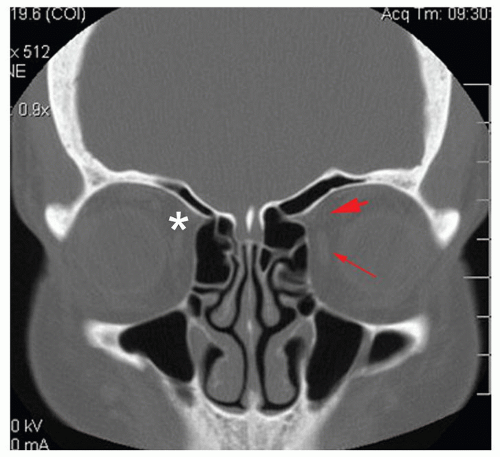
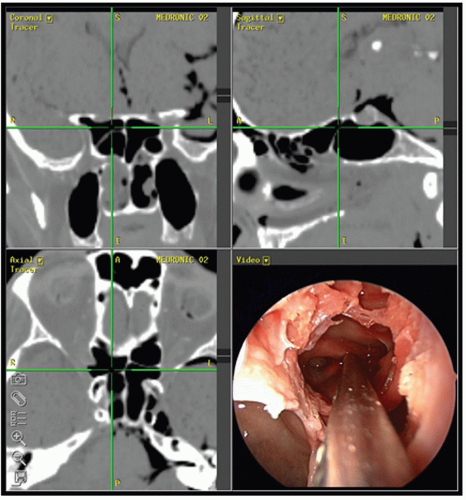
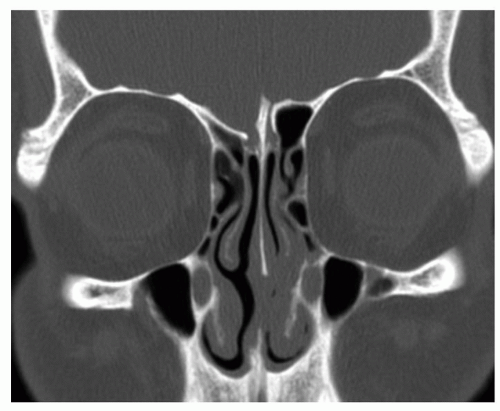
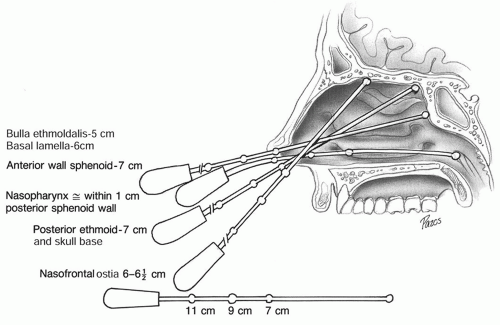
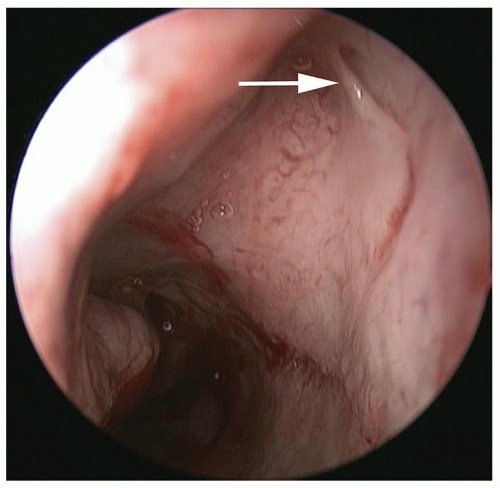
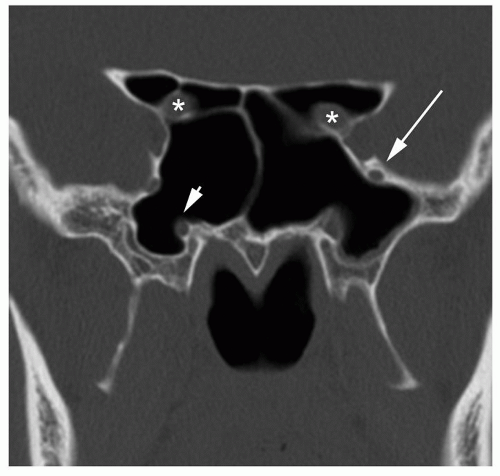
space contains fat and the infraorbital nerve and vessels. The medial extraconal space is the most relevant space in sinus surgery and contains a plethora of vascular structures: distal portions of the posterior ethmoidal artery, the distal portion of the ophthalmic artery, and the anterior ethmoidal artery as well as fat. Of extreme importance is the relationship of the ophthalmic artery and the anterior ethmoidal artery. The ophthalmic artery courses anteriorly in the extraconal space just inferior to the superior oblique muscle before giving rise to the anterior ethmoidal artery near the anterior ethmoidal foramen along the medial orbital wall. Radiographically, this is best identified in the coronal plane along the convergence of the medial rectus muscle and the superior oblique muscle (Fig. 44.1). In approximately 10% of cases, this neurovascular bundle can be suspended from the anterior ethmoid skull base in a bony mesentery, often associated with a supraorbital ethmoid air cell (1). Considering the limen nasi as a fixed landmark, the artery is located approximately 55 degrees from the nasal floor and at 50 mm.
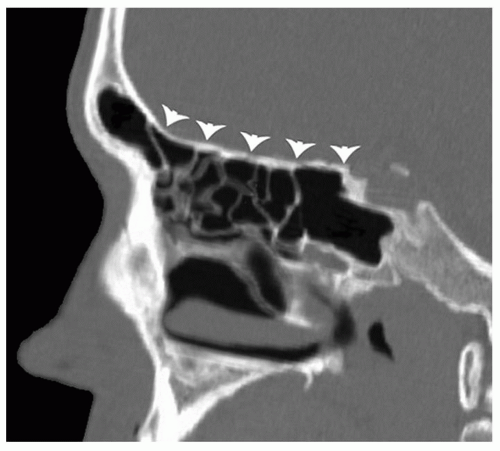
Two excellent articles relating to anatomic variations on CT scanning important to the sinus surgeon describe and enhance this anatomic discussion and are highly recommended (8,9). As the skull base transitions posteriorly to meet the planum sphenoidale, the ethmoid roof can be identified at the same level as the cribriform plate.
TABLE 44.1 SUMMARY OF IMPORTANT ANATOMIC RELATIONS | |
|---|---|
|
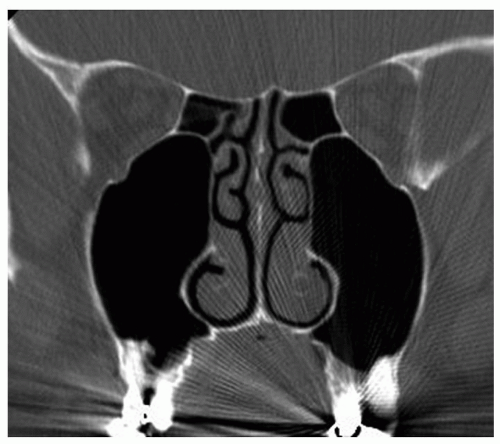
three-dimensional variance. The cribriform plate represents the lowest midline structure in the medial aspect of the nasal vault. The lateral mass of the ethmoid is suspended from the fovea ethmoidalis or ethmoid roof. Intervening between the ethmoid roof and cribriform plate is the lateral cribriform lamella, or simply lateral lamella. The length of the lateral lamella (and hence the depth of the cribriform plate) was noted by Keros (7) in several anatomic dissections. Keros classified the anterior skull base depth based upon the length of the lateral lamella: 1 to 3 mm (type I), 4 to 7 mm (type II), and 8 to 16 mm (type III). The skull base may also be asymmetric in design (Fig. 44.5). Some (10) have shown that type II anatomy is encountered most frequently and that patients with a lower skull base depth (i.e., type I) have a lower incidence of skull base injury.
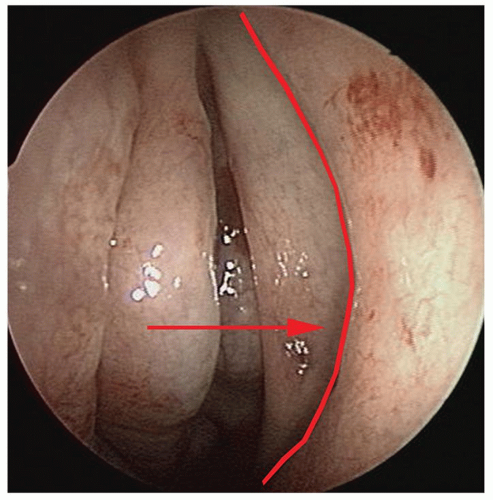
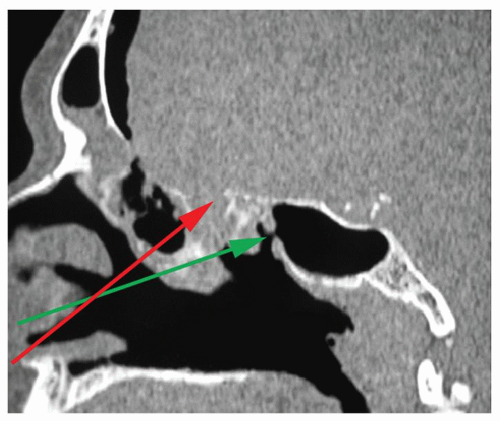
proceeding through the basal lamella if the patient has a 2:1 or greater than 2:1 ratio. Therefore, the surgeon must consider this “angle of attack” when penetrating the basal lamella and entering the posterior ethmoid cavity. Entering the posterior ethmoids via the medial-inferior aspect of the coronal face of the basal lamella, along the roof of the maxillary sinus or floor of the ethmoid bulla, will provide a much safer avenue toward the sphenoid sinus and away from the skull base (Fig. 44.8).
ethmoidectomy as “one of the easiest operations with which to kill a patient.” Most of the catastrophic complications are related to ethmoidectomy and frontal sinus surgery. Table 44.2 lists the complications of sinus surgery. May et al. (12) studied the complications of sinus surgery among large populations of patients noting CSF leak and blindness were the common major complications; orbital hematoma the most common minor complication.
TABLE 44.2 COMPLICATIONS SINUS SURGERY | ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| ||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||
respectively (13) and resolve within 1 to 2 weeks of the procedure. DeFreitas and Lucente (13) reviewed 670 Caldwell-Luc procedures and found a 9.1% and 3% incidence of facial paresthesias and dacryocystitis, respectively. Yarington (14) reported on 271 Caldwell-Luc procedures with a 3% overall complication rate. The most common complications were postoperative hypesthesia, devitalized teeth, and postoperative ethmoiditis. Blindness can occur with the Caldwell-Luc procedure if the orbit is entered, but this is a rare complication. DeFreitas and Lucente (13) also noted a recurrence of sinusitis and polyps in 12% and 5% of patients as well.
loss (average 384 mL) and an average hospitalization of 3.6 days. A total of 20.4% of patients had complications.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree