Uveitis
12.1 ANTERIOR UVEITIS (IRITIS/IRIDOCYCLITIS)
Symptoms
 Acute: Pain, redness, photophobia, consensual photophobia (pain in the affected eye when a light is shone in the fellow eye), excessive tearing, decreased vision.
Acute: Pain, redness, photophobia, consensual photophobia (pain in the affected eye when a light is shone in the fellow eye), excessive tearing, decreased vision.
 Chronic: Decreased vision [from vitreous debris, cystoid macular edema (CME), or cataract]. May have periods of exacerbations and remissions with few acute symptoms [e.g., juvenile idiopathic (rheumatoid) arthritis (JIA/JRA)].
Chronic: Decreased vision [from vitreous debris, cystoid macular edema (CME), or cataract]. May have periods of exacerbations and remissions with few acute symptoms [e.g., juvenile idiopathic (rheumatoid) arthritis (JIA/JRA)].
Signs
Critical. Cells and flare in the anterior chamber, ciliary flush, keratic precipitates (KP):
 Fine KP (“stellate”; typically covers entire corneal endothelium): Herpetic, Fuchs heterochromic iridocyclitis (FHIC), cytomegalovirus (CMV) retinitis, and others.
Fine KP (“stellate”; typically covers entire corneal endothelium): Herpetic, Fuchs heterochromic iridocyclitis (FHIC), cytomegalovirus (CMV) retinitis, and others.
 Small, nongranulomatous KP: Human leukocyte antigen (HLA)-B27 associated, trauma, masquerade, JIA, Posner–Schlossman syndrome (glaucomatocyclitic crisis), and all the granulomatous entities.
Small, nongranulomatous KP: Human leukocyte antigen (HLA)-B27 associated, trauma, masquerade, JIA, Posner–Schlossman syndrome (glaucomatocyclitic crisis), and all the granulomatous entities.
 Granulomatous KP [large, greasy (“mutton-fat”); mostly on inferior cornea]: Sarcoidosis, syphilis, tuberculosis, sympathetic ophthalmia, lens-induced, Vogt–Koyanagi–Harada (VKH) syndrome, and others.
Granulomatous KP [large, greasy (“mutton-fat”); mostly on inferior cornea]: Sarcoidosis, syphilis, tuberculosis, sympathetic ophthalmia, lens-induced, Vogt–Koyanagi–Harada (VKH) syndrome, and others.
Other. Low intraocular pressure (IOP) more commonly seen (secondary to ciliary body hyposecretion), elevated IOP can occur (e.g., herpetic, lens-induced, FHIC, Posner–Schlossman syndrome), fibrin (HLA-B27 or endophthalmitis), hypopyon (HLA-B27, Behçet disease, infectious endophthalmitis, rifabutin, tumor), iris nodules (sarcoidosis, syphilis, tuberculosis), iris atrophy (herpetic), iris heterochromia (FHIC), iris synechiae (especially HLA-B27, sarcoidosis), band keratopathy (especially JIA in younger patients, any chronic uveitis in older), uveitis in a “quiet eye” (consider JIA, FHIC, masquerade syndromes), CME (see Figure 12.1.1).
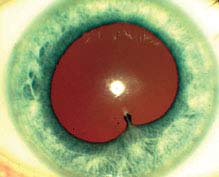
FIGURE 12.1.1. Anterior uveitis with posterior synechiae.
Differential Diagnosis
 Posterior uveitis with spillover into the anterior chamber: Mainly floaters and decreased vision, positive fundoscopic findings (see 12.3, Posterior Uveitis).
Posterior uveitis with spillover into the anterior chamber: Mainly floaters and decreased vision, positive fundoscopic findings (see 12.3, Posterior Uveitis).
 Traumatic iritis. See 3.5, Traumatic Iritis.
Traumatic iritis. See 3.5, Traumatic Iritis.
 Posner–Schlossman syndrome: Recurrent episodes of very high IOP and minimal inflammation. See 9.8, Glaucomatocyclitic Crisis/Posner–Schlossman Syndrome.
Posner–Schlossman syndrome: Recurrent episodes of very high IOP and minimal inflammation. See 9.8, Glaucomatocyclitic Crisis/Posner–Schlossman Syndrome.
 Drug-induced uveitis (e.g., rifabutin, cidofovir, sulfonamides, pamidronate, systemic moxifloxacin).
Drug-induced uveitis (e.g., rifabutin, cidofovir, sulfonamides, pamidronate, systemic moxifloxacin).
 Sclerouveitis: Uveitis secondary to scleritis; typically presents with profound pain.
Sclerouveitis: Uveitis secondary to scleritis; typically presents with profound pain.
 CLARE (contact lens-associated red eye): Red eye, corneal edema, epithelial defects, iritis with or without hypopyon, and no stromal infiltrates.
CLARE (contact lens-associated red eye): Red eye, corneal edema, epithelial defects, iritis with or without hypopyon, and no stromal infiltrates.
 Infectious keratouveitis: Corneal infiltrate is present. See 4.11, Bacterial Keratitis.
Infectious keratouveitis: Corneal infiltrate is present. See 4.11, Bacterial Keratitis.
 Infectious endophthalmitis: History of recent surgery or penetrating trauma, pain, hypopyon, fibrin, vitritis, decreased vision, red eye; may have endogenous source with fever, elevated white count. See 12.13 to 12.16, Endophthalmitis sections.
Infectious endophthalmitis: History of recent surgery or penetrating trauma, pain, hypopyon, fibrin, vitritis, decreased vision, red eye; may have endogenous source with fever, elevated white count. See 12.13 to 12.16, Endophthalmitis sections.
 Schwartz–Matsuo syndrome: Pigment released from a chronic retinal detachment clogs the trabecular meshwork resulting in elevated IOP.
Schwartz–Matsuo syndrome: Pigment released from a chronic retinal detachment clogs the trabecular meshwork resulting in elevated IOP.
 Tumor: Retinoblastoma in children, intraocular lymphoma in elderly, metastatic disease in all ages, and others.
Tumor: Retinoblastoma in children, intraocular lymphoma in elderly, metastatic disease in all ages, and others.
 Pseudouveitis from pigment dispersion syndromes. Other findings include krukenburg spindle and iris transillumination defects.
Pseudouveitis from pigment dispersion syndromes. Other findings include krukenburg spindle and iris transillumination defects.
Etiology
 Idiopathic.
Idiopathic.
 HLA-B27 associated uveitis: Systemic associations include ankylosing spondylitis, reactive arthritis (Reiter syndrome), psoriatic arthritis, inflammatory bowel disease.
