Purpose
To analyze and compare the postoperative outcomes of eyes with accidental intraoperative inversion of implantable collamer lens (ICL) and viscocannula-assisted reinversion in high myopia.
Design
Retrospective observational case comparison.
Methods
setting: Institutional practice. patients: Consecutive eyes with accidental intraoperative inversion of ICL and viscocannula-assisted reinversion from January 2007 to September 2010 were analyzed retrospectively. They were compared with the fellow eyes with normal ICL implantation at 1 month, 6 months, and 2 years. main outcome measures: Uncorrected visual acuity (UCVA), best-corrected visual acuity (BCVA), corneal pachymetry, endothelial cell loss, intraocular pressure, lens transparency, anterior chamber depth, and postoperative uveitis.
Results
A total of 206 myopic eyes had ICL implantation. Eight eyes (3.8%) of 8 patients had accidental intraoperative reinversion. Their fellow eyes had normal ICL implantation. There was no significant change ( P = .611) in UCVA (reinverted and fellow eyes) at 2 years. There was no significant difference in postoperative UCVA ( P = .611) and BCVA ( P = .854) between the reinverted and the fellow eyes. The mean endothelial loss at 1 month, 6 months, and 2 years was 0.96% ± 0.5%, 0.92% ± 0.63%, and 0.89% ± 0.52% respectively in the reinverted eyes. There was no significant difference in the endothelial loss between the 2 groups at 1 month ( P = .753), 6 months ( P = .834), and 2 years ( P = .916). One out of 8 eyes with reinversion had postoperative corneal edema, which resolved at 48 hours. None of the eyes reported uveitis or glaucoma. There was no loss of lens transparency.
Conclusion
Intraoperative inversion can occur during insertion of ICL and viscocannula-assisted reinversion can be performed without significant complications.
Phakic intraocular lens (IOL) implantation is one of the promising interventions in the recent past for the correction of high myopia. There have been various reports on the visual outcome and postoperative complications of implantable collamer lens (Visian ICL; STAAR Surgicals, Monrovia, California, USA). The major concerns are the postoperative inflammation, anterior capsular opacities, minimal endothelial loss, angle-closure glaucoma, and the luxation of Visian ICL. The inadvertent upside-down Visian ICL implantation is one of the rare complications that can occur. This may cause continuous contact between the ICL and the crystalline lens capsule, which can induce lenticular opacities over a time period or change the refractive outcome. In this article we have shown the incidence and the visual outcome of eyes with accidental intraoperative inversion of the Visian ICL and reinversion with a viscoelastic cannula along with the continuous viscoelastic injection without explantation. We have compared the intraoperative reinverted eyes with the fellow eyes of the patients who had normal phakic IOL implantation.
Materials and Methods
This retrospective study evaluated the eyes of consecutive patients from January 1, 2007 to September 30, 2010 who had accidental intraoperative inversion of Visian ICL (STAAR Surgicals) for the correction of myopia. All the case files of ICL implantation from the described period were reviewed. Patients with bilateral ICL implantation with accidental intraoperative inversion of the Visian ICL followed by viscocannula-assisted reinversion in 1 eye and normal Visian ICL implantation in the fellow eye were included. The best-corrected visual acuity (BCVA), uncorrected visual acuity (UCVA), intraocular pressure (noncontact tonometry), endothelial count (SP-2000P; Topcon, Tokyo, Japan), anterior chamber reaction (Standardization of Uveitis Nomenclature), lens transparency (assessed with serial slit-lamp lens photography), corneal topography (Orbscan; Bausch & Lomb, Rochester, New York, USA), anterior chamber depth (ACD), and slit-lamp biomicroscopy were compared at various time intervals (1 month, 6 months, 2 years) between the reinverted and the fellow eyes.
