Current Management Decisions in Retinal Vein Occlusion
Philip Storey
Anita P. Schadlu
Jason Hsu
CENTRAL RETINA VEIN OCCLUSION
Background
Central retinal vein occlusion (CRVO) is caused by obstruction of retinal venous flow, resulting in dilated and tortuous retinal veins. Diffuse intraretinal hemorrhage, cotton-wool spots, and macular edema are typically seen. The pathogenesis of CRVO is believed to follow Virchow’s triad of endothelial damage, hemostasis, and hypercoagulability.1 The most commonly accepted cause of venous obstruction is thrombus formation in the region of the lamina cribrosa precipitated by a thickened retinal artery, often due to atherosclerosis, compressing an adjacent retinal vein. The hypothesis that CRVO is caused by thrombus in the central retinal vein is based upon an autopsy study confirming fresh or recanalized thrombus in eyes with both recent and longstanding CRVO.2 The most common cause of vision loss in patients with CRVO is macular edema. Vision loss may also be caused by macular ischemia or neovascularization leading to vitreous hemorrhage or neovascular glaucoma. Visual improvement in patients following acute CRVO occurs by reduction of macular edema or by reperfusion of the retinal vasculature through either recanalization of the central vein or collateral vessel development. The natural history of CRVO is variable. In a systematic literature review of 3,271 eyes, baseline visual acuity (VA) was generally poor (<20/40) and decreased in the majority of cases.3 One-third of nonischemic CRVO eyes converted to ischemic CRVO over a 3-year period and neovascular glaucoma developed in approximately one quarter of eyes with ischemic CRVO within 15 months. Finally, macular edema spontaneously improved in only 30% of eyes with nonischemic CRVO.
Until recently, treatment of CRVO was largely limited to laser photocoagulation for neovascularization. Over the last decade, a number of interventions have been developed for the treatment of CRVO. Treatment modalities can be broadly classified into two categories: aiming to treat the sequelae of venous occlusion, including macular edema, retinal ischemia, and neovascularization or targeting the causal pathology of venous obstruction.
Interventions Targeting Sequelae
Laser Treatment
Published in 1995, the Central Vein Occlusion Study (CVOS) was a multicenter, randomized, controlled trial of 155 eyes investigating the effectiveness of laser treatment for CRVO, which successfully defined the standard of care. The CVOS established panretinal photocoagulation as the treatment of choice for neovascularization due to CRVO as the risk of neovascular glaucoma was significantly reduced with treatment.4 However, the study also demonstrated that prophylactic panretinal photocoagulation in eyes with ischemic CRVO does not result in significant decreases in the development of neovascularization of the iris or of the angle. The authors of the CVOS therefore recommended that panretinal photocoagulation be deferred until neovascularization develops. The study also showed that patients with visual acuity of 20/50 or worse due to CRVO and macular edema did not maintain or improve their vision after 3 years of treatment with grid laser photocoagulation.5 While the CVOS demonstrated that grid macular laser photocoagulation decreases macular edema, the treatment is not recommended, as it did not result in improvement of final visual acuity.
