The use of cartilage in middle ear surgery is not a new concept and has been recommended on a limited basis to manage retraction pockets for many years.1,2 More recently, however, it has been increasingly described for the reconstruction of large portions of the pars tensa of the tympanic membrane (TM) in cases of recurrent perforation, atelectasis, and cholesteatoma.3,4 Although one might anticipate a significant conductive hearing loss with cartilage due to its thickness and rigidity, several studies have reported results to the contrary, suggesting hearing results with cartilage to be no different than those with fascia.3,4 The cartilage graft retains its rigid quality and resists resorption and retraction, even in the milieu of continuous Eustachian tube dysfunction.
Two distinct techniques are commonly employed for cartilage reconstruction of the TM: the perichondrium/cartilage island flap, which uses tragal cartilage; and the mosaic technique, which uses cartilage from the tragus or cymba. The choice of technique is typically dictated by the specific middle ear pathology or, in cases where the TM reconstruction is in conjunction with ossiculoplasty, the status of the ossicular chain. The mosaic technique is preferred in cases of cholesteatoma and when ossicular reconstruction is needed in the malleus-present situation. In this situation an exact fit is necessary to prevent cholesteatoma recurrence. The perichondrium/cartilage island flap is preferred for management of the atelectatic ear and the high-risk perforation. This chapter describes the two techniques in detail, followed by descriptions of the modifications that should be taken in response to specific surgical indications.
25.2 Patient Selection
Generally speaking, cartilage is used as a graft material in any ear considered to be at high risk for failure with traditional techniques utilizing temporalis fascia or perichondrium. Included in this would be the high-risk perforation, the atelectatic ear, and cholesteatoma. The high-risk perforation comprises a revision surgery, a perforation anterior to the annulus, a perforation draining at the time of surgery, a perforation >50%, or a bilateral perforation, all of which have been shown to be associated with increased failure rates using traditional techniques.5,6 The atelectatic ear is one of the most important indications for cartilage tympanoplasty, and numerous reports have established its efficacy over fascia in this situation.1,2 For similar reasons, the use of cartilage to reconstruct and reinforce the scutum and posterior half of the eardrum in cholesteatoma surgery has reduced the incidence of recurrent atrophy and retraction pockets in these difficult cases.
Cartilage tympanoplasty has proven to be efficacious in both pediatric and adult patients, with special precautions used in the former group. The general approach to pediatric patients is to avoid repairing the TM during the otitis-prone years (<3 years of age). If the contralateral ear is normal, routine tympanoplasty is performed at age 4 years.7 If the contralateral ear is abnormal at this time, adenoidectomy is considered, and tympanoplasty is generally deferred until age 7 years.8 If contralateral disease is still present at this time, cartilage tympanoplasty is performed on the worse-hearing ear because a perforation in the contralateral ear has been shown to be associated with a high risk for failure.9
As part of the preoperative preparation, all patients are encouraged to perform the Valsalva maneuver (or use the Otovent [Invotec International, Jacksonville, Florida] in younger children). Those unable to insufflate the ear are placed on nasal steroids 6 weeks prior to surgery, and these are continued in the postoperative period until an aerated middle ear cleft is documented. Although we have found no difference in graft take between those who can and cannot perform the Valsalva maneuver, we have found a slightly increased need (7%) for postoperative tube insertion in the Valsalva-negative group. Likewise, an attempt is made to optimize concomitant sinonasal disease (allergy, chronic sinusitis) prior to ear surgery, and smoking cessation is encouraged where applicable. The draining ear is treated with antibiotic/steroid-containing topical solutions and aural toilet for 6–8 weeks prior to surgery. While every attempt is made to dry an ear prior to surgical intervention, it is not considered a prerequisite for tympanoplasty.
25.3 Surgical Technique
25.3.1 General Considerations
The surgical approach for cartilage tympanoplasty does not differ from that for traditional otologic surgery and is dictated by the extent and location of the disease. The postauricular approach is utilized in most patients as these cases, by definition, tend to have more extensive middle ear pathology. A small, localized, posterior retraction or perforation can be performed through a transcanal or endaural incision, but great care must be taken to assure that the depths of the retraction can be reached. Likewise, the placement of the cartilage graft utilizes the underlay technique, so that no special tympanomeatal flaps or skin incisions are required.
Some general observations should be made regarding the differences in cartilage that occur with aging. The cartilage thickness of the tragus and cymba are not appreciably different between children and adult patients, but the perichondrium seems to be more adherent in children. For this reason, when the perichondrium is removed from one side when fashioning the graft (described below), care must be taken to ensure the correct plain is dissected, especially in the pediatric patient. Likewise, cartilage is more pliable in children, making it slightly easier to work with than adult cartilage, which can become somewhat brittle in patients over 65 years of age. For this reason, during the fashioning of the graft, it is generally a good practice to manipulate and hold the cartilage with fingers instead of forceps, and toothed-forceps should not be used at any time to grasp the cartilage to avoid fracture.
As a general rule, the perichondrium is left attached to the side of the cartilage that faces the ear canal, regardless of which technique is used. It is believed that the perichondrium improves graft stability and facilitates the ingrowth of fibrous tissue and epithelialization. It should be noted, however, that with the mosaic technique, perichondrium has been removed from both sides of the cartilage on occasion due to untoward curling of the graft, which will typically curve toward the side with the perichondrium. No ill effect has been noted, other than increased fragility of the graft during formation and placement.
25.3.2 The Perichondrium/Cartilage Island Flap
The general technique of reconstruction using the perichondrium/cartilage island flap begins with harvest of the cartilage from the tragal area.10 This cartilage is ideal because it is thin, flat, and in sufficient quantities to permit reconstruction of the entire TM. The cartilage is used as a full-thickness graft and is typically slightly less than 1 mm thick in most cases. Although it has been suggested that a slight acoustical benefit could be obtained by thinning the cartilage to 0.5 mm,11 this advantage is offset by the unacceptable curling of the graft, which occurs when the cartilage is thinned and perichondrium is left attached to one side.
An initial cut through skin and cartilage is made on the medial side of the tragus, leaving a 2-mm strip of cartilage in the dome of the tragus for cosmesis (▶ Fig. 25.1). The cartilage, with attached perichondrium, is dissected medially from the overlying skin and soft tissue by spreading a pair of sharp scissors in a plane that is easily developed superficial to the perichondrium on both sides. It is necessary to make an inferior cut as low as possible to maximize the length of harvested cartilage. The cartilage is then grasped and retracted inferiorly, which delivers the superior portion from the incisura area. The superior portion is then dissected out while retracting, which produces a piece of cartilage typically measuring 15 mm x 10 mm in children and somewhat larger in adults.
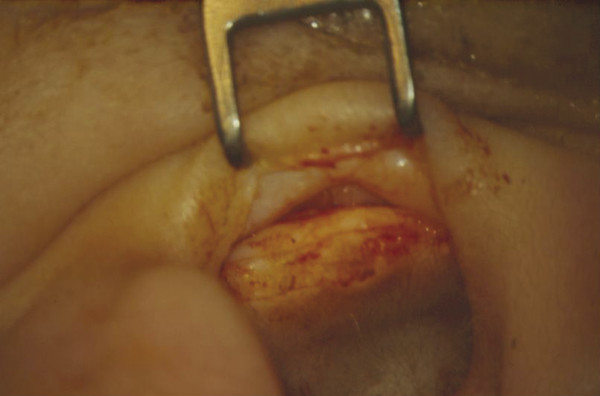
Fig. 25.1 Harvest of cartilage, leaving small rim of cartilage in dome for cosmesis (right ear).
Used with permission from Dornhoffer JL. Cartilage tympanoplasty: indications, techniques, and outcomes in a 1000-patient series. Laryngoscope 2003;113:1844–1856.
The perichondrium from the side of the cartilage furthest from the ear canal is dissected off, leaving the thinner perichondrium on the reverse side. A perichondrium/cartilage island flap is then constructed in the following manner.10 Using a round knife, cartilage is dissected from the graft to produce an eccentrically located disc, approximately 7–9 mm in diameter, that will be used for total TM reconstruction. A flap of perichondrium is produced posteriorly that will eventually drape over the posterior canal wall. A complete strip of cartilage 2 mm in width is then removed vertically from the center of the graft to accommodate the entire malleus handle (▶ Fig. 25.2). The creation of two cartilage islands in this manner is essential to enable the reconstructed TM to bend and conform to the normal conical shape of the TM. When the ossicular chain is intact, an additional triangular piece of cartilage is removed from the posterior-superior quadrant to accommodate the incus. This excision prevents the lateral displacement of the posterior portion of the cartilage graft that sometimes occurs because of insufficient space between the malleus and incus.
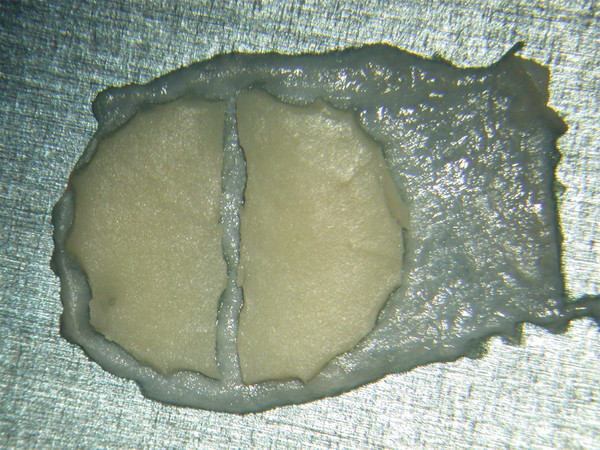
Fig. 25.2 Prepared perichondrium/cartilage island graft, showing strip of cartilage removed to facilitate malleus.
Used with permission from Dornhoffer JL. Cartilage tympanoplasty: indications, techniques, and outcomes in a 1000-patient series. Laryngoscope 2003;113:1844–1856.)
The entire graft is placed in an underlay fashion, with the malleus fitting in the groove and actually pressing down into and conforming to the perichondrium, as shown in ▶ Fig. 25.3. The cartilage is placed toward the promontory, with the perichondrium immediately adjacent to the TM remnant, both of which are medial to the malleus. Failure to remove enough cartilage from the center strip will cause the graft to fold up at the center instead of lying flat in the desired position. Likewise, if the strip is insufficient, the cartilage may be displaced medially instead of assuming a more lateral position in the same plane as the malleus.
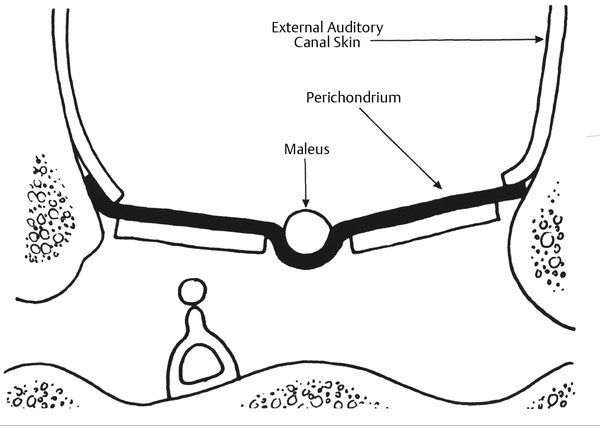
Fig. 25.3 Lateral line drawing demonstrating proper placement of graft.
Used with permission from Dornhoffer JL. Cartilage tympanoplasty: indications, techniques, and outcomes in a 1000-patient series. Laryngoscope 2003;113:1844–1856.
Gelfoam (Upjohn Laboratories, Kalamazoo, Michigan) is packed in the middle ear space underneath the anterior annulus to support the graft in this area, and the posterior flap of perichondrium is draped over the posterior canal wall. Middle ear packing is avoided on the promontory and in the vicinity of the ossicular chain. One piece of Gelfoam is placed lateral to the reconstructed TM, and antibiotic ointment is placed in the ear canal (▶ Fig. 25.4).
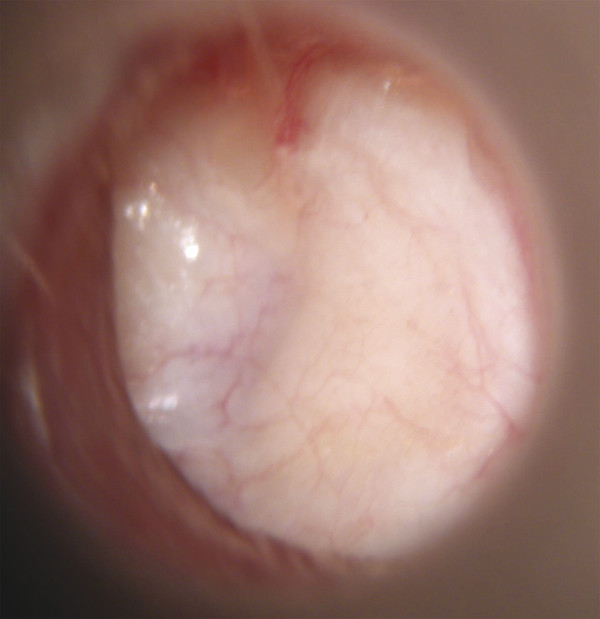
Fig. 25.4 Postoperative ear with perichondrium/cartilage island graft (left ear).
Used with permission from Dornhoffer JL. Cartilage tympanoplasty: indications, techniques, and outcomes in a 1000-patient series. Laryngoscope 2003;113:1844–1856.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


