Bacterial Corneal Ulcers
Richard L. Abbott
Colleen P. Halfpenny
Michael Zegans
Paul A. Kremer
Ulceration of the cornea may be either infectious or sterile and requires immediate intervention to prevent complications. Widespread use of contact lenses and the increasing number of refractive corneal surgical procedures require ophthalmologists to be well versed in the diagnosis and treatment of bacterial keratitis. The accurate determination of an infectious agent and management of the ulceration can be among the most challenging of clinical problems. The causative organisms, laboratory diagnosis, therapeutic approach, and major antibiotics are reviewed.
Pathogenesis
Numerous micro-organisms on the lid margin and in the normal uninfected conjunctival sac provide a constant source of potentially pathogenic bacteria to the cornea.1 The ability of the cornea to prevent invasion by most bacteria depends on an intact epithelial surface and a normal tear flow. Any impairment in the integrity of these natural barriers may permit entrance of micro-organisms and produce ulceration.
The smooth surface of the cornea offers some protection from infection by combining the action of tears and blinking to mechanically remove organisms from the surface. In addition, lysozymes, beta lysins, and antibodies in the tears exert antibacterial action. Most cases of bacterial keratitis result from a disruption in the corneal epithelium. There are many compromising factors that can adversely affect the integrity of the corneal epithelium and tear film, causing breakdown and secondary infection (Table 18.1).1,2,3,4,5,6,7,8,9
TABLE 18.1 Predisposing Condition to Bacterial Keratitis | |
|---|---|
|
The association between contact lens wear and infectious ulcerative keratitis has been well documented.10,11,12,13,14,15 A 38-year study of the incidence of ulcerative keratitis in Olstead County, Minnesota, found contact lens wear to be a predisposing factor in 56% of patients.16 This was followed by ocular trauma, which was a predisposing factor in 25% of patients. Extended-wear contact lens regimens have been associated with an increased risk of developing ulcerative keratitis compared with daily-wear regimens.17,18 The risk of ulcerative keratitis appears to be directly related to the extent of overnight wear.19 Disposable contact lenses used on an extended-wear basis may not provide significant protection against the development of corneal ulcers compared with conventional extended-wear lenses.20,21,22 Annual risks of ulcerative keratitis in cosmetic contact lens wearers have been estimated to be 13.3 to 20.9 cases per 10,000 for extended soft contact lens wear; 2.2 to 4.1 cases per 10,000 for daily soft contact lens wear; and 2 cases per 10,000 for rigid gas-permeable lens wear.23
Certain organisms, such as Neisseria gonorrhoeae, Listeria, Corynebacterium, and Haemophilus aegypticus may invade directly through intact corneal epithelium. These bacteria must first adhere to the epithelium or stroma before they can initiate penetration and infection.24,25 This biological adhesion allows diffusion of toxins and bacterial by-products necessary to facilitate actual entrance of the bacteria into the stroma.26
Once bacteria have invaded the corneal stroma, the host response is initiated by the polymorphonuclear leukocyte (PMN). The PMN phagocytoses the bacteria and, by means of intracytoplasmic lysosomes, destroys the organism.3 Although the enzymes produced by the PMNs help destroy the invading bacteria, they also produce toxic metabolites, which may contribute to progressive corneal destruction.
Causative Organisms
Most of the organisms cultured from corneal infections are of the same species that are normally found on the lids and periocular skin, in the conjunctival sac, or in adjacent nasal passages.1 The spectrum of micro-organisms that produce bacterial corneal infection is influenced by pre-existing disease or injury and the severity of any other compromising factors (Table 18.2).2,7 Although regional variations within the United States may exist, the most common organisms cultured from bacterial ulcers in the uncompromised, healthy cornea are Staphylococcus, Streptococcus, Pseudomonas, Enterobacteriaceae, Moraxella species, and Klebsiella pneumoniae.4,27 Pseudomonas has been reported to be the bacteria most commonly isolated from contact lens–associated corneal ulcers. In the compromised cornea, normally harmless bacteria can become opportunistic pathogens and may produce infected corneal ulcers. The most common organisms in this group are Staphylococcus aureus, the coagulase-negative staphylococci, alpha-hemolytic streptococcus, beta-hemolytic streptococcus, Pseudomonas, and Proteus.4,27 Ulcers in the pediatric age group are most commonly caused by Pseudomonas, Staphylococcus, and fungi.1,28 Among patients with AIDS, fungal ulcers also appear to be more common.29 Streptococcus pneumoniae seems to be a particularly important cause of bacterial keratitis in the developing world, where contact lens–associated corneal ulceration represents a smaller portion of cases of bacterial keratitis. In a large study of Indian patients with corneal ulceration, S. pneumoniae was the most commonly isolated bacterial pathogen.30
TABLE 18.2 Organisms Commonly Isolated From Corneal Ulcers | |||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
The severity of corneal infection usually depends on the underlying condition of the cornea and the pathogenicity of the infecting organism. Toxins produced by some organisms facilitate infection through cytotoxic destruction of the cell membrane or by inhibiting cellular protein synthesis.3 An understanding of the characteristics and pathogenicity of bacteria commonly known to cause infectious keratitis is helpful in the treatment of these infections.
The more common bacteria isolated from bacterial corneal ulcers, their clinical characteristics, and the laboratory techniques used in their identification are presented.
Gram-Positive Cocci
Staphylococci
Staphylococci are among the most common bacteria encountered in ocular infections. S. aureus (coagulase-positive staphylococcus) is generally considered to be a pathogenic organism. The coagulase-negative staphylococci include Staphylococcus epidermidis, which is believed to be part of the normal body flora. There are at least 14 other species of coagulase-negative staphylococci that are rarely associated with infectious keratitis.31
During microscopic examination, staphylococci almost always appear gram positive, are spherical with a mean diameter of approximately 1 mm, and are seen extracellularly. Old cultures or scrapings from antibiotic-treated cases may show gram-negative staining characteristics. Although grapelike clusters are frequently seen in scrapings or smears from nonocular tissues, these are unusual in scrapings from corneal ulcers, in which single cocci or clusters of two to six cocci are observed. Two species, S. epidermidis and S. aureus, cannot be distinguished by Gram stain; however, they show distinct characteristics in culture. In general, the staphylococci are easily cultured on standard bacteriologic media (see Laboratory Diagnosis section) and grow rapidly in incubation at 37°C. They do not have a distinctive odor and grow in the presence or absence of oxygen. Typical colonies are round, flat, smooth, and several millimeters in diameter by 48 hours (Fig. 18.1). S. aureus colonies show beta hemolysis (clear zones of hemolysis on blood agar) and some degree of pigmentation (light cream to golden yellow). In contrast, S. epidermidis colonies are usually nonhemolytic and rarely exhibit pigmentation.
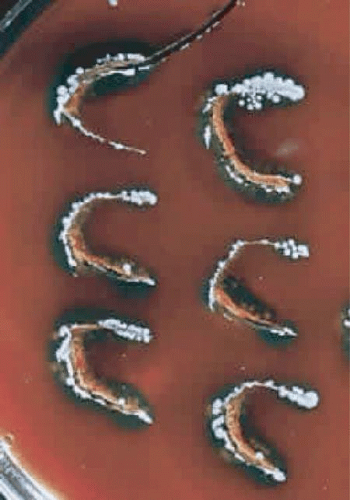 Figure 18.1 Typical colonies of Staphylococcus aureus growing on “C” streaks placed on blood agar at 37°C. Note the round, flat, smooth appearance of the colonies. |
Because S. epidermidis is often a nonpathogenic component of normal conjunctival and eyelid flora, it is important to differentiate it from the often pathogenic S. aureus. The usual approach is to perform a catalase test, which is positive for staphylococcus but negative for streptococcus. This is followed by a coagulase test, which is positive for S. aureus and negative for S. epidermidis. Typing of S. aureus strains has indicated that the vast majority of S. aureus infections are caused by organisms normally carried by the patient.32,33 With the emergence of methicillin-resistant S. aureus (MRSA), antibiotic susceptibility testing of corneal S. aureus isolates has become essential. MRSA should be suspected in hospitalized patients. Since the late 1990s, however, MRSA infections occurring in the community among healthy persons, especially children, are becoming prevalent. These community-acquired strains demonstrate faster growth rates but have broader antimicrobial susceptibility.34 If MRSA infection is discovered, consultation with an infectious disease specialist or hospital epidemiologist may be warranted in order to determine whether the patient is a carrier of MRSA so that appropriate treatment may be initiated.