Corticosteroids
Macular edema due to CRVO is thought to occur due to local inflammation6 as well as the breakdown of the blood-retinal barrier mediated in part by vascular endothelial growth factor (VEGF).7 Corticosteroids have been shown to inhibit the expression of VEGF8 and to have anti-inflammatory properties,9 thus justifying the exploration of their use for CRVO. The Standard Care versus Corticosteroid for Retinal Vein Occlusion (SCORE) study was a multicenter, randomized, controlled trial evaluating 1 and 4 mg doses of intravitreal triamcinolone every 4 months for the duration of the study when re-treatment criteria were met compared to observation in 271 patients with vision loss due to CRVO and macular edema.10 At 12 and 24 months, patients treated with triamcinolone were three to four times more likely than the observation group to have gained at least 15 letters (3 lines) than the observation group (12 months: 27% 1 mg group, 26% 4 mg group, 7% observation group; P = .001; 24 months: 31% 1 mg group, 26% 4 mg group, 9% observation group; P = .001). At 2 years, the beneficial effect of triamcinolone had attenuated somewhat, which the authors postulated may have been related to cataract formation. Nevertheless, the triamcinolone groups remained favorable compared to observation in terms of visual acuity and proportion gaining at least 15 letters (31% 1 mg group, 26% 4 mg group, 9% observation group). Adverse effects of triamcinolone included elevated ocular pressure and increased risk of cataracts, which were more prevalent in the 4 mg group as compared to the 1 mg group. At 12 months, patients treated with triamcinolone had significantly higher rates of initiating IOP-lowering medication (20% 1 mg group and 35% 4 mg group vs. 8% observation group). At 2 years, 25 eyes in the 4 mg group received cataract surgery and 3 eyes in the 1 mg group received surgery compared to 0 in the observation group (P = .12 observation vs. 1 mg; P < .001 observation vs. 4 mg). As a result of this landmark study, intravitreal triamcinolone is generally accepted as a valid therapy for the treatment of macular edema in CRVO.
Periocular administration of triamcinolone acetonide may have fewer associated side effects when compared to intravitreal triamcinolone. A prospective, noncomparative study evaluated posterior sub-Tenon injection of 40 mg of triamcinolone acetonide given in three biweekly injections.11 Eighteen eyes with macular edema secondary to CRVO occurring within 4 weeks of presentation were treated. Improvement in visual acuity was not significant at 1 or at 3 months but was significant at 6 and 9 months. Nonischemic eyes benefited more than ischemic eyes from treatment. The authors found a gain of 10 or more letters in all 10 of the former, and in only 3 out of 8 of the latter. Only two patients required treatment of intraocular pressure with topical drops. However, due to the small number of patients and nonrandomized nature of this study, the results should be interpreted with caution.
Fluocinolone acetonide intravitreal implants (Retisert; Bausch and Lomb, Rochester, NY) for chronic macular edema due to CRVO were prospectively evaluated in 24 eyes.12 The device is surgically implanted through the pars plana and releases drug at a steady state over approximately 2.5 years. At 3 years after implantation, treated eyes showed a mean visual acuity gain of 3.4 letters and 50% of eyes showed at least a 10-letter gain. However, all treated eyes received cataract surgery and 9 eyes underwent treatment for glaucoma, 5 of which were treated surgically. To date, no phase 3 clinical trials have been initiated for Retisert as a treatment for CRVO and therefore it is not currently FDA approved for this indication.
Dexamethasone intravitreal implants (Ozurdex; Allergan, Irvine, CA) of 0.35 mg and 0.7 mg were evaluated over 6 months in 1,267 patients with macular edema associated with branch and central retinal vein occlusion.13 In the CRVO group, there was a significant improvement in visual acuity in eyes treated with either dose of dexamethasone implant at day 30, 60, and 90, but not at day 180. The improvement in visual acuity peaked at day 60 with a mean gain from baseline visual acuity of 10 letters for the 0.35 mg group and 9 for the 0.7 mg group compared to -0.5 for the control group. However, at day 180 the mean change in visual acuity was 2 letters for the 0.35 mg group, 0 for the 0.7 mg group, and -2 for the observation group. After 6 months, the study was continued for an additional 6 months with open label 0.7 mg implants given to 997 patients.14 Mean gain in visual acuity increased in both re-treatment and delayed treatment groups, peaking at 60 days following initiation of open label implant (8 months after start of initial trial) with an increase of 8 and 7 letters, respectively, but diminished at 6 months (12 months after start of initial trial) to a gain of 2.3 and -1 letters, respectively. Dexamethasone implants were associated with increased IOP, which generally resolved by 6 months after implantation, as well as increased incidence of cataracts with rates of 30% in the retreated 0.7 mg/0.7 mg group, 20% in the retreated 0.35 mg/0.7 mg group, and 10.5% in the sham/0.7 mg group (P < .001) at 12 months. While this study clearly demonstrated the need for repeated injections, its safety and efficacy data allowed Ozurdex to be FDA approved for the treatment of macular edema in retinal vein occlusions.
