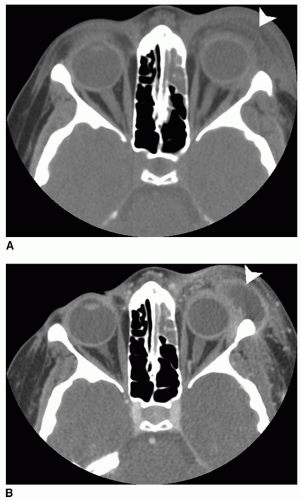
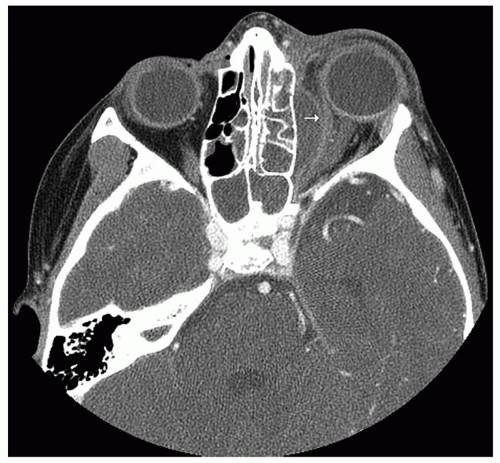
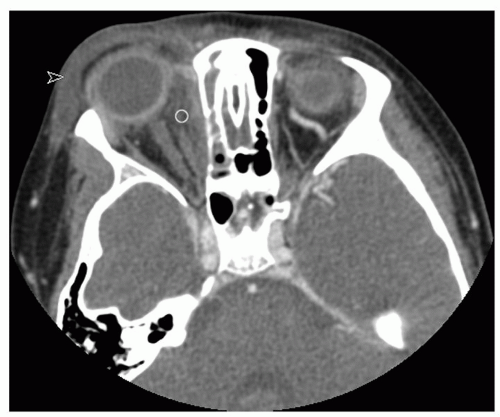
bites), or a foreign body (6,7). In contrast to other orbital complications, medical comorbidities such as cystic fibrosis, HIV, leukemia, diabetes, and other immune deficiencies are risk factors for preseptal cellulitis (7). Preseptal cellulitis manifests as eyelid swelling, erythema, and tenderness. Occasionally these may progress to an eyelid abscess (Fig. 38.2) and can also be associated with edema of the orbital (postseptal) contents. There are no limitations of extraocular movements and no impairment of visual acuity. Sinonasal infections cause periorbital swelling due to impaired venous drainage of the ethmoidal vessels that are obstructed by inflammation and pressure.
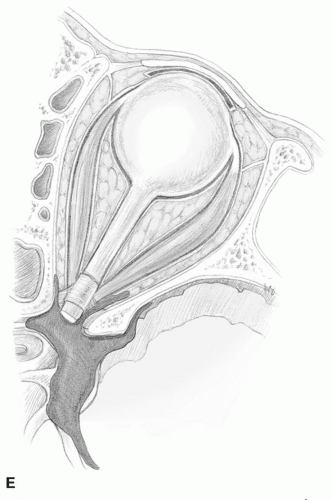
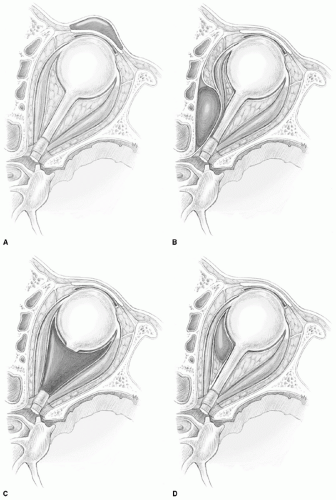 Figure 38.1 Chandler classification of orbital complications of sinusitis. A: Preseptal cellulitis (eyelid edema), (B) Subperiosteal abscess, (C) Orbital cellulitis, (D) Orbital abscess, |
TABLE 38.1 ORBITAL COMPLICATIONS OF SINUSITIS | |||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| |||||||||||||||||||||
indicating optic neuritis and/or ischemia can occur as the disease progresses; these are prognostically worrisome findings. Not all cases of orbital cellulitis are due to sinusitis, however. Patients presenting with pain and diplopia and a history of recent orbital trauma or dental surgery should be assessed for orbital cellulitis. In diabetic patients with ketoacidosis and immunocompromised patients, more severe infections such as invasive fungal sinusitis should be considered. Orbital cellulitis is more concerning than preseptal cellulitis because it can evolve into an orbital abscess.
in the orbit results in orbital pain, chemosis, proptosis, and ophthalmoplegia. Cranial nerves III, IV, V1, V2, V3, and VI traverse the sinus and can all be affected. Extension of the phlebitis posteriorly into the cavernous sinus results in progression of symptoms in the opposite eye. This contralateral involvement is a distinguishing feature of cavernous sinus thrombosis. It can be associated with sepsis and meningismus or frank meningitis may be present.
series (5,6,7,22) (Table 38.2). Less common but consistent causes of complicated sinusitis are S. pneumoniae, other Streptococci, and anaerobic microorganisms. H. influenza, Eikenella, and other gram-negative bacilli are also implicated in some cases of complicated sinusitis.
TABLE 38.2 MICROBIOLOGY OF SINUSITIS AND RELATED COMPLICATIONS | |||||||||
|---|---|---|---|---|---|---|---|---|---|
|