HLA-B27 associated uveitis: Systemic associations include ankylosing spondylitis, reactive arthritis (Reiter syndrome), psoriatic arthritis, inflammatory bowel disease.
NOTE: Bilateral recurrent alternating anterior uveitis is very characteristic of HLA-B27 uveitis.
 Lens-induced uveitis: Immune reaction to lens material, often secondary to incomplete cataract extraction, trauma with lens capsule damage, or hypermature cataract. See 9.12, Lens-Induced (Phacogenic) Glaucoma.
Lens-induced uveitis: Immune reaction to lens material, often secondary to incomplete cataract extraction, trauma with lens capsule damage, or hypermature cataract. See 9.12, Lens-Induced (Phacogenic) Glaucoma.
 Postoperative iritis: Anterior chamber inflammation following intraocular surgery. Endophthalmitis must be considered if severe inflammation and pain are present. See 12.14, Chronic Postoperative Uveitis.
Postoperative iritis: Anterior chamber inflammation following intraocular surgery. Endophthalmitis must be considered if severe inflammation and pain are present. See 12.14, Chronic Postoperative Uveitis.
 Uveitis–Glaucoma–Hyphema (UGH) syndrome: Usually secondary to irritation from an intraocular lens (particularly a closed-loop anterior chamber lens or single-piece lens in ciliary sulcus). See 9.16, Postoperative Glaucoma.
Uveitis–Glaucoma–Hyphema (UGH) syndrome: Usually secondary to irritation from an intraocular lens (particularly a closed-loop anterior chamber lens or single-piece lens in ciliary sulcus). See 9.16, Postoperative Glaucoma.
 Behçet disease: Young adults, acute hypopyon, iritis, aphthous ulcers, genital ulcerations, erythema nodosum, retinal vasculitis (arteries and/or veins) and hemorrhages, may have recurrent episodes.
Behçet disease: Young adults, acute hypopyon, iritis, aphthous ulcers, genital ulcerations, erythema nodosum, retinal vasculitis (arteries and/or veins) and hemorrhages, may have recurrent episodes.
 Lyme disease: May have history of a tick bite and rash. See 13.3, Lyme Disease.
Lyme disease: May have history of a tick bite and rash. See 13.3, Lyme Disease.
 Anterior segment ischemia: Flare out of proportion to cellular reaction. Pain. Secondary to carotid insufficiency, tight scleral buckle, or previous muscle surgeries.
Anterior segment ischemia: Flare out of proportion to cellular reaction. Pain. Secondary to carotid insufficiency, tight scleral buckle, or previous muscle surgeries.
 Other rare etiologies of anterior uveitis: Mumps, influenza, adenovirus, measles, Chlamydia, Leptospirosis, Kawasaki disease, rickettsial disease, and others.
Other rare etiologies of anterior uveitis: Mumps, influenza, adenovirus, measles, Chlamydia, Leptospirosis, Kawasaki disease, rickettsial disease, and others.
Chronic
 JIA: Usually young girls, may be painless and asymptomatic with minimal injection. Often bilateral. Iritis may precede the typical pauciarticular arthritis (four or fewer joints involved). Positive antinuclear antibody (ANA), negative rheumatoid factor, and increased erythrocyte sedimentation rate (ESR) most commonly seen. Associated with glaucoma, cataracts, band keratopathy, and CME. Uveitis may occur in polyarticular and less frequently in systemic JIA.
JIA: Usually young girls, may be painless and asymptomatic with minimal injection. Often bilateral. Iritis may precede the typical pauciarticular arthritis (four or fewer joints involved). Positive antinuclear antibody (ANA), negative rheumatoid factor, and increased erythrocyte sedimentation rate (ESR) most commonly seen. Associated with glaucoma, cataracts, band keratopathy, and CME. Uveitis may occur in polyarticular and less frequently in systemic JIA.
 Chronic iridocyclitis of children: Usually young girls, similar to JIA except no arthritis.
Chronic iridocyclitis of children: Usually young girls, similar to JIA except no arthritis.
 FHIC: Few symptoms, diffuse iris stromal atrophy often causing a lighter-colored iris with transillumination defects and blunting of the iris architecture. Gonioscopy may reveal fine vessels that cross the trabecular meshwork, typically without posterior synechiae. Fine KP over the entire corneal endothelium, mild anterior chamber reaction. Vitreous opacities, glaucoma, and cataracts are common.
FHIC: Few symptoms, diffuse iris stromal atrophy often causing a lighter-colored iris with transillumination defects and blunting of the iris architecture. Gonioscopy may reveal fine vessels that cross the trabecular meshwork, typically without posterior synechiae. Fine KP over the entire corneal endothelium, mild anterior chamber reaction. Vitreous opacities, glaucoma, and cataracts are common.
 Sarcoidosis: More common in African-Americans and Scandinavians. Usually bilateral; can have extensive posterior synechiae or conjunctival nodules. See 12.6, Sarcoidosis.
Sarcoidosis: More common in African-Americans and Scandinavians. Usually bilateral; can have extensive posterior synechiae or conjunctival nodules. See 12.6, Sarcoidosis.
 Herpes simplex/varicella zoster: Corneal scars, history of unilateral recurrent red eye, occasionally history of skin vesicles, associated with decreased corneal sensation, increased IOP and iris atrophy.
Herpes simplex/varicella zoster: Corneal scars, history of unilateral recurrent red eye, occasionally history of skin vesicles, associated with decreased corneal sensation, increased IOP and iris atrophy.
 Syphilis: May have a maculopapular rash, iris roseola (vascular papules on the iris), and interstitial keratitis with ghost vessels in late stages. Inflammation of any ocular structure may occur. Neurosyphilis can have vitritis and meningismus. See 12.12, Syphilis.
Syphilis: May have a maculopapular rash, iris roseola (vascular papules on the iris), and interstitial keratitis with ghost vessels in late stages. Inflammation of any ocular structure may occur. Neurosyphilis can have vitritis and meningismus. See 12.12, Syphilis.
 Tuberculosis: Positive protein derivative of tuberculin (PPD), typical chest radiograph findings, occasionally phlyctenular or interstitial keratitis, sometimes signs of posterior uveitis. See 12.3, Posterior Uveitis.
Tuberculosis: Positive protein derivative of tuberculin (PPD), typical chest radiograph findings, occasionally phlyctenular or interstitial keratitis, sometimes signs of posterior uveitis. See 12.3, Posterior Uveitis.
