg/mL usually mixed 1:1 with 2% lidocaine with epinephrine) into the lesion is performed instead of minor surgery, especially if the chalazion is near the lacrimal apparatus. The total dosage depends on the size of the lesion. All recurrent or atypical chalazia must be sent for pathology.
NOTE: A steroid injection can lead to permanent depigmentation or atrophy of the skin at the injection site. The manufacturer of triamcinolone has recently recommended against its use intraocularly and in the periocular region. Vigorous injection can rarely result in retrograde intraarterial injection with resultant central retinal artery occlusion. Use of triamcinolone injection for chalazion treatment must include a detailed discussion between physician and patient, as well as adequate documentation in the patient’s record.
Follow-Up
Patients are not seen after instituting medical therapy unless the lesion persists beyond 3 to 4 weeks. Patients who have incision and curettage are reexamined in 1 week or as needed.
6.3 ECTROPION
Symptoms
Tearing, eye or eyelid irritation. May be asymptomatic.
Signs
(See Figure 6.3.1.)
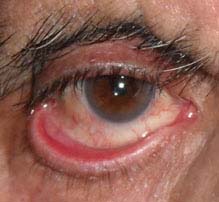
FIGURE 6.3.1. Ectropion.
Critical. Outward turning of the eyelid margin.
Other. Superficial punctate keratopathy (SPK) from corneal exposure; conjunctival injection, thickening, and eventual keratinization from chronic conjunctival dryness. Scarring of skin may be seen in cicatricial cases. Facial hemiparesis and lagophthalmos may be seen in paralytic cases.
Etiology
 Involutional: Aging.
Involutional: Aging.
 Paralytic: Seventh cranial nerve palsy.
Paralytic: Seventh cranial nerve palsy.
 Cicatricial: Due to chemical burn, surgery, eyelid laceration scar, skin diseases (e.g., eczema, ichthyosis), and others.
Cicatricial: Due to chemical burn, surgery, eyelid laceration scar, skin diseases (e.g., eczema, ichthyosis), and others.
 Mechanical: Due to herniated orbital fat, eyelid tumor, and others.
Mechanical: Due to herniated orbital fat, eyelid tumor, and others.
 Allergic: Contact dermatitis.
Allergic: Contact dermatitis.
 Congenital: Facial dysmorphic syndromes (e.g., Treacher–Collins syndrome) or isolated abnormality.
Congenital: Facial dysmorphic syndromes (e.g., Treacher–Collins syndrome) or isolated abnormality.
Work-Up
1. History: Previous surgery, trauma, chemical burn, or seventh nerve palsy?
2. External examination: Check orbicularis oculi function, look for an eyelid tumor, eyelid scarring, herniated orbital fat, and other causes.
3. Slit-lamp examination: Check for SPK due to exposure and evaluate conjunctival integrity.
Treatment
1. Treat exposure keratopathy with lubricating agents. See 4.5, Exposure Keratopathy.
2. Treat an inflamed, exposed eyelid margin with warm compresses and antibiotic ointment (e.g., bacitracin or erythromycin t.i.d.). A short course of combination antibiotic–steroid ointment (e.g., neomycin/polymixin B/dexamethasone) may be helpful if close follow-up is ensured.
3. Taping the eyelids into position may be a temporizing measure.
4. Definitive treatment usually requires surgery. Surgery is delayed for 3 to 6 months in patients with a seventh nerve palsy because the ectropion may resolve spontaneously (see 10.9, Isolated Seventh Nerve Palsy). Corneal exposure may make repair more urgent.
Follow-Up
Patients with signs of corneal or conjunctival exposure are examined every 1 to 2 weeks to evaluate the integrity of the ocular surface. Otherwise, follow-up is not urgent.
6.4 ENTROPION
Symptoms
Ocular irritation, foreign-body sensation, tearing, redness.
Signs
(See Figure 6.4.1.)
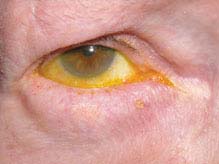
FIGURE 6.4.1. Entropion.
Critical. Inward turning of the eyelid margin that pushes otherwise normal lashes onto the globe.
Other. SPK from eyelashes contacting the cornea, conjunctival injection. In severe cases, corneal thinning and ulceration are possible.
Etiology
 Involutional: Aging.
Involutional: Aging.