Anti-VEGF Agents
Eyes with CRVO have been shown to have intraretinal upregulation of VEGF, which is thought to contribute to macular edema and neovascularization.15 Several anti-VEGF agents have been evaluated for central retinal vein occlusions and are now considered by many to be the standard of care.
Pegaptanib (Macugen, OSI Pharmaceuticals, Northbrook, IL) is an RNA aptamer that binds VEGF-165, which is considered the primary isoform responsible for pathologic ocular neovascularization and vascular permeability.16 A randomized controlled trial of 33 patients treated with 0.3 mg pegaptanib, 1 mg pegaptanib, or sham treatment showed that at 1 week, pegaptanib treated patients had significantly decreased central retinal thickness (CRT) (-269 µm 0.3 mg group and -210 µm 1 mg group vs. -5 µm sham).17 At 30 weeks pegaptanib treated eyes had greater improvements in visual acuity with the 0.3 mg group gaining 7.1 letters (P = 0.09 vs. sham) and the 1 mg group gaining 9.9 letters (P = 0.02 vs. sham) compared to a loss of 3.2 letters in the sham group. No serious ocular or systemic events were reported. No larger randomized studies have been performed to date and pegaptanib is not currently FDA approved for retinal vein occlusions.
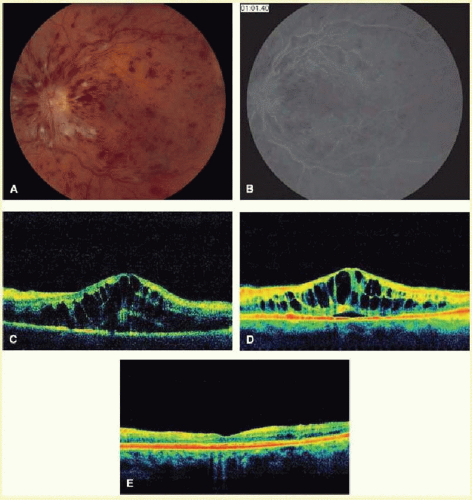
Bevacizumab (Avastin, Genentech, South San Francisco, CA) is a recombinant monoclonal antibody binding all isoforms of VEGF. While it was FDA approved for the treatment of colon cancer, it has been used in an off-label fashion as an intravitreal injection for several retinal conditions, including the treatment of CRVO. Several small noncontrolled studies have demonstrated that bevacizumab treatment of CRVO results in short-term improvements in visual acuity and decreased central retinal thickness (CRT)18,19,20,21 (Fig. 15A.1). Unfortunately, data is still quite limited with the majority of studies including less than 20 eyes. The longest study to date evaluated 10 patients initially treated with bevacizumab and followed for 2 years.23 Short term visual acuity gain was 14 letters at 3 weeks after initial injection, decreasing to an 8-letter gain at 2 years. There was no correlation between injection number, occlusion time, or macular edema changes with long-term visual gain.
Ranibizumab (Lucentis, Genentech, South San Francisco, CA), a humanized monoclonal antibody Fab fragment, is known to bind all isoforms of VEGF-A and is currently FDA approved for use in retinal vein occlusion within the United States. The Central Retinal Vein Occlusion Study (CRUISE) evaluated the safety and efficacy of monthly intraocular injections of 0.3 or 0.5 mg ranibizumab in 392 patients with macular edema following CRVO.22 At 6-months follow-up, the mean change from baseline best corrected visual acuity (BCVA) letter score was +12.7 for the 0.3 mg group, +14.9 for the 0.5 mg group, and 0.8 for the sham group. The median percent reduction in excess foveal thickness at 6 months was 94.0% for the 0.3 mg group, 97.3% for the 0.5 mg group, and 23.9% for the sham group. At 12 months, change from baseline BCVA letter score was +13.9, +13.9, and +7.3, respectively.23 The decreased foveal thickness in the treatment groups was maintained at 12 months. There was a small, but significant increase in cataract incidence at 12 months in the ranibizumab groups—3.8% (0.3 mg) and 7.0% (0.5 mg) versus 0% (sham). There was no significant difference in serious adverse events—ocular or nonocular—between the treatment groups.