 Others: Leprosy, brucellosis, etc.
Others: Leprosy, brucellosis, etc.
Work-Up
1. Obtain a thorough history and review of systems (Tables 12.1.1 and 12.1.2).
TABLE 12.1.1 Epidemiology of Anterior Uveitis
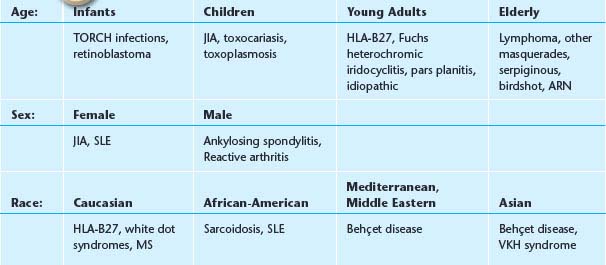
TABLE 12.1.2 Review of Systems
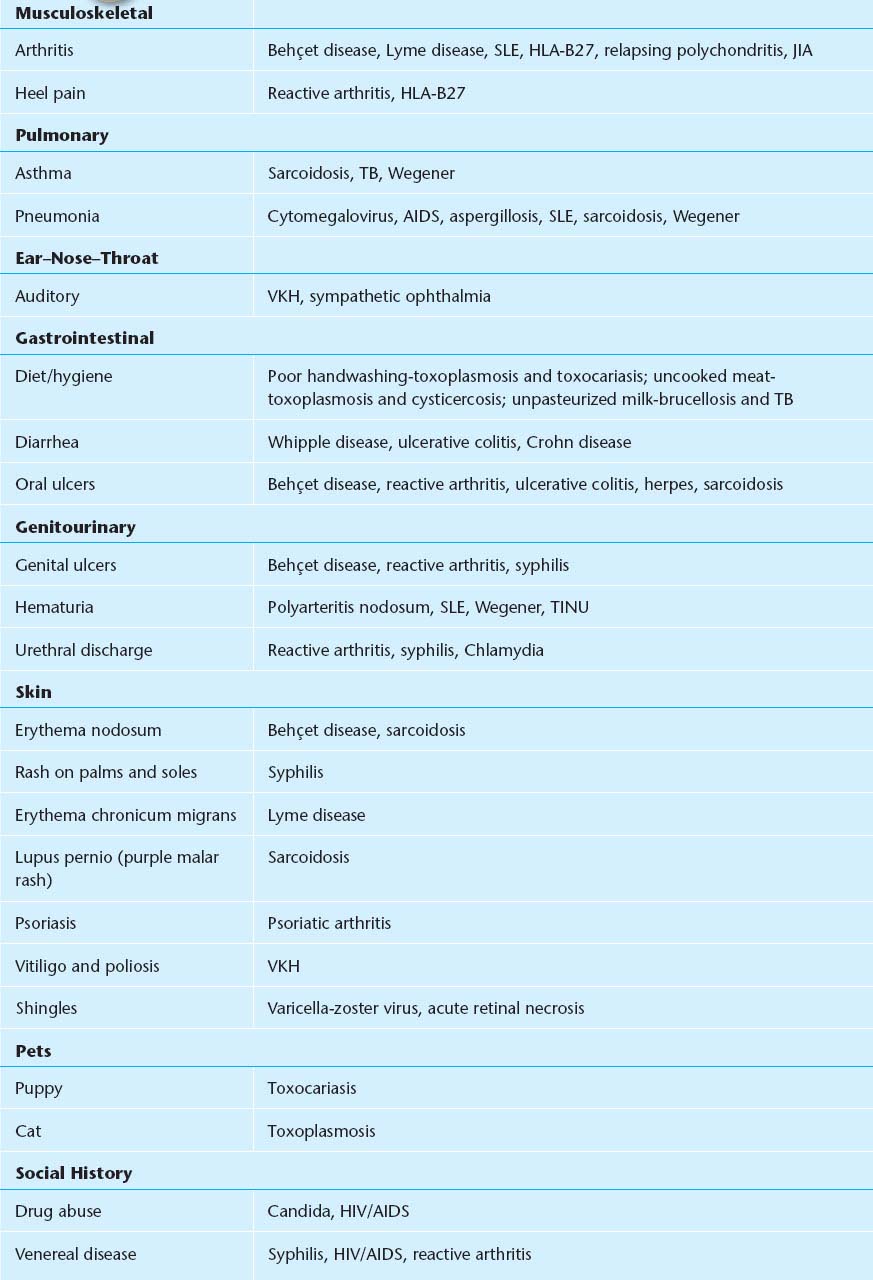
NOTE: Autoimmune diseases are less common in the very young and very old—consider masquerades.
Inflammatory arthritis typically presents with stiffness in the morning that improves after activity.
2. Complete ocular examination, including an IOP check, gonioscopy, and a dilated fundus examination. The vitreous should be evaluated for cells.
3. A laboratory work-up may be unnecessary in certain situations:
—First episode of a mild, unilateral, nongranulomatous uveitis with a history and examination that is not suggestive of systemic disease.
—Uveitis in the setting of known systemic disease such as sarcoidosis or the use of medicines known to cause uveitis (e.g., rifabutin).
—Clinical findings are classic for a particular diagnosis (e.g., herpetic keratouveitis, FHIC, toxoplasmosis).
4. If the uveitis is bilateral, granulomatous, or recurrent, and the history and examination are unremarkable, then a nonspecific initial work-up is conducted:
—Rapid plasma reagin (RPR) or venereal disease research laboratories test (VDRL).
—Fluorescent treponemal antibody absorption (FTA-ABS).
—PPD and anergy panel.
—Chest radiograph to rule out sarcoidosis and tuberculosis.
—Angiotensin-converting enzyme [(ACE); questionable utility].
—Lyme titer.
—ESR.
—HLA-B27.
NOTE: In children with uveitis, it is recommended to perform ANA, RF, and HLA-B27. Lyme titer and ACE may also be considered. Evaluation for systemic disease by a pediatric rheumatologist may be warranted.
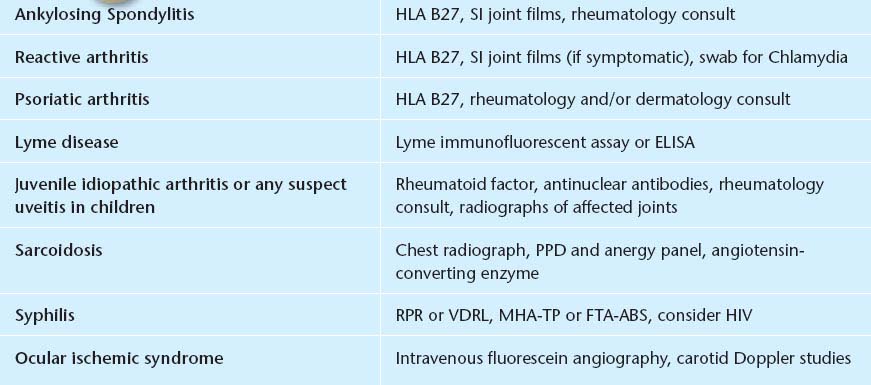
5. If a specific diagnosis is suspected, perform the appropriate work-up. If too many tests are ordered unnecessarily, a portion of them may come back false-positive and confuse the diagnosis. See Table 12.1.3.
TABLE 12.1.3 Suggested Diagnostic Workup for Anterior Uveitis
Treatment
1. Cycloplegic (e.g., scopolamine 0.25% b.i.d. for mild to moderate inflammation; atropine 1% b.i.d. for severe inflammation).
2. Topical steroid (prednisolone acetate 1% one drop q1–6h, depending on the severity, brand name is better than generic and often necessary). Most cases of moderate to severe acute uveitis require q1–2h dosing initially. Difluprednate 0.05% may allow less frequent dosing than prednisolone acetate. Consider FML ophthalmic ointment at night. If the anterior uveitis is severe, unilateral, and is not responding to topical steroids, then consider periocular repository steroids (e.g., triamcinolone 20 to 40 mg subtenon injection). See Appendix 10, Technique for Retrobulbar/Subtenon/Subconjunctival Injections.
NOTE: This is an off-label use of medication and patients must be advised appropriately. A trial of topical steroids at full strength for several weeks may help identify patients at risk of a significant IOP increase from steroids. Additionally, periocular depot steroids are relatively contraindicated in patients with scleritis.
3. If there is no improvement on maximal topical and repository steroids, or if the uveitis is bilateral and severe, consider systemic steroids, or immunosuppressive therapy. Consider referral to a uveitis specialist and rheumatologist.
NOTE: Prior to initiating systemic steroids or periocular depot steroids, it is important to rule out infectious causes.
4. Treat secondary glaucoma with aqueous suppressants. Avoid pilocarpine. Glaucoma may result from:
—Cellular blockage of the trabecular meshwork. See 9.7, Inflammatory Open-Angle Glaucoma.
—Secondary angle closure from synechiae formation. See 9.4, Acute Angle-Closure Glaucoma.
—Neovascularization of the iris and angle. See 9.14, Neovascular Glaucoma.
—Steroid-response. See 9.9, Steroid-Response Glaucoma.
5. If an exact etiology for the anterior uveitis is determined, then systemic management is required.
—Ankylosing spondylitis: Often requires systemic antiinflammatory agents (e.g., NSAIDs such as naproxen). Consider cardiology consult (high incidence of cardiomegaly, conduction defects, and aortic insufficiency), rheumatology consult, and physical therapy consult.
—Inflammatory bowel disease: Often benefits from systemic steroids, sulfadiazine, or other immunosuppressive agents. Obtain a medical or gastrointestinal consult.
—Reactive arthritis (Reiter syndrome): If urethritis is present, then the patient and sexual partners are treated for chlamydia (e.g., azithromycin 1 g, single dose). Obtain medical and/or rheumatology consult.
—Psoriatic arthritis: Consider a rheumatology and/or dermatology consult.
—Glaucomatocyclitic crisis: See 9.8, Glaucomatocyclitic Crisis/Posner–Schlossman Syndrome.
—Lens-induced uveitis: Usually requires removal of lens material. See 9.12, Lens-Induced (Phacogenic) Glaucoma.
—Herpetic uveitis: Herpes simplex typically requires topical or oral antivirals and steroid drops for corneal disease. Herpetic iridocyclitis benefits from topical steroids and systemic antiviral medications (e.g., acyclovir/valacyclovir). See 4.15, Herpes Simplex Virus and 4.16, Herpes Zoster Ophthalmicus/Varicella Zoster Virus.
—UGH syndrome: See 9.16, Postoperative Glaucoma.
—Behçet disease: See 12.7, Behçet Disease.
—Lyme disease: See 13.3, Lyme Disease.
—JIA: Steroid dosage is adjusted according to the degree of anterior chamber cells, not flare. Prolonged cycloplegic therapy may be required. Consult rheumatology or pediatrics as systemic steroid therapy or other systemic immunomdulatory therapy is often needed. Regular follow up is essential as flares may be asymptomatic but can cause extensive damage from synechiae, glaucoma, cystoid macular edema, and cataract formation.
NOTE: JIA has a high complication rate with cataract surgery. Avoid cataract surgery if possible until patient is free of inflammation for at least 3 months. An intraocular lens (IOL) may be placed in select circumstances.
—Chronic iridocyclitis of children: Same as JIA.
—FHIC: Usually does not respond to or require steroids (a trial of steroids may be attempted, but they should be tapered quickly if there is no response); cycloplegics are rarely necessary.
NOTE: Patients with FHIC usually do well with cataract surgery, however they may develop a hyphema.
—Sarcoidosis: See 12.6, Sarcoidosis.
—Syphilis: See 12.12, Syphilis.
—Tuberculosis: Avoid systemic steroids. Refer the patient to an internist or infectious disease specialist for consideration of systemic antituberculous treatment.
Follow-Up
1. Every 1 to 7 days in the acute phase, depending on the severity; every 1 to 6 months when stable.
2. At each visit, the anterior chamber reaction and IOP should be evaluated.
3. A vitreous and fundus examination should be performed for all flare-ups, when vision is affected, or every 3 to 6 months.
4. If the anterior chamber reaction has resolved, then the steroid drops can be slowly tapered [usually one drop per day every 3 to 7 days (e.g., q.i.d. for 1 week, then t.i.d. for 1 week, then b.i.d. for 1 week)]. Steroids are usually discontinued following the taper when the anterior chamber does not have any cellular reaction (flare may still be present). Rarely, long-term low-dose steroids every day or every other day are required to keep the inflammation from recurring. Punctal occlusion techniques may increase potency of drug and decrease systemic absorption. The cycloplegic agents also can be tapered as the anterior chamber reaction improves. Cycloplegics should be used at least every evening until the anterior chamber is free of cells.
NOTE: As with most ocular and systemic diseases requiring steroid therapy, the steroid should be tapered. Sudden discontinuation of steroids can lead to severe rebound inflammation.
12.2 INTERMEDIATE UVEITIS
Symptoms
Painless floaters and decreased vision. Minimal photophobia or external inflammation. Usually, 15 to 40 years of age and bilateral.
Signs
(See Figure 12.2.1.)
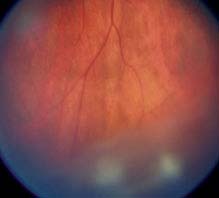
FIGURE 12.2.1. Pars planitis/intermediate uveitis with snowballs.
Critical. Vitreous cells, white exudative material over the inferior ora serrata and pars plana (snowbank), cellular aggregates floating predominantly in the inferior vitreous (snowballs). Younger patients may present with vitreous hemorrhage.
NOTE: Snowbanking is typically in the inferior vitreous and can often be seen only with indirect ophthalmoscopy and scleral depression.
Other. Peripheral retinal vascular sheathing, peripheral neovascularization, mild anterior chamber inflammation, CME, posterior subcapsular cataract, band keratopathy, secondary glaucoma, epiretinal membrane, and exudative retinal detachment.
Etiology
 Idiopathic pars planitis (>70%).
Idiopathic pars planitis (>70%).
 Sarcoidosis. See 12.6, Sarcoidosis.
Sarcoidosis. See 12.6, Sarcoidosis.
 Multiple sclerosis. See 10.14, Optic Neuritis.
Multiple sclerosis. See 10.14, Optic Neuritis.
 Lyme disease. See 13.3, Lyme Disease.
Lyme disease. See 13.3, Lyme Disease.
 Syphilis. See 12.12, Syphilis.
Syphilis. See 12.12, Syphilis.
 Toxocariasis. See 12.3, Posterior Uveitis, and 8.1, Leukocoria.
Toxocariasis. See 12.3, Posterior Uveitis, and 8.1, Leukocoria.
 Others: Inflammatory bowel disease, Bartonella, Whipple syndrome, primary Sjogrens syndrome, lymphoma, tubulointerstitial nephritis uveitis (TINU) syndrome, etc.
Others: Inflammatory bowel disease, Bartonella, Whipple syndrome, primary Sjogrens syndrome, lymphoma, tubulointerstitial nephritis uveitis (TINU) syndrome, etc.
Work-Up
1. Chest radiograph, PPD, ACE level, RPR, FTA-ABS.
2. Consider intravenous fluorescein angiography (IVFA) and/or optical coherence tomography (OCT) to document CME or retinal vasculitis.
3. Consider lab testing for Lyme disease, toxoplasmosis, cat-scratch disease. In older individuals, consider work-up for malignancy/lymphoma.
4. Consider magnetic resonance imaging (MRI) of the brain with gadolinium to evaluate for demyelinating lesions if review of systems is positive for current or previous focal neurologic deficits. Refer to neurologist for multiple sclerosis work-up if necessary.
Treatment
Treat all vision-threatening complications in symptomatic patients with active disease. Mild vitreous cell in the absence of symptoms or vision loss may be observed.
1. Topical prednisolone acetate 1% or difluprednate 0.05% q1–2h, and consider simultaneous subtenon steroid (0.5 to 1.0 mL of triamcinolone 40 mg/mL). Repeat the injections every 6 to 8 weeks until the vision and CME have stabilized. Slowly taper the frequency of injections. Subtenon steroid injections must be used with extreme caution in patients with steroid-responsive glaucoma. See Appendix 10, Technique for Retrobulbar/Subtenon/Subconjunctival Injections.
2. If no improvement after three injections, consider systemic steroids (e.g., prednisone 40 to 60 mg p.o. q.d. for 4 to 6 weeks), tapering gradually according to the patient’s response. Systemic steroid therapy should be no longer than 3 months, including taper. Other options include slow release steroid implants (dexamethasone 0.7 mg intravitreal implant, and fluocinolone acetonide 0.59 mg intravitreal implant), and immunomodulatory therapy, often in conjunction with Rheumatology.
NOTE: In bilateral cases, systemic steroid therapy is often preferred to periocular injections.
3. Transscleral cryotherapy to the area of snowbanking should be considered in patients who fail to respond to either oral or subtenon corticosteroids.
4. Pars plana vitrectomy may be useful in cases refractory to systemic steroids or to treat vitreous opacification, tractional retinal detachment, epiretinal membrane, and other complications. Additionally, vitreous biopsy through a pars plana vitrectomy may be indicated in cases of suspected masquerade syndromes, particularly, intraocular lymphoma.
NOTE:
1. Some physicians delay steroid injections for several weeks to observe whether the IOP increases on topical steroids (steroid response). If a steroid response is found, depot injections should be avoided.
2. Topical NSAIDs (e.g., ketorolac q.i.d.) may be added in patients with CME.
3. Cataracts are a frequent complication of intermediate uveitis. If cataract extraction is performed, the patient should ideally be free of inflammation for 3 months. Consider starting the patient on oral prednisone 60 mg daily 5 days prior to surgery and tapering the prednisone over the next month. Consider a combined pars plana vitrectomy at the time of cataract surgery if significant vitreous opacification is present.
Follow-Up
1. In the acute phase, patients are reevaluated every 1 to 4 weeks, depending on the severity of the condition.
2. In the chronic phase, reexamination is performed every 3 to 6 months.
12.3 POSTERIOR UVEITIS
Symptoms
Blurred vision and floaters. Pain, redness, and photophobia are typically absent unless anterior chamber inflammation is present.
NOTE: Posterior uveitis with significant pain suggests bacterial endophthalmitis or posterior scleritis.
Signs
Critical. Cells in the anterior and/or posterior vitreous, vitreous haze, retinal or choroidal inflammatory lesions, vasculitis (sheathing and exudates around vessels).
Other. Anterior segment inflammatory signs, CME.
Differential Diagnosis
Panuveitis
Describes a pattern of severe, diffuse inflammation of both anterior and posterior segments. Often bilateral. Possible etiologies are listed below:
 Sarcoidosis: See 12.6, Sarcoidosis.
Sarcoidosis: See 12.6, Sarcoidosis.
 Syphilis: See 12.12, Syphilis.
Syphilis: See 12.12, Syphilis.
 VKH syndrome: See 12.11, Vogt–Koyanagi–Harada Syndrome.
VKH syndrome: See 12.11, Vogt–Koyanagi–Harada Syndrome.
 Behçet disease: See 12.1, Anterior Uveitis (Iritis/Iridocyclitis), and 12.7, Behçet Disease.
Behçet disease: See 12.1, Anterior Uveitis (Iritis/Iridocyclitis), and 12.7, Behçet Disease.
 Lens-induced uveitis: See 9.12, Lens-Induced (Phacogenic) Glaucoma.
Lens-induced uveitis: See 9.12, Lens-Induced (Phacogenic) Glaucoma.
 Sympathetic ophthalmia: See 12.18, Sympathetic Ophthalmia.
Sympathetic ophthalmia: See 12.18, Sympathetic Ophthalmia.
 Tuberculosis: Produces varied clinical manifestations. The diagnosis is usually made by ancillary laboratory tests. Miliary tuberculosis may produce multifocal, small, yellow-white choroidal lesions. Most patients have concomitant anterior granulomatous or nongranulomatous uveitis.
Tuberculosis: Produces varied clinical manifestations. The diagnosis is usually made by ancillary laboratory tests. Miliary tuberculosis may produce multifocal, small, yellow-white choroidal lesions. Most patients have concomitant anterior granulomatous or nongranulomatous uveitis.
Postsurgical/Trauma
See 12.13, Postoperative Endophthalmitis; 12.14, Chronic Postoperative Uveitis; 12.15, Traumatic Endophthalmitis; and 12.18, Sympathetic Ophthalmia.
Choroiditis
 Acute posterior multifocal placoid pigment epitheliopathy (APMPPE): Acute visual loss in young adults, often after a viral illness. Multiple, creamy yellow–white, plaque-like subretinal lesions in both eyes. Lesions block early and stain late on IVFA. Usually spontaneously improves. Rarely associated with a cerebral vasculitis.
Acute posterior multifocal placoid pigment epitheliopathy (APMPPE): Acute visual loss in young adults, often after a viral illness. Multiple, creamy yellow–white, plaque-like subretinal lesions in both eyes. Lesions block early and stain late on IVFA. Usually spontaneously improves. Rarely associated with a cerebral vasculitis.
 Birdshot retinochoroidopathy: Usually middle-aged, with bilateral, multiple, creamy-yellow spots deep to the retina, approximately 1 mm in diameter, scattered throughout the fundus. A mild to moderate vitritis is present. Retinal or optic nerve edema or both may be present. Positive HLA-A29 in approximately 90% of patients. Consider systemic immunosuppression.
Birdshot retinochoroidopathy: Usually middle-aged, with bilateral, multiple, creamy-yellow spots deep to the retina, approximately 1 mm in diameter, scattered throughout the fundus. A mild to moderate vitritis is present. Retinal or optic nerve edema or both may be present. Positive HLA-A29 in approximately 90% of patients. Consider systemic immunosuppression.
 Multifocal choroiditis: Visual loss in young myopic women, typically bilateral. Multiple, small, round, pale inflammatory lesions (similar to histoplasmosis) are located at the level of the pigment epithelium and choriocapillaris. Unlike histoplasmosis, vitritis occurs in 98% of patients. The lesions are predominantly in the macula and frequently respond to oral or periocular steroids, but typically recur. Choroidal neovascularization (CNV) is common, and so patients should return for urgent evaluation if they have decreased vision or metamorphopsia.
Multifocal choroiditis: Visual loss in young myopic women, typically bilateral. Multiple, small, round, pale inflammatory lesions (similar to histoplasmosis) are located at the level of the pigment epithelium and choriocapillaris. Unlike histoplasmosis, vitritis occurs in 98% of patients. The lesions are predominantly in the macula and frequently respond to oral or periocular steroids, but typically recur. Choroidal neovascularization (CNV) is common, and so patients should return for urgent evaluation if they have decreased vision or metamorphopsia.
 Punctate inner choroidopathy: Blurred vision, paracentral scotoma, and/or photopsias, usually in young myopic women. Multiple, small round yellow–white spots predominantly in posterior pole with minimal intraocular inflammation. Lesions become well-demarcated atrophic scars within weeks. CNV may develop in up to 40% of patients.
Punctate inner choroidopathy: Blurred vision, paracentral scotoma, and/or photopsias, usually in young myopic women. Multiple, small round yellow–white spots predominantly in posterior pole with minimal intraocular inflammation. Lesions become well-demarcated atrophic scars within weeks. CNV may develop in up to 40% of patients.
 Serpiginous choroidopathy: Typically bilateral, recurrent chorioretinitis characterized by acute lesions (yellow–white subretinal patches with indistinct margins) bordering old atrophic scars. The chorioretinal changes usually extend from the optic disc outward; however, one-third may begin peripherally. Patients are typically aged 30 to 60 years. Strongly consider systemic immunosuppression. CNV may develop.
Serpiginous choroidopathy: Typically bilateral, recurrent chorioretinitis characterized by acute lesions (yellow–white subretinal patches with indistinct margins) bordering old atrophic scars. The chorioretinal changes usually extend from the optic disc outward; however, one-third may begin peripherally. Patients are typically aged 30 to 60 years. Strongly consider systemic immunosuppression. CNV may develop.
 Toxocariasis: Typically unilateral. Usually occurs in children. The most common presentations are a macular granuloma (elevated white retinal/subretinal lesion) with poor vision, unilateral pars planitis with peripheral granuloma, or endophthalmitis. A peripheral lesion may be associated with a fibrous band extending to the optic disc, sometimes resulting in macular vessel dragging. A severe vitritis and anterior uveitis may be present. A negative undiluted Toxocara titer in an immunocompetent host usually rules out this disease. See 8.1, Leukocoria.
Toxocariasis: Typically unilateral. Usually occurs in children. The most common presentations are a macular granuloma (elevated white retinal/subretinal lesion) with poor vision, unilateral pars planitis with peripheral granuloma, or endophthalmitis. A peripheral lesion may be associated with a fibrous band extending to the optic disc, sometimes resulting in macular vessel dragging. A severe vitritis and anterior uveitis may be present. A negative undiluted Toxocara titer in an immunocompetent host usually rules out this disease. See 8.1, Leukocoria.
 Presumed ocular histoplasmosis syndrome: Punched-out chorioretinal scars, peripapillary atrophy, and often CNV. Vitreous cells are absent. See 11.24, Ocular Histoplasmosis.
Presumed ocular histoplasmosis syndrome: Punched-out chorioretinal scars, peripapillary atrophy, and often CNV. Vitreous cells are absent. See 11.24, Ocular Histoplasmosis.