Surgical Technique
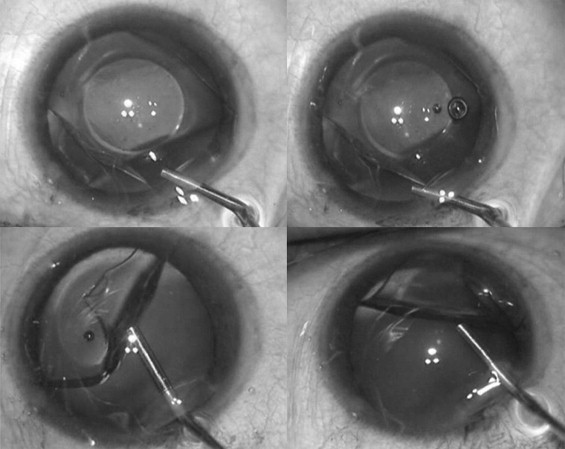
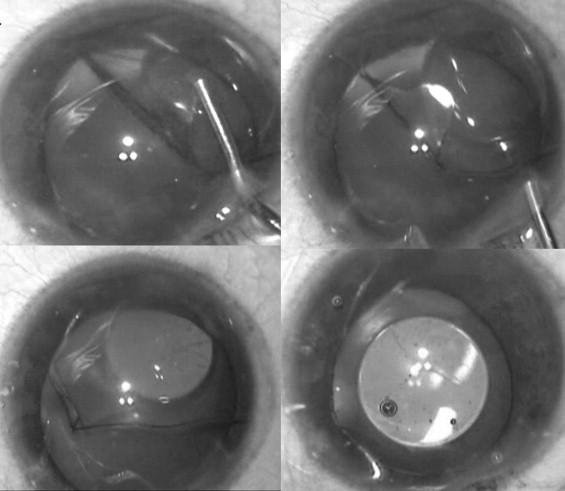
When the Visian ICL was found to have unfolded in the upside-down direction, the anterior chamber was immediately formed with dispersive viscoelastic 2% hydroxypropylmethylcellulose (Viscomet; Milmet Pharma Ltd, Baroda, India). The haptic edge of the Visian ICL was tilted from below with the tip of the viscocannula in the clockwise direction and at the same time the viscoelastic was injected behind the ICL ( Figure 1 ). This step was continued until the ICL was halfway folded. Then the viscocannula tip was placed below the lower flap of the folded ICL and the haptic was pushed up ( Figure 2 ), thereby unfolding the ICL. This placed the ICL in the correct position. Care was taken not to touch the optical center of the ICL. A surgical peripheral iridectomy (PI) was performed and the entry wound in the cornea was hydrated. All patients were on topical antibiotics and steroids in the immediate (2 weeks) postoperative period.
Statistical Analysis
Data were entered in a Microsoft Excel spreadsheet (Microsoft Corp, Redmond, Washington, USA) and analyzed using SPSS version 16.1 (SPSS Inc, Chicago, Illinois, USA). The differences were considered statistically significant at P < .05.
Results
In the retrospective analysis, a total of 206 eyes underwent Visian ICL implantation in the described period. Out of 206 eyes, 8 eyes (3.8%) of 8 patients had accidental intraoperative inversion. All 8 patients had inversion of ICL with viscocannula-assisted reinversion in 1 eye and normal ICL implantation in their fellow eyes. All 8 inversions were noted only in the early learning curve. There were 4 right (OD) and 4 left (OS) reinverted eyes. The preoperative refractive error ranged from −14 diopters (D) to −18 D in the reinverted and −14.5 D to −18 D in the fellow eyes. The mean preoperative ACD was 2.88 ± 0.08 mm and 2.89 ± 0.07 mm in the reinverted and the fellow eyes respectively. The mean white-to-white (WTW) distance was 11.3 ± 0.4 mm and 11.2 ± 0.4 mm in the reinverted and the fellow eyes respectively.
The mean postoperative UCVA and BCVA were 0.74 ± 0.21 and 0.78 ± 0.25 respectively in the reinverted eyes. There was significant improvement in the postoperative UCVA in the reinverted (Wilcoxon signed rank test P = .012) and the fellow eyes ( P = .028). There was no significant difference (Mann-Whitney U test, 1 month, 6 months, and 2 years) between the 2 groups with respect to UCVA ( P = .611) and BCVA ( P = .854).
There was no significant difference ( Table 1 ) in the pachymetry from the preoperative to the postoperative period in both groups. There was no significant difference between the preoperative and the postoperative anterior chamber depth in the reinverted eyes (Wilcoxon signed rank test P = .066). There was no significant difference between the reinverted and the fellow eyes with respect to the postoperative ACD ( P = .915). The mean preoperative cell density was 3256.4 ± 299.9 cells/mm 2 and the mean cell density at 2 years postoperatively was 3169.4 ± 277.5 cells/mm 2 in the reinverted eyes. The mean percentage loss at 1 month, 6 months, and 2 years was 0.96% ± 0.5%, 0.92% ± 0.63%, and 0.89% ± 0.52% respectively in the reinverted eyes. There was no significant difference ( Table 2 ) in the percentage loss of the endothelial cells between the 2 groups at 1 month ( P = .753), 6 months ( P = .834), and 2 years ( P = .916). One out of 8 eyes with reinversion had postoperative corneal edema, which spontaneously resolved at 48 hours, and on day 1 the endothelial cell count was measured as 2530 cells/mm 2 . There was no significant difference between the reinverted and the fellow eyes with respect to postoperative Sim K value in Orbscan ( P = .645). None of the eyes reported postoperative uveitis or glaucoma in the 2 years of follow-up. Lens transparency was maintained in all eyes, as seen by the serial slit-lamp lens photography. The mean vault in the reinverted eyes was 0.41 mm ± 0.3 mm.
| Preoperative UCVA (Decimal Equivalent) | 1 Month | 6 Months | 24 Months | Preoperative CCT (μm) | 1 Month | 6 Months | 24 Months | Preoperative ACD (mm) | 1 Month | 6 Months | 24 Months | |
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Fellow eyes | 0.66 | 1 | 1 | 1 | 594 | 578 | 588 | 588 | 2.9 | 2.88 | 2.88 | 2.88 |
| 1 | 1 | 1 | 1 | 588 | 584 | 588 | 588 | 2.9 | 2.91 | 2.91 | 2.91 | |
| 1 | 1 | 1 | 1 | 652 | 658 | 650 | 652 | 2.88 | 2.86 | 2.86 | 2.86 | |
| 0.16 | 0.33 | 0.33 | 0.33 | 603 | 756 | 630 | 606 | 2.9 | 2.9 | 2.9 | 2.9 | |
| 0.25 | 0.66 | 0.66 | 0.66 | 429 | 448 | 440 | 440 | 3 | 3 | 3 | 3 | |
| 0.05 | 0.66 | 0.66 | 0.66 | 559 | 562 | 560 | 558 | 3 | 2.9 | 2.9 | 2.9 | |
| 0.16 | 0.66 | 0.66 | 0.66 | 487 | 490 | 480 | 484 | 2.8 | 2.78 | 2.78 | 2.78 | |
| 0.16 | 1 | 1 | 1 | 580 | 500 | 482 | 442 | 2.8 | 2.8 | 2.8 | 2.8 | |
| Reinverted eyes | 0.01 | 1 | 1 | 1 | 594 | 578 | 588 | 588 | 2.82 | 2.81 | 2.81 | 2.81 |
| 0.01 | 1 | 1 | 1 | 588 | 584 | 588 | 588 | 2.9 | 2.9 | 2.9 | 2.9 | |
| 0.01 | 0.5 | 0.5 | 0.5 | 652 | 658 | 650 | 652 | 2.88 | 2.86 | 2.86 | 2.86 | |
| 0.01 | 0.66 | 0.66 | 0.66 | 603 | 756 | 630 | 606 | 2.9 | 2.9 | 2.9 | 2.9 | |
| 0.01 | 0.5 | 0.5 | 0.5 | 429 | 448 | 440 | 440 | 3 | 3 | 3 | 3 | |
| 0.03 | 1 | 1 | 1 | 559 | 562 | 560 | 558 | 3 | 2.96 | 2.96 | 2.96 | |
| 0.05 | 0.66 | 0.66 | 0.66 | 487 | 490 | 480 | 484 | 2.8 | 2.78 | 2.78 | 2.78 | |
| 0.1 | 0.66 | 0.66 | 0.66 | 520 | 512 | 514 | 498 | 2.8 | 2.8 | 2.8 | 2.8 |
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