Patients that completed the CRUISE trial were eligible for the HORIZON trial, which was a 12-month open-label, single-arm study of 0.5 mg ranibizumab.24 A total of 304 patients completed exams every 3 months and were given injections if they had recurrent macular edema that was deemed to affect the patient’s visual acuity or if the mean central subfield thickness was ≥ 250 µm. The mean number of treatments and mean change from baseline BCVA at month 12 was 2.0 injections and -4.2 letters for the sham/0.5 mg group, 2.4 injections and -5.2 letters for the 0.3/0.5 mg group, and 3.5 injections and -4.1 for the 0.5/0.5 mg group. No new safety events were identified. Loss of visual acuity despite treatment in year 2 showed that during the second year of ranibizumab treatment for CRVO, follow-up and injections should be individualized and may need to be more frequent than every 3 months in order to maintain the vision gains seen in the first year.
Aflibercept (Eylea, Regeneron, Tarrytown, NY) is a decoy receptor fusion protein consisting of the second domain of the human VEGF receptor 1 and the third domain of VEGF receptor 2 fused to the Fc domain of a human immunoglobulin,25 which has been shown to have substantially greater binding affinity for VEGF than either bevacizumab or ranibizumab and also binds placental growth factor.26 A randomized controlled trial of 189 eyes with CRVO treated with either 2 mg aflibercept every 4 weeks or sham showed that after 6 months of treatment, aflibercept patients had improved CRT (457.2 µm decrease vs. 144.8 µm decrease; P < .001) and visual acuity (mean gain of 17.3 letters vs. loss of 4.0 letters; P < .001) compared to the sham group.27 Serious ocular adverse events were reported in 3.5% of aflibercept patients compared to 13.5% of sham patients while serious nonocular adverse events were evenly distributed between the two groups. Based on these promising results, aflibercept is under evaluation by the FDA for the treatment of CRVO.
Interventions Targeting Venous Occlusion
Laser-induced Chorioretinal Anastomosis
Laser-induced chorioretinal anastomosis (L-CRA) uses a high-intensity argon laser to rupture Bruch’s membrane and the overlying retinal vein to allow an anastomosis to form, thereby bypassing the occlusion.28 A randomized controlled trial of L-CRA in 113 patients with nonischemic CRVO of at least 3 months duration and visual acuity of 20/50 or worse showed that the procedure did not significantly improve visual acuity at 18-month follow-up but was superior to no treatment, which resulted in a loss of nine letters of visual acuity.29 Complications of the procedure included neovascularization at the site of the L-CRA in 18% of subjects and macular traction or vitreous hemorrhage requiring vitrectomy surgery in 9.1% of patients.
Surgical Interventions
The results of surgical treatment for CRVO have been mixed. Radial optic neurotomy (RON), as proposed by Opremcak,30 was the first such procedure. The theory behind RON is to “decompress” the optic nerve to relieve the compartment-syndrome-like effect on the occluded central retinal vein at the level of the cribriform plate. A retrospective review of 11 cases of CRVO treated with RON showed promising results. All patients had visual acuity of 20/400 or less secondary to CRVO. After pars plana vitrectomy (PPV), a micro vitreoretinal blade was used to make a relaxing incision of the scleral ring, cribriform plate, and adjacent sclera to decompress the central retinal vein and theoretically allow reperfusion of the retina. Eight of the 11 patients in this study had rapid improvement of visual acuity by an average of five lines. All of the 11 patients had clinical improvement based on fundus appearance and fluorescein angiogram, whereas 9 had equal or improved postoperative visual acuity at an average follow-up of 9 months. Other studies have not shown the same level of improvement31,32 and it has been postulated that the beneficial effects of the surgery may be due to vitrectomy alone.33 Serious adverse effects including vitreous hemorrhage, retinal detachment, visual field defects, recurrent CRVO, and neovascularization have been reported.31,32,34,35,36 Consequently, the routine use of radial optic neurotomy is not currently recommended.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree