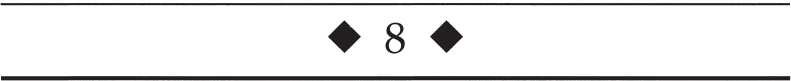
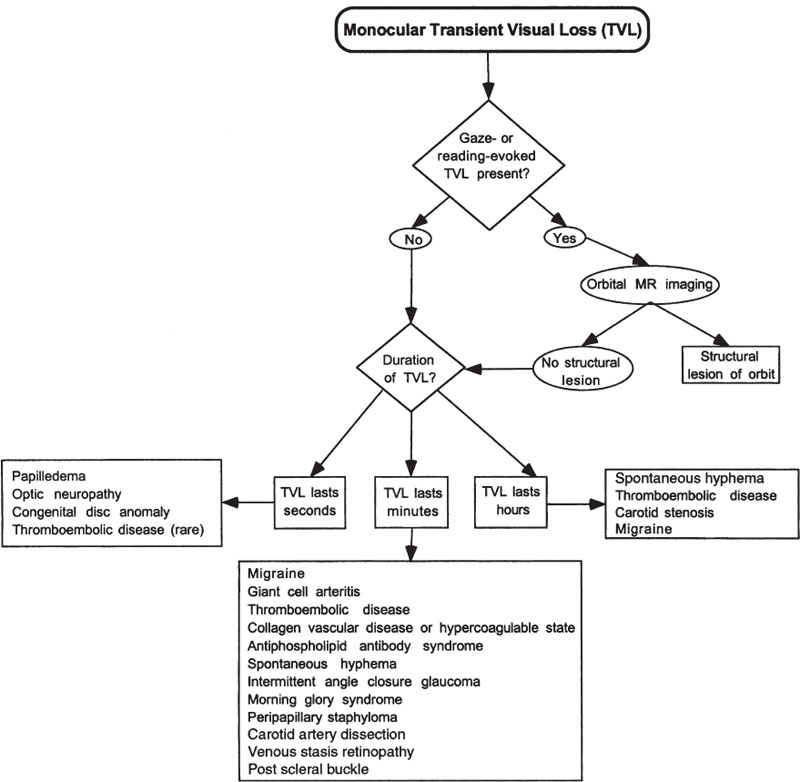
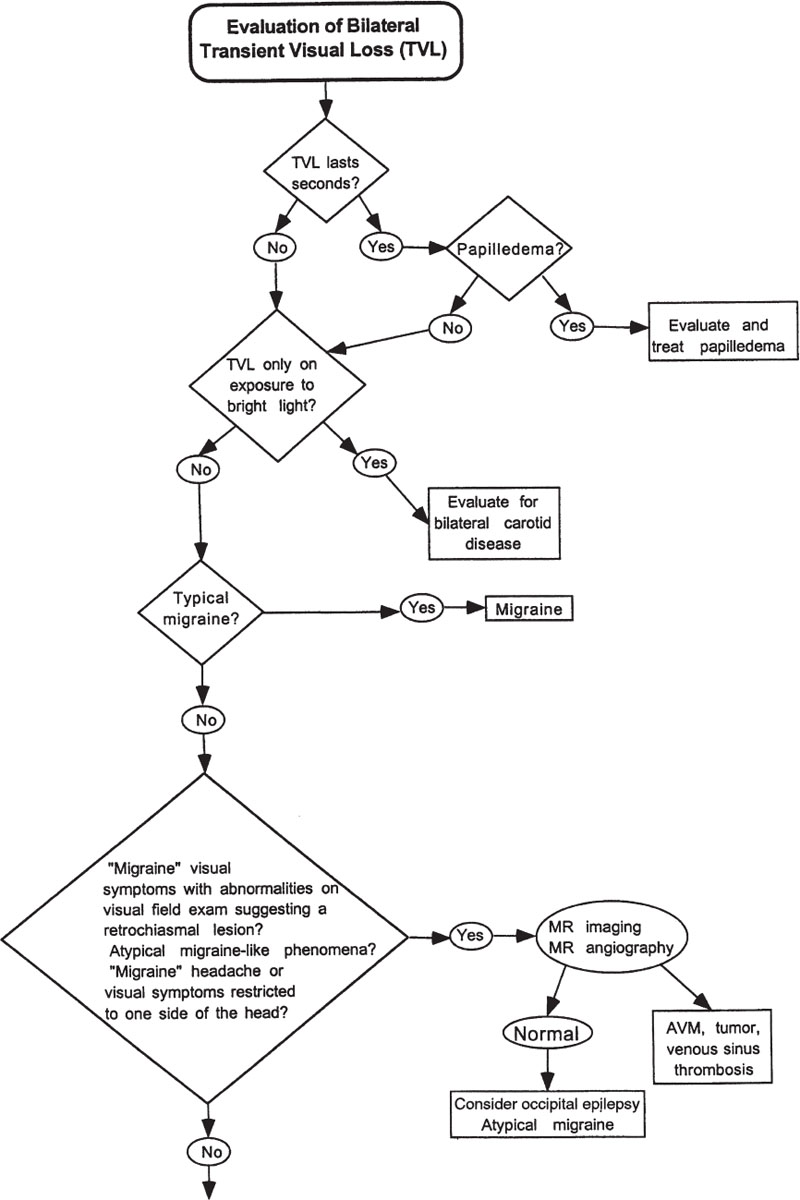
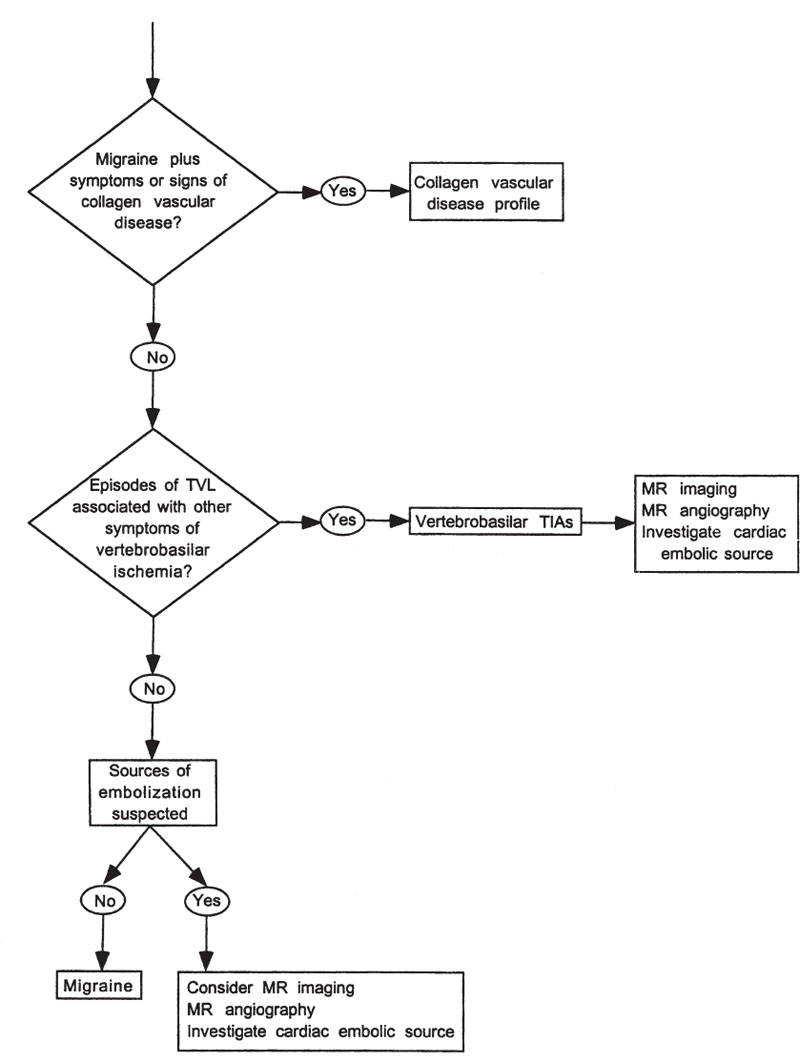
Transient Visual Loss What Questions Should Be Asked of a Patient with Transient Visual Loss? The most important questions that need to be addressed in the assessment of the patient with transient visual loss (TVL) include the following: 1. Is the visual loss monocular or binocular? Monocular TVL implies disease of the eye, retina, optic nerve, orbit, circulation to the eye (e.g., heart, aorta, carotid artery, ophthalmic artery, central retinal artery), or migraine. Binocular TVL implies bilateral eye disease, disease affecting the circulation to both eyes (e.g., bilateral carotid stenosis), increased intracranial pressure with papilledema, vertebrobasilar ischemia or insufficiency, or migraine. 2. What is the temporal profile of the transient loss of vision? For example, TVL in one eye lasting seconds is characteristic of transient obscurations of vision resulting from optic nerve ischemia or papilledema. Monocular TVL lasting 2 to 30 minutes is characteristic of TVL associated with carotid artery disease. 3. What are the precipitants of the visual loss? For example, patients with an intraorbital mass may develop TVL only in certain eye positions due to the mass compressing the ipsilateral optic nerve or optic nerve circulation (gaze-evoked amaurosis). Monocular or binocular TVL due to carotid disease may occur following exposure to bright light. 4. Are optic nerve or retinal vessel abnormalities evident on funduscopic examination? For example, the fundus exam may reveal papilledema in transient obscurations of vision, retinal emboli in carotid or cardiac disease, and disc anomalies in monocular TVL. This chapter discusses various entities that may cause monocular or binocular TVL. Approaches to patients with monocular and binocular transient visual loss are given in Figures 8–1 and 8–2, respectively. Figure 8–1. Evaluation of monocular transient visual loss (TVL). Does Monocular TVL Occur Only in Certain Positions of Gaze (Gaze-Evoked TVL)? Patients who experience TVL evoked by eccentric position of gaze (gaze-evoked TVL) usually have an intraorbital mass that intermittently compresses the circulation to the optic nerve or retina (Bremner, 1999; Danish-Meyer, 2001; Knapp, 1992; Kohmoto, 1993; Mezer, 1997; Smith, 1998). The visual loss immediately clears when the direction of gaze is changed. The most common lesions are orbital cavernous hemangiomas or optic nerve sheath meningiomas. Other orbital lesions producing this sign include osteomas, neurofibromas, gliomas, medial rectus granular myoblastoma, metastases, varices, orbital trauma, thyroid eye disease, and intraocular foreign body (buckshot pellet). The examination may be normal or show evidence of an optic neuropathy with an afferent pupil defect, color vision impairment, disc edema, and optociliary collateral vessels. Other signs of orbital tumor, such as proptosis, limitation of extraocular muscle movement, swelling of the eyelids, Chemosis, and conjunctival congestion, may be evident. Evaluation requires magnetic resonance imaging (MRI) or computed tomography (CT) scans of the orbital structures. Intermittent visual loss and exophthalmos may occur with bending over or the Valsalva maneuver (Sobottka Ventura, 2001). Gaze-evoked monocular TVL has also been noted in patients with pseudotumor cerebri (O’Duffy, 1998). It has been hypothesized that in an eccentric position of gaze, ischemic compression of a tense dilated optic nerve sheath results in elevation of intrasheath pressure compromising blood flow to the retina or optic nerve (Miller, 1991; O’Duffy, 1998). Figure 8–2. Evaluation of binocular transient visual loss (TVL). Does the Visual Loss Occur After Prolonged Reading (Reading-Evoked TVL)? Reading may also induce monocular TVL. Manor et al described a 49-year-old man with a 5-year history of dimming of central vision in the left eye provoked only during reading (Manor, 1996). An orbital apex tumor situated lateral to and above the optic nerve was found. This reading-evoked visual dimming may be a variant of gaze-evoked TVL. The optic nerve, displaced laterally and superiorly and stretched by the act of reading, may have been compressed between the tumor and the contracted inferior rectus muscle. Thus, orbital neuroimaging is appropriate in patients with reading-induced TVL. Intermittent angle closure glaucoma may cause TVL, and reading-induced TVL has been reported in one case. O’Sullivan et al described a 66-year-old patient with episodes of monocular TVL lasting 3 minutes to several hours that were precipitated by reading, writing, or watching television (O’Sullivan, 1995). Ophthalmologic exam was normal but reading over 4 hours induced corneal edema, a poorly reactive semidilated pupil, and a shallow anterior chamber with intraocular pressure of 50 mm Hg. The intermittent angle closure glaucoma and the patient’s symptoms were treated successfully by iridotomies. Do the Episodes of Monocular TVL Last Seconds? Episodes of TVL lasting less than 60 seconds may occur in patients with papilledema (Wall, 1991). These transient obscurations of vision may occur in one or both eyes (individually or simultaneously) and typically last only a few seconds, though in rare cases they may last for hours. The episodes may be precipitated by changes in position, and are thought to be related to the effects of increased intracranial pressure on the flow of blood to the eye, perhaps where the central retinal artery penetrates the optic nerve sheath to enter the substance of the nerve (Miller, 1991). Similar monocular TVL lasting seconds may occur in optic nerve sheath meningiomas unrelated to increased intracranial pressure. The pathogenesis of these episodes in meningioma is unknown and may be caused by the effect of the meningioma on the central retinal artery where it enters the optic nerve (Miller, 1991). Transient obscurations of vision may also occur in an eye with congenital abnormalities of the optic disc, such as peripapillary staphyloma (see below), or optic disc drusen. A case of ice-pick headaches associated with monocular visual loss with scintillating scotoma lasting seconds has been described in a patient with a history of migraine with visual aura (Ammache, 2000). The patient was treated with oxygen inhalation and indomethacin with complete resolution of the symptoms. Finally, carotid atherosclerotic disease may rarely cause very brief episodes of transient visual loss, but more often attacks of TVL with carotid disease last 2 to 15 minutes (see below). Patients with transient visual obscurations first require ophthalmologic examination. If papilledema is evident (Chapter 7), these patients must have an MRI scan of the brain. If this study is normal, a spinal tap is indicated to investigate the possibility of infection or pseudotumor cerebri (idiopathic intracranial hypertension). Patients with drusen or other optic disc anomalies causing monocular TVL may require no further evaluation. If there are signs of an optic neuropathy on the side of the TVL (e.g., relative afferent pupillary defect, ipsilateral swollen or atrophic optic nerve, etc.), then MRI with attention to the orbit is warranted to evaluate a compressive lesion. Patients without apparent disc abnormalities should be screened for carotid atherosclerotic disease or other sources of emboli (see below). In selected cases, MRI should be performed to investigate the possibility of a structural brain lesion such as optic nerve sheath meningioma. Do the Episodes of Monocular TVL Last Minutes? Monocular TVL lasting 5 to 60 minutes (usually 2 to 30 minutes) is strongly suggestive of thromboembolic disease. Retinal emboli may arise from the aorta (Romano, 1998), the carotid artery, or the heart. Patients often describe the TVL as a veil or shade descending or ascending over a portion of their visual field. Other patients complain of patchy visual loss (“Swiss cheese” pattern) or peripheral constriction with central visual sparing (Bruno, 1990). Some episodes of monocular TVL are accompanied by a sensation of color or other photopsias. These may superficially be similar to migraine, consisting of showers of stationary flecks of light that disperse quickly (Bruno, 1990; Goodwin, 1987; Pessin, 1977). Most episodes of embolic monocular TVL last 2 to 30 minutes. Marshall and Meadows found that in 51 of 67 patients (76%) episodes lasted 30 minutes or less, with 29 patients (43%) experiencing episodes lasting 5 minutes or less (Marshall, 1968). Pessin et al noted that attacks lasted less than 15 minutes in 30 of 33 patients, and in 14 patients (42%) the episodes lasted 5 minutes or less (Pessin, 1977). Among 35 patients evaluated by Goodwin et al, 22 patients (63%) had attacks lasting 5 minutes or less, 8 (23%) had episodes lasting 6 to 15 minutes, and 6 patients (17%) had episodes lasting more than 15 minutes (Goodwin, 1987). Episodes of monocular TVL due to thromboembolic disease rarely last several hours. Patients with thromboembolic disease may demonstrate emboli within the retinal vessels. Emboli may be composed of clotted blood, fibrin, platelets, atheromatous tissue, white cells, calcium, infectious organisms (septic emboli), air, fat, tumor cells, amniotic fluid, or foreign materials (e.g., talc, artificial valve material, catheters, silicone, cornstarch, mercury, corticosteroids). The most common types of emboli seen in atherosclerotic disease of the aorta/carotid arteries or cardiac disease include the following: 1. Cholesterol emboli (Hollenhorst plaques) are bright, glistening, yellow or copper-colored fragments, most often seen in peripheral arterioles in the temporal fundus. These emboli most often arise from atheromatous plaques in the aorta or carotid bifurcation. 2. Platelet-fibrin emboli are dull, white, gray, often elongated, and subject to fragmentation and distal movement. These emboli most often lodge at bifurcations of retinal vessels and arise from the walls of atherosclerotic arteries or from the heart, especially from heart valves. They may also be seen in coagulopathies. 3. Calcific emboli tend to be large, ovoid or rectangular, and chalky-white. These emboli often occur over or adjacent to the optic disc. They usually arise from cardiac (aortic or mitral) valves and less often from the aorta or carotid artery. Unlike cholesterol emboli, which often disappear in a few days, calcific emboli may remain permanently visible. Sharma et al found the sensitivity and specificity of visible retinal emboli for the detection of hemodynamically significant (defined as greater than or equal to 60%) carotid stenosis to be 39% and 68%, respectively, in patients with acute retinal artery occlusion (Sharma, 1998). The presence of a visible embolus generated a likelihood ratio of 1.24, whereas the absence of a visible embolus generated a likelihood of 0.88. The authors concluded that the presence of a visible embolus is a poor diagnostic test for the detection of hemodynamically significant carotid artery stenosis in the setting of acute retinal artery occlusion. Klein et al described the prevalence at baseline and the 5-year incidence of retinal emboli in the Beaver Dam Study. They reported the associated risk factors, the relationship of retinal emboli at baseline to stroke, and ischemic heart disease mortality in these patients. The study consisted of 4,926 patients, aged 43 to 86 years at baseline (Klein, 1999). The prevalence of retinal emboli at baseline was 1.3% and the 5-year incidence was 0.9%. The prevalence of retinal emboli was associated with high pulse pressure, hypertension, diabetes mellitus, past and current smoking, cardiovascular disease, and the presence of retinopathy. Patients with retinal emboli had a significantly higher risk of dying with stroke than those without retinal emboli. TVL may also occur from ocular hypoperfusion rather than embolization. In some patients, monocular TVL may occur when the patient is exposed to bright light. These patients usually have severe, ipsilateral carotid occlusive disease. Bilateral, simultaneous TVL induced by exposure to bright light may rarely occur with bilateral severe carotid stenosis or occlusion (Kaiboriboon, 2001). The light-induced TVL probably reflects the inability of a borderline ocular circulation to sustain the increased retinal metabolic activity associated with light exposure. Alternating transient visual loss to bright light has also been described with giant cell arteritis (Galetta, 1997). One prospective study assessed the clinical features of monocular TVL and the likelihood of atherosclerotic lesions of the internal carotid artery (ICA) (Donders, 2001). Of the 337 patients, 159 had a normal ICA on the relevant side, 33 had a stenosis of 0 to 69%, 100 had a stenosis of 70 to 99%, and 45 had an ICA occlusion. An altitudinal onset or disappearance of symptoms was associated with atherosclerotic lesions of the ipsilateral ICA. A severe (70 to 99%) stenosis was also associated with duration of TVL between 1 and 10 minutes, and with a speed of onset in seconds. An ICA occlusion was associated with attacks being provoked by light, an altitudinal character, and the occurrence of more than 10 attacks. TVL may also occur with carotid artery dissection. In a review of the clinical features of 146 patients with extracranial carotid artery dissection, 41 patients (28%) had monocular TVL. The TVL was painful in 31 cases, associated with a Horner’s syndrome in 13 cases, and described as “scintillations” or “flashing lights” (often related to postural changes suggesting choroidal hypoperfusion) in 23 cases (Biousse, 1998b). Two of 23 patients with spontaneous carotid artery dissection experienced transient monocular blindness; in one of these patients, episodes were provoked by sitting up from a supine position (Kerty, 1999). Postprandial transient visual loss has also been described (Levin, 1997). In one patient, episodes of splotchy visual loss occurred unilaterally on the left 1 hour after eating her largest meal of the day. The episodes lasted approximately 3 hours and were occasionally accompanied by numbness and weakness of the contralateral arm. Severe left carotid stenosis was noted. In a second patient, blotchy bilateral transient visual loss episodes lasting 2 minutes to 1.5 hours were precipitated by eating or standing from a sitting or lying position. This second patient was found to have complete occlusion of the right carotid artery and moderate stenosis of the left carotid artery. The authors proposed that postprandial visual loss may be a symptom of critical carotid stenosis, with retinal and choroidal hypoperfusion probably caused by a combination of mesenteric steal, decreased cardiac output, and abnormal vasomotor control (Levin, 1997). Venous stasis retinopathy (hypotensive retinopathy), associated with severe carotid or ophthalmic artery occlusive disease, may also be associated with TVL (Gass, 1997). This syndrome is characterized by visual loss and ischemic retinal infarction often accompanied by signs of ciliary artery obstruction, pallor of the disc, and hypotony. Venous stasis retinopathy may simulate Purtscher’s retinopathy (multifocal areas of ischemia) and be associated with a variety of fundus pictures (Gass, 1997): 1. Minimal or no ophthalmoscopic changes in some patients with monocular TVL. 2. Few widely scattered blot and dot hemorrhages and mild dilation of retinal veins (venous stasis retinopathy), usually in patients with minimal visual complaints. 3. Dilation of the retinal arterial tree, dilation of the retinal veins, and cotton-wool patches. 4. Retinal capillary changes, including microaneurysms, cystoid macular edema, and angiographic evidence of areas of capillary nonperfusion that may be confined to the areas along the horizontal raphe. 5. Larger areas of peripheral capillary nonperfusion, retinal neovascularization, and hemorrhage. 6. Any degree of branch retinal vein occlusion, branch retinal vein occlusion, branch retinal artery occlusion, and central retinal artery occlusion. 7. Ischemic optic neuropathy. 8. Fluorescein angiography showing diffuse retinal capillary telangiectasia, delayed retinal artery circulation time, late staining of the disc, and aggregations of microaneurysms around the preequatorial zone mimicking idiopathic juxtafoveal retinal telangiectasia. 9. Any of the above associated with panuveitis, neovascular glaucoma, and a rapidly progressing cataract (ocular ischemic syndrome). Venous stasis retinopathy may be difficult to differentiate from central retinal vein occlusion (CRVO). Helpful differentiating features include the following: 1. The retinal veins are irregular in caliber with venous stasis retinopathy. 2. Hemorrhages, microaneurysms, and capillary dilations are often peripheral rather than in the posterior pole with venous stasis retinopathy (with CRVO these changes are often diffuse rather than peripheral). 3. Venous stasis retinopathy is not associated with disc edema or optociliary veins (compared with CRVO). The ocular ischemic syndrome (Gass, 1997; Malhotra, 2000) is a progressive disorder due to hypoperfusion of eye that may be associated with TVL and ocular discomfort or frank pain localized to the orbit and upper face that is often decreased when the patient lies down. Rubeosis iridis in an older nondiabetic patient without evidence of venous obstructive disease or other predisposing cause is suggestive of the ocular ischemic syndrome. In persons over the age of 50 with new-onset iritis, the possibility of ocular ischemic syndrome should be considered. It is usually due to atherosclerotic carotid or ophthalmic artery disease. Other less common causes for venous stasis retinopathy and the ocular ischemic syndrome include giant cell arteritis, carotid artery dissection, cavernous sinus thrombosis, Takayasu’s disease, fibromuscular dysplasia, mucormycosis, herpes zoster ophthalmicus, myelofibrosis, vasospasm, and postaneurysm repair (Borruat, 1993; Casson, 2001; Gupta, 1990; Hamed, 1992; Hwang, 1999; Lewis, 1993; Meire, 1991; Winterkorn, 1995; Zimmerman, 1995). Four of seven patients with maxillofacial arteriovenous malformations (AVMs) that had been treated previously with proximal ligation of the supplying external carotid artery had signs of ocular ischemia (Andracchi, 2000). These four patients had significant ophthalmic artery supply by the malformations, suggesting that when the ophthalmic arterial blood supply is recruited, an ophthalmic artery “steal” phenomenon occurs, causing ocular ischemia. This “steal” may be precipitated or worsened by previous surgical proximal ligation of external carotid arterial branches that are potential collaterals with the ophthalmic artery but fail to occlude the arteriovenous shunt. Giant cell arteritis (GCA) may produce attacks of TVL lasting minutes to hours indistinguishable from those produced by atheromatous disease (Hayreh, 1998a,b) (see Chapter 5). TVL probably results from intermittent inflammatory occlusion of the ophthalmic, posterior ciliary, or central retinal arteries. A postural form of TVL has been described in giant cell arteritis and a tenuous optic disc perfusion (Wykes, 1984). Alternating monocular TVL may occur with GCA (Finelli, 1997) and may be induced by bright light (Galetta, 1997). TVL may also occur in association with antiphospholipid antibodies, hyperviscosity and hypercoagulable states, polycythemia vera, systemic lupus erythematosus (SLE), and hepatitis C–associated type II cryoglobulinemia-mediated systemic vasculitis with mononeuritis multiplex. AVMs may divert blood flow from or reduce blood flow in the ophthalmic artery (ophthalmic steal syndrome) (Case Records of the MGH, 1999; Donders, 1998; Levine, 1990). The TVL may alternate from eye to eye. Donders et al noted that TVL occurred in 6% of patients with SLE (Donders, 1998). In patients with SLE, there was no relationship between TVL and the presence of antiphospholipid antibodies or livedo reticularis. Five of 10 patients with SLE had TVL in either eye (alternating TVL).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