Retinitis
 Multiple evanescent white-dot syndrome: Photopsias and acute unilateral visual loss, often after a viral illness, usually in young women. Uncommonly bilateral or sequential. Multiple, small, creamy white lesions deep in the retina or at the level of the retinal pigment epithelium with foveal granularity and occasionally vitreous cells. There is often an enlarged blind spot on formal visual field testing. May have a shimmering scotoma. Vision typically returns to normal within weeks without treatment.
Multiple evanescent white-dot syndrome: Photopsias and acute unilateral visual loss, often after a viral illness, usually in young women. Uncommonly bilateral or sequential. Multiple, small, creamy white lesions deep in the retina or at the level of the retinal pigment epithelium with foveal granularity and occasionally vitreous cells. There is often an enlarged blind spot on formal visual field testing. May have a shimmering scotoma. Vision typically returns to normal within weeks without treatment.
 CMV: Whitish patches of necrotic retina are mixed with retinal hemorrhage. Seen in neonates and immunocompromised patients. See 12.9, Cytomegalovirus Retinitis.
CMV: Whitish patches of necrotic retina are mixed with retinal hemorrhage. Seen in neonates and immunocompromised patients. See 12.9, Cytomegalovirus Retinitis.
 Acute retinal necrosis (ARN): Unilateral or bilateral peripheral white patches of thickened necrotic retina with vascular sheathing that progress rapidly. A significant vitritis is typically present. See 12.8, Acute Retinal Necrosis.
Acute retinal necrosis (ARN): Unilateral or bilateral peripheral white patches of thickened necrotic retina with vascular sheathing that progress rapidly. A significant vitritis is typically present. See 12.8, Acute Retinal Necrosis.
 Progressive outer retinal necrosis (PORN): Clinically similar to ARN, but may not have vitreous cells and involves the posterior pole early. Often in immunocompromised patients. See 12.8, Acute Retinal Necrosis.
Progressive outer retinal necrosis (PORN): Clinically similar to ARN, but may not have vitreous cells and involves the posterior pole early. Often in immunocompromised patients. See 12.8, Acute Retinal Necrosis.
 Toxoplasmosis: Retinal lesion associated with a pigmented chorioretinal scar. Focal dense vitritis. See 12.5, Toxoplasmosis.
Toxoplasmosis: Retinal lesion associated with a pigmented chorioretinal scar. Focal dense vitritis. See 12.5, Toxoplasmosis.
 Candida: Early discrete drusen-like choroidal lesions progressing to yellow–white, fluffy retinal or preretinal lesions. See 12.17, Candida Retinitis/Uveitis/Endophthalmitis.
Candida: Early discrete drusen-like choroidal lesions progressing to yellow–white, fluffy retinal or preretinal lesions. See 12.17, Candida Retinitis/Uveitis/Endophthalmitis.
Vasculitis
Retinal sheathing around vessels. Branch retinal vein and branch retinal artery occlusions may occur.
 Periphlebitis (predominantly veins).
Periphlebitis (predominantly veins).
—Sarcoidosis: Yellow “candlewax” exudates around veins.
—Syphilis.
—Pars planitis: Most prominent in the inferior periphery, NVE may be present.
—Eales disease: Peripheral neovascularization and/or avascular retina.
—Multiple sclerosis.
—Birdshot retinochoroidopathy.
 Arteritis (predominantly arteries).
Arteritis (predominantly arteries).
—Giant cell arteritis.
—Polyarteritis nodosum.
—Frosted branch angiitis.
—Churg-Strauss.
—ARN.
—IRVAN (idiopathic retinal vasculitis, aneurysms, and neuroretinitis).
 Both arteries and veins.
Both arteries and veins.
—Systemic lupus erythematosus.
—Wegener granulomatosis.
—Behçet disease.
—HLA-B27-associated.
Other Infectious Causes of Posterior Uveitis
 Cat-scratch disease: Stellate macular exudates, optic nerve swelling, vitreous cells, positive Bartonella serology. See 5.3, Parinaud Oculoglandular Conjunctivitis.
Cat-scratch disease: Stellate macular exudates, optic nerve swelling, vitreous cells, positive Bartonella serology. See 5.3, Parinaud Oculoglandular Conjunctivitis.
 Diffuse unilateral subacute neuroretinitis: Typically unilateral visual loss in children and young adults, caused by a nematode. Optic nerve swelling, vitreous cells, and deep gray–white retinal lesions are present initially, but may be subtle. Later, optic atrophy, narrowing of retinal vessels, and atrophic pigment epithelial changes develop. Vision, visual fields, and ERG deteriorate with time. Treatment is to laser nematode.
Diffuse unilateral subacute neuroretinitis: Typically unilateral visual loss in children and young adults, caused by a nematode. Optic nerve swelling, vitreous cells, and deep gray–white retinal lesions are present initially, but may be subtle. Later, optic atrophy, narrowing of retinal vessels, and atrophic pigment epithelial changes develop. Vision, visual fields, and ERG deteriorate with time. Treatment is to laser nematode.
 Lyme disease: Produces varied forms of posterior uveitis. See 13.3, Lyme Disease.
Lyme disease: Produces varied forms of posterior uveitis. See 13.3, Lyme Disease.
 Nocardia, Coccidioides species, Aspergillus species, Cryptococcus species, meningococcus, ophthalmomyiasis, onchocerciasis, and cysticercosis (seen more commonly in Africa and Central and South America).
Nocardia, Coccidioides species, Aspergillus species, Cryptococcus species, meningococcus, ophthalmomyiasis, onchocerciasis, and cysticercosis (seen more commonly in Africa and Central and South America).
Other Causes of Vitreous Cells
 Ocular ischemia.
Ocular ischemia.
 Spillover from anterior uveitis.
Spillover from anterior uveitis.
 Masquerade syndromes: Always consider these in the very old or very young patient.
Masquerade syndromes: Always consider these in the very old or very young patient.
—Large cell lymphoma (reticulum cell sarcoma): Persistent vitreous cells in patients >50 years, which usually do not respond completely to systemic steroids. Yellow–white subretinal infiltrates, retinal edema and hemorrhage, anterior chamber inflammation, or neurologic signs may be present.
—Malignant melanoma: A retinal detachment and associated vitritis may obscure the underlying tumor. See 11.36, Choroidal Nevus and Malignant Melanoma of the Choroid.
—Retinitis pigmentosa: Vitreous cells and macular edema may accompany waxy pallor of the optic disc, “bone-spicule” pigmentary changes, and attenuated retinal vessels. See 11.28, Retinitis Pigmentosa and Inherited Chorioretinal Dystrophies.
—Rhegmatogenous retinal detachment (RRD): A small number of pigmented anterior vitreous and anterior chamber cells frequently accompany an RRD. See 11.3, Retinal Detachment.
—Retained intraocular foreign body: Persistent inflammation after a penetrating ocular injury. May have iris heterochromia. Diagnosed by indirect ophthalmoscopy, gonioscopy, B-scan ultrasonography (US), US biomicroscopy, or computed tomography (CT) scan of the globe. See 3.15, Intraocular Foreign Body.
—Retinoblastoma: Almost always occurs in young children. May also present with a pseudohypopyon and vitreous cells. One or more elevated white retinal lesions are usually, but not always, present. See 8.1, Leukocoria.
—Leukemia: Unilateral retinitis and vitritis may occur in patients already known to have leukemia.
—Amyloidosis: Retrolenticular footplate-like deposits, vitreous globules, or membranes without any signs of anterior segment inflammation. Serum protein electrophoresis and diagnostic vitrectomy confirm the diagnosis. Rare.
—Asteroid hyalosis: Small, white, refractile particles (calcium soaps) adherent to collagen fibers and floating in the vitreous. Usually asymptomatic and of no clinical significance.
Work-Up
1. Complete history and review of systems: Systemic disease or infection, skin rash, intravenous (i.v.) drug abuse, indwelling catheter, risk factors for AIDS? Recent eye trauma or surgery? Travel to the Ohio–Mississippi River Valley, Southwestern United States, New England, or Middle Atlantic area? Tick bite?
2. Complete ocular examination, including IOP measurement and careful ophthalmoscopic examination. Indirect ophthalmoscopy with scleral depression of the ora serrata.
3. Consider IVFA to help in diagnosis or plan for therapy.
4. Blood tests (any of the following are obtained, depending on the suspected diagnosis): Toxoplasma titer, ACE level, serum lysozyme, FTA-ABS, RPR, ESR, ANA, HLA-B51 (Behçet disease), HLA-A29 (birdshot retinochoroidopathy), Toxocara titer, Lyme immunofluorescent assay or ELISA. In neonates or immunocompromised patients, consider checking titers for CMV, herpes simplex, varicella zoster, and rubella virus. Cultures of blood and i.v. sites may be helpful when infectious etiologies are suspected. Polymerase chain reaction (PCR) techniques are available for varicella zoster, herpes simplex, Toxoplasma, and other pathogens.
5. PPD with anergy panel.
6. Chest radiograph.
7. Urine for CMV in immunocompromised patients.
8. CT/MRI scan of the brain and lumbar puncture when reticulum cell sarcoma is suspected and when human immunodeficiency virus (HIV)-associated opportunistic infections indicate a potential for central nervous system (CNS) involvement.
9. Diagnostic vitrectomy when appropriate (see individual sections).
See the individual sections for more specific guidelines for work-up and treatment.
12.4 HUMAN LEUKOCYTE ANTIGEN–B27–ASSOCIATED UVEITIS
Symptoms
Acute pain, blurred vision, photophobia. Associated systemic complaints include back pain, arthritis, oral ulcers (typically not as painful as those seen in Behçet disease), pain with urination, gastrointestinal complaints, rashes.
Signs
Critical. Recurrent, unilateral (or bilateral) nongranulomatous anterior uveitis.
Other. Severe anterior chamber reaction with cell, flare, and fibrin. May have hypopyon. Tendency to form posterior synechiae early. Ciliary flush. More common in men than women.
Differential Diagnosis
 Other hypopyon uveitides: Behçet disease (posterior involvement more common than in HLA-B27), infectious endophthalmitis, retinoblastoma, metastatic tumors, rifabutin, sarcoidosis, masquerade syndromes.
Other hypopyon uveitides: Behçet disease (posterior involvement more common than in HLA-B27), infectious endophthalmitis, retinoblastoma, metastatic tumors, rifabutin, sarcoidosis, masquerade syndromes.
 Idiopathic anterior uveitis.
Idiopathic anterior uveitis.
Types of HLA-B27 Disease
 HLA-B27-associated uveitis without systemic disease.
HLA-B27-associated uveitis without systemic disease.
 Ankylosing spondylitis: Young adult men, often with low back pain or stiffness, abnormalities on sacroiliac spine radiographs, increased ESR, positive HLA-B27.
Ankylosing spondylitis: Young adult men, often with low back pain or stiffness, abnormalities on sacroiliac spine radiographs, increased ESR, positive HLA-B27.
 Inflammatory bowel disease: Crohn disease and ulcerative colitis. Chronic diarrhea.
Inflammatory bowel disease: Crohn disease and ulcerative colitis. Chronic diarrhea.
 Reactive arthritis (Reiter syndrome): Young adult men, conjunctivitis, urethritis, polyarthritis, occasionally keratitis, increased ESR, positive HLA-B27, may have recurrent episodes. Arthritis tends to involve the lower extremities.
Reactive arthritis (Reiter syndrome): Young adult men, conjunctivitis, urethritis, polyarthritis, occasionally keratitis, increased ESR, positive HLA-B27, may have recurrent episodes. Arthritis tends to involve the lower extremities.
 Psoriatic arthritis: Characteristic skin findings with arthritis typically involving the upper extremities.
Psoriatic arthritis: Characteristic skin findings with arthritis typically involving the upper extremities.
Work-Up
1. HLA-B27 to confirm diagnosis.
2. Ankylosing spondylitis: Sacroiliac spine radiographs show sclerosis and narrowing of the joint spaces, ESR.
3. Inflammatory bowel disease: Medicine or Gastroenterology consult.
4. Reactive arthritis: Conjunctival and urethral swabs for Chlamydia if indicated; a Medicine or Rheumatology consult.
5. Psoriatic arthritis: A Rheumatology or Dermatology consult.
Treatment
See 12.1, Anterior Uveitis (Iritis/Iridocyclitis). Patients with HLA-B27 uveitis often suffer multiple recurrences. For particularly relapsing cases, consider longer-term steroid sparing immunomodulatory therapy, often in conjunction with Rheumatology.
12.5 TOXOPLASMOSIS
Symptoms
Blurred vision and floaters. May have redness and photophobia. Pain is typically absent, except with iridocyclitis.
Signs
(See Figure 12.5.1.)
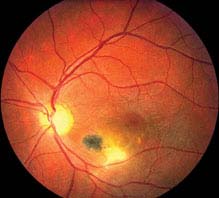
FIGURE 12.5.1. Toxoplasmosis.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