S. aureus and the coagulase-negative staphylococci produce corneal ulcerations that may appear similar; however, those caused by S. aureus are in general more severe and are associated with more complications. The production of extracellular proteins and enzymes by S. aureus helps facilitate the spread of infection by combating host defense mechanisms and destroying healthy corneal tissue.1 A staphylococcal ulcer may present as either a central, infected ulcer or a marginal, toxic (allergic) ulcer. Most commonly, S. aureus is the responsible organism; however, coagulase-negative staphylococci may be causative agents in eyes with prior corneal disease such as bullous keratopathy or herpes simplex, or with prolonged wearing of a bandage contact lens.27
Clinically, the infected staphylococcal corneal ulcer presents with a yellow-white, well-demarcated area of infiltrate, which appears directly beneath an epithelial defect (Fig. 18.2). On occasion, multiple, small satellite lesions may develop. The infection may initially be superficial; however, if inadequately treated, it can produce a mid- to deep stromal abscess that may eventually lead to perforation. Stromal edema and white blood cell migration frequently surround the dense infiltrate and clear as the infection comes under control. Although there may be a marked anterior chamber reaction with hypopyon, the ulcer more frequently is indolent, with only a minimal inflammatory reaction.35
The more peripheral marginal infiltrate is sterile and is caused by a hypersensitivity reaction to the exotoxin or the bacterial antigens of S. aureus.36,37 The peripheral infiltrates are usually associated with blepharitis or conjunctivitis and frequently begin in the areas where the lid margins cross the limbus (at 2-, 4-, 8-, and 10-o’clock positions). The lesions often have a typical clinical appearance characterized by one or more small, well-circumscribed anterior stromal infiltrates, with a lucid interval between them and the limbus (Fig. 18.3). Although the epithelium is usually intact, it may break down, leading to ulceration, scarring, and neovascularization.
Streptococci
The streptococci consist of a diverse collection of organisms that have been classified into many different groups based on antigenic properties, types of hemolysis, and growth characteristics.31 The most common of these organisms, cultured from infected corneal ulcers, are Streptococcus pneumoniae (pneumococcus), Streptococcus viridans (alpha-hemolytic streptococcus), Streptococcus pyogenes (beta-hemolytic streptococcus), and the group D streptococci Streptococcus faecalis (nonhemolytic streptococcus).
Although S. pneumoniae was once the most common cause of bacterial keratitis, it has been surpassed by Staphylococcus and Pseudomonas7,8 in the United States. However, S. pneumoniae remains the most common cause of bacterial keratitis in the developing world.30 S. viridans ulcers occur more frequently than those caused by the more virulent S. pyogenes, presumably because the former may be part of the normal flora of the upper respiratory tract. The less common Enterococcus faecalis (enterococcus) corneal infections have been reported in either immunosuppressed hosts or after epithelial corneal injury and direct transmission from the gastrointestinal tract.25 E. faecalis is the third leading cause of nosocomial infection in the United States, and recently, cases of vancomycin-resistant enterococcus have been reported.38,39
The microscopic appearance of all streptococci, except for pneumococcus, is similar. Smears taken from culture material show gram-positive cocci in chains of varying lengths. Scrapings taken directly from infected ocular tissues may not demonstrate the chain effect, and differentiation from staphylococci may be difficult (Fig. 18.4). The morphologic characteristics of the Staphylococcus and Streptococcus organisms are outlined in Table 18.3.