 Cicatricial: Due to conjunctival scarring in ocular cicatricial pemphigoid, Stevens–Johnson syndrome, chemical burns, trauma, trachoma, and others.
Cicatricial: Due to conjunctival scarring in ocular cicatricial pemphigoid, Stevens–Johnson syndrome, chemical burns, trauma, trachoma, and others.
 Spastic: Due to surgical trauma, ocular irritation, or blepharospasm.
Spastic: Due to surgical trauma, ocular irritation, or blepharospasm.
 Congenital.
Congenital.
Work-Up
1. History: Previous surgery, trauma, chemical burn, or infection (trachoma, herpes simplex, and varicella zoster)?
2. Slit-lamp examination: Check for corneal involvement as well as conjunctival and eyelid scarring.
Treatment
If blepharospasm is present, see 6.7, Blepharospasm.
1. Antibiotic ointment (e.g., erythromycin or bacitracin ophthalmic t.i.d.) for SPK.
2. Everting the eyelid margin away from the globe and taping it in place with adhesive tape may be a temporizing measure.
3. For spastic entropion, a Quickert suture placed at the bedside or in the office can temporarily resolve the eyelid malposition.
4. Surgery is often required for permanent correction.
Follow-Up
If the cornea is relatively healthy, the condition does not require urgent attention or follow-up. If the cornea is significantly damaged, aggressive treatment is indicated (see 4.1, Superficial Punctate Keratopathy). Follow-up is determined by the severity of corneal involvement.
6.5 TRICHIASIS
Symptoms
Ocular irritation, foreign-body sensation, tearing, redness.
Signs
Critical. Misdirected eyelashes rubbing against the globe.
Other. SPK, conjunctival injection.
Differential Diagnosis
 Entropion: Inward turning of eyelid pushing normal lashes onto cornea. See 6.4, Entropion.
Entropion: Inward turning of eyelid pushing normal lashes onto cornea. See 6.4, Entropion.
 Epiblepharon: Congenital or familial condition in which an extra lower eyelid skin fold redirects lashes into a vertical position, where they may contact the globe. Most common in Asian individuals, especially children.
Epiblepharon: Congenital or familial condition in which an extra lower eyelid skin fold redirects lashes into a vertical position, where they may contact the globe. Most common in Asian individuals, especially children.
 Distichiasis: An aberrant second row of lashes that emanates from meibomian gland openings. Most commonly acquired in the setting of trauma or chronic inflammation (e.g., blepharitis). Congenital distichiasis is a rare, sometimes hereditary condition in which the meibomian glands are replaced by an extra row of eyelashes.
Distichiasis: An aberrant second row of lashes that emanates from meibomian gland openings. Most commonly acquired in the setting of trauma or chronic inflammation (e.g., blepharitis). Congenital distichiasis is a rare, sometimes hereditary condition in which the meibomian glands are replaced by an extra row of eyelashes.
Etiology
 Idiopathic.
Idiopathic.
 Chronic blepharitis: Inflamed eyelid margin. See 5.8, Blepharitis/Meibomitis.
Chronic blepharitis: Inflamed eyelid margin. See 5.8, Blepharitis/Meibomitis.
 Cicatricial: Eyelid scarring from trauma, surgery, ocular cicatricial pemphigoid (see 5.10, Ocular Cicatricial Pemphigoid), trachoma, and others.
Cicatricial: Eyelid scarring from trauma, surgery, ocular cicatricial pemphigoid (see 5.10, Ocular Cicatricial Pemphigoid), trachoma, and others.
Work-Up
1. History: Recurrent episodes? Severe systemic illness in the past? Previous trauma?
2. Slit-lamp examination: Evert the eyelids and inspect the palpebral conjunctiva for scarring and symblepharon. Check the cornea for abrasions and SPK.
Treatment
1. Epilation: Remove the misdirected lashes.
—A few misdirected lashes: Remove them at the slit lamp with fine forceps. Recurrence is common.
—Diffuse, severe, or recurrent trichiasis: Can attempt to epilate as described; definitive therapy usually requires electrolysis, cryotherapy, radiofrequency epilation, or eyelid surgery.
2. Treat SPK with antibiotic ointment (e.g., erythromycin or bacitracin t.i.d.).
3. Treat any underlying blepharitis. See 5.8, Blepharitis/Meibomitis.
Follow-Up
As needed based on the symptoms and integrity of the cornea. Closer follow-up is needed if evidence of SPK or corneal abrasion.
6.6 FLOPPY EYELID SYNDROME
Symptoms
Chronically red, irritated eye with mild mucous discharge, often worst on awakening from sleep due to eyelid eversion during the night. Usually bilateral but may be asymmetric. Typically seen in obese males. Strongly associated with sleep apnea.
Signs
Critical. Upper eyelids are easily everted without an accessory finger or cotton-tipped applicator exerting counterpressure.
Other. Soft and rubbery superior tarsal plate, superior tarsal papillary conjunctivitis, SPK, ptosis. Associated with keratoconus, obesity, hyperglycemia, and sleep apnea.
Differential Diagnosis
Key differentiating factor is laxity and spontaneous eversion of the upper eyelids.
 Vernal conjunctivitis: Seasonal, itching, and giant papillary reaction. See 5.2, Chronic Conjunctivitis.
Vernal conjunctivitis: Seasonal, itching, and giant papillary reaction. See 5.2, Chronic Conjunctivitis.
 Giant papillary conjunctivitis: Often related to contact lens wear or an exposed suture. See 4.22, Contact Lens-Induced Giant Papillary Conjunctivitis.
Giant papillary conjunctivitis: Often related to contact lens wear or an exposed suture. See 4.22, Contact Lens-Induced Giant Papillary Conjunctivitis.
 Superior limbic keratoconjunctivitis: Hyperemia and thickening of the superior bulbar conjunctiva. See 5.4, Superior Limbic Keratoconjunctivitis.
Superior limbic keratoconjunctivitis: Hyperemia and thickening of the superior bulbar conjunctiva. See 5.4, Superior Limbic Keratoconjunctivitis.
 Toxic keratoconjunctivitis: Papillae or follicles are usually more abundant on the inferior tarsal conjunctiva in a patient using eye drops. See 5.2, Chronic Conjunctivitis.
Toxic keratoconjunctivitis: Papillae or follicles are usually more abundant on the inferior tarsal conjunctiva in a patient using eye drops. See 5.2, Chronic Conjunctivitis.
Etiology
The underlying defect is not definitively known. Studies have suggested an abnormality of collagen and elastin fibers. The symptoms are thought to result from spontaneous eversion of the upper eyelid during sleep, allowing the superior palpebral conjunctiva to rub against a pillow or sheets. Unilateral symptoms are often on the side on which the patient predominantly sleeps.
Work-Up
1. Pull the upper eyelid toward the patient’s forehead to determine if it spontaneously everts or is abnormally lax.
2. Conduct slit-lamp examination of the cornea and conjunctiva with fluorescein staining, looking for upper palpebral conjunctival papillae and SPK.
3. Ask family members whether patient snores severely or if the patient has a history of sleep apnea.
Treatment
1. Topical antibiotic ointment for any mild corneal or conjunctival abnormality (e.g., erythromycin ointment b.i.d. to t.i.d.). May change to artificial tear ointment when lesions resolve.
2. The eyelids may be taped closed during sleep, or a shield may be worn to protect the eyelid from rubbing against the pillow or bed. Patients are asked to refrain from sleeping face down. Asking patients to sleep on their contralateral side may be therapeutic as well as diagnostic.
3. Surgical horizontal tightening of the eyelid is often required for definitive treatment.
Follow-Up
1. Every 2 to 7 days initially and then every few weeks to months as the condition stabilizes.
2. Refer to an internist, otolaryngologist, or pulmonologist for evaluation and management of possible obstructive sleep apnea. Evaluation is important because of the systemic sequelae of untreated sleep apnea and for anesthesia risk assessment before eyelid surgery.
6.7 BLEPHAROSPASM
Symptoms
Uncontrolled blinking, twitching, or closure of the eyelids. Always bilateral, but may briefly be unilateral at first onset.
Signs
Critical. Bilateral, episodic, involuntary contractions of the orbicularis oculi muscles.
Other. Disappears during sleep. May have uncontrolled orofacial, head, and neck movements (Meige syndrome).
Differential Diagnosis
 Hemifacial spasm: Unilateral contractures of the entire side of the face that do not disappear during sleep. Usually idiopathic but may be related to prior cranial nerve VII palsy, injury at the level of the brainstem, or compression of cranial nerve VII by a blood vessel or tumor. MRI of the cerebellopontine angle should be obtained in all patients to rule out tumor. Treatment options include observation, botulinum toxin injections, or neurosurgical decompression of cranial nerve VII.
Hemifacial spasm: Unilateral contractures of the entire side of the face that do not disappear during sleep. Usually idiopathic but may be related to prior cranial nerve VII palsy, injury at the level of the brainstem, or compression of cranial nerve VII by a blood vessel or tumor. MRI of the cerebellopontine angle should be obtained in all patients to rule out tumor. Treatment options include observation, botulinum toxin injections, or neurosurgical decompression of cranial nerve VII.
 Ocular irritation (e.g., corneal or conjunctival foreign body, trichiasis, blepharitis, dry eye).
Ocular irritation (e.g., corneal or conjunctival foreign body, trichiasis, blepharitis, dry eye).
 Eyelid myokymia: Subtle eyelid twitch felt by the patient but difficult to observe, commonly brought on by stress, caffeine, alcohol, or ocular irritation. Usually unilateral lower eyelid involvement. Typically self-limited and can be treated by avoiding precipitating factors.
Eyelid myokymia: Subtle eyelid twitch felt by the patient but difficult to observe, commonly brought on by stress, caffeine, alcohol, or ocular irritation. Usually unilateral lower eyelid involvement. Typically self-limited and can be treated by avoiding precipitating factors.
 Tourette syndrome: Multiple compulsive muscle spasms associated with utterances of bizarre sounds or obscenities.
Tourette syndrome: Multiple compulsive muscle spasms associated with utterances of bizarre sounds or obscenities.
 Tic douloureux (trigeminal neuralgia): Acute episodes of pain in the distribution of the fifth cranial nerve, often causing a wince or tic.
Tic douloureux (trigeminal neuralgia): Acute episodes of pain in the distribution of the fifth cranial nerve, often causing a wince or tic.
 Tardive dyskinesia: Orofacial dyskinesia, often with dystonic movements of the trunk and limbs, typically from long-term use of antipsychotic medications.
Tardive dyskinesia: Orofacial dyskinesia, often with dystonic movements of the trunk and limbs, typically from long-term use of antipsychotic medications.
 Apraxia of eyelid opening. Usually associated with Parkinson disease. Unlike blepahrospasm, apraxia of eyelid opening does not feature orbicularis spasm. Instead, apraxic patients simply cannot voluntarily open the eyelids.
Apraxia of eyelid opening. Usually associated with Parkinson disease. Unlike blepahrospasm, apraxia of eyelid opening does not feature orbicularis spasm. Instead, apraxic patients simply cannot voluntarily open the eyelids.
Etiology
 Idiopathic and likely multifactorial, possibly involving dopaminergic pathways within the basal ganglia.
Idiopathic and likely multifactorial, possibly involving dopaminergic pathways within the basal ganglia.
Work-Up
1. History: Unilateral or bilateral? Are the eyelids alone involved or are the facial and limb muscles also involved? Medications?
2. Slit-lamp examination: Examination for ocular disorders such as dry eyes, blepharitis, or a foreign body.
3. Neuro-ophthalmic examination to rule out other accompanying abnormalities.
4. Typical blepharospasm does not require CNS imaging as part of the work-up. MRI of the brain with attention to the posterior fossa is reserved for atypical cases or other diagnoses (e.g., hemifacial spasm).
Treatment
1. Treat any underlying eye disorder causing ocular irritation. See 4.3, Dry-Eye Syndrome, and 5.8, Blepharitis/Meibomitis.
2. Consider botulinum toxin injections into the orbicularis muscles around the eyelids if the blepharospasm is severe.
3. If the spasm is not relieved with botulinum toxin injections, consider surgical excision of the orbicularis muscle from the upper eyelids and brow (e.g., limited myectomy).
4. Muscle relaxants and sedatives are rarely of value but can be helpful in some patients. Oral medications such as lorazepam can help but their use is often limited by their sedative qualities.
Follow-Up
Not an urgent condition, but with severe blepharospasm, patients can be functionally blind.
6.8 CANALICULITIS
Symptoms
Tearing or discharge, red eye, mild tenderness over the nasal aspect of the lower or upper eyelid.
Signs
(See Figure 6.8.1.)
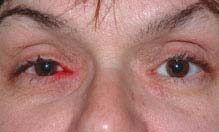
FIGURE 6.8.1. Canaliculitis.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


