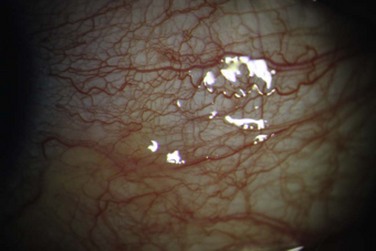
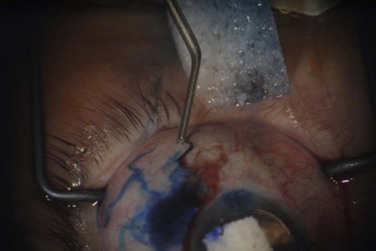
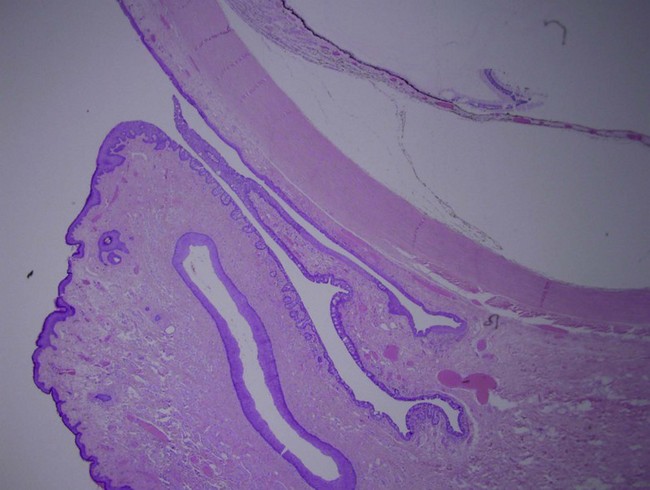
4 The conjunctiva is the mucosal surface that extends from the corneoscleral limbus to the eyelid margins and caruncle.1–4 Often overlooked, conjunctival tissue’s complex functions are necessary to maintain ocular surface homeostasis. Many important functions are performed by the conjunctiva including: (1) protection of the soft tissues of the orbit and the eyelid, (2) provision of the tear film’s aqueous and mucous layers, (3) supply of immune tissue, and (4) facilitation of independent globe movement. The conjunctiva can be divided into three distinct regions: bulbar, forniceal, and palpebral. The total surface area of the conjunctiva and cornea in an average adult measures approximately 16 cm2 per eye.2–4 The non-keratinized stratified secretory epithelium interfaces with a basement membrane and substantia propria below to create the blanket-like covering of the globe. Bulbar conjunctiva has a preponderance of cuboidal epithelial cells around goblet cells, Langerhans cells, melanocytes, and lymphocytes. In the normal bulbar conjunctiva, epithelial thickness can be more than six cell layers. Apical cell tight junctions, gap junctions, and desmosomes exist to create selective permeability, whereas the epithelial cell microvilli–glycocalyx complex encourages tear film adherence due to hydrophilicity.1–4 Mucous-secreting goblet cells constitute 5–10% of the conjunctival epithelial basal cells. The highest density of goblet cells occurs in the inferonasal bulbar conjunctiva and tarsal conjunctiva. Goblet cells are a likely apocrine in nature. Release of secretory granules results from parasympathetic activation.2,3 The underlying epithelial basement membrane is primarily composed of type IV collagen. The substantia propria, located beneath the epithelial basement membrane, is a highly vascularized, loose connective tissue. The substantia propria in the limbal conjunctiva is thin and compact.2–4 The bulbar conjunctiva is relatively loosely adherent to the underlying Tenon’s capsule. The conjunctiva and Tenon’s fascia are less mobile within the first few millimeters adjacent to the limbus, where the epithelium transitions to flatter epithelial cell morphology. Radiating infolds at the limbus are known as the palisades of Vogt. The stem cells of the cornea are located here.2,3 The dimensions of the bulbar conjunctiva vary with age, race, eye position, inherent redundancies of tissue and method of measurement. The adult chord length from limbus to fornix averages between approximately 13 and 16 mm superiorly. The inferior fornix is typically between 10 and 12 mm in normals and decreases with age. Cicatrizing conditions can create a foreshortened fornix, thereby decreasing the area of measurable bulbar conjunctiva.5 Temporally, the bulbar conjunctiva extends for more than 12 mm from the limbus and with a significant portion hidden by the lateral canthus. The nasal bulbar conjunctiva covers the smallest area, limited by the presence of the caruncle and the medial wall of the orbit.2 The vascular supply of the bulbar conjunctiva comes principally from anterior ciliary arteries and the peripheral tarsal arcades of the eyelid. The arteries eventually anastomose to create an arteriolar plexus near the limbus to ensure redundancy of oxygenation (Fig. 4.1). The majority of the blood supply for the bulbar conjunctiva near the limbus is derived from the anterior ciliary arteries. The venous drainage is similar: conjunctiva drains into anterior ciliary veins and into many peripheral conjunctival veins that connect to the eyelid’s venous plexus, before joining the superior and inferior ophthalmic veins. Bulbar conjunctival veins can become dilated and prominent along with those of the episclera in primary pulmonary hypertension, carotid cavernous fistulas, and other vascular malformations.2 The lymphatics of the nasal bulbar conjunctiva drain to the submandibular nodes. Temporal bulbar conjunctival lymphatics drain to preauricular nodes. Bulbar conjunctival lymphatic channels can be seen with injection of dyes at or near the limbus.2 The darker dye contrasts the lymphatic channel against the white background of sclera (Fig. 4.2). The ophthalmic branch of the trigeminal nerve contains sensory afferent fibers for the bulbar conjunctiva. Afferent nerves do not synapse until the fifth nerve nucleus. Autonomic efferent nerves supply vessels, accessory lacrimal glands, and the epithelia.2 The conjunctiva of the fornix is continuous with the skin and lies between bulbar and palpebral conjunctiva (Fig. 4.3). It contains a nonkeratinized stratified squamous epithelium that is typically three layers thick.2 The superficial layer is cylindrical, the middle layer is polyhedral, and the deep layer is cuboidal. Within the epithelium, goblet cells, melanocytes and dendritic cells are often encountered.
Conjunctival Anatomy and Physiology
Introduction
Anatomy and Histology
Fornix
![]()
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


Conjunctival Anatomy and Physiology