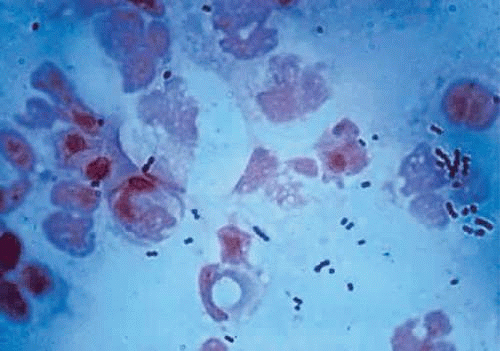 Figure 18.4 Gram-stained smear of Streptococcus organisms from a corneal ulcer. Note the fragmentation of the chains into smaller lengths, making differentiation from Staphylococcus difficult. |
TABLE 18.3 Morphologic Characteristics of Staphylococcus and Nonpneumococcal Streptococcus on Gram-Stained Smear | ||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
The Gram stain of S. pneumoniae differs from that of other Streptococcus organisms by the presence of a polysaccharide capsule surrounding the lancet-shaped diplococci. Streptococci grow best on blood agar or nutritionally enriched media such as brain-heart infusion medium. Identification of the different species is aided by the hemolytic nature of the organism. With alpha hemolysis, the red blood cells are not completely lysed, and a green color change is observed in the surrounding blood agar. With beta hemolysis, there is complete lysis of the red blood cells in the agar surrounding the Streptococcus colony. In general, the colonies of Streptococcus are elevated but quite small and measure between 1 and 2 mm in diameter. The pneumococci produce alpha hemolysis and may be differentiated in culture from S. viridans by the nonelevated, pitted appearance of the pneumococcal colony at 48 hours. In addition, the pneumococci produce capsules that impart a more translucent appearance to the colony.
Because the 24-hour culture of pneumococci may be easily confused with that of S. viridans (alpha-hemolytic streptococcus), laboratory tests are needed to make a definitive identification. Optochin susceptibility and bile solubility suggest S. pneumoniae.
Because all streptococci are fermentative organisms and lack the enzyme catalase, this characteristic may be used to help differentiate the nonhemolytic streptococci from similar-appearing colonies of Staphylococcus. The catalase test is useful in quickly determining whether a colony is a Streptococcus.
Although S. pneumoniae is an inhabitant of the upper respiratory tract in approximately 50% of normal human adults, it is also frequently found in the conjunctiva and lacrimal drainage apparatus. This close anatomic proximity to the cornea provides a source of organisms for possible infection. Any minor corneal trauma associated with disruption in the epithelium may lead to rapid invasion by this organism. The virulence of the S. pneumoniae organism is influenced by its polysaccharide capsule, which is serologically specific for more than 80 serotypes.4 Ocular isolates of these infections, however, do not seem to be caused by any particular pneumococcal serotype.40
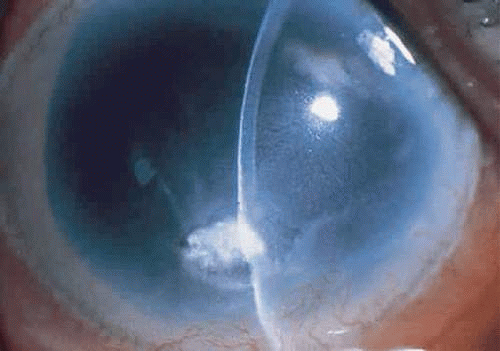
Corneal ulcers caused by S. pneumoniae are typically described as serpiginous or creeping and most often spread toward the center of the cornea. They are characterized by a gray-yellow disc-shaped ulcer with an overhanging margin at the advancing edge (Fig. 18.5). The ulcer usually progresses rapidly, extending into the deep stroma and often leading to corneal perforation. Extensive damage to corneal tissue, as well as a characteristic sterile hypopyon, are caused by the rapid production of bacterial exotoxin within the stroma.41,42
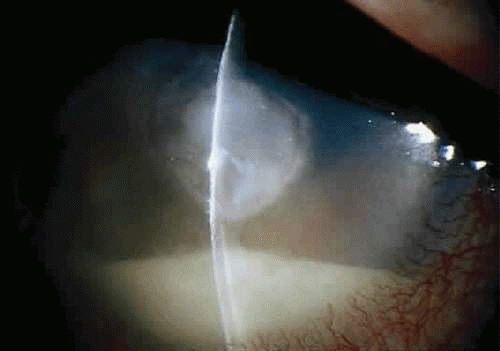 Figure 18.5 Large, disk-shaped corneal ulcer caused by Streptococcus pneumoniae in an elderly woman. The presence of a sterile hypopyon is often associated with these ulcers. |
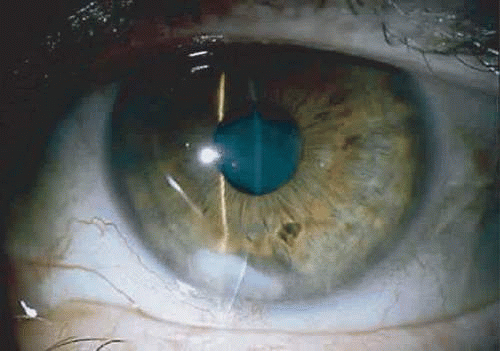
S. viridans (alpha streptococcus), although of low-grade pathogenicity, may be a cause of corneal ulceration, particularly in the locally immunosuppressed host.43 The organism produces a characteristically indolent, anterior stromal inflammatory reaction that is slow to progress and that may be accompanied by a minimal to moderate anterior chamber reaction. The ulcer is usually well-circumscribed, gray-white, “dry” in appearance, and lying beneath a well-demarcated epithelial defect (Fig. 18.6). Because the organism is of relatively low-grade pathogenicity, the infection responds rapidly to specific antibiotic therapy.
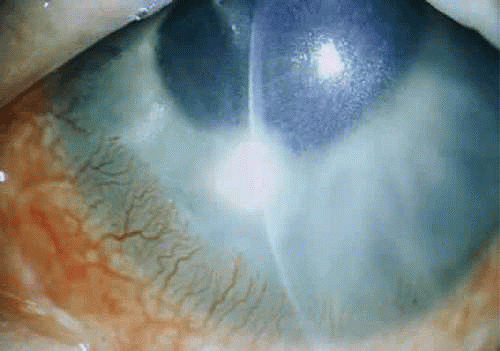 Figure 18.6 Streptococcus viridans corneal ulcer in a young woman wearing cosmetic soft contact lenses. The ulcer is well defined and dry in appearance with only a minimal anterior chamber reaction. |
Infectious crystalline keratopathy is most commonly associated with S. viridans infection.44,45,46 This keratitis is characterized by discrete, white, crystalline, or fernlike stromal opacities, often under an intact epithelium, that are slowly progressive and have little associated corneal inflammation (Fig. 18.7). There is a strong association with prior topical corticosteroid therapy or penetrating keratoplasty. The condition has been termed infectious crystalline keratopathy and has also been reported with other organisms, including Haemophilus aphrophilus, Peptostreptococcus, and S. epidermidis, as well as the fungal infections Alternaria and Candida tropicalis.47,48,49,50
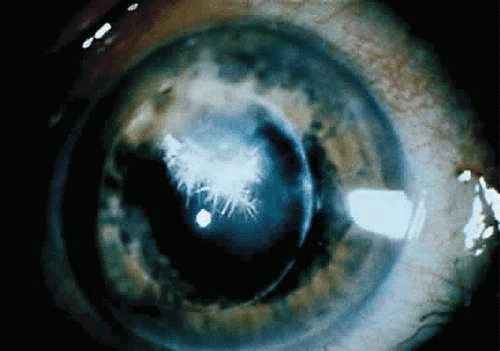 Figure 18.7 Infectious crystalline keratopathy caused by Streptococcus viridans. This infiltrate typically is slowly progressive, with little associated corneal inflammation. |
A corneal biopsy may be necessary to gain access to the “crystalline” infiltrates for identification and culture of organisms. This may be accomplished using a disposable 2-mm dermatologic biopsy punch. These infections may be extremely resistant to therapy, requiring an extended course of antibiotics.
S. pyogenes (group A Streptococcus), although an important pathogen in other areas of medicine, is an infrequent cause of corneal infection. Marginal corneal ulcers associated with dacryocystitis have been reported with this organism.51 These marginal ulcers appear similar to the catarrhal ulcers associated with staphylococcal blepharitis. They may result from either a hypersensitivity or toxic response to the organism or from direct infection of the cornea.51
Enterococcus, a common organism found in the gastrointestinal tract, may produce a corneal ulcer in the presence of severely impaired host resistance or after epithelial injury. The organism produces a rapid and severe inflammatory response that can be devastating to the eye.
Other Gram-Positive Organisms
Less common causes of infectious ulcerative keratitis that are classified as gram-positive organisms include the aerobic, spore-forming bacilli Bacillus coagulans and Bacillus brevis,52 as well as the non–spore-forming bacillus Corynebacterium diphtheriae.52 Bacillus infections of the cornea are associated with prior injury and produce severe local tissue damage. C. diphtheriae corneal ulceration is a rare complication of conjunctivitis and can progress rapidly to perforation within 24 hours. The mechanism responsible for the rapid and massive dissolution of the cornea is presumably related to diphtheria toxin.53
Peptostreptococcus, an anaerobic gram-positive coccus, may produce a corneal ulcer after injury to the cornea.54 Other rare causes of virulent corneal ulcers include the anaerobic spore-forming bacilli Clostridium perfringens and Clostridium tetani and the anaerobic non–spore-forming bacilli Actinomyces species and Propionibacterium acnes.55 Mixed aerobic and anaerobic bacterial infections may also occur and are frequently misdiagnosed and difficult to treat.
Other infrequent bacterial agents causing corneal ulcers include the nontuberculous mycobacteria56,57 and Nocardia species.3,4 These organisms are similar in appearance on scrapings and cultures, and usually require 3 to 5 days to grow on blood agar. Stained smears show gram-positive, slender rods that are variable in size. Mycobacterial ulcers occur after foreign body or surgical trauma.57 They are best isolated in Lowenstein-Jensen medium and require an aerobic atmosphere with an increased amount of carbon dioxide. Nocardia species are obligate aerobes and are best isolated on blood or Sabouraud’s agar. Clinically, corneal ulcers caused by these organisms are indolent, progressing slowly for weeks to months, and are often recalcitrant to treatment.
Gram-Negative Rods
Pseudomonas
Pseudomonas is a gram-negative rod that is ubiquitous in our environment and is a common cause of bacterial keratitis. The organism is a slender rod with parallel sides and rounded ends. There are 30 species within the genus; however, Pseudomonas aeruginosa is by far the one that is most often implicated in keratitis. Xanthomas Pseudomonas maltophilia and Pseudomonas cepacia are also well recognized corneal pathogens; Pseudomonas stutzeri and Pseudomonas acidovorans are blamed more rarely.58 The members of this genus are usually free-living bacteria and are considered opportunistic pathogens.
P. aeruginosa is easily seen on Gram stain, although there tends to be a paucity of organisms (Fig. 18.8), in contrast to pneumococcal ulcers (Fig. 18.4). The organism is easily grown on a variety of substances and can tolerate a wide temperature range, but is an obligate aerobe. The oxidase test is positive early in almost all pseudomonas infections and can be helpful for rapid identification. P. aeruginosa has a distinctive “fruity” odor, is extremely active and motile on wet mounts, and elaborates two pigments (fluorescein and pyocyanin) with a striking blue-green color.
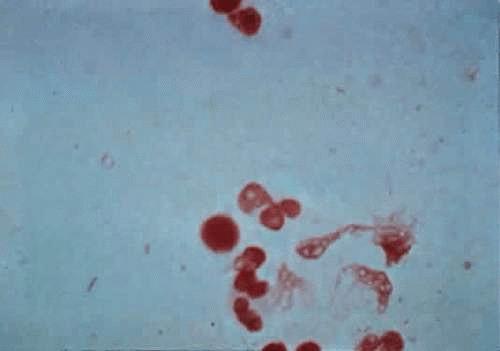 Figure 18.8 Gram-stained smear of Pseudomonas organisms (arrows). Typically, there is a paucity of organisms present, and care must be taken to identify the slender gram-negative rods. |
It has been demonstrated experimentally in mice that corneal injury is often a predisposing cause of Pseudomonas keratitis because it allows bacteria to adhere to damaged epithelial cells and exposed stroma.24,59 Considerable biochemical and experimental evidence indicates that Pseudomonas can elaborate an extracellular protease (not a collagenase as suggested in early reports60) capable of destroying the corneal stroma.61,62,63 Several investigators have also demonstrated the ability of P. aeruginosa to produce exotoxin-A, which can inhibit protein synthesis and is similar to diphtheria toxin.64,65 The exotoxin is capable, when injected intrastromally into rabbit corneas, of producing loss of epithelium, endothelium, keratocytes, and opacification of the cornea.66 This effect is dose related and can be completely neutralized with a specific antitoxin. This evidence helps explain why Pseudomonas corneal ulcers are potentially so devastating and destructive even after the active replicating bacteria have been killed with antibiotics.
Of the gram-negative bacteria that cause keratitis in the United States, Pseudomonas is the most common, and in some areas, such as Miami, it is the most common cause of corneal ulcers.7 These infections have commonly been traced to contaminated eye makeup,67,68 fluorescein solutions,69 and contact lens cases.10 They have also been associated with abnormal epithelium such as occurs with bullous keratopathy and after herpes simplex keratitis.26 P. aeruginosa corneal ulcers have often been seen in patients using daily-wear contact lenses,11,12 extended-wear cosmetic lenses,12,14,15 and aphakic extended-wear lenses.11,15 Less common infective sources include the patient’s own sputum and tracheostomy sites.70,71
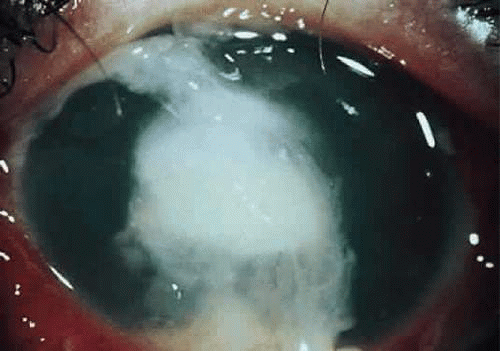
Clinically, a bacterial corneal ulcer caused by P. aeruginosa evolves quite rapidly and involves large areas of the cornea. It is frequently seen in a debilitated, elderly patient, and especially in those wearing extended-wear aphakic contact lenses.11,15 It generally begins centrally with a gray infiltrate that has an overlying epithelial defect. The adjacent cornea often has a hazy appearance secondary to epithelial and stromal edema. The ulcer commonly has a yellow green discharge and a “soupy” appearance (Fig. 18.9). The discharge contains both fluorescein and pyocyanin pigments and fluoresces with Wood’s lamp (but not with the cobalt blue light of the slit lamp biomicroscope).72
Ring abscesses can occur and may represent antigen-antibody reactions to exotoxin or other substances.73 A large, sterile hypopyon is frequently present and should not be mistaken for endophthalmitis. The infection spreads rapidly in all directions without treatment and can involve the sclera, with serious consequences, or can cause corneal destruction with perforation.74 Occasionally, the clinical course is much more indolent.72 In patients with HIV infection, the keratitis may be much more resistant to therapy.75
Treatment of these ulcers is often quite difficult; many resistant strains have been encountered. It is important to be aware of the optimal treatment for this common corneal ulcer and to modify therapy appropriately.
Proteus
Infections of the cornea with Proteus organisms are somewhat rare, but are very severe when they do occur. The organism is prevalent in the environment and can be cultured from many seemingly normal eyes.76 These organisms are members of the family Enterobacteriaceae and are commonly found in the intestinal tracts of humans and animals. There are four species in the genus: Proteus vulgaris, Proteus mirabilis, Proteus myxofaciens, and Proteus penneri. P. mirabilis is most commonly isolated from corneal ulcers. The other species are rarely found in eye cultures.
The organisms are gram-negative rods that vary in length according to the amount of time in culture. In early cultures, they appear very long, in snakelike forms, but become much shorter in older cultures and can resemble coccoid rods. Characteristic of the organism is its ability to “swarm” over a culture plate in hours, which produces a sense of wavelike growth. This ability is owing to the presence of many flagella. Like many enteric organisms, it also has many pili, or fine hairlike structures whose functions and purposes are unknown.
The Proteus organisms are nonfastidious and grow rapidly on almost any medium. They exhibit a characteristic, strong, offensive odor when grown on rich media. When identification is not obvious, the more specific tests, such as the phenylalanine deaminase test (only Proteus is positive for this enzyme), may be used. The urease test is occasionally helpful; however, other bacteria are also capable of producing this enzyme, so it is far less specific. The indole test is helpful to speciate Proteus because only P. mirabilis does not produce indole.77 The ornithine decarboxylase test is also helpful to separate species: only P. mirabilis and P. morganii are associated with this enzyme.
The Proteus species elaborate a number of degradative enzymes such as ureases, deaminase, decarboxylase, gelatinase, and lipases.78 Like all enteric gram-negative bacteria, Proteus also produces endotoxin, which may play a role in pathogenesis. Clinically, Proteus causes an intense keratitis, which is characteristic of most enteric bacteria. Dense stromal infiltration with occasional ring abscesses and even perforation has been seen.
Serratia
Serratia marcescens was considered to be a benign saprophyte found in water, soil, and food. It has since been reported to cause central corneal ulceration.79,80
Serratia is an aerobic, gram-negative rod of the Enterobacteriaceae family. It often appears as sheets of gram-negative rods on Gram stain and grows easily on blood agar and enriched broth. There are many species; however, only S. marcescens has been implicated in human disease.
Two cornea-damaging proteases have been isolated and implicated in its pathogenesis. The organism is most commonly associated with contact lens wear and locally compromising ocular conditions, such as bullous keratopathy, neurotrophic keratitis, or keratitis sicca.79 There is a report of three postkeratoplasty patients who developed Serratia corneal ulcers that were traced to the outer grooves of medication bottle tops and the inner surface of eyedrop caps.80 The solution inside these bottles did not yield the organism; the moisture that collected between the cap and the bottle was apparently a culture medium for Serratia.
Clinically, the organism often produces a large yellowish or grayish infiltrate beneath an irregular epithelial defect. There is often significant tissue destruction and necrosis associated with a large hypopyon. Like Pseudomonas, the acute ulcer is associated with stromal edema and swelling, followed by thinning and, occasionally, perforation. As with most bacteria, Serratia has no characteristic that allows certain identification on clinical grounds alone.